Neuromuscular Hip Surgery: Prevention to Reconstruction
Benjamin J. Shore
Neuromuscular Hip Surgery: Prevention
Adductor longus lengthening
Adductor brevis lengthening
Gracilis lengthening
Iliopsoas lengthening
Application of phenol to the anterior branch of the obturator nerve
Operative Indications
Progressive hip subluxation as measured on plain radiography (anteroposterior [AP] pelvis), migration percentage (MP) greater than 30% and less than 50% with minimal bony deformity
Progressive loss of hip abduction or presence of hip adduction or flexion contracture which affects activities of daily living (diapering, cleaning, etc)
Scissoring which is affecting gait or standing tolerance
Given the natural history of untreated neuromuscular hip subluxation, the ultimate goal is to prevent the development of hip arthritis and maintain a flexible pain-free hip which remains in the acetabular socket
Preventative surgery is indicated for younger children with progressive hip subluxation
MP is monitored every 3 to 6 months, and gradual increase greater 40% is an indication for preventative surgery
Children younger than 4 years with MP greater than 50% can still be indicated for preventative surgery, where preventative surgery is considered a bridge to “buy time” for a more definitive reconstructive procedure when the child is older and better suited to tolerate said intervention
Preventative surgery in those younger than 4 years often can help address increasing hip percentage MP and increasing difficulties with activities of daily living (ADLS) due to scissoring
Surgery and dose of prevention is tailored to the child’s age, functional level, and degree of subluxation
Preventative surgery is often included at the time of reconstruction
Results of preventative surgery are best in those children with the greatest functional potential (Gross Motor Function Classification System [GMFCS] levels II and III) and worse in those children with limited ambulatory potential (GMFCS IV and V)
While percutaneous lengthening has been described, it is not something we endorse due to the relative inaccuracy of the surgical dosing
Equipment
Regular table
Supine positioning
Waterproof covering for the perineal area to prep into the surgical field
Impervious dressing below the knees to limit surgical field
5% phenol is used for the anterior branch of the obturator nerve
Right angle retractors (Ragnell or Langenbecks) and peanuts are helpful for deep dissection around the iliopsoas
Monocryl for dressing and Dermabond to make incision waterproof
Examination Under Anesthesia
Examination with the child asleep is helpful to differentiate muscle spasticity from contracture
Examine the hips in flexion to test adductor longus and adductor brevis muscles and in extension to test the gracilis muscle
The goal is to have a hip abduction of 45° after surgical lengthening in flexion and extension if possible. If still less than 45° of abduction after adductor longus lengthening, then consider partial or complete myotomy of adductor brevis
Presence of a hip flexion contracture greater than 20° as measured using the Thomas test is an indication for iliopsoas lengthening
Positioning
Supine
Towel under buttocks to elevate slightly, can also accomplish on a stack of linen to elevate child off the table if additional procedures are being performed
Position yourself opposite to the side you are operating on
Arms are folded across the chest so that anesthesia has access if needed
Upper body Bair Hugger to keep patient warm
Surgical Approach
The adductor longus is the “lighthouse” to the medial incision, so before you cut it make sure that you have identified this muscle as well as the adjacent muscles to confirm your location and orientation
Be wary of revision adductor lengthening procedures as the anatomy can be distorted and large vessels may be in close proximity to your surgical approach
Orientation of the anatomy is as follows—adductor longus is most palpable and small tendon which is easily seen inserting onto the tubercle. The inferior border of the tendon is often the easiest to define surgically with a combination of sharp and blunt dissection. The inferior border will help you identify the adductor brevis which is lying below
Superior to adductor longs lies the muscle interval between adductor longs and pectineus. The interval between adductor longus and pectineus is easier to exploit at the medial border close to the pubic tubercle, the more lateral one dissects within the interval typically involves crossing blood vessels making the dissection more challenging
Deep to the interval of pectineus and adductor longus lies the anterior branch of the obturator nerve which is lying on the muscle belly of the adductor brevis. The nerve is exiting from the obturator foramen and arborizes into several branches on the belly of the adductor brevis muscle as you go more lateral from the foramen
Working deep through the interval of adductor longus and pectineus will take you to the level of the lesser trochanter and iliopsoas tendon. The anterior branch of the obturator nerve is retracted on the belly of the adductor brevis which lies inferior in the above interval. Occasionally, branches of the medial femoral circumflex vessel will be seen but often can be avoided as they tend run in a cranial-caudal direction more medial than the lesser trochanter
Adductor Longus Tenotomy
A 4-cm incision is made about 1 fingerbreadth lateral to the adductor tubercle
Center the incision over the adductor longus tendon which can be made tight with flexion and abduction of the leg. Typically, position both legs in a flexed abducted position to tension both adductor longus tendons simultaneously
Use the skin knife for skin but go to cautery thereafter to limit bleeding
Insert a small self-retainer and army navy retractors to facilitate visualization and exposure
Incise with cautery along the length of the adductor longus tendon until you can see the fibers of the muscle and white of the tendon at the insertion to the tubercle
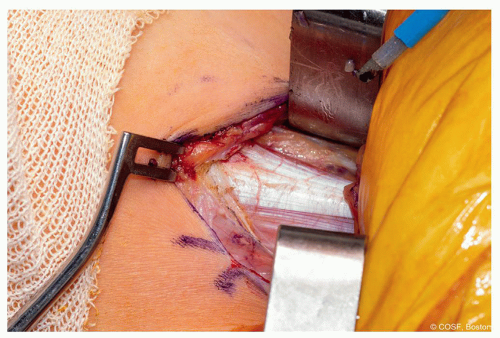
Typically, identify the cranial and caudal borders of the adductor longus tendon and with an army navy retractor retract the tendon superiorly and inferiorly to confirm that you are around the tendon completely (Figure 37.1)
If you are in the correct location when you retract the adductor longus tendon superiorly, you should see the branches of the anterior obturator nerve on the brevis below
A right angle retractor is used to identify the adductor longus tendon, and full tenotomy is made close to the tubercle in the tendon to limit bleeding
Adductor Brevis Lengthening
Using the same incision as mentioned above, the adductor brevis is lengthened
Adductor brevis is a broader muscle, and rarely a complete release of brevis is indicated
Adductor brevis lengthening is rarely indicated for GMFCS I and II children and commonly indicated for GMFCS IV and V children
Tension of the adductor brevis is made with the leg in flexion and adduction, similar as for longus
If after lengthening the adductor longus, one has not achieved 40 degrees of hip abduction, then adductor brevis lengthening is pursued
Lengthening of the adductor brevis is more of a fascial striping of the tight musculature with continued tension of the leg in abduction and flexion
Be mindful of the anterior branch of the obturator nerve, and perform your lengthening close to the adductor tubercle to avoid iatrogenic nerve injury
Gracilis Lengthening
Gracilis lengthening is often indicated as this is a muscle which crosses the hip and knee and if frequently tight in children with cerebral palsy
The lengthening of the gracilis can be done through the same incision as previously described for the adductor lengthening
The gracilis muscle has a unique shape and is quite “gracile” or long and thin, which allows for easy identification in the surgical wound (Figure 37.2)
The gracilis is identified by placing the leg into extension and abduction, which makes the gracilis muscles quite tight and easy to identify in the caudal aspect of the adductor incision
Once the tendon is identified, electrocautery is used to open the superior aspect of the sheath of the tendon, and then cranial and caudal dissection is performed to open the sheath and identify the extent of the tendon
The gracilis is a long and thin muscle with a broad insertion on the tubercle
As a result, a right ankle clamp is NOT passed around the tendon, rather with abduction and extension, progressive release of the tendon is performed with electrocautery and palpation until the remaining inferior aspects of the tendon are completely released from the tubercle
Iliopsoas Lengthening at the Lesser Trochanter
If a hip flexion contracture of greater than 20° is present or there is evidence of hip subluxation, release of the iliopsoas at the lesser trochanter through the adductor incision can aid in seating of the hip in the acetabulum
The interval between the pectineus and adductor brevis muscles are exploited; lengthening of the iliopsoas is easier if done PRIOR to adductor brevis lengthening
Keep the anterior branch of the obturator nerve on the adductor brevis and retract inferiorly to access the lesser trochanter
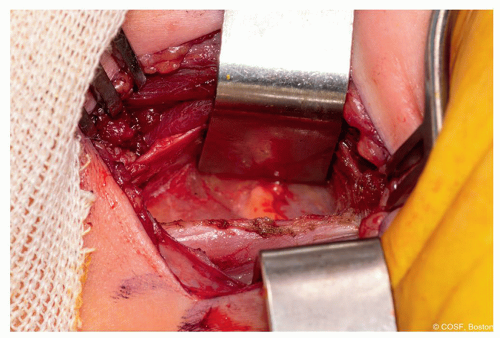
Using a combination of sharp and blunt dissection with deep Ragnell retractors, the interval is easily identified to the level of the lesser trochanter (Figure 37.3)
Digital palpation of the lesser trochanter is helpful at this stage to orientate the surgeon
Using a combination of electrocautery and peanuts, the soft tissue overlying the iliopsoas tendon is released through pressure and sweeping in-line with the tendon toward the ipsilateral nipple
Once the tendon is identified, there are some small vessels which are seen on the base of the tendon as it inserts into the lesser which can be cauterized prophylactically
The hip is placed in flexion and external rotation to deliver the lesser trochanter into the wound and facilitate passage of the right angle retractor
A complete tenotomy of the iliopsoas is made under direct visualization with electrocautery
Application of Phenol to the Anterior Branch of the Obturator Nerve
The anterior branch of the obturator nerve is a pure motor nerve responsible for adduction of the leg
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree