17 Tarsorrhaphy
Tarsorrhaphy is the surgical fusion of upper and lower eyelid margins to narrow the palpebral fissure. It is usually performed to provide protection to the cornea from exposure in conditions such as proptosis, seventh nerve palsy, neuroparalytic keratitis, indolent corneal ulcer, or tear film deficiencies.
A tarsorrhaphy may be temporary, in which case no lid tissues are excised and intermarginal sutures are used for lid closure. It may be a useful adjunct to ptosis repair, eyelid retractor recession, and other procedures for which temporary corneal protection is required. In situations where a permanent bond between the lids is desired, raw tarsal edges are created to form a more lasting adhesion. A tarsorrhaphy may be performed laterally, medially, or both, depending on the clinical situation. Typically, union of the temporal third of the eyelid affords excellent corneal protection and still allows an adequate medial fissure opening for vision. Although tarsorrhaphy is sometimes recommended to narrow the palpebral fissure to produce improved cosmesis in patients with eyelid retraction, such as in Graves ophthalmopathy, the reader is cautioned that, in patients with progressive exophthalmos, a tarsorrhaphy may exert counterpressure on the orbital contents—preventing autodecompression. Thus, the patient’s proptosis and optic nerve functions should be stable before contemplating this procedure. In patients with exposure keratopathy secondary to eyelid retraction, disinsertion and recession of the eyelid retractors afford a much better cosmetic and functional result (see Chapter 16). For patients with seventh nerve palsy, gold weight lid load and lid reanimation with palpebral wire spring are alternatives to improve eyelid blinking and closure (see Chapters 18 and 19). The procedure described in this chapter is a simple, permanent tarsorrhaphy technique that does not require bolsters or sutures that need to be removed. It preserves the integrity of the anterior lamella, minimizing the potential problem of lid margin irregularity. In patients in whom the tarsorrhaphy has to be opened, the margins of the posterior lamellae will epithelialize normally without cosmetic or dysfunctional sequelae.
OPERATIVE PROCEDURE
The length of the eyelid adhesion necessary for the desired degree of narrowing is determined by pinching the upper and lower eyelids together with a nontoothed forceps and marking the parallel margins with a marking pen. The temporal portions of the upper and lower lids within the marking are anesthetized with a subcutaneous injection of 2% lidocaine (Xylocaine) with 1:100,000 dilution of epinephrine. A small amount of anesthetic is also injected under the forniceal conjunctiva.
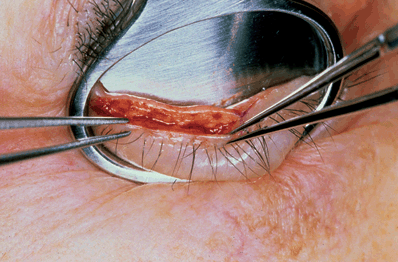
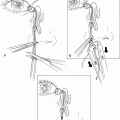
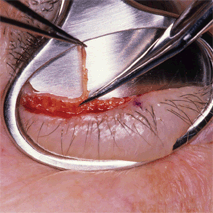
Figure 17-1. The eyelid is gently grasped and stabilized with nontoothed forceps held perpendicular to the lid margin. A chalazion clamp may also be used. It provides good hemostasis as well as firm support to the eyelid during marginal dissection. The anterior and posterior lamellas of the eyelid are split along the gray line with a size 11 Bard-Parker blade. Care is taken not to incise into the tarsal plate or the eyelash follicles. Occasionally, the anatomic landmarks of the lid margin (gray line and meibomian gland orifices) are indistinct. The tarsal plate can be readily identified by gently squeezing the lid margin with a smooth forceps and looking for the oily secretion at the meibomian gland orifice. The gray line is located just anterior to the meibomian gland openings. The blade is passed down along, and held firmly against, the anterior surface of the tarsal plate, and separation of the two lamellae is carried out to a depth of approximately 2 to 3 mm. After the incision in the gray line along the predetermined length has been made, an identical gray line incision is performed in the opposing lid to the same depth and length.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree