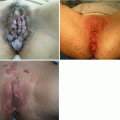
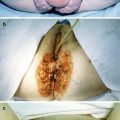
(1)
Universidade Federal Fluminense, Niterói, Rio de Janeiro, Brazil
1.1 Introduction
The skin is the largest organ of the human body, and corresponds to 15% of the body’s weight. Although there are topographical variations, it is composed of three basic structures layered in the following order: hypodermis (subcutaneous layer), dermis and epidermis.
This covering tissue that bounds the individual of his environment has as vital functions the protection against external aggressions, the maintenance of fluids in the body, and the thermoregulation, besides playing an important sensorial role. Due to its great accessibility to inspection, unlike the viscera, the skin becomes one of the major components of the physical beauty providing self-esteem and social coexistence. Frequently, aesthetic changes cause inferiority feelings and unthinkable social discrimination to people for the rest of their lives.
This inspection easiness requires the knowledge of a number of skin changes related only to aesthetics, in order to differentiate them from those that actually bring harm to health.
The cutaneous integrity is fundamental so that the skin can properly put in practice its prevention function against the access of toxic agents, microorganisms and excess of ultraviolet radiation to the body, impede the loss of fluids, and protect against excess of temperature, mechanical forces and low-voltage electric current.
1.2 Skin Structure and Function (Fig. 1.1)
1.2.1 Epidermis
The epidermis is a stratified, keratinized, not vascularized pavement epithelium of ectodermal origin. The epidermis originates the following cutaneous attachments: pilosebaceous follicle, sudoriparous glands, hair, and nails. Its main functions are the relative impermeability, which prevents the free movement of fluids and molecules in both directions, the protection from the entry of microorganisms, as well as from excessive ultraviolet radiation and low-voltage electric power.
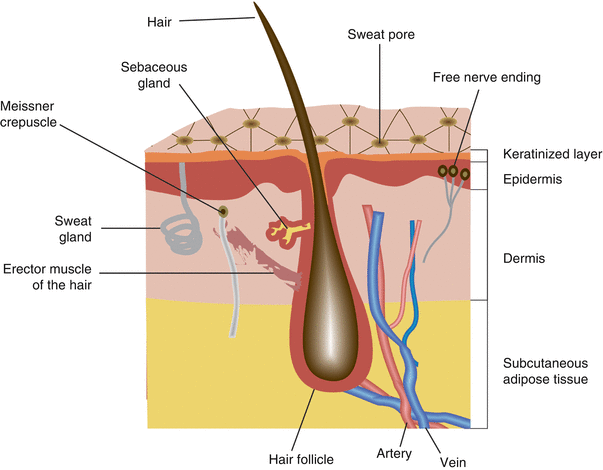

Fig. 1.1
Skin Structure and Function
As it is not vascularized, the epidermis depends on the supply of nutrients through the dermis, with which establishes a relationship of interdependence.
The dermis basic element is the keratinocyte, which during its migration towards the surface undergoes a differentiation process, whose goal is the production of keratin. When the keratinocyte reaches the surface, it is transmuted into an inviable and anucleated cell full of keratin, which will then perform the main epidermic functions.
The epidermis is divided into four cell extracts, characterized by degrees of its keratinocytes differentiation and morphology. The nearest layer to the dermis is the basal layer, following towards the surface the spinous extract, the granulous and finally the corneal (Fig. 1.2).
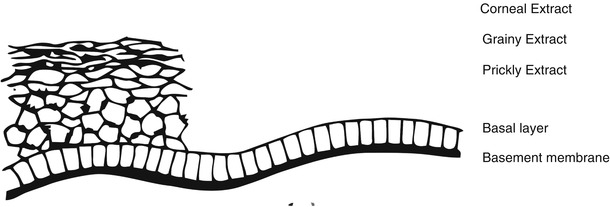

Fig. 1.2
Epidermis
1.2.1.1 Basal or Germinative Layer
As the cornea’s cells are continuously removed, the maintenance of the epidermis depends on a permanent replacement of new cells. This replacement is promoted by the keratinocytes mitosis of the basal layer, which are little differentiated, and retain proliferative capacity. The basal layer is composed of a single layer of cylindrical cells, with the largest axis perpendicular to the dermoepidermal junction. In normal skin, around 10% of the basal cells are in mitosis. At any given time this percentage could increase depending on the physiological (repair) or pathological (e.g., psoriasis) needs.
1.2.1.2 Spinous Extract
It consists of several layers of polygonal keratinocytes under differentiation process. These are rich in cytoplasmic tonofilaments, grouped more compactly, as the cell progresses toward the surface. These tonofilaments are the precursors of keratin.
1.2.1.3 Granulous Extract
It consists of variables layers of flattened keratinocytes containing granules of keratohyalin associated with cytoplasmic tonofilaments. These granules seem to contribute to the formation of the cytoplasmic matrix of corneal cells.
1.2.1.4 Corneal Extract
It consists of 8–15 layers of flattened anucleated keratinocytes. The cytoplasm is completely filled with a very resistant and insoluble fibrous protein called keratin.
As it is the final product of the keracinocyte differentiation, the corneal extract is the main responsible for the protective functions of the epidermis. Although it is not completely impermeable, it is an excellent barrier to the movement of fluids, molecules and microorganisms, and any damage to its integrity harms this function extremely.
Its low water content is the unique and exclusive feature that raises difficulties to the establishment of microorganisms on the surface of the skin.
The epidermic extracellular space is extremely impermeable, allowing the nutrition of all epidermic layers, except the corneal extract. A water-soluble barrier is located in the boundary between the granulous and the corneal extract. This barrier is probably responsible for the abrupt transformation of the viable cornified cells in not viable ones, because it disables the nutritional supply to those cells located above it. The impermeable property of this region appears to be caused by two factors: a special substance secreted at this level and represented by Odland bodies or lamellar bodies, and a type of intercellular contact found only there, named zonula occludens, in which there is an intimate union between the adjacent cytoplasmic membranes.
There are still two other specialized types of epidermal intercellular contact: the gap junction and the desmosome. The gap junction sets a free traffic corridor between the adjacent cells and plays an important role in the differentiation of the epidermis as a whole; only missing in the corneal extract.
The demosomes are the main and most numerous types of epidermal intercellular contact. They occur in all layers, providing stability to the tissue. The hemidesmosomes occur between the basal cells and the basal lamina (Fig. 1.3).
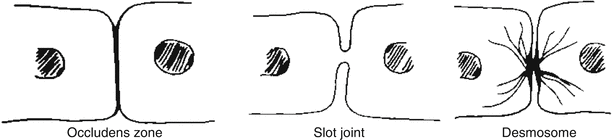

Fig. 1.3
Epidermal intercellular contacts
1.2.1.5 Dermoepidermic Junction
The dermoepidermic junction corresponds to the basal membrane in the optical microscopy. The electronic microscopy is a complex structure comprising the cytoplasmic membrane of the basal cells, the lucid blade (empty space), the basal lamina and the most superficial portion of the papillary dermis. Promoting adhesion between the basal cells and the basal lamina, are the hemidesmosomes, and between this and the dermis, the anchoring fibrils and microfibrills (Fig. 1.4).


Fig. 1.4
Dermoepidermal junction
The basal lamina has the following functions: ensure the dermoepidermic adherence, guide the migratory direction of keratinocytes to the surface and work as a system of pores of different sizes, allowing the quick passage of small molecules and making difficult the passage of larger molecules.
1.2.1.6 Other Epidermic Cellular Components
Non-keratinocytes cells of the epidermis are called clear cells, as they require special coloring to become evident. We will consider the melanocyte, the Langerhans cell and the Merkel cell.
Melanocyte
The melanocyte is a dendritic cell of neural crest origin (neuroectodermal) located between cells in the basal layer in an approximate proportion of one melanocyte to ten keratinocytes.
Its function is the synthesis of melanin obtained by the action of the enzyme tyrosinase on tyrosine. Melanin is stored in rounded cytoplasmic structures, the melanosomes, which are transferred to the adjacent keratinocytes via phagocytosis of dendritic cytoplasmic portions. Thus, the melanocyte functions as a unicellular exocrine gland.
Melanin is a brown pigment with photoprotection action. Racial variations of skin color depends on the quantity, size and morphology of the melanosome produced, as the melanocytes number and the melanin quality are basically the same.
The exposure to ultraviolet radiation increases the production of melanosome and its transference to the keratinocytes, causing skin pigmentation and providing greater protection against future exposures. White skins are more susceptible to harmful immediate action (burning) and late action (elastosis, keratosis, epitheliomas, melanomas) of this radiation.
Melanocytes are still susceptible to MSH (Melanocyte Stimulating Hormone), as well as to sex hormones, to inflammatory agents and to vitamin D produced in the epidermis.
Langerhans Cell
Is a dendritic cell situated in the basal and granulous layers, containing cytoplasmic granules in the form of a racket. Also originated in the bone marrow, performs an important immune function, presenting the antigen to dermal lymphocytes.
Merkel Cell
It is found in the basal layer of the skin of the fingers, lips, gums and palate, playing a mechanoreceptor sensorial function.
1.2.1.7 Cuttaneous Attachments
Pilosebaceous Follicle
Structure formed by the hair follicle, sebaceous gland, and hair erection muscle.
Hair Follicle
The hair follicle is distributed throughout the skin except in the palmoplantar regions. It is formed in the embryonic life by invagination of the keratinocytes. In the hair follicle ends the sebaceous gland duct, and in certain regions (axilla and genital region) the duct of the apocrine sweat glands also. All these structures are located in the deep dermis.
The hair presents three cyclical and permanent stages: anagen, catagen and telogen, corresponding respectively to growth, regression and resting of the follicle. The growth speed varies according to different parts of the body.
Much more than the aesthetic and the sensorial function, the hair is important for the protection from solar radiation, thermal homeostasis and tissue repair, acting as true reservoir of epidermal stem cells.
Sebaceous Gland
This gland originates in a protuberance of the hair follicle. Vary in number, size, and activity in the parts of the body. Under action of testosterone becomes active from puberty. Their secretion (sebum) is basically composed of liquids, which, together with the lipids derived from the corneal layer, will form the lipid mantle, which is a factor of impermeability (hydrophobic) and antisepticing.
Apocrine Sebaceous Gland
Derives from the same invagination germinal layer, which gives rise to the hair follicle. It is an androgen-dependent scent gland present only in the axillary, genital and periareolar areas, whose secretion is metabolized by the skin saprophytic bacteria, producing characteristic odour that functions as a social and sexual attraction.
Erector Hair Muscle
Smooth muscle positioned at the top of the dermis inside the hair follicle.
Eccrine Sudoriparous Glands
These glands, formed by epidermal sprouting, are distributed throughout the skin. The greater concentrations areas are located in the palmoplantar regions. They are located in the deep dermis and flow directly on the surface of the skin. Their number varies from two to four million, and its total mass is equivalent to a kidney’s. An individual can secrete up to 10 L of sweat per day.
Its basic and vital function is the thermoregulation obtained through the sweat evaporation with the consequent cooling of the cutaneous surface.
The composition of the secretion includes water, sodium, calcium, magnesium, iodine, phosphorus, sulfur, iron, zinc, manganese, mercury, urea, amino acids, albumin, types IgA, IgG and IgD alfa globulins and immunoglobulins. However, the serum metabolites depuration is fully held by the kidneys and is not considered a vital function of these glands.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree