Hair Loss: Established Treatments and Emerging Therapies
Hair Loss: Established Treatments and Emerging Therapies
Marc Avram, MD
Nikhil Shyam, MD
Hair loss, or alopecia, affects a significant proportion of the world’s population and can have numerous psychological and social consequences. Alopecia is known to be associated with depression, introversion, and lower self-esteem. While there are several different types of hair loss, they are broadly categorized into two forms: nonscarring (preservation of hair follicles) and scarring (loss of follicular ostia). The most common type of hair loss is androgenetic alopecia (AGA) and affects 80% of men and 50% of women in the course of their lifetime.
1,2,3

ANDROGENETIC ALOPECIA
AGA is an androgen-dependent loss of hair that occurs in genetically predisposed men and women. Androgens, specifically dihydrotestosterone (DHT), have been shown to play an important role in the progression of AGA. Testosterone is converted to DHT by the type II isoenzyme of 5-alpha reductase that is expressed in the dermal papillae of hair follicles. Elevated levels of DHT result in many of the classic features of AGA including miniaturization of terminal hairs to vellus-like hairs and a prolonged telogen phase with shortening of the anagen growth phase.
4,5,6 Several androgen receptor
polymorphisms have been noted, highlighting a polygenetic condition as well as an autosomal dominant inheritance.
7,8 Several studies have also reported single-nucleotide polymorphisms at different genomic loci associated with hair loss, including the AR/EDA2R locus and 20p11 locus.
9 Clinically, men and women often exhibit different patterns of hair loss that have been described as male pattern hair loss (MPHL) and female pattern hair loss (FPHL), respectively. However, overlap in terms of distribution of hair loss may occur as well.
Male Pattern Hair Loss
Androgen-dependent hair loss is well established in men and typically presents with gradual thinning of hairs in the vertex scalp along with recession of the frontotemporal hairline. Typically, the occipital and parietal scalp remain unaffected. Classically, the Hamilton-Norwood scale (
Figure 6.1) is utilized to describe the severity of MPHL.
Diagnosis is usually made through clinical history and physical exam with notable decreased density of hairs in the bitemporal and vertex scalp with prominent sparing of occipital and parietal areas.
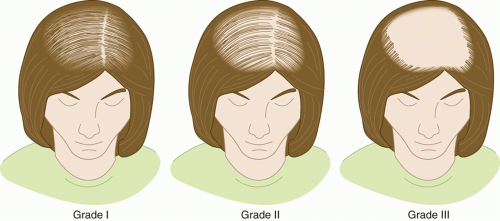
Female Pattern Hair Loss
The role of androgens in the progression of FPHL is less well established. However, there is a strong genetic predisposition with 40% to 54% of patients reporting family history of pattern hair loss. The frequency of FPHL increases with age with 12% of women reporting symptoms by age 29%, 25% by 49 years, and >50% by 79 years.
10While FPHL and MPHL share a similar pathology resulting in progressive follicular miniaturization of terminal to vellus hairs and decreased anagen growth phase, the etiology of FPHL remains unclear. Interestingly, unlike MPHL, miniaturization in FPHL is not uniform and intense with relatively few areas of complete alopecia. While androgens are a primary driver of MPHL, many women with FPHL do not have elevated androgens. However, a genetic predisposition may exist whereby normal circulating levels of androgens act on follicular receptors that are highly sensitized. In addition, androgen-independent pathways may also exist that have yet to be elucidated.
11,12,13Polycystic ovarian syndrome and metabolic syndrome are the two most commonly associated comorbidities noted with FPHL. The association of decreased iron levels and thyroid disorders has also been associated with FPHL. Some studies have shown that antiandrogen therapy is more efficacious in patients with ferritin levels >40 µg/L.
14,15The diagnosis of FPHL is largely based on clinical history and physical exam. Details including when the hair loss started, whether it was gradual or sudden onset, and any associated physical, mental, or emotional stressors within the prior 3 to 6 months of hair loss are important to rule out acute and chronic telogen effluvium. Details regarding possible signs of hyperandrogenism including hirsutism, menstrual irregularities, acne, infertility, and ovarian abnormalities should be ascertained as positive findings and may necessitate laboratory workup. The physical exam is usually notable for widening of the central part with diffuse reduction in hair density over the frontal scalp (
Figure 6.2). If there is any question regarding the diagnosis of hair loss, a scalp biopsy can provide valuable information.

ESTABLISHED TREATMENTS OF ANDROGENETIC ALOPECIA
Get Clinical Tree app for offline access