Introduction
Skin banks play a critical role in the management of complex wounds, particularly in the treatment of severe burns. These specialized facilities are responsible for the procurement, processing, preservation, and distribution of human skin tissue primarily used as temporary biological coverage. In this chapter, we will focus specifically on the types of skin substitutes and biologic materials processed and dispensed by hospital-based skin banks, which traditionally serve the needs of regional burn centers and surgical units. These include cadaveric skin allografts, human amniotic membrane (HAM), and in selected European centers, human acellular dermal matrices (HADM) or de-epidermized dermis (DED) prepared within the skin bank itself. It is important to distinguish hospital skin banks from a broader category of tissue banks, many of which are managed by private or commercial entities. These organizations may offer a wide and evolving range of biologic and synthetic graft materials—such as decellularized dermis, bone allograft, bone matrix, cartilage allograft, tendon allograft, fascia allograft, xenograft, and various advanced wound matrices—that are not within the direct purview of traditional skin banks. The discussion of such commercially produced and rapidly changing products is beyond the scope of this chapter. A complete list of establishments accredited by the AATB (American Association of Tissue Banks) can be found online.
Our aim is to provide a clear and practical overview of the standard products routinely processed and provided by hospital skin banks, their indications, limitations, and clinical applications, particularly in the context of burn surgery and reconstructive care.
The most used hospital skin bank product is skin allograft. After excision and debridement of deep partial-thickness or full-thickness burns, allograft skin is frequently used as a temporary biologic dressing. Allografts are harvested from cadaveric human donors and typically consist of split-thickness skin including both epidermis and part of the dermis. Their primary role is to provide immediate physiologic wound coverage—protecting the underlying tissue from infection, minimizing evaporative fluid and heat loss, reducing pain, and preparing the wound bed for eventual definitive closure. Allografting serves not only as protection but also as a biologic “test dressing” that allows for assessment of the wound bed’s viability; successful adherence and graft take indicate a vascularized surface suitable for final grafting. This approach is particularly valuable in patients with extensive burns who may not have sufficient donor sites available or are not yet physiologically stable for definitive skin grafting. By temporarily covering the wound, the allograft allows the wound to stabilize, promotes granulation, reduces the risk of contamination, and provides time for donor site recovery. Although initially viable, allografts are immunologically foreign tissue and are therefore not permanently accepted by the host. Within 7 to 14 days, they are progressively rejected by the recipient’s immune system, undergo necrosis, and are subsequently sloughed off. This predictable rejection is not considered a treatment failure but rather an expected and essential phase in the staged management of complex burn wounds. Allografts thus play a critical role in bridging the gap between excision and definitive coverage with an autologous split-thickness skin graft (STSG). In many cases, the autologous STSG is typically performed on day 7–10 after the application of allograft, but this can be earlier or later depending on individual patient needs. Before applying the autologous STSG, the residual allograft that eventually took and got incorporated is excised, so that the wound bed is prepared to host the final autologous STSG.
A skin bank is a facility that stores and distributes donated epidermal and dermal tissue and amnion for use in medical procedures such as grafting. The stored skin is called allograft or homograft, and it is harvested from human cadavers. Donated skin from cadavers is carefully screened, processed, and stored to ensure its quality and safety.
By providing a source of donated skin tissue, the skin bank can help to ensure that patients receive the care they need in a timely manner, which can be critical for their recovery.
In addition to providing a source of skin tissue for grafts, the skin bank can also help to reduce the risk of complications associated with skin grafts. Donated skin tissue is carefully screened and processed to ensure that it is disease-free and noncontaminated, which is particularly important in burn patients, who have profoundly decreased immune function and are therefore susceptible to a multitude of opportunistic and nosocomial infections. This can help to reduce the overall risk of infection and other complications that can arise from skin grafts and can improve the overall success rate of the procedure. Another benefit of the skin banks is that they can help to reduce the demand for live skin donors. In the past, skin grafts were often performed using skin taken from other parts of the patient’s body (autograft). However, this can be a painful and invasive procedure, and it may not be feasible in cases where the patient has suffered extensive burns or injuries. The application of allograft is only a temporary solution because the patient will eventually need autograft when their condition improves, but the utility in providing temporary coverage lies in the ability to improve wound healing, reduce fluid loss and electrolyte imbalances, and ultimately reduce mortality. ,
Furthermore, biologically active cryopreserved human skin allografts (homograft) have been found to be safe and effective in treating wounds with exposed bone and/or tendon, which are notoriously difficult to successfully provide coverage for.
Available products
Products processed, stored, and distributed by the skin bank include:
-
■
Skin from cadavers (called allograft or homograft). This is typically a Split-Thickness Skin Allograft that includes epidermis and part of dermis but can also be a be a Full-Thickness Skin Allograft which includes the entire epidermis and the full dermis. Fresh or Fresh-Frozen Human Skin is available in some academic hospital tissue banks; it has a very short shelf life (5–10 days) and its use is rare; it is used when living cells are preferred.
-
■
Dermis (de-epidermized dermis [DED] , and human acellular dermal matrix [HADM]) only available in European skin banks, due to specific regulations .
-
■
Human amniotic membrane (HAM or human amnion)
Allograft skin is widely used for wound management in burn centers and it functions as biological dressing for the burn wound.
The production of DED by the skin bank of Siena, Italy, and its properties have been described by Fimiani et al. and by Tognetti et al. To prepare the DED, the skin is de-epidermized manually. DED can be cryopreserved or glycerol-preserved and has several indications including full-thickness burns. The skin can also be de-epidermized using the sodium chloride solution method.
The DED can then undergo a decellularization process to produce HADM. HADM has been used since 1995 for burn-wound treatment. Moreover, split-thickness skin grafting on HADM scaffold for the treatment of deep burn wounds has been described by several authors. HADM acts as a dermal scaffold for neodermis and neoepidermis formation in deep-dermal burn wounds. Extracellular matrix (ECM) is the largest element of the dermal layer, and its components include proteoglycans, hyaluronic acid, collagen, and elastin. Human acellular dermal matrices provide an ECM scaffold used to treat deep burn wounds.
The HAM is a waste product in cesarean section procedures and normal labor, therefore it has no ethical objections. , Amnion has been shown to alleviate pain, prevent infection, reduce pruritus, and accelerate wound healing. , , Our institution has used amniotic membrane for temporary total ocular surface coverage in the treatment of toxic epidermal necrolysis, which has shown improvements in corneal clarity, conjunctival scaring, and dry eye symptoms at 3-month follow-up as compared with a historical group that received maximal medical treatment available. Furthermore, dehydrated HAM wound dressing is a safe alternative to cadaveric allografts in treating pediatric partial-thickness facial burns.
The preparation and storage of amnion has been a role for many skin banks around the world. Although using human amnion as a temporary biological wound dressing is inferior to allogenic skin, it is an excellent, cost-effective means of burn treatment in developing countries that experience a high incidence of burn injuries complicated by financial constraints. , Although these countries may not be able to finance costly skin banks, the procurement and storage of amniotic membrane is affordable comparatively, relatively easy to execute, and provides a reliable and long-lasting resource for burn wound coverage.
In a recent meta-analysis, Yang et al. found out that HAM treatment was more effective than conventional methods, silver sulfadiazine, and polyurethane membrane in treating burn wounds, but HAM appeared to be less effective than honey. Other products are not typically dispensed by hospital skin banks, but are produced, stored and dispensed by private biotech/wound care companies (for example Acellular Dermal Matrices like AlloDerm, FlexHD, Bioengineered skin like Apligraf or Dermagraft, and injectables like micronized dermis; these are not hospital skin bank products).
History
The idea of storing human skin stemmed from Wentscher in 1903 when he reported cellular viability of human skin after it was refrigerated for 3 to 14 days. However, it was not until the 1930s that blood and tissue banking took their place in the clinical practice of medicine. The clinical utility of allograft skin in burn-wound coverage was first described by Bettman in 1938. He reported his success in the treatment of children with extensive full-thickness burn injuries and pleaded for the use of homogenous Thiersch grafts as lifesaving measures against otherwise fatal sepsis. Webster and Matthews later described the successful healing of skin autografts stored for 3 weeks at 4°C to 7°C; however it was not until 1949, after the establishment of the US Navy tissue bank, that modern-day skin banking began. In 1960, the first tissue bank in Europe was founded in England, the Yorkshire Regional Tissue Bank, and the Netherlands followed suit in 1976 with establishment of the Dutch National Skin Bank, now known as the Euro Skin Bank.
The establishment of skin banking signaled the beginning of significant research related to the processing, preservation, and storage of human tissues. Baxter explored the histologic effects of freezing on human skin and discovered that the formation of ice crystals caused the destruction of skin architecture. This was followed in 1952 by the pioneering research of Billingham and Medawar, who demonstrated that skin could be effectively cryopreserved using glycerol. Soon afterward, Taylor was able to demonstrate that the addition of glycerol to storage solutions decreased ice crystal formation in frozen tissues. These advancements permitted Brown and Jackson to popularize the use of allogeneic human skin grafts as biologic dressings for extensive burns and denuded tissue. By 1966, Zaroff had reported the 10-year experience using allograft skin in the treatment of thermally injured patients at the Brooke Army Medical Center. In this report, he described the mechanical and physiologic advantages of allograft skin as a biologic dressing. In 1966, Cochrane reported the first successful use of frozen autologous skin grafts after controlled-rate freezing in 15% glycerol and rapid rewarming before implantation. This was followed by Morris’s report demonstrating the beneficial effects of using allogeneic skin in the treatment of infected ulcers and other contaminated wounds and by Shuck’s report suggesting the potential use of allogeneic skin in the treatment of traumatic wounds based on their Vietnam War experience. These increased uses of allograft skin led to further research into the beneficial effects of allograft skin on wound healing, including its association with a reduced incidence of bacterial infections , and the stimulation of wound bed neovascularization. ,
Bondoc and Burke are credited with the establishment of the first functional skin bank in 1971. Their experience with allograft skin led to a report of successful burn-wound excision and allografting with temporary immunosuppression in children with extensive injuries. Today, allograft skin remains an ideal temporary cover for extensive or excised cutaneous or soft-tissue wounds, particularly when sufficient autograft skin is not available or when temporary wound coverage is desired. Currently, many synthetic skin substitute dressings are available in the market.
One biologic dressing with a long history in the treatment of burned patients is amniotic membrane. It was initially introduced for skin transplantation by Davis in 1910 and was subsequently described for use on burned and ulcerated skin by Sabella in 1912. , During the immediate period after these reports, the use of amniotic membranes was attempted as permanent skin replacements, although the grafts were rejected. In 1952, Douglas was the first to report the use of amniotic membrane as a temporary burn wound covering. Since that time, amnion has been one of the tools available in the treatment of partial-thickness burns. , , ,
The growth of skin banking
The widespread use of allograft skin in the management of patients with extensive burn, traumatic, and soft-tissue injuries has had a major impact on the number of skin banking facilities over the past two decades. Consequently, the majority of skin banks have been founded close to regional burn centers or within burn center hospitals themselves. Skin banks must therefore maintain a close working relationship with regional burn centers, not only to meet the specific needs of the burn surgeon, but also to help generate community support for skin donation through combined educational outreach programs.
From 1969 to 1988, there was a steady growth in the number of skin banks. This number of banks eventually began to decline and reached its nadir in 2002. Since that time, however, there has been a steady increase in the number of skin banking facilities to its current total of 74 American Association of Tissue banks (AATB)- Accredited Establishments that recover, process, store, and/or distribute skin for transplantation worldwide. Fig. 13.1 shows the total number of skin donors and the total square feet of skin distributed by skin banks throughout the United States and Canada from 1995 through 2015.
Skin donation and distribution in the United States and Canada, 1995–2015.
Role of the American Association of Tissue banks
As skin banking facilities grew in number, it became apparent that policies and procedures required standardization. This was quite difficult initially because there were insufficient data to develop a consensus regarding standards of practice. As early as 1976, the AATB had begun to address this issue by the formation of a Skin Council. This provided a forum for the discussion of skin banking practices and was complemented by the activities of the American Burn Association’s (ABA) Skin Banking Special Interest Group. The Standards and Procedures Committees were created in 1977 and produced the first guidelines for tissue banking in 1979. The first Standards for Tissue Banking were published in 1984, and tissue-specific technical manuals (including skin) were developed in 1987. , Since that time, the Standards have been modified and refined based on consensus and, where available, supportive scientific research, with the latest (14th) edition released in 2016. In addition, shortly after the development and promulgation of its Standards for Tissue Banking, the AATB created an inspection and accreditation committee in 1982 and began conducting voluntary inspections in 1986. This program continues today and is important in ensuring that tissue banks adhere not only to AATB Standards but also the US Food and Drug Administration (FDA) regulations governing all aspects of human tissue banking. In 1992, the AATB presented its Year 2000 Plan, outlining the institution’s goals of supporting tissue and cell banks and ensuring the safety and quality of tissues, as well as advancing and strengthening the AATB. The AATB has worked with many organizations, such as the FDA, the Centers for Disease Control and Prevention, and the ABA, to update standards and quickly respond when necessary, such as through the timely creation of instructions and methods to screen potential donors for emerging infectious diseases, including the COVID-19/SARS-CoV-2, monkeypox, West Nile, Ebola, and Zika viruses to reduce risk of infection. Currently, 128 worldwide AATB-accredited tissue banks are listed on the AATB website. Only 74 of them have skin products available in some form, and fewer (estimated around 50) are hospital skin banks. The FDA’s search of registered tissue banks is available online.
Clinical uses of allograft skin
Coverage of extensive full-thickness wounds
The increasing use of allograft skin in specialized burn care centers has been one of the driving forces behind the growth and development of skin banks in the United States. The general indications for its use in wound management are listed in Box 13.1 . Allograft skin possesses many of the ideal properties of biologic dressings and plays a major role in the surgical management of extensive wounds when autologous tissue may not be immediately available ( Box 13.2 ). , It reduces evaporative water loss and the exudation of protein-rich fluids, prevents wound desiccation, and suppresses microbial proliferation. Wound pain is lessened, which is associated with better patient compliance with occupational and physical therapy. By restoring the physiologic barrier at the wound surface, the allografts reduce heat loss through the wound and mitigate the hypermetabolic response to burn injury.
Box 13.1
Indications for Allograft Skin Use in Wound Management
-
■
Coverage of extensive wounds where autologous tissue is not available
-
■
Coverage of widely meshed skin autografts
-
■
Extensive partial-thickness burns
-
■
Extensive epidermal slough
-
■
Stevens-Johnson syndrome
-
■
Toxic epidermal necrolysis
-
■
Staphylococcal scalded skin syndrome
-
■
Testing the wound bed’s ability to accept autograft
-
■
Template for the delayed application of keratinocytes
Box 13.2
Advantages of Human Allograft Skin Use
-
■
Reduce water, electrolyte, and protein loss
-
■
Prevent desiccation of tissue
-
■
Suppress bacterial proliferation
-
■
Reduce wound pain
-
■
Reduce energy requirements
-
■
Promote epithelialization
-
■
Prepare wounds for definitive closure
-
■
Provide dermal template for epidermal grafts
Fresh allograft skin represents the gold standard for all biologic dressings employed for temporary wound closure based on a number of its distinctive properties compared with cryopreserved skin ( Box 13.3 ). Its availability is critically important for the surgeon faced with the need to provide immediate coverage of large, excised burn wounds. Fresh allografts become well-vascularized, stimulate neovascularization in the underlying wound bed, and prepare the recipient sites for permanent coverage with autologous skin. In addition, fresh allografts tolerate modest wound contamination and adhere better to the freshly excised subcutaneous fat than do cryopreserved grafts. The allogeneic skin is usually removed once the patient’s donor sites have healed sufficiently for reharvesting or once autologous cultured skin is available for permanent wound closure.
Box 13.3
Advantages of Fresh Allograft Skin
-
■
Rapidity and strength of adherence to the wound
-
■
Control of microbial growth
-
■
Rapidity of revascularization
-
■
Reproducible clinical results
Although fresh allografts provide these essential advantages and are the ideal material, their use has become extremely limited in recent years due to increased FDA regulations put in place to reduce risk of disease transmission. When fresh allograft is not available, cryopreserved skin is an excellent alternative for temporary wound coverage. Although frozen cryopreserved skin generally has less measurable viability than fresh skin, it is currently difficult to maintain continuous and ample stores of fresh skin beyond 14 days. It has therefore been standard skin banking practice to cryopreserve allograft skin within 7 and 10 days of recovery if it is not planned to be used within the time period that viability can be maintained. Fig. 13.2 depicts the quantitative use of allograft skin and amnion in thermally injured children treated at Shriners Children’s Texas in Galveston since 2012.
Allograft and amnion skin usage at Shriners Children’s Texas in Galveston.
Coverage of widely meshed skin autografts and partial-thickness wounds
Another use of allograft skin has been to apply it as an overlay on top of widely expanded, meshed autologous skin graft ( Fig. 13.3 ). This technique was originally described using meshed allograft and provides immediate closure that can be both temporary and permanent. Our institution uses 2:1 meshed cadaver skin for the coverage of widely expanded autografts (with a ratio greater than 2:1). Because it is usually less viable than fresh skin, it functions more as a biologic dressing than as a temporary skin replacement. Its adherence to the underlying wound bed results in pain relief, limitation of exudative and water loss, and reduces the need for frequent dressing changes. As the underlying wound bed reepithelializes, the allograft slowly separates without disturbing the delicate underlying epithelium. These properties of frozen allograft are also used in the coverage of partial-thickness wounds. Studies by Rose and Naoum demonstrated more rapid healing times and shorter hospital stays for children with extensive partial-thickness burns when treated with early wound debridement and allografting compared with conventional topical antimicrobial therapy.
Diagrammatic illustration of meshed allograft overlay technique (as described by Alexander et al.). The allograft is generally meshed 1.5:1 or 2:1, whereas the underlying autograft may be meshed 3:1 or greater.
(From Alexander JW, MacMillan BG, Law E, et al. Treatment of severe burns with widely meshed skin autograft and widely meshed skin allograft overlay. J Trauma. 1981;21:433-438.)
There has also been some concern that allografts may induce an inflammatory rejection response resulting in delayed reepithelialization of underlying autografts. Therefore the use of lyophilized tissue has been suggested because the lyophilization process destroys cellular components and results in a diminished immunologic response from the graft recipient. , A 2013 study of 11 patients treated with lyophilized allograft showed no evidence of immunologic reactions due to the administration of allograft.
Potential disadvantages of allograft use
Infection
Allograft skin has the potential to transmit bacterial infection. It is therefore imperative that skin banks perform microbial cultures before releasing the tissue for transplantation. In fact, the AATB Standards require that skin be discarded if pathogenic bacteria or fungi are present. This is particularly important given the immunocompromised status of the intended recipient and the potential for developing wound sepsis after exposure to contaminated materials.
There have also been reports of viral disease transmission by skin allografts. In 1987, Clarke reported what was thought to be the transmission of HIV-1 to a burn patient from an HIV-positive donor ; however, the results of donor testing were not known before skin use. Moreover, the recipient, who had a number of risk factors for HIV, had not been tested before receiving the allograft. Therefore they were not able to ascertain whether their posttransplant HIV-positive status was present before the application of their allograft. To date, there have been no other reported cases of HIV or hepatitis transmission from skin allografts.
Kealey reported the transmission of cytomegalovirus (CMV) from cadaver skin allografts. Because nearly 23% of the CMV-negative patients seroconverted, they recommended the use of CMV-negative allograft skin for seronegative burn patients. They reasoned that although tissue from seronegative donors would be ideal for use in seronegative patients, such a practice would significantly limit the availability of fresh allograft skin for most thermally injured patients. In addition, whereas there is good evidence to support the transmission of CMV by allograft in burn patients, there is little evidence that CMV seroconversion is clinically significant or affects outcomes in thermally injured patients.
Furthermore, Herndon and Rose reiterated that the benefits of using cadaver allograft skin for the treatment of burn patients clearly outweigh the small risks associated with CMV seroconversion. At present, most burn surgeons and skin banks recommend that the decision regarding the use of allograft skin from CMV-positive donors should be made by the burn/transplanting surgeon.
Rejection
Although demonstrating many characteristics of an ideal wound covering, allograft skin contains Langerhans cells that express class II antigens on their surface. These cells reside in the epidermis of the skin and are ultimately rejected by the recipient as the result of an immunologic rejection response. This typically results in an acute inflammatory reaction and can lead to wound infection. Vascularized allogeneic skin grafts typically remain intact on the wound of a burn patient for 2 to 3 weeks, although there have been reports of allograft skin survival for up to 67 days due to the inherent immunosuppression of extensive burn injury. Recent improvements in nutrition, critical care management, and a more aggressive surgical approach to definitive wound closure, however, have now made the persistence of allografts less predictable.
Efforts to prevent rejection have included methods that might reduce antigen expression by controlling the activity of the Langerhans cells in the allograft skin. Treatment of the allografts with ultraviolet light irradiation and incubation of the skin in glucocorticoids have been reported to result in a modest prolongation of allograft survival compared with nontreated skin; however, the utility of this methodology has not been substantiated. Other investigators have studied the effects of pharmacologic agents to induce immunosuppression in patients with major burn injuries. Initial clinical trials reported an improvement in both allograft and patient survival when children were treated with azathioprine and antithymocyte globulin ; however this regimen was associated with azathioprine-induced neutropenia, and the clinical outcomes were not corroborated by others. More recently, the use of cyclosporin A was demonstrated to prolong skin allograft survival in patients with extensive full-thickness burns. , In these studies, allograft rejection was generally observed within a few days of discontinuing treatment; however, there were instances where engraftment persisted after the completion of therapy. Further studies of these and newer immunosuppressive agents may be warranted.
Technical aspects of skin banking
Donor screening
It is vitally important that complete and accurate medical information about the potential tissue donor be obtained to ensure the safety of the tissue for transplantation. The AATB and the FDA require a comprehensive medical and social history of the donor. , For this purpose, the AATB developed a Donor Risk Assessment Interview (DRAI) in cooperation with the FDA and other organ and tissue recovery organizations.
A panel of serologic screening tests for transmissible diseases is required. These include:
-
■
Antibodies to human immunodeficiency virus, types 1 and 2 (anti-HIV-1 and anti-HIV-2)
-
■
Nucleic acid test (NAT) for HIV-1
-
■
Hepatitis B surface antigen
-
■
Total antibodies to hepatitis core antigen (including both IgG and IgM)
-
■
Antibodies to hepatitis C virus (anti-HCV)
-
■
NAT for HCV
-
■
Syphilis (a nontreponemal or treponemal-specific assay may be performed)
-
■
NAT for the hepatitis B virus (HBV)
Test kits should be FDA licensed, approved, or cleared for donor screening and, ideally, should be approved for cadaveric specimens. Barnett et al. reported their 2-year experience with cadaveric skin donor discards due to positive serologic tests. In that report, they noted that 61 of 813 donors (7.5%) required tissue discard due to positive serologic tests. A positive hepatitis B core antibody test accounted for 52.3% of the serology-based discards, whereas hepatitis B surface antigen testing accounted for 18.1%, and hepatitis C, HIV-1/2, HTLV-1, and syphilis tests accounted for 14.3%, 4.9%, 4.9%, and 5.5%, respectively.
Skin recovery
Once donor screening is complete and proper authorization has been obtained, the recovery team must arrange the time and location for skin recovery in an appropriate facility (i.e., hospital morgue or operating room, medical examiner’s office, or the tissue bank). It is extremely important that the time of death and body storage conditions be accurately documented because these have a significant bearing on skin viability and microbial contamination, as can the time from skin recovery to banking. Current AATB Standards require that skin prep begin within 24 hours of asystole, provided the donor’s body was cooled (e.g., application of sufficient amounts of wet ice or a cooling blanket, cold weather conditions) or refrigerated within 12 hours of asystole. The skin prep must begin within 15 hours of death if the deceased donor’s body has not been cooled or refrigerated. If the donor’s body is cooled for a period of time, then not cooled for a period of time, the time period the donor’s body is not cooled cannot exceed 15 cumulative hours.
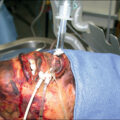
In brief, the skin is recovered under aseptic conditions. However, first a thorough physical assessment is necessary to determine if the donor should be deferred for other medical reasons and allows determining the quality of the skin and technical feasibility of skin recovery by evaluating the donor’s size and skin condition. Box 13.4 lists disease states that are commonly associated with deferral of a potential skin donor. Blood samples are also obtained for the required infectious disease testing. The areas from which the skin is taken are shaved of hair and cleansed with an antimicrobial agent approved for use in operative procedures (i.e., povidone-iodine, chlorhexidine). The tissue-recovery technician wears the appropriate personal protective equipment (i.e., surgical cap, mask with face shield, shoe covers), performs a surgical scrub, and dons a sterile gown and gloves while the circulating technician completes the required documentation of the tissue recovery and prepares the tissue and transport containers. This is generally followed by a chlorhexidine prep surgical scrub of the tissue donor, rinsing with 70% isopropyl alcohol after the required contact time of the surgical scrub and allowing the skin surface to dry. A back table with all the required supplies for skin recovery is set up, and the donor is then surgically draped. Split-thickness skin grafts are then removed using a dermatome at a thickness of 0.012 to 0.018 inch. The width of the grafts generally should range from 3 to 4 inches, but ideally should be determined by the preference of the transplanting surgeon(s). Skin retrieval sites are usually limited to the torso, hips, thighs, and upper calves. The amount of skin obtained may vary depending on body habitus, skin defects or lesions, and body geometry; however, an average yield of 4 to 6 square feet per donor is not unusual for an experienced tissue-recovery technician. After tissue is obtained from the posterior surfaces, the donor is turned to expose the anterior surface, prepped again, and draped before completing the recovery process. The skin is then placed in tissue culture medium and maintained at wet ice temperatures (above freezing to −10°C) during transport to the skin bank for processing.
Box 13.4
Disease States Commonly Associated With Potential Skin Donor Deferral
-
■
Extensive dermatitis
-
■
Acute burn injuries
-
■
Cutaneous malignancy
-
■
Poor skin quality
-
■
Extensive tattoos
-
■
Collagen vascular disease
-
■
Toxic chemical exposure
-
■
Skin infections
-
■
Extensive skin lesions
-
■
Extensive skin or soft-tissue trauma
Skin processing
Processing environment
Skin should be processed under aseptic conditions in a bacteriologically and climate-controlled environment ( Fig. 13.4 ). Although current AATB Standards mandate the processing of cardiovascular tissues in a class 100 laminar flow environment, no such requirement exists for human skin banking.
Aseptic tissue processing environment.
Microbiologic testing
After returning to the skin bank, the tissue-recovery team should obtain cultures for aerobic and anaerobic bacteria, yeast, and fungi. Tissue cultures can be obtained by swabbing, destructive testing of companion tissue, or by fluid elution. Cultures from representative anatomical areas shall be obtained before processing. Culture methods shall be validated to ensure the suitability of the culture method selected. Inhibitory substances (e.g., skin prep solution(s), transport media, antibiotics) that may be added to unprocessed skin during recovery or for transport must not interfere with culture results (i.e., produce false-negative results). Testing should be conducted in accordance with adherence to relevant standards (e.g., College of American Pathologists (CAP), International Organization for Standardization (ISO), American Society for Testing and Materials (ASTM), Association for the Advancement of Medical Instrumentation (AAMI), United States Pharmacopeia (USP)), and the skin should not be used for transplantation if it contains any of the following microorganisms:
-
■
Staphylococcus aureus
-
■
Group A β-hemolytic streptococci
-
■
Enterococcus spp.
-
■
Gram-negative bacilli
-
■
Clostridium spp.
-
■
Fungi (yeasts or molds)
Whereas AATB Standards require that microbiology culture results should not be reported before 7 days of incubation before releasing the tissues for transplantation, when fresh, noncryopreserved allograft skin is used for transplantation within days of tissue recovery, the results of the microbial cultures are frequently unavailable.
These findings were substantiated by Britton-Byrd et al. in their review of tissue donors whose skin was used after only 3 days of incubation. They reported three cases resulting in tissue recall due to positive microbiological cultures and concluded that 3-day culture results do not result in significant microbiologic contamination of allograft skin. White et al. have suggested that cadaver allograft containing less than 10 3 organisms per gram of tissue can be safely used for temporary wound coverage. Despite the results of these studies, it is strongly recommended that the tissue bank communicate all available information regarding donor and tissue suitability to the transplanting surgeon so that they can adequately assess the potential risks and benefits for each individual recipient.
Maintenance of viability
Maintenance of cell viability and structural integrity are vital for the engraftment and neovascularization of allograft skin. Yet, there have been no studies that have quantified the degree of viability necessary to ensure allograft take. Postmortem time lapse appears to have the single greatest effect on skin viability, as May demonstrated when the functional metabolic activity of the skin rapidly declined if the donor was not refrigerated within 18 hours of death. , The ideal nutrient tissue culture medium also has not yet been identified. Eagle’s MEM and RPMI-1640 continue to be generally accepted.
To date, it remains unclear which cryoprotectants offer the greatest preservation of cell viability and structural integrity. Glycerol (10%–20%) and dimethylsulfoxide (10%–15%) have been reported to maintain skin viability after incubation times ranging from 30 minutes to 2 hours; however, the optimal concentrations of these cryoprotectants have not been identified, nor have these agents been compared for efficacy. Last, factors such as age and sex do not appear to influence skin viability.
Refrigeration
Refrigeration slows the metabolic rate of the viable cells, and nutrient tissue culture medium supports cellular metabolic activity. “Fresh” allograft skin is typically stored at 4°C in tissue culture medium with or without antibiotics. The skin should be free-floating in a sterile container with approximately 300 mL of medium per square foot of skin. Recent studies suggest that skin viability can be maintained for up to 2 weeks at 4°C if the nutrient medium is changed every 3 days.
It has been common practice to cryopreserve the skin within 10 days of tissue recovery. This has been based on the work of May et al., who demonstrated that glucose metabolism declined at a rate of 10%–15% each day during refrigerated storage.