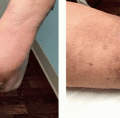
Microdermabrasion utilizes mild mechanical abrasion to resurface the outer epidermis, promoting skin rejuvenation and enhancing cosmesis.
Cellulite is a common complaint of the female aesthetic patient; treatments include topicals, injectables, subcision, and the use of various energy-based devices.
Microneedling is an aesthetic technique that uses focal tissue injury to stimulate remodeling and neocollagenesis.
Platelet-rich plasma has numerous uses in the aesthetic medicine, including for rejuvenation, treatment of alopecia, and improvement in the appearance of scars.
these devices are often considered less aggressive than in-office systems, patients should consider completing a pretreatment visit with a board-certified dermatologist to ensure they are an appropriate candidate.
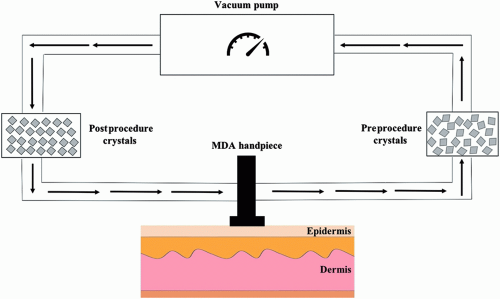 FIGURE 10.1 Schematic depicting a typical microdermabrasion device. (Image courtesy of Ronda S. Farah, MD, University of Minnesota, Department of Dermatology, MN, USA.) |
TABLE 10.1 Comparison of Crystal and Crystal-free Devices | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
indications, alternatives, risks, and benefits; it is also critical to set realistic expectations prior to a patient’s first treatment session. Furthermore, a thorough medical history and skin examination should be conducted to ensure there are no major contraindications to treatment.
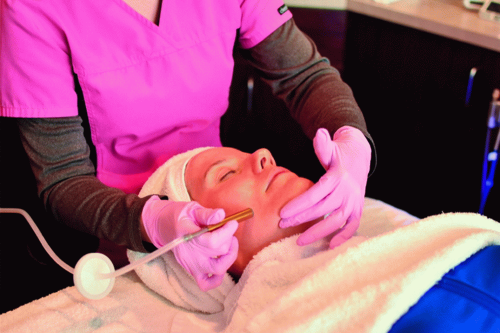 FIGURE 10.2 Photograph depicting a typical microdermabrasion procedure. (Courtesy of Dr. Charles E Crutchfield III, Crutchfield Dermatology, Eagan, MN.) |
TABLE 10.2 Description of Typical Microdermabrasion Preparations and Treatment Techniques | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
may result if the patient has particularly thin skin or is taking an antiplatelet agent or anticoagulant at time of the procedure. Scarring and abrasions are rare but may occur if MDA is performed with overly aggressive treatment settings. As with any skin procedure, physicians should caution patients on the risks of hypo- and hyperpigmentation. Autoinoculation of viral infections (e.g., herpes simplex virus, warts, molluscum contagiosum) may occur; certain authors suggest pretreatment prophylaxis with acyclovir or valacyclovir among patients with a history of herpes simplex or varicella infection.14 Devices should always be cleaned thoroughly or sterilized after use to avoid transmission of infectious disease. For staff members, there has been suggestion that inhalation of aluminum oxide crystals may be related to risk of fibrotic lung disease or Alzheimer dementia. Further research is needed to identify a direct relationship.9,19
of 18 and 45 years, 70% of all participants reported that cellulite “hampered their lives greatly.”34 Published in abstract form and also published in Cellulite: Pathophysiology and Treatment by Goldman, Hexsel et al. again evaluated 50 female volunteers and found that cellulite caused women to restrict their outdoor activities, types of clothes worn, resulted in feelings of poor self-esteem, and caused fear of spouses’ attention and judgment.35 However, full details of this study are not available. Additional studies needed to quantify cellulite’s effect of quality on life are needed.
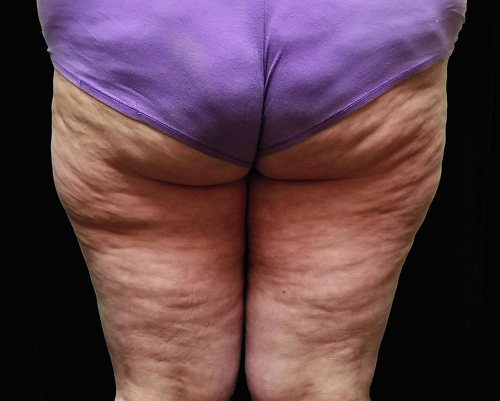 FIGURE 10.3 This image illustrates a 34-year-old female with cellulite, displaying uneven dimpling and nodularity. (Courtesy of Dr. Charles E Crutchfield III, Crutchfield Dermatology, Eagan, MN.) |
cellulite in men.30,31,32,33 During the physical examination, the area of skin suspected to have cellulite should be evaluated by the clinician in an effort to differentiate it from obesity or other cellulite-mimicking processes. While obesity and cellulite may appear similar, cellulite tends to occur more so in the skin of the abdomen, pelvic region, buttocks, and lower extremities.27 Other abnormalities that can appear similar to cellulite and should be considered in the differential diagnosis include lipoedema, lymphedema, lipoatrophy, or infragluteal folds.31,50 It is important for physicians to understand the differences between cellulite and skin findings associated with cellulite-mimicking processes, as treatments for cellulite can lead to worsening of other skin conditions.31
| ||||||||||||
rollers, aims to mobilize deep tissue and subcutaneous fat by providing negative pressure and tissue manipulation.57,58 The typical treatment regimen consists of ten 45-minute sessions twice a week, until an improvement in cellulite appearance is seen.30,57,58 Despite being a popular treatment for cellulite, data on efficacy are limited. Some studies show mild improvement in cellulite,57,58 while others show no statistically significant difference.59 Collis et al. conducted a study on 52 women with cellulite, randomizing them to two treatment arms consisting of Endermologie® and topical aminophylline cream. Only 10 of 35 women treated with Endermologie® had improvement in cellulite appearance when assessed by study subjects. No statistical significance was found for either topical aminophylline cream or Endermologie®.59 Evaluation for improvement by investigators did not reach this level of efficacy. Kutlubay et al. describe a statistically significant reduction in cellulite grade, as well as in mean body circumference. Gulec also demonstrated a mild statistically significant reduction in cellulite grade. Patient’s weight loss and hydration status may also be impacting the results of these studies; Additional studies are needed to delineate efficacy of this therapy.
TABLE 10.4 Cellulite Treatments at a Glancea | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree