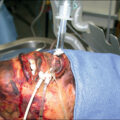
Introduction
Severe burn injury causes myriad hematologic perturbations. Burn excision and substantial in-hospital phlebotomy cause severe blood loss anemia and even hemorrhagic shock, requiring substantial transfusion. Large-scale fluid resuscitation and shock cause a significant coagulopathy. Surgical extirpation can similarly cause a significant dilutional coagulopathy requiring transfusion. Hematopoiesis, the generation of new blood cells, is directed away from red blood cell (RBC) production toward myeloid blood cell production by the hyperinflammatory cytokine cascade. The hyperinflammatory nature of burn injury further makes the patient hypercoagulable, generally requiring anticoagulation or thromboprophylactic therapy. Providing total burn care requires knowledge of hematology, hemostasis, thromboprophylaxis, and transfusion medicine to overcome the substantial pathophysiology experienced by these patients.
Etiology of anemia in burn patients
Anemia is the condition occurring when the RBC concentration, or hemoglobin (Hb) concentration, falls below normal laboratory limits for healthy adults. These normative values do not correlate with sufficient oxygen delivery, which is also influenced by pH and 2,3-bisphosphoglycerate concentration. Weiskopf and Feiner classically demonstrated normal oxygen delivery despite dramatic acute anemias while examining Hb concentrations as low as 5 g/dL in euvolemic subjects. Anemia is common in burn patients, especially in those with severe thermal injuries. Burn patients suffer from anemia due to surgical blood loss and the anemia of critical illness. This can occur in patients with as little as 10% total body surface area (TBSA) burned. A mild reduction of RBC mass is of little clinical significance ; when the concentration is markedly reduced, and as the total blood volume loss continues beyond 15%, the advanced trauma life support stages of hemorrhagic shock predictably appear, signaling impaired end-organ perfusion and oxygenation. The initial 2 weeks postburn feature anemia mainly resulting from blood loss from destruction through the burn wound, dilution due to resuscitation, and surgical blood loss from repeated debridement to prepare the wound bed with well-vascularized tissue. Subsequently, anemia is characterized as the anemia of critical illness and develops from inadequate nutrition, , stunted erythropoiesis, or phlebotomy and dressing changes. Specifically, bone marrow dysfunction leading to dampened erythropoiesis has been explored in autopsy studies and in the mouse model of burn injury in vitro. In an autopsy study of patients who died from myocardial infarction, sepsis, or burns, the bone marrow of burn patients contained significantly fewer erythroblasts compared with the other groups; the associated anemia is typically erythropoietin (EPO) resistant.
Burn excision results in blood loss according to the size (percent TBSA) of the excised area and the age of the burn wound. The latter is a determinant of blood flow in the burned and excised area. During major burn excisions, there is commonly major blood loss often requiring massive transfusions (MTs). MT is defined as the transfusion of packed red blood cells (pRBCs) of 10 units or more within 24 hours of admission. Whereas acute surgical blood loss is obvious and prominent during the treatment phase, burn patients suffer a prolonged anemia of critical illness during their recoveries that is insidious. The anemia of critical illness is the inability of RBC production to meet RBC demand and losses during critical illness. , More than 50% of transfusions during a burn patient’s hospital course may be caused by the anemia of critical illness. It has been equated to an acute form of the anemia of chronic disease and anemia of inflammation in conjunction with nutritional deficiencies. , This anemia of critical illness can promote and also be exacerbated by superimposed kidney injury. Acute blood loss anemia is controlled with surgical technique, whereas the anemia of critical illness can be restrained with reduced phlebotomy, decreased blood loss with dressing changes, improved nutrition, and resolving the critical illness by covering the patient with skin, thereby abating the disease. Prevention of anemia is accomplished through alteration of its sources, whereas the mainstay of treatment for both types of anemia is the transfusion of pRBCs.
Hemostasis in burn patients
Controlling blood loss and hemorrhage during burn care is important to prevent episodes of hemorrhagic shock and limit total transfusion need. Although Barbosa and Rowell demonstrated that a 6-hour RBC transfusion requirement is one of the mortality predictors in MT trauma patients, it is unclear if these findings extend to controlled blood loss during a burn extirpation. In these cases, a skilled anesthesiologist can match the transfusion rate and blood product mix to the bleeding rate, thus preventing hemorrhagic shock, maintaining euvolemia, and avoiding coagulopathy while the surgeon removes burned and diseased tissue and engrafts the patient.
As with burn-susceptible infections, preventing burn-associated anemia from developing is preferable to treating the anemia or subsequent sequelae. Multiple adjuncts and methods have been established to mitigate acute surgical blood loss, including epinephrine tumescence, elevation, compression, thrombin-soaked dressings, pharmacologic adjuncts, and tourniquet use. Additionally, excision with electrocautery at a fascial or subcutaneous level can limit blood loss significantly in large, deep, and/or invasively infected burns. Regardless of the excision methodology employed, multiple studies show that the injection of dilute epinephrine into the subdermal space promotes vasoconstriction and reduces blood loss during surgical management of the wound. In a pediatric trial, epinephrine tumescence alone decreased blood loss from 3.5% to 5% to 0.98% of total blood volume per percent of body excised and grafted. Importantly, sufficient time must be allotted for the epinephrine to take effect, with an ideal interval of 25 minutes. Properly performed epinephrine tumescence has no significant hemodynamic consequences, nor does it alter wound healing. A recent study confirmed that subcutaneous epinephrine injection had no adverse effect on perfusion, pain, or scar quality versus the saline-administered control group. Of interest lately has been tumescent infiltration of lidocaine and epinephrine by clysis. Gumus showed that this technique resulted in more facile excision with diminished blood loss. Similarly, clysis has been demonstrated to reduce the need for blood transfusions. The use of thrombin-soaked pads for additional hemostasis support postoperatively has been studied in the context of epinephrine tumescence and provides supplementary hemostasis by reducing unnecessary ooze from the dressing site. , New silicone gel dressings also significantly reduced the amount of blood loss per percent excised and the amount of blood transfused. , We employ nonadherent dressings (Telfa) soaked with epinephrine intraoperatively. This facilitates hemostasis and does not restart the bleeding upon removal of the pads, as often occurs with epinephrine-soaked laparotomy pads that avulse the nascent clots they helped induce on the wound surface when they are removed. Finally, the use of extremity tourniquets during excision and debridement can decrease acute surgical blood loss without compromising graft adherence. , Kragh et al. found tourniquet use efficacious in both adults and children. In combination, all three techniques (epinephrine tumescence, thrombin-soaked dressings, and tourniquet use) can reduce intraoperative transfusion from 3.3 to 0.1 unit per operative case with 96% graft take and total units transfused from 15.7 to 7.9 per patient. However, recent analysis indicates that using the epinephrine-tumescent technique may somewhat obviate the need for tourniquets. Of note, administration of topical bovine thrombin is avoided in burn patients with prior exposure because they have been shown to develop coagulation derangements and severe bleeding complications from an acquired factor V deficiency. Mullins et al. reported safe and effective hemostasis through recombinant human thrombin applied as a spray. Due to rampant overestimations of operative transfusion needs and the expenses incurred by blood typing and cross-matching, a preoperative estimate of 1.78 units of pRBCs per 1000 cm 2 of burn wound excised best utilizes blood bank resources.
Coagulopathy in burn patients
In addition to anemia, thermal injuries are associated with systemic coagulopathy, and the hemostatic changes seen in patients with severe burns appear similar to those in patients with other major traumas. The severity of the burn correlates with the extent of hemostatic changes , ; typically only severely burned patients (≥30% TBSA) develop extensive coagulopathy. However, no consensus currently exists on the definition of coagulopathy in burn injuries. Despite being documented since the 1970s, the physiology of coagulopathy in burns is still ill-defined. However, coagulopathy of thermal trauma does present with characteristics common to sepsis-induced coagulopathy: decreased levels of antithrombin and other native anticoagulants, elevated levels of activated factor VII, fibrinogen degradation products, plasminogen activator inhibitor-1 (PAI-1), and thrombin-antithrombin complex (TAT). The three types often discussed in burn- and trauma-related literature are trauma-induced coagulopathy (TIC), disseminated intravascular coagulation (DIC), and acute traumatic coagulopathy (ATC). Acute coagulopathy of trauma shock has largely been subsumed under TIC. Caused by trauma, TIC is characterized by coagulation activation, hyperfibrinolysis, and consumption coagulation. The main pathophysiology of TIC is DIC. , , Specifically DIC presents as the fibrinolytic phenotype in the early, acute phase of trauma and burn, , , , whereas the thrombolytic phenotype is associated with sepsis-induced DIC, which typically presents later in the clinical course of burn pathophysiology. As defined by the Scientific and Standardization Committee of the International Society on Thrombosis and Hemostasis, DIC is an acquired syndrome characterized by the intravascular activation of coagulation with loss of localization originating from and causing damage to the microvasculature, potentially leading to multisystem organ dysfunction (MOD). , DIC is characterized not by the significant bleeding, transfusion requirements, and fourfold higher mortality associated with TIC, , but also by excessive thrombosis, unchecked inflammation and MOD, insufficient anticoagulation mechanisms, and increased fibrinolysis. Indeed, early coagulopathy is associated with increased incidence of ventilator-associated events among burn patients. MTs are administered more frequently in patients with DIC. ATC is associated with the depletion of fibrinogen, platelet dysfunction, and activation of protein C. This particular coagulopathy is not secondary to other conditions, such as hypothermia, and markers for it can be discerned within 30 minutes of the inciting thermal event. , In the pediatric population, ATC is defined by an international normalized ratio (INR) of 1.3 or greater, and those who present with fibrinolytic shutdown are more likely to develop deep vein thrombosis (DVT). Exacerbating this, prophylactic anticoagulant administration is not recommended by some in the pediatric population due to their lower rates of venous thromboembolism (VTE). Coagulopathy seen in burns is conditioned by preexisting conditions (e.g., age and comorbidities), as well as environmental (e.g., ambient temperature) and therapeutic factors (e.g., prehospital fluid administration).
As demonstrated in multiple studies, the timing and onset of coagulopathy correspond with the severity of the burn, , , , and TIC may present without initial hypercoagulopathy. Few burn patients present with coagulopathy at admission, but a large number develop it within a day postburn. In fact, at admission, no statistically significant differences were observed between nonsurvivors and survivors in coagulation and fibrinolysis markers. Inciting causes of coagulopathy in burned patients include tissue hypoperfusion from fluid resuscitation, systemic inflammatory response syndrome (SIRS), blood loss from surgical excision, hypothermia, endothelial damage, consumption and/or dilution of coagulation factors, and acidemia. Tejiram et al. effectively reviewed the myriad changes seen in the clotting dynamics of burn patients and related more subtle factor changes as possible markers of mortality than partial thromboplastin time (PTT) and INR, which were normal in their cohort. Classically, hypothermia, acidosis, and coagulopathy are collectively known as the lethal triad, , , corresponding to MTs and mortality in burn and trauma patients.
Prevention of hypothermia in the operative theater is completely within the purview of the operative team and the operating room in the same way that the temperature of a steak is completely within the purview of the chef and the oven. As a manifestation of the first law of thermodynamics, a patient cannot cool beyond the temperature of the operating room. The clinical practice guideline in many burn centers is to maintain the ambient temperature of the intensive care unit (ICU) and operating rooms at 30°C to 40°C as a component of standard of care in the treatment of burn patients. , Maintaining sufficient heat in the operating room to prevent hypothermia is essential. In patients undergoing surgery, inadvertent perioperative hypothermia resulted from 50% to 90% of the cases. Singer et al. determined hypothermia to be associated with high mortality, although it was much more commonly found in patients with large burns. , In fact, it has been shown that hypothermia, the condition where the core temperature falls below 36°C (96.8°F), is not associated with external factors at the time of the burn but correlates to burn severity and patient physiologic status. Burn patients are most vulnerable during excisional surgery due to operative heat loss concurrent with evaporative water loss or massive fluid therapy. , ,
Acidosis is an ever-present threat for the recovering burn patient. Lactic acidosis from shock states occurs transiently during recovery and surgery and exacerbates bleeding, as does hypercarbia. Uremia causes an anion gap acidosis and reduces platelet aggregation, which can be reversed with desmopressin. Hyperchloremia of normal saline administration is an effect of hemodilution or a decrease in renal excretion of H + . Whereas administration of natural saline is associated with hyperchloremia-induced metabolic acidosis, lactated Ringer’s solution, the other crystalloid solution typically used, correlates with metabolic alkalosis.
Diagnosis of coagulopathy depends on detection. The INR measured upon admission is the basis for the diagnosis of ATC. , Initial Hb levels may mask bleeding, and repeated measurements are necessary to use Hb levels diagnostically as a marker for bleeding. Notably, low initial Hb is considered an indicator for hemorrhage-associated coagulopathy. However, assessing specific coagulation markers has proved both time-consuming and expensive, and typical laboratory tests, such as PTT, are limited in diagnostic value. , , The markers of the various coagulopathies seen in burns present similarly to the coagulopathy seen in patients with sepsis and severe trauma. , , Among the coagulopathic changes are increased levels of markers of thrombin activation, activated factor VII (FVIIa), TAT, and inhibited fibrinolysis with increased levels of PAI-1, as well as decreased levels in proteins C and S, fibrinogen, and antithrombin. , In the first day postburn, patients with severe burns show marked decreases in fibrinolysis, , , as well as platelet activity. Lavrentieva et al. demonstrated that, in the early postburn phase (days 3–7 postburn), survivors could be distinguished from nonsurvivors by the levels of natural coagulation inhibitors (i.e., proteins C and S and antithrombin), fibrinolytic factors (i.e., PAI-1 and tissue-plasminogen activator), and TAT, a marker of thrombin generation, but not at admission when both groups presented with statistically similar levels in all parameters. Although van Haren et al. also found that severely burned patients become hypercoagulable after admission despite pharmacologic thromboprophylaxis, they determined that thromboelastography (TEG) was a more reliable indicator of coagulopathy than were coagulation markers. Interpretation of TEG data is reviewed in Fig. 18.1 . Furthermore, TEG provides diagnostic answers in a much shorter time than standard laboratory testing, resulting in faster goal-directed therapies. , The majority of burn centers worldwide use standard coagulation tests, but the move to using TEG is warranted. With the advent of a portable fibrinogen analyzer, fibrinogen levels can be measured in mere minutes. Low levels of fibrinogen have been shown to be predictors for MTs ; Hayakawa et al. demonstrated that fibrinogen reached critical diagnostic levels (150 mg/dL) sooner than other coagulation parameters, making it a key factor in determining blood product needs as well as being a coagulation indicator. More recently, other studies showed higher levels of fibrinogen (211 mg/dL and 190 mg/dL) functioned as useful predictors of MT. ,
Panel 1 depicts the thromboelastography (TEG) device, in which a cuvette of whole sample blood is incubated with a pin and torsion wire rotates within the sample. The tracing depicted in Panel 2 reflects the force required to spin the pin over time as the fibrin strands form a clot that resists pin movement. Reaction time (R) in minutes reflects the latency time to initial fibrin formation. Elevations are typically treated with fresh frozen plasma or reversal of anticoagulants, which delay initiation of clot formation. Kinetics (K) is the time taken to achieve a clot strength of 20 mm. α is the angle between R and K and measures the speed of fibrin buildup and cross-linking, which reflects the availability of fibrinogen; defects are typically treated with cryoprecipitate. Time to maximum amplitude (MA) is another measure of speed to fibrin buildup. MA represents the ultimate strength of the fibrin clot and overall stability and is a measure of platelet action and stabilization of the clot. Deficits in MA are typically treated with platelets or ddAVP to augment platelet aggregation. FPL, A30, or LY30 reflect the amplitude of the clot strength at 30 minutes as a measurement of fibrinolysis. Fibrinolytic patterns are treated with tranexamic acid typically. (A) Normal TEG tracing. (B) Low clotting factor availability causing a decreased α-angle. (C) Various pathological hemorrhagic TEG tracings. (D) Fibrinolytic TEG tracings. (E) Various thrombotic TEG tracings.
(From Mauffrey C, Cuellar DO III, Pieracci F, et al. Strategies for the management of haemorrhage following pelvic fractures and associated trauma-induced coagulopathy. Bone Joint J . 2014; 96–B(9):1143-1154.)
Not only is there limited consensus on the diagnosis of the type of coagulation dysfunction associated with burns, there is no agreement on the therapies used to respond to the condition when it presents. It is accepted that the activation of fibrinolysis is inadequate to offset the excessive fibrinogen formation in the early postburn phase in patients severely burned. Hemostasis depends on fibrinogen for clot formation and platelet aggregation, and the depletion of fibrinogen correlates with poor outcomes. Although fibrinogen is the coagulation protein with the highest plasma concentration, plasma transfusions do not correct the fibrinogen depletion seen in TIC and ATC unless massive volumes are infused. Current European Trauma Guidelines suggest the administration of fibrinogen concentrate or cryoprecipitate if a trauma patient presents with both significant bleeding and thromboelastometric signs of functional fibrinogen deficit or a fibrinogen concentration (FIB) of less than 1.5 to 2 g/L. Topical hemostatic agents such as thrombin spray rely on plasma FIB to effect hemostasis in operative wounds.
Limiting fibrinolysis is another important method to control blood loss during burn excisions. Tranexamic acid (TXA), a synthetic derivative of lysine, has found utility in treating burn patients. In the landmark CRASH2 randomized controlled trial, Roberts et al. demonstrated a reduction of blood loss and mortality with TXA use in trauma patients. Not only does TXA safely and significantly reduce the mortality rates of trauma patients with, or at risk of, substantial bleeding when administered early in the course of treatment, but its de minimis side effect profile in conjunction with its low cost and ease of use have made it an integral component of resuscitation protocols worldwide. However, the benefits of TXA are seen only when administered within 3 hours of injury; after that window, it has been shown to increase mortality. , Thus it is most efficacious to treat ATC. Fibrinolysis is less likely to be fully activated the sooner patients receive TXA; fibrinolysis continues unceasingly once activated, and only restoration of endogenous antifibrinolytic elements can abate the activity. Some practitioners feel that the potential risk is too great for use in patients whose bleeding is not life threatening. Although reports exist highlighting the prothrombotic effects resulting from each antifibrinolytic drug, we advocate the use of TXA perioperatively for large burn excisions. ,
Transfusion of blood cells
Burn patients have many disparate indications for transfusion. In the setting of active operative hemorrhage, the rapid transfusion of pRBC, plasma, and other products is essential to prevent hemorrhagic shock. In the postoperative period, transfusion is necessary to treat blood loss anemia, coagulopathies, and consumptive thrombocytopenias. As a component of resuscitation, plasma transfusion is often required to treat coagulopathies resulting from consumption and underproduction of factors, as well as for volume expansion, as discussed in Chapter 7 on the pathophysiology of burn shock and burn edema and in Chapter 9 on fluid resuscitation and early management. Understanding the vastly disparate indications for transfusion in burn patients allows clarity in the urgency and aggressiveness of transfusion used in these patients with ever-changing status.
The first major indication for transfusion is intraoperative blood loss during burn wound excision. The anesthesia team must monitor overall preload while estimating blood loss to prevent hypovolemia and hemorrhagic shock. Surgical control of hemorrhage is critical, but large blood loss is expected, especially in the setting of large burns. Surgical blood loss has been estimated and measured in a variety of ways, , but reports based on surgical and anesthesia team estimates are simple and reliable. Following serial hematocrit value along with hemodynamic markers is a standard method of monitoring blood loss and transfusion success. Various formulae have been developed to calculate the estimated blood loss. Total blood volume is estimated using the patient’s weight, preoperative and postoperative Hb, and presumed normal adult Hb of 70 mL/kg. Generally accepted and employed constants are adult males, 75 mL/kg; adult females, 65 mL/kg; infants (babies less than a year), 80 mL/kg; term infants (39 week gestation), 85 mL/kg; and premature neonates, 95 mL/kg. Gross initially described the mathematics of the formula in 1983 ; we have derived an equation estimating allowable operative blood loss with which we estimate blood loss for all our operations. Fig. 18.2 reflects the formula we use, and, although patient conditions, such as venous capacitance and changes in vascular tone, can significantly alter blood volume of distribution, this formula has proved the best estimator of blood loss in our experience.
An algebraic formula to estimate surgical blood loss. In the first group of terms, labeled A, the patient’s weight is multiplied by the expected blood volume for age: adult males 75 mL/kg, adult females 65 mL/kg, infants 80 mL/kg, term infants 85 mL/kg, and premature neonates 95 mL/kg. The second portion of the equation uses preoperative and postoperative hemocrit (H ct ) to derive the fraction of blood lost to account for the observed change in H ct . Finally, blood transfused is added in to account for intraoperative transfusion effects.
Because of blood type and cross-match expenses and overestimation of operative transfusion needs, a preoperative estimate of 1.78 units of pRBCs per 1000 cm 2 of burn wound excised best utilizes blood bank resources. However, even since publication of the previous edition of this book, studies show 25% of patients received cross-match orders exceeding national guidelines, with surgeons being most responsible for this overestimation. Interestingly, change in hematocrit, not Hb, is considered the most reliable indicator for continuing blood loss, and, at admission, is the best predictor of 24-hour blood product requirements, as well as being associated with signs of shock and hemorrhage in trauma patients, both adult and pediatric. Additionally multiple studies have found massive blood transfusion in trauma, surgery, and critical care to be a predictor of SIRS, multiple organ failure, and increased infection and mortality, although it is unclear if the need for significant transfusion is a marker for disease severity rather than the transfusion itself being the etiologic cause.
In the setting of active operative hemorrhage, transfusion rates should match the rate of blood loss. Estimation of ongoing rates of bleeding and matching transfusion rates requires careful coordination between the anesthesia and operative teams. MT protocols have been demonstrably lifesaving in these cases. In the setting of operative hemorrhage, the standard transfusion ratio is 1 unit pRBC to 1 unit fresh frozen plasma (FFP). Electrolytes must be monitored to prevent hypocalcemia instigated by the citrate anticoagulant in the blood products. As was demonstrated in the PROPPR study, major trauma centers were unable to deliver adequate amounts of thawed plasma for MT sufficiently quickly, so a burn team anticipating significant blood loss intraoperatively is well advised to order appropriate amounts of blood products before initiating the surgery. With modern rapid infusers, such as the Belmont, capable of transfusing warmed, mixed blood products at rates of 500 mL/min, there is little reason for insufficient transfusion rates during a burn extirpation.
In the ICU, blood transfusions are typically unnecessary to treat or prevent hemorrhagic shock; rather, they are warranted for less emergent indications, such as blood loss anemia, coagulopathy, or volume expansion. Traditionally, a defined Hb trigger of 10 g/dL or hematocrit of 30%—the “10-and-30” rule—has guided transfusion practices. These triggers continue in many centers worldwide. However large-scale works in critical care literature and smaller, retrospective reviews of adult and pediatric burn patients have established the benefits of a lower, more restrictive transfusion triggers, indicating that some patients had been receiving blood to no benefit. The Society of Critical Care Medicine addressed transfusions in the intensive care setting. For critically ill patients, a restrictive strategy was found as efficacious as the conventional liberal one, so in patients with evidence of hemorrhagic shock, hemodynamic instability, or acute bleeding, an Hb trigger of less than 7 g/dL indicates for transfusion, and this should be given as single units in the absence of acute bleeding. , Recent research supports the theory that pRBC transfusions should not rely on the use of standardized triggers, but rather be tailored to the burn patient’s blood volume status, acuity of blood loss, and perfusion requirements. ,
Transfusion needs increase with burn size, , , , as do complications. Each 1% increase in TBSA of burn has a corresponding 6% increase in mortality risk. In a large study of transfusion trends in burn patients, those with 20% or greater TBSA required 13.7 ± 1.1 units, whereas those with 50% or greater TBSA required more than 30 units of pRBCs. Burn patients often receive multiple transfusions; in one study, more than half the transfusions resulted from anemia of critical illness (nonsurgical). Although pRBC transfusion rapidly and reliably corrects anemia, it is associated with many of the consequences of bloodborne transmission, including hepatitis B, hepatitis C, and HIV. Whereas the infectious transmission rate has significantly decreased with improved screening methods, , it is markedly higher in low- and middle-income countries than in high-income countries like the United States (0.1% and 0.003%, respectively). More importantly, pRBC transfusion is associated with immunomodulation, including increased infectious morbidity, with a 13% increase in risk of developing an infection per unit of blood transfused. Muszynski et al. nicely reviewed the extensive hyperinflammatory and severe immunosuppressive effects of blood transfusions and related these data to critical care outcomes.
Other significant consequences include transfusion-related acute lung injury (TRALI), which is difficult to diagnose in burn patients because simultaneous lung injury from resuscitation or inhalation injury may contribute to TRALI diagnostic criteria, and ABO incompatibility, which can be rapidly fatal. Implementation of restrictive-transfusion strategies in which pRBCs are transfused only for hemodynamic instability or at lower Hb concentrations has reduced overall transfusion and infection rates, benefitting both cost and survival. , , FFP transfusion is also associated with TRALI in burn patients, and early transfusion of FFP correlates with increased incidence of other deleterious effects postburn. However, by not administering plasma from females with a history of pregnancy, the risk of TRALI from FFP is significantly mitigated, and using pathogen-inactivated plasma reduces the risk of transmitting infectious diseases. The indicators for increased transfusions of FFP and pRBC were high TBSA and use of argatroban anticoagulation.
Except in the setting where MTs are indicated, greater ratios of FFP and platelets to pRBCs correlate to longer ICU stays and higher mortality rates. When high ratios of FFP to pRBC are unable to be transfused, it has been demonstrated that resuscitating patients with a minimum of 1 L crystalloid per unit pRBC leads to improved mortality rates. However, a recent study showed that TBSA burn and patient age independently correlated to mortality, not RBC or plasma transfusions. Blood product resuscitation was not hemostatic, and coagulopathy and thrombocytopenia combined may contribute to intraoperative hemorrhage, which blood product transfusions would be inadequate to correct. Brakenridge and coworkers showed that, despite earlier reports of associations between FFP and large-volume crystalloid transfusions with MOD, it was the MT volumes of pRBC that correspond to MOD, not blood products. Blood component ratios failed to predict inflammatory complications, whereas injury severity, sex, and total pRBC volume did. Additionally, transfusion of stored pRBC correlates with increased complications due to microparticles released from RBCs able to induce cellular dysfunction. The poor quality of stored erythrocytes has been documented with dynamic microscopy. Furthermore, recent data would suggest different protocols for transfusion in the operating room (acute blood loss) versus in the setting of critical illness (bedside). A series of studies examining different ratios of FFP to pRBC transfusions have yet to demonstrate any difference in transfusion volume for burned pediatric patients. , Last, it has been demonstrated that transfusion protocols for adults are not efficacious in children; a new score should be developed for transfusions in the burned pediatric population.
Recently, platelet-rich plasma (PRP), in which the platelet concentration is above baseline in blood plasma, has come under consideration for use in transfusing burn patients because its hemostatic antimicrobial effects have shown promise in wound healing in animal studies. The concentration of growth factors and number of platelets dictate the clinical efficacy of PRP. It is not transfusions of pRBCs but rather of platelets that have recently been correlated to nosocomial infections in the critically ill. Platelet transfusion is not without complications because platelets are stored at room temperature, thereby facilitating higher rates of bacterial contamination than for other blood products. One in 1000 to 3000 platelet units may be bacterially contaminated; one-sixth of these episodes result in a septic event. In a study of blood bank use by a burn unit, 15% of all admitted patients received platelets with either pRBCs or FFP. , Given that cryopreserved platelets demonstrate superior hemostatic activity over liquid platelets, studying the efficacy of storing platelets at cold temperatures for burn units is warranted. , Last, immediate administration of pRBCs, plasma, and platelets upon admission has been shown to benefit patient outcome.
Commonly coincident with sepsis, thrombocytopenia requiring platelet transfusion is rare in burn patients. Often platelet counts and function are stable unless there is an infectious or septic event. In coagulopathic patients with hemodynamically significant oozing from wound and donor sites, the administration of platelets and recombinant factor VIIa has been shown to improve hemostasis. , Of interest, recombinant factor VIIa seems most efficacious at lower temperatures. Prothrombin complex concentrate (PCC) is gaining utility in treating coagulopathies derived from medications such as warfarin or argatroban and now has an expanding role in treating trauma and perioperative coagulopathies. PCC is also gaining use as an adjunct or replacement for FFP to reverse factor-deficient coagulopathies and expedite operative intervention. ,
Venothromboembolic prophylaxis
Once burn patients recover from TIC, they develop an elevated risk of venous thrombosis and thromboembolism. A recent study indicated that platelet-derived microparticles are responsible for the hypercoagulability seen immediately postburn, particularly the decline in platelets, and that an adenosine diphosphate–induced platelet activation was crucial to the enhanced clotting seen a week postburn. Additionally, Levin et al. showed that thermal trauma incites an increase in the number of erythrocyte-derived microvesicles. These, in turn, increase the procoagulant activity while reducing the antithrombin and fibrinolytic activity of erythrocytes, thereby contributing to postburn hypercoagulability. Furthermore, the typically defined criteria for hypercoagulability described in Virchow’s triad exist in all major burn patients: venous stasis from reduced activity such as bed rest, endothelial activation or injury from shock state and inflammation, and hypercoagulability from acute-phase reactants. , Venous and central venous indwelling catheters represent a further risk factor, implicated in as many as 70% of postburn venous thromboses. Meizoso recently characterized the detailed pathophysiology of hypercoagulability in burn patients, concluding that larger-scale studies are needed to protocolize safe and effective thromboprophylaxis. A typical burn ICU patient will be high or highest risk based on the American College of Chest Physician guidelines and Caprini score, indicating both mechanical and chemical prophylaxis. In a 2005 survey of 84 US burn centers, 76.1% routinely provided VTE prophylaxis, 31 used subcutaneous unfractionated heparin (UFH), 16 used low-molecular-weight heparin (LMWH), and 1 used a heparin infusion. In a 2013 review of their institution’s patients in a single year, Mullins et al. reported an incidence of 113 DVTs in 86 patients for an incidence of 5.92%.
The modalities that underlie VTE prophylaxis are mechanical and pharmacologic prophylaxis. Mechanical treatments, such as intermittent pneumatic compression, aim to prevent venous pooling and mechanically pump blood from the extremities. These devices also stimulate fibrinolytic pathways, which further decreases the risk of venous thrombosis. , Chemical prophylaxis, such as heparin, is intended to reduce thrombosis by interfering with the coagulation cascade. Prophylaxis is often complicated in the burn population. For instance, mechanical prophylaxis is often impractical or impossible due to donor sites or wounds on the legs. Pharmacoprophylactic agents can have inconsistent effects due to altered pharmacokinetics and pharmacodynamics leading to either venous thrombosis or hemorrhage.
Pharmacologic anticoagulants fall under four major classes: antithrombin-III (AT-III) activators, such as UFH; factor X inhibitors, such as LMWHs; direct thrombin inhibitors (DTIs), such as argatroban; and vitamin K antagonists, such as warfarin. The ideal pharmacoprophylactic agent for a burn patient has a short half-life allowing dose titration and operative interventions, the ability to monitor resulting effects with laboratory values, an available reversal agent, and limited nursing workload. Warfarin is not used for prophylaxis in hospitalized burn patients due to its long half-life, which requires days to take effect and reestablish normal coagulation, all of which complicates operative management. DTIs carry a high risk of bleeding and are irreversible so typically are employed only in the rare setting of antibody-confirmed heparin-induced thrombocytopenia (HIT) when treating burn patients. Most VTE prophylaxis and treatment in burn patients is carried out using UFH or LMWH.
UFH exerts the principal part of its action by binding to and activating AT-III, the most abundant anticoagulant in the plasma. AT-III, in turn, breaks down activated thrombin, thereby terminating the propagation of coagulation. A minor portion of AT-III’s action is attributable to inactivating factor X, the central factor joining the intrinsic and extrinsic coagulation cascades. Anticoagulant activity can be monitored, with a PTT targeting time of 30 to 41 seconds for prophylaxis and 60 to 80 seconds for therapeutic anticoagulation. UFH can be administered either subcutaneously or via a continuous intravenous infusion. Subcutaneous dosing of 5000 units every 8 hours is considered an effective prophylactic dose; however, in burn patients with unpredictable subcutaneous absorption and variable creatinine clearances due to hypermetabolism, this route is far less predictable. In our critical care population, we prefer a low-dose UFH infusion targeting a PTT of 30 to 41 seconds, or 1.5 times preprophylaxis aPTT. With this protocol, we are able to provide a verifiable prophylactic effect regardless of the physiologic state of the patient, although this comes at the cost of greater nursing usage. UFH also has the benefit of a short half-life, and, in the setting of hemorrhage, it is reversible with protamine. There is a risk of development of HIT with this medication, and platelet levels must be monitored. Should thrombocytopenia develop in a burn patient, all heparin administration should be held until antibody titers can be returned. Because there are myriad causes of thrombocytopenia in burn patients, conversion to a secondary agent, such as a DTI, ought to be considered carefully on a case-by-case basis given the increased risk of bleeding associated with these medications and their lack of reversal agents.
LMWH exerts its principal effect by inactivating factor X. Anticoagulant activity can be monitored with an antifactor Xa level target of 0.2 to 0.5 U/mL for prophylaxis and 0.5 to 1.2 U/mL for therapeutic anticoagulation. In a review of practice at a large academic medical center, levels were determined to be insufficiently monitored and frequently outside the intended range in patients weighing less than 45 kg, more than 150 kg, or with impaired renal function. These medications are delivered by subcutaneous injection and thus carry pharmacodynamic concerns regarding inconsistent absorption. There are also oral factor Xa inhibitors; however, there are not currently sufficient data or experience to advocate their prophylactic use in the acute burn patient for VTE prophylaxis. The half-lives of these agents are longer than UFH, and they only require dosing every 12 to 24 hours, which reduces nursing workload but increases the duration of bleeding, should it occur. In particular, fondaparinux has a 17- to 21-hour half-life and thus is particularly prone to cause bleeding in our experience with burn patients; the use of fondaparinux is ill-advised. When these medications are chosen for burn patients, factor Xa levels should be monitored due to unpredictable subcutaneous absorption and large changes in creatinine clearance from hypermetabolism or renal impairment, although these pharmacologic issues are most often studied related to antibiotic dosing. There are currently no reversal agents for this class, although scant data suggest that PCC may limit bleeding.
There are circumstances in which VTE prophylaxis may need to be held in a major burn patient, such as bleeding. In these instances, an inferior vena cava filter can be considered to reduce the risk of fatal pulmonary embolism. Furthermore, several centers routinely monitor patients for DVT formation with a weekly Doppler exam. Good evidence suggests that delay to initiation of VTE prophylaxis results in higher rates of DVT and pulmonary embolism.
Hematopoiesis
Given the myriad risks incurred to glean the benefits of transfusion, it is preferable for patients to generate their own replacement blood. Hematopoiesis is the production of the more than 10 distinct mature peripheral blood cell types. Well-regulated hematopoietic differentiation is vital to generate all blood cells necessary for defense against invasive pathogens, gas exchange, and wound healing. This process begins in the yolk sac, continues in the placenta and the aorta-gonad-mesonephros region, and progresses to the fetal liver until finally occurring throughout postnatal life in the bone marrow. , Table 18.1 details the roles of growth factors and cytokines in directing hematopoiesis. Unfortunately, production is often insufficient to meet a burn patient’s RBC requirements in the setting of large excisions and grafting procedures combined with critical care. This stems from the large volume of blood loss seen in burn surgeries, as well as the fact that thermal trauma directs hematopoiesis away from erythropoiesis and toward immune cell production.
Table 18.1
The Roles of Growth Factors and Cytokines in Hematopoiesis
| Growth Factor or Cytokine | Role in Hematopoiesis |
|---|---|
| Stem cell factor |
|
| Flt-3 ligand |
|
| IL-3 | Plays a role in hematopoietic stem cell, myeloid, and erythroid cell line expansion |
| IL-6 |
|
| G-CSF |
|
| CSF-1 or M-CSF |
|
| GM-CSF |
|
| IL-7 | Necessary for both engagement into lymphoid lineage and maintenance and expansion of lymphoid cells |
| Erythropoietin |
|
| Thrombopoietin |
|
DC, Dendritic cell; G-CSF , granulocyte colony-stimulating factor; GM-CSF , granulocyte-monocyte colony-stimulating factor; IL , interleukin; rhEPO, recombinant human erythropoietin; RhG-CSF, recombinant human G-CSF.
Two pathways exist for hematopoiesis: myeloid and lymphoid. The myeloid lineage ultimately produces RBCs and the cells comprising the innate immune system (e.g., platelets, macrophages, neutrophils, eosinophils, and basophils). The lymphoid lineage forms the cornerstone of the adaptive immune system by generating B and T cells. Dendritic cells (DCs) and natural killer cells develop from either lineage. Although only half the bone marrow is hematopoietically active, an estimated 200 billion erythrocytes (0.5–2% of total RBCs), , 100 billion leukocytes, and 100 billion platelets (~7% of total platelets) are nonetheless produced daily in a healthy adult.
Accounting for one in every 10 nucleated cells in the bone marrow of a healthy adult, hematopoietic stem cells (HSCs) are the fountainhead of the hematopoietic hierarchy. They are the only cells in this system able to be both self-renewing and multipotent (able to differentiate into all potential blood cells). , The two variants of HSCs, long-term (LT) and short-term (ST), are distinguishable by more than their divergent self-renewal and differentiation capacities. Aptly named, LT-HSCs remain permanently self-renewing cells with minimal response to physiologic stress and exhibit a total dearth of lineage-specific surface markers. ST-HSCs derive from LT-HSCs and affect their production and differentiation depending on the existing pathologic state in their niches. ST-HSCs give rise to multipotent progenitor cells (MPPs), which lack self-renewal potential but remain able to differentiate into every hematopoietic lineage. , , The progression of hematopoiesis, from stem cells to progenitor groups to terminally differentiated cells ( Fig. 18.3 ), allows for the rapid amplification of cell production by the upstream proliferation of stem cells. The hematopoietic hierarchy is not without controversy; other suggested hematopoietic progressions , differ in the branch points at which certain progenitor populations lose lineage potential or advocate that select cell groups have the potential to dedifferentiate and enter a different lineage. MicroRNAs (miRNAs), growth factors, and cytokines present in the bone marrow influence the commitment patterns of these progenitor cells, yielding mature, fully differentiated bone marrow cells that later populate the bloodstream.
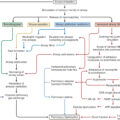
A hierarchical model of hematopoiesis. The model here shows the three compartments of hematopoietic cells: stem cells, lineage-committed progenitors, and terminally differentiated cells. The first step in lineage commitment occurs at the branch point from multipotent progenitors (MPPs) to myeloid (common myeloid progenitor [CMP] ) or lymphoid lineages (common lymphoid progenitor [CLP] or mast cell progenitors [MCPs] ). CLPs differentiate into T and B cells. The CMP population can branch in to granulocyte-monocyte progenitors (GMPs) or megakaryocyte-erythroid progenitors (MEPs), which then lead to their respective terminally differentiated populations. LT-HSC, Long-term hematopoietic stem cell; ST-HSC, short-term hematopoietic stem cell.
Upregulation of fetal liver kinase-2 (Flk2) is a shared feature of all lineages of HSC differentiation as is the epigenetic regulation exerted by miRNAs on every stage of hematopoiesis. The expression of a limited set of transcription factors, controlled by growth factors, cytokines, and miRNAs present in the bone marrow milieu, control lineage commitment, cell fate, and, ultimately, the composition of cells in the bloodstream. As patients age, there is an HSC shift toward myeloid potential.
Bone marrow hematopoiesis demonstrated an overall increase in the HSC population (identified as LSKs [Lineage-negative, Sca-1 + cKit + ] in mice) as early as 48 hours after burn injury, and the expansion of LSKs persisted for at least 21 days postburn. Despite their multilineage potential (see Fig. 18.3 ), LSKs do not differentiate evenly across all lineages. Only ST-HSCs and MPPs increase, with no significant change in LT-HSCs. In the progenitor compartment, there is a significant increase in granulocyte-monocyte progenitors (GMPs) with a concomitant decrease in megakaryocyte-erythroid progenitor (MEP) production. Given the hierarchical nature of hematopoiesis, changes in ST-HSC and MPP production, and the lineage shift toward greater GMP and lesser MEP production may herald the overall problems present after burn injury: erythropoietic production (anemia) and myeloid function (immune dysfunction). , In a recent work, myeloerythroid commitment after thermal insult was shown to be under β-adrenergic control via MafB regulation, indicating that burn injury perturbs the hematopoietic paradigm. For more details, please refer to Chapter 23 on the significance of the hormonal, adrenal, and sympathetic responses to burn injury. Further work on HSCs and progenitor cell responses may provide avenues for early therapeutic intervention, which may ameliorate the negative hematopoietic consequences of burn injury.
HSCs have considerable potential in treating blood disorders. The use of these cells as a possible therapy for the anemia or immune dysfunction present in severely burned patients is currently not in progress. Rea and colleagues assayed the cells present in the healing burn wound, finding that hematopoietic cells were merely transient and predominantly present only in the acute inflammatory phase, with a small number persisting in the healing dermis. Ascertaining the long-term hematopoietic response to various degrees of burn wounds will be crucial in developing HSC-based therapies for burn injuries.
Because of burn-associated anemia, EPO levels should be increased during treatment and recovery from the burn injury. However, contrary to the expected EPO response to anemia, there is limited increase in EPO after burn. Earlier studies had small sample sizes, used unreliable urine bioassays, and could not overwhelmingly support an appropriate EPO response, leading to contradictory results. , Later comparison of serum bioassays and radioimmunoassays showed no correlation between the two methods, and their results suggested significant differences between the sensitivity of these tests. , More recent larger studies using serum radioimmunoassays demonstrated an increase in EPO in response to decreased Hb concentrations but inconsistent/reduced erythropoietic response to this EPO increase. ,
Whereas only erythroid-committed cells in the bone marrow possess the EPO receptor, a related EPO receptor and response to EPO have been identified in nonhematopoietic tissues, including neurons, glial cells, retina, heart, skeletal muscle, kidney, ovary, uterus, testis, and endothelial cells. Consequently the ability of EPO to reduce apoptosis and prevent damage to these tissues has been explored. Recombinant human erythropoietin (RhEPO) in particular can reduce apoptosis after cerebral ischemia ; protect the myocardium and promote remodeling after myocardial ischemia, allowing for restoration of cardiac function , ; and protect against renal injury from ischemia, improving renal function. Despite these findings and the expected erythropoietic response to rhEPO, its use in burn patients has not been substantiated.
rhEPO helps augment erythropoiesis in patients with chronic anemias (e.g., end-stage renal disease and HIV with antiretroviral use), decreasing transfusion rates and improving quality of life. To decrease transfusion rates and correct the anemia of critical illness, multiple trials have explored rhEPO use in the critically ill, including burn patients. Unfortunately, both large clinical trials and meta-analyses of critically ill medical, surgical, and trauma patients show no significant reduction in transfusion rates with rhEPO use. , Still and others performed a study of rhEPO in burn patients resulting in no significant increase in hematocrit percentage or decrease in transfusion rates. Critically ill patients may possess a resistance to EPO, which may be a function of anti-EPO antibodies or a relative reduction in erythropoietic response due to less EPO-responsive erythroid precursors after burn-induced hematopoietic hierarchy shift. As such, rhEPO is not indicated for use in burn patients. However, a recent study showed that rhEPO significantly reduced the markers of multisystem organ failure and, in the lung, specifically reduced apoptosis and histologic signs of tissue injury in mice with second-degree scald burns. Although the use of rhEPO has been shown to increase the rate of reepithelialization in scald injury and decrease time to close the wound when injected directly into the injury site, we still cannot recommend the use of rhEPO in burn patients to decrease transfusion rates. These new data highlight the potential use for other burn-induced complications beyond the purview of this chapter. Before the recognition of the role of EPO in stimulating hematopoiesis, pharmacologic treatment of anemia consisted of supplementation (iron, B 12 , folate) and anabolic steroids. There are indications that burn patients remain sensitive to the erythropoietic effect of anabolic steroids such as oxandrolone, which had been demonstrated to help moderate numerous aspects of pathophysiology postburn.
Myeloid growth factors
Granulocyte colony-stimulating factor
Granulocyte colony-stimulating factor (G-CSF) is the primary growth factor responsible for the proliferation and differentiation of bone marrow granulocyte progenitors into mature granulocytes. , G-CSF is produced by monocytes, fibroblasts, and endothelial cells stimulated to produce G-CSF in response to inflammatory cytokines (tumor necrosis factor-α, interleukin [IL]-6, IL-1). Although it stimulates the production of neutrophils in the bone marrow, in the periphery G-CSF augments the bactericidal activity of neutrophils by priming the oxidative burst, increases neutrophil half-life by preventing apoptosis, and downregulates the overall inflammatory response by decreasing the cytokine production of monocytes and macrophages. In various animal models of burn and burn sepsis, the benefits of G-CSF were shown to be the killing of translocated bacteria, regulating the proinflammatory response to injury, enhancing neutrophil chemotaxis, and improving survival in combination with antibiotic therapy. ,
At baseline, there are very low levels of G-CSF present in the blood. However, after an inflammatory or infectious process, G-CSF levels dramatically increase. After a burn injury, G-CSF levels in the blood are initially increased and then gradually decline to baseline 3 to 4 weeks after injury. The initial increase in G-CSF may prime the neutrophilic component of the immune response for future bacterial insult. However, the immune dysfunction seen after burn injury or burn sepsis may be related to hyporesponsiveness of bone marrow progenitors and peripheral neutrophils to G-CSF. Recent studies suggest that the increase in serum G-CSF postburn corresponds to an increase in the resistance to infection, activation of innate immune responses, and prioritization of bone marrow responses, indicating that it plays a central role for burn patient survival, especially in the setting of infection.
Administration of recombinant human G-CSF (rhG-CSF) to burn septic animals before the initiation of septic insult has been shown to improve the survival rate of burn septic mice. , , However, administration of G-CSF 24 hours after the onset of septic insult had little effect on survival. , Despite the potential benefit of exogenous G-CSF administration on the inflammatory and infectious response during burn injury, the use of rhG-CSF (filgrastim) is not indicated in the treatment of burn patients.
CSF-1
CSF-1 (M-CSF) is a preeminent growth factor for the differentiation, proliferation, and survival of monocytes and macrophages. It also stimulates chemotaxis, cytokine, and superoxide production in macrophages. , Hume et al. first demonstrated that administration of CSF-1 to mice resulted in monocytosis and an increase in peritoneal and tissue macrophages. In response to burn injury, GM-CFU responsive to CSF-1 are increased in the bone marrow, and this results in enhanced monocytopoiesis. The underpinning of this monocytopoiesis postburn arises from increased expression of CSF-1 receptors in the ERMP-20 + bone marrow compartment, comprising monoblasts and promonocytes, which begins to be initiated much earlier at progenitor level in GMPs and CMPs. Additionally, burn injury and sepsis also alter the inflammatory cytokine phenotype of macrophages derived from CFU-GM in that they predominately result in hyporesponsive macrophages. , Similar hyporesponsiveness in monocytes has been demonstrated in trauma patients. These findings provide a plausible mechanism and a role for CSF-1 and its cognate receptor interactions in monocyte/macrophage biology after burn injury.
GM-CSF
Granulocyte-monocyte colony-stimulating factor (GM-CSF) regulates proliferation and differentiation of hematopoietic progenitor cells and modulates the function of mature leukocytes. GM-CSF enhances the antigen-presenting capacity of macrophages and DCs, increases complement-mediated phagocytosis, and augments bacterial killing by both innate immune cells , and chemotaxis of leukocytes. , GM-CSF is produced by a variety of cells, including macrophages, B lymphocytes, pulmonary epithelial cells, neutrophils, and stromal cells. , In response to burn injury, bone marrow GM progenitors respond by producing more GM-CFU colonies. Administration of GM-CSF before burn injury and Escherichia coli sepsis enhanced bacterial clearance and survival of experimental animals. Similarly, GM-CSF improved the survival of neonatal rats when administered prophylactically before Staphylococcus aureus infection. However, GM-CSF administration after the onset of infection did not provide a survival benefit. Although the inactivation of GM-CSF or GM-CSF receptor genes in mice did not alter the number of granulocytes and monocytes, these animals exhibited significant alveolar macrophage dysfunction. Furthermore, GM-CSF–deficient mice are very susceptible to pulmonary group B streptococcal infection. Cioffi et al. studied the effects of GM-CSF in burned adults. They found a 50% increase in mean leukocyte counts after the first week postburn in treated patients. Application of GM-CSF did increase myeloperoxidase activity (cytosolic oxidative function) 1 week postburn, but these levels returned to unburned control levels during weeks 2 and 3 of treatment while remaining elevated in the untreated patients. Extracellular oxidative function, measured by superoxide production, was initially depressed in both burned groups compared with nonburned controls, although patients treated with GM-CSF demonstrated a return to nonburned control levels after week 1, whereas these levels remained below control levels in the untreated burn patients. In a multicenter clinical trial, administration of rhGM-CSF in hydrogel to deep second-degree burn wounds has been shown to be both safe and to accelerate wound healing. , A subsequent study found topical application of GM-CSF reduced healing time of partial-thickness burn wounds by 5.1 days compared with standard treatment with no significant increase in adverse effects. The same study examined two other growth factors, fibroblast and epidermal, and found a decrease in healing time by 5.02 and 3.12 days, respectively, as well as improvement in scar color, height, pliability, and vascularity. Further research examining the efficacy of topical administration of rhGM-CSF on deep partial-thickness burn wounds similarly found accelerated wound healing with no difference in adverse reactions. These data corroborated other studies that likewise found accelerated wound healing with application of topical rhGM-CSF and no difference in adverse reactions in adult and pediatric burn patients. Given the promising data, cautious increasing use as a topical treatment to promote wound healing is warranted, but further examination of rhGM-CSF, along with fibroblast and epidermal growth factors, is needed.
Lymphoid growth factors
Several growth factors/cytokines contribute to the formation of lymphoid cells; the most prominent and well studied is IL-7. The IL-7 receptor is unique to lymphoid cells. Thus IL-7 is the cytokine/growth factor that influences the expansion of this cell line. IL-7 receptor engagement is essential not only for lymphoid cell proliferation and survival but also for HSC differentiation into the lymphoid lineage. The IL-7 receptor enhances lymphoid cell survival through maintenance of Bcl-2. Bone marrow stromal cells and the thymus predominantly produce IL-7. T cells are unique because their maturation takes places in the thymus as opposed to the bone marrow, and they undergo a process of positive and negative selection dependent on both IL-7 activation and expression of the transcription factor Notch1. Alterations in IL-7 production, in addition to other cytokines, can negatively impact survival after inhalation injury. Additional growth factors/cytokines contributing to lymphopoiesis include IL-2, IL-15, and IL-23.
Megakaryocyte growth factors
Production of megakaryocytes and platelets is regulated by thrombopoietin. Similar to EPO, thrombopoietin enhances megakaryocyte progenitor proliferation by amplifying cell-cycle regulators and preventing apoptosis. It is the only growth factor necessary for proliferating megakaryocytes and their progenitors. Unlike EPO, thrombopoietin has a synergistic role with other growth factors and cytokines in the maintenance and proliferation of HSCs and can be used in their expansion. Thrombopoietin stimulates platelet release from the bone marrow and in the periphery, thereby upregulating platelet function and aggregation. Produced in the liver, kidney, skeletal muscle, and stromal cells of the bone marrow, , thrombopoietin production may be increased in response to increased IL-6 production. Given the elevated IL-6 levels present after burn injury, IL-6-induced thrombopoietin release may be responsible for the thrombocytosis often seen immediately postburn. Elevated levels of thrombopoietin, and subsequently platelet activation, may be present after burn injury. Evidence from a recent study supports the notion that thrombopoietin blockade could help prevent organ damage in burn patients with sepsis.
Transcription factors
Whereas growth factors control hematopoietic cell fate, the development of terminally differentiated cells is under the control and coordination of a limited set of transcription factors. Ultimately, specific sequential and temporal gene expression patterns dictate hematopoietic commitment. These genetic processes are governed though modulations in the rate of gene transcription, which are accomplished through the binding of DNA-binding proteins or transcription factors to specific regions on a gene. Transcription factors are nuclear proteins that act as control points in the conversion of a gene to a functional protein. Because many key proteins are turned over rapidly to meet the changing needs of the tissues, a complex system of cell signaling architecture, with the final common pathway of gene transcription, must exist to produce bioactive proteins on demand. Because cells respond to several signals simultaneously, and many ligand–cell interactions stimulate similar proximal signals, tight control of transcriptional initiation must exist for the proper orchestration of cellular responses.
The role of transcription factors in hematopoietic cell fate is an evolving topic of study. The lineage-restricted proliferation and differentiation program of hematopoiesis is achieved through switching on and off specific sets of genes in response to cell signals. Because thermal injury and sepsis are accompanied by hematologic and hematopoietic changes that determine the overall pathophysiologic response of burn patients, it is reasonable to assume that transcriptional regulation of hematopoietic developmental genes play a significant role. It is known that GATA-1, sct/tal1, and Klf1 form the transcriptional core of the erythroid lineage and are all expressed by the earliest hematopoietic progenitors. The relationship between transcription factors is complex because they are not independent of one another but demonstrate antagonism. In fact, the inability of one transcription factor to suppress the other has been linked to the development of hematologic malignancies. However, little is known about hematopoietic transcription factor changes after injury, even though they may control the dramatic hematopoietic shifts after severe trauma and burn injury. Given the importance of these transcription factors to cell fate and the significant shifts in lineage commitment patterns, knowledge of these transcription factors and their roles in hematopoiesis may help provide a foundation for future research. Furthermore, recent studies indicating the poor correlation of animal models to humans with regards to transcriptional response after burn/trauma/endotoxemia highlight the need for medical research to shift to higher fidelity models, especially mouse models, although the clinical translatability will continue to be debated.
Conclusion
Hematology plays a major role in burn care. Patients suffer from anemia due to RBC losses in surgery as well as the anemia of critical illness. Operative hemostasis is important both to limit RBC loss and prevent shock. Coagulopathies develop due to factor consumption and insufficient production, as well as hypothermia. Transfusion of various blood products is critical to the management of patients. Hematopoiesis is directed away from erythropoiesis to the production of the immune cells to fight off invading microbes and heal wounds. Venous thrombosis is a major risk in these critically ill patients, potentially increasing mortality. Hematologic management is a central component of burn critical care, and progress in this area should lead to progress in the treatment of burned and critically ill individuals generally.
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree