Laser and Light Devices in Aesthetic Medicine
Jordan V. Wang, MD, MBE, MBA
Nazanin Saedi, MD
Chapter Highlights
The use of laser, light, and energy-based devices in aesthetic medicine has grown exponentially in recent years.
Intense pulsed light is one of the most versatile and widely used devices in aesthetic dermatology, with applications for treatment of photoaging, telangiectasias, hair removal, and a variety of other skin conditions.
Selective photothermolysis is the process by which laser therapy uses a particular wavelength of energy to target a specific structure within tissue.
Aesthetic lasers include ablative and nonablative devices, both of which can be fractionated to decrease downtime.
In addition to laser and light devices, energy devices utilizing radiofrequency, ultrasound, and microwave technologies have aesthetic applications.
The field of aesthetic medicine has continued to grow in recent years, especially as the technology behind laser, light, and energy-based devices has further developed. What were once considered revolutionary and pioneering procedures have evolved to become the mainstays of modern cosmetic treatment. In 2017, members of the American Society for Dermatologic Surgery (ASDS) performed nearly 3.3 million laser, light, and energy-based procedures, which was greatly increased from the 2 million procedures in 2012.1 With the widespread adoption and routine use of these devices, aesthetic practitioners should be familiar with the technologies that are commonly utilized in the field. This chapter will provide an overview of the laser, light, and energy-based devices commonly used in aesthetic medicine.
The use of laser technology in aesthetic medicine dates back to the 1960s when Theodore Maiman developed the first laser for clinical application. Several years later, Dr Leon Goldman demonstrated the use of lasers for several dermatologic applications, including
tattoo removal and skin lesion destruction. In the 1980s, Drs R. Rox Anderson and John Parrish published the theory of selective photothermolysis, a process by which a wavelength of a particular energy can be used to selectively target and destroy a particular structure within the skin.2,3 Since that time, the dermatologic armamentarium has exponentially expanded to include a myriad of laser, light, and energy-based devices with applications for use in aesthetic dermatology.
tattoo removal and skin lesion destruction. In the 1980s, Drs R. Rox Anderson and John Parrish published the theory of selective photothermolysis, a process by which a wavelength of a particular energy can be used to selectively target and destroy a particular structure within the skin.2,3 Since that time, the dermatologic armamentarium has exponentially expanded to include a myriad of laser, light, and energy-based devices with applications for use in aesthetic dermatology.
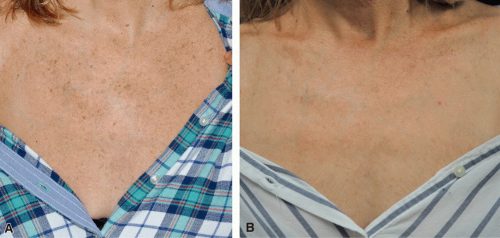
The intense pulsed light (IPL) device is one of the most commonly used and versatile devices in aesthetic medicine. The IPL technology utilizes a xenon flashlamp to emit an intense, broad-spectrum pulse of visible light, usually in the range of the electromagnetic spectrum of 400 to 1200 nm. Cooling of the epidermis with the contact method, aqueous gel, and/or exogenous forced chilled air is important to protect the overlying epidermis during treatment. In contrast to a laser which emits a single wavelength of energy, IPL can be used to treat numerous skin conditions due to the broad range of wavelengths emitted during therapy. However, this nonselectivity is the very reason why IPL is not typically a perfect treatment for any one specific skin disorder. Since IPL can improve a range of skin complaints, including telangiectasias and dyspigmentation, it is often used to treat cutaneous signs of photodamage (Figure 4.1). Studies have reported about 50% to 75% improvement in both the vascular and pigmented components with a relatively low and tolerable side effect profile.4 Cutoff filters can also be utilized to target specific structures and chromophores, such as 550- or 560-nm filter for treatment of telangiectasias. Other common uses of IPL include photoepilation, or hair removal, acne vulgaris, rosacea, and melasma. Practitioners must ensure proper overlap of pulses in order to avoid “striping”, which can manifest in the presence of untreated skin between the treated areas. Striping can be especially seen with single-pass treatment techniques; using multiple passes that
are oriented at different angles can help to ameliorate this risk. Caution should be used in darker skin types or tanned skin, as these patients are more likely to experience cutaneous burns and pigment alterations with IPL therapy. Patient comfort is typically achieved with contact cooling or topical anesthesia alone. For the majority of indications, a series of IPL treatments are needed to achieve the desired outcome. Treatments typically occur at 4 to 6 week intervals until optimal results are achieved, and touch-ups may be needed every few months thereafter.
are oriented at different angles can help to ameliorate this risk. Caution should be used in darker skin types or tanned skin, as these patients are more likely to experience cutaneous burns and pigment alterations with IPL therapy. Patient comfort is typically achieved with contact cooling or topical anesthesia alone. For the majority of indications, a series of IPL treatments are needed to achieve the desired outcome. Treatments typically occur at 4 to 6 week intervals until optimal results are achieved, and touch-ups may be needed every few months thereafter.
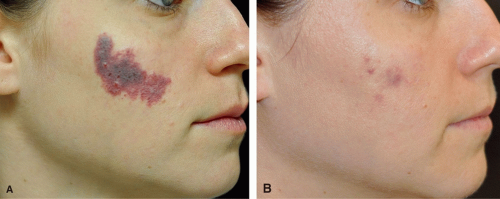
Vascular lesions are common complaints of aesthetic patients. Such concerns can include background erythema, telangiectasias, poikiloderma of Civatte, small leg veins, and port wine stains. Traditionally, the pulsed dye laser (PDL) has been the prototypical laser for these concerns (Figure 4.2). However, other lasers can be used, including the 532-nm potassium titanyl phosphate (KTP) laser, the 755-nm alexandrite laser, and the 1064-nm neodymium:yttrium-aluminum-garnet (Nd:YAG) laser.
The PDL was first developed to treat capillary malformations and port wine stains, but its use has expanded to the treatment of vascular lesions of various etiologies. The initial lasers emitted a 577-nm light; modern devices emit 585 or 595 nm to allow for deeper tissue penetration (up to 1.2 mm). Treatment parameters can be adjusted to elicit specific responses according to the desired posttreatment downtime and clinical efficacy. For example, shorter pulse durations can cause purpura from intravascular coagulation, but may also be more effective for treating lesions. In contrast, longer pulse durations can offer shorter downtime, but may require multiple treatments to achieve the desired clinical outcome. The addition of pulse stacking can also help to improve clinical efficacy.5 Practitioners must ensure proper overlap of pulses in order to avoid “footprinting”, which appears as a honeycomb-like pattern in the presence of untreated skin between the treated circles. Recently, a 585-nm light has been developed with a diode laser, in order to avoid dye kits, and in combination with a scanning handpiece.6
The KTP laser was originally created by passing the light of a 1064-nm Nd:YAG laser through a KTP crystal, which doubles the frequency and halves the wavelength.7 The resultant wavelength is absorbed competitively by melanin, oxyhemoglobin, and tattoo
pigment. Therefore, postprocedural dyspigmentation can be a side effect, especially when treating skin of color or tanned individuals. For many KTP lasers, a chilled sapphire plate or glass window is utilized in order to provide cooling to the skin surface and to protect from epidermal injury. The small beam diameter often induces fewer side effects than the PDL, including bruising, swelling, pain, and erythema. While long-pulsed PDL was shown to achieve better clearance of facial telangiectasias, patients often preferred multiple treatments with the KTP due to its favorable side effect profile.8
pigment. Therefore, postprocedural dyspigmentation can be a side effect, especially when treating skin of color or tanned individuals. For many KTP lasers, a chilled sapphire plate or glass window is utilized in order to provide cooling to the skin surface and to protect from epidermal injury. The small beam diameter often induces fewer side effects than the PDL, including bruising, swelling, pain, and erythema. While long-pulsed PDL was shown to achieve better clearance of facial telangiectasias, patients often preferred multiple treatments with the KTP due to its favorable side effect profile.8
The Nd:YAG laser is another laser commonly used to treat vascular lesions, due to its deeper penetration and decreased affinity for melanin. However, the 1064-nm wavelength has significantly less hemoglobin absorption than the PDL and KTP lasers, which makes higher fluences or multiple treatments often necessary. The deeper penetration allows for treatment of larger caliber vessels, which are typically darker in color and anatomically deeper within tissue. Examples of appropriate targets include venous lakes on the lips and perialar telangiectasias. The limited absorption by epidermal melanin makes the Nd:YAG safe in darker skin tones, whereas other wavelengths may result in posttreatment pigment alteration in these individuals. When using higher fluences and longer pulse durations, practitioners must be cautious of the potential for volumetric heating and collateral damage to adjacent tissue. This makes the need for cooling even more important in order to protect the epidermis from thermal injury and scarring and to control patient discomfort.
With the widespread adoption of quality-switching, or Q-switch (QS), lasers in the 1980s, the treatment of pigmented skin lesions was revolutionized. These lasers quickly became the standard treatment and remain so even several decades later. With selective photothermolysis, sufficient energy must be delivered to the target chromophore with a pulse duration that is less than or equal to its thermal relaxation time. A strong burst of energy delivered within this small amount of time causes rapid expansion and contraction of the target with subsequent mechanical fragmentation of pigment particles through a photoacoustic effect. The particles of pigment are then released into the extracellular space and eliminated through the lymphatic system.
QS nanosecond lasers provided the ability to appropriately target melanosomes for destruction. QS lasers have traditionally been an effective treatment for lightening lentigines. In medium dark skin tones, lower fluences should be used in order to reduce the risk of post-inflammatory hyper- or hypopigmentation. QS 1064-nm Nd:YAG can also be utilized for darker skin tones. The intended treatment end point is immediate graying or whitening from rapid heating of the target chromophore. The lentigines then darken over several days before lightening or fading away. The treatment of café-au-lait macules is typified by mixed results, and patients must therefore be counseled appropriately. Lesions may initially fade, but typically recur in time. Despite medical and laser advancements, melasma remains a challenging pigmentary disorder to treat with only modest results. While laser therapy may lighten the pigmentation associated with melasma, difficulty remains in achieving long-term remission even with concomitant strict photoprotection and topical lightening agents. Additional larger studies may focus on combining laser treatments for melasma with kojic acid, bakuchiol, and oral, intradermal, and topical tranexamic acid formulations.
Recently, picosecond (PS) lasers have been developed and broadly commercialized for the treatment of pigmented lesions and tattoos. These lasers deliver energy in the picosecond range, which is one-trillionth of a second. Although PS lasers have been available for several years, their prohibitive costs represented a major roadblock to their widespread adoption. The field is just now experiencing an influx of scientific studies in the medical
literature demonstrating their clinical utility.9 PS lasers have been shown to be effective for the treatment of various pigmented lesions and disorders, including solar lentigines, nevus of Ota, melasma, and café-au-lait macules.9,10,11,12,13
literature demonstrating their clinical utility.9 PS lasers have been shown to be effective for the treatment of various pigmented lesions and disorders, including solar lentigines, nevus of Ota, melasma, and café-au-lait macules.9,10,11,12,13
Laser tattoo removal procedures have experienced a recent rise in demand. In 2017, about 85,000 laser, light, and energy-based tattoo removal procedures were performed by ASDS members alone.1 With improved technology and increasing knowledge of the treatment of tattoo pigments, clinical outcomes have continued to improve. The first step in treating tattoos is to properly evaluate the pigment as different pigments preferentially absorb specific wavelengths of light. Therefore, the goal of optimizing treatment is to specifically target the correct color. A rapid rise in temperature of the targeted chromophore leads to a pressure wave that exceeds the tensile strength of the pigment particle, causing it to shatter into smaller fragments. Short pulse durations allow for photoacoustic and photomechanical destruction of pigment while avoiding significant collateral thermal damage. In comparison to melanin, tattoo pigments have a significantly shorter thermal relaxation time, so shorter pulse durations, especially in the picosecond range, may prove to be more efficacious.14,15
For many years, QS nanosecond lasers were considered the standard of care for tattoo removal.16 The most common wavelengths of laser devices for tattoo removal are 1064, 532, 694, and 755 nm.17,18,19 The 1064-nm Nd:YAG laser can treat black, dark blue, and brown tattoos, while the frequency doubled 532 nm can treat brown, red, orange, and yellow tattoos. The 755-nm alexandrite laser can effectively treat black, blue, and green colors, while the 694-nm ruby laser can remove black, blue, green, and purple. Some colors are known to offer variable results, including purple, green, yellow, and red. Flesh-colored pigments are notoriously difficult to treat. A common phenomenon that can occur with their treatment is paradoxical darkening immediately after a single laser pulse. This is caused by a shift from an oxidized to a reduced state in the tattoo pigment.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree