Soft tissue augmentation is currently the second most common minimally invasive aesthetic procedure in the United States.
Numerous soft tissue fillers are commercially available, but the most commonly used products are made of hyaluronic acid.
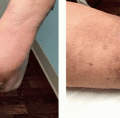
Soft tissue augmentation is most commonly performed on the face; other anatomic locations include the dorsal hands and genitalia.
Common adverse events include edema and ecchymosis. Serious adverse events include vascular occlusion, resulting in tissue necrosis, blindness, and central nervous system sequelae.
Strong understanding of anatomy and appropriate training of the injector are paramount to prevent complications and maximize aesthetic results.
tissue augmentation, which led to the utilization of liquid injectable silicone products in the 1950s.5 With the early liquid injectable silicone products, there were issues with purity and the formation of granulomas, foreign body reactions, and extrusion of the product through the skin.6 Due to these adverse events, the Food and Drug Administration (FDA) banned the sale of injectable liquid silicone for aesthetic purposes in the 1960s.5 These issues prompted the search for other injectable products and ultimately the creation of collagen products in the 1970s.6 The first collagen injectable was bovine collagen; however, it only had short-lived results. Additionally, skin testing was required prior to use of bovine collagen fillers to identify those at risk for allergic reactions. These concerns led to the development of additional soft tissue fillers, including some hyaluronic fillers, in the 1990s and early 2000s.6
TABLE 3.1 Commercially Available Fillers in the United States | |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
the subcutaneous tissue and the water is absorbed by the body.7,28 The particles in the subcutis are treated as small foreign bodies similar to PMMA, which induces fibrosis and collagenesis.5,6,7,28 It is important to keep this in mind as the injections are being performed because the patient will lose some volume initially as the water is resorbed and then will gain more volume over the following several months with collagenesis.7,28 Techniques to avoid clogging the needle while injecting the PLLA suspension include using a 25-gauge needle or a wider cannula for injection, reconstituting the particles with larger volumes than recommended by the package insert, storage of the reconstituted product for 48 to 72 hours before injection, and thorough remixing of the product suspension just prior to injection.7,28
dissolve CaHA filler in cadaveric porcine skin samples.36 Rullan et al. applied these concepts to two patient cases and illustrated the utility of intralesional sodium thiosulfate to dissolve CaHA nodules in vivo.37 The durability of results from CaHA is typically 1 to 2 years depending on the site injected.5,6,7,32 CaHA has a radio-opaque appearance on x-ray and CT images because it is composed of a constituent of the bone.7
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree