Surgical Decision-Making in Pediatric Spine Surgery
John B. Emans
Pediatric Spinal Deformity Is Different
Abnormal curvature in the pediatric spine carries a unique set of challenges: multiple types of deformity, multiple diagnoses, and a wide assortment of surgical techniques. Growth of the spine generally worsens the deformity but also presents opportunities for improvement. Concurrent growth and development of the thorax, hips, and other structures are at risk from a deformed spine. Underlying etiologic diagnoses for pediatric spine deformity vary widely in their effect on deformity progression, natural history, and effect on the child’s general health. Choosing the correct treatment requires coordinating all of this information into an individualized plan appropriate for the child at that time and going forth into the future. Choices made at this time have a lifetime effect on children with spinal deformity.
Assessing Pediatric Spinal Deformity
Understand the Deformity
Think in 3 dimensions. The Cobb angle risks reducing deformity analysis into a number, with values below a certain threshold treated less aggressively than those above the threshold. Like all disordered spine shape, pediatric spine deformity is a complex set of abnormalities in multiple planes—coronal, sagittal, and axial, as well as local individual vertebral distortion. Curve behavior with growth and long-term significance often relates more to the overall deformity than to the Cobb angle. Our analyses tend to focus on the most numerically severe deformity, but secondary deformities in the adjacent spine above or below or deformity in another plane may prove over the long run to be equally important. One helpful distinction in pediatric spine is to categorize deformity into global versus local or combinations. Local or global deformity can occur alone and require different goals and approaches. Local deformity may be rigid, while global may be less so. Combinations are common. The local deformity may have appeared first, with the global deformity compensating. Fixing the local deformity alone may also fix the global, but often in children, both local and global must be addressed, but not necessarily at the same time or with the same technique.
Understand the Stage in Growth and Growth Remaining
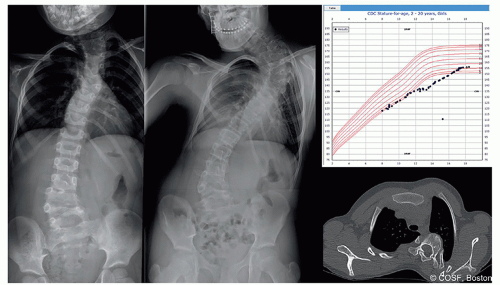
Rate of growth and stage in growth are fundamental to assessing the natural history of pediatric spinal deformity. Curve progression is most common during rapid growth in the first 3 years of life and then again in the rapid growth spurt that occurs in preadolescence. Many pediatric spinal deformity patients grow at a pace other than normal. Some syndromes are accompanied by precocious puberty, while others experience delayed growth. Chronically ill children or those with neuromuscular or endocrine diagnoses may grow slowly into their early twenties, greatly altering plans for spine deformity treatment
(Figure 1.1). The Risser classification and state of the triradiate cartilage are the most commonly used markers for growth, but the Risser sign in particular can be misleading. The Sanders digital score helps with assessing stage of growth in healthy early and late adolescents. For more complex situations and younger children, bone age determination can help greatly in assessing the stage in growth. The pediatric growth chart on paper or in the electronic medical record offers additional insight into the complex patient. Failure to grow, poor nutrition, and stage in growth are most sensitively displayed in the growth chart; much more than the snapshot in time that a single-hand x-ray displays. Knowledge of stage in growth, height percentile, and access to the growth chart allows a reasonable estimate of predicted final height. Spinal curvature, multiple congenital vertebral anomalies, and spinal fusion all negatively impact spine length. Assessing the potential effect of treatment on spine height is integral to deciding on treatment. A working knowledge of Dimeglio or others’ data on spinal growth is essential to making treatment choices. Actually calculating the predicted growth remaining and discussing with family facilitates a correct choice.
(Figure 1.1). The Risser classification and state of the triradiate cartilage are the most commonly used markers for growth, but the Risser sign in particular can be misleading. The Sanders digital score helps with assessing stage of growth in healthy early and late adolescents. For more complex situations and younger children, bone age determination can help greatly in assessing the stage in growth. The pediatric growth chart on paper or in the electronic medical record offers additional insight into the complex patient. Failure to grow, poor nutrition, and stage in growth are most sensitively displayed in the growth chart; much more than the snapshot in time that a single-hand x-ray displays. Knowledge of stage in growth, height percentile, and access to the growth chart allows a reasonable estimate of predicted final height. Spinal curvature, multiple congenital vertebral anomalies, and spinal fusion all negatively impact spine length. Assessing the potential effect of treatment on spine height is integral to deciding on treatment. A working knowledge of Dimeglio or others’ data on spinal growth is essential to making treatment choices. Actually calculating the predicted growth remaining and discussing with family facilitates a correct choice.
Understand the Underlying Disease Pathophysiology
Most idiopathic and congenital deformities occur in otherwise healthy individuals, but many other pediatric spinal deformities do not. Underlying genetic syndromes, connective tissue disorders, metabolic abnormalities, stable or progressive neurologic diseases, and other diagnoses may be at least in part responsible for the deformity. Etiology greatly influences risk of progression, rate or age at which progression occurs, and response to nonoperative treatment. Perioperative and longer term complications as well as likelihood of revision all depend heavily on the underlying diagnosis. A thorough knowledge of the underlying pathophysiology will prepare the surgeon and may avert an adverse event. Some underlying diagnoses are overarching in their effect on decision-making. Some with short life expectancies or predictable adverse effects from anesthesia may preclude surgical treatment. Others, like neurofibromatosis, have predictably high rates of fusion failure and dictate a modified surgical approach. Associated cardiac or pulmonary disease may dictate early surgical intervention before predictable decline in cardiopulmonary function precludes spinal surgery. Although pediatric spinal deformity patients with complex diagnoses inevitably have the correct medical subspecialists participating in their care and decision-making, the surgeon still needs to understand the pathophysiology well enough to make the best decision for that patient.
Understand the Natural History and Long-term Consequences of the Deformity
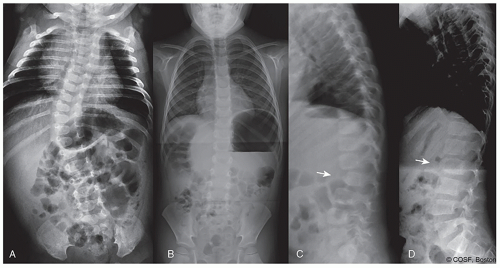
The rate and timing of progression vary widely in pediatric spine deformity with differing diagnoses and ages. Accurately predicting the future of a deformity with a particular diagnosis is challenging, but made more likely by a thorough knowledge of the natural history of that particular diagnosis. For example, spontaneous improvement is likely in infantile idiopathic scoliosis (IIS) with a low rib-vertebral angle difference (RVAD) or in developmental thoracolumbar kyphosis (Figure 1.2), while progression of a dysplastic kyphoscoliosis in neurofibromatosis in the preadolescent growth spurt is inevitable. Many congenital deformities progress during rapid growth in the first 3 years of life, remain stable through the remainder of childhood, and then progress again with the early adolescent growth spurt (Figure 1.1). Knowledge of these diagnosis-specific natural histories permits accurate timing of intervention and avoids unnecessary treatment. Deformity behavior after growth is similarly dependent upon underlying diagnosis. Localized congenital deformity within the thorax likely remains stable after growth in spite of a large Cobb angle, while a thoracolumbar curve with a lesser magnitude in a connective tissue disorder will steadily progress after growth. Neuromuscular patients with poor core muscle strength may likewise progress steadily after maturity. Measuring deformity Cobb angle is an incomplete predictor in pediatric spine deformity. Only by knowing the natural history of the individual diagnosis can we make appropriate surgical choices.
Understand the Response to Nonsurgical Treatment
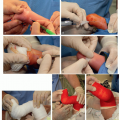
Part of surgical decision-making is choosing when or if to pursue nonoperative, orthotic treatment for a deformity, even if surgery is likely the ultimate goal. An intimate knowledge of brace treatment of spinal deformities affords the pediatric spine surgeon the best chance to make the appropriate surgical decision and timing. The potential response to brace treatment for different diagnoses varies widely from curative, to temporary curve control with growth, or to actually causing harm. Some significant portion of IIS can be cured with casting, some juvenile idiopathic scoliosis (JIS) reversed and held with bracing, and some adolescent idiopathic curves permanently improved with brace treatment. In
neuromuscular curves, orthoses may slow curve progression, but in some, they also provide the much needed torso support for sitting and improved upper extremity function. In others, spinal orthoses may inhibit adequate respiratory function, enhance the risk of aspiration, exacerbate gastroesophageal reflux, or worsen heat intolerance. In congenital scoliosis, casting and bracing cannot cure the underlying deformity but may well buy time and permit spine growth while limiting progression of deformity, particularly in the normally segmented parts of the spine. Knowing how a particular diagnosis and deformity may respond to nonsurgical treatment is critical and factors into surgical decision-making.
neuromuscular curves, orthoses may slow curve progression, but in some, they also provide the much needed torso support for sitting and improved upper extremity function. In others, spinal orthoses may inhibit adequate respiratory function, enhance the risk of aspiration, exacerbate gastroesophageal reflux, or worsen heat intolerance. In congenital scoliosis, casting and bracing cannot cure the underlying deformity but may well buy time and permit spine growth while limiting progression of deformity, particularly in the normally segmented parts of the spine. Knowing how a particular diagnosis and deformity may respond to nonsurgical treatment is critical and factors into surgical decision-making.
Are There Secondary Effects of the Deformity?
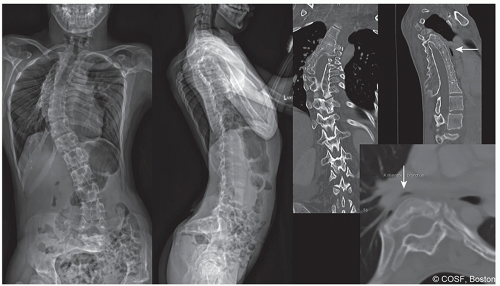
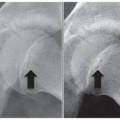
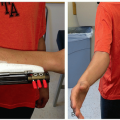
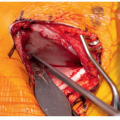
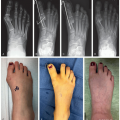
The secondary effects of the spinal deformity may be of greater or equal significance than the spine curvature itself (Figure 1.3). The interrelationship between the evolution of thoracic early onset scoliosis (EOS) and chest wall deformity leading to thoracic insufficiency syndrome (TIS) is an excellent example where the long-term effect on chest wall shape, lung development, and mechanics of thoracic function are often more problematic than the spine curve itself (Figure 1.4). Avoidance of TIS, a secondary effect, often drives surgical decision-making in EOS. Localized congenital or other curves may have a profound negative effect on the adjacent, previously normal spine (Figure 1.5). An abrupt upper lumbar congenital kyphosis or the thoracolumbar kyphosis associated with bone dysplasias or storage disorders may with time produce permanent thoracic lordosis above or painful hyperlordosis below. Persistent severe pelvic obliquity from lumbar scoliosis in the young child may effectively uncover one hip, contributing to hip dysplasia (Figure 1.6). Persistent pelvic obliquity in the nonambulatory neuromuscular patient reinforces the trend toward hip subluxation and adduction contracture. Surgical decision-making needs therefore to take into account the possible permanent effect of the evolving deformity on the rest of the spine and adjacent structures, not just the spine alone.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree