Introduction
The endocrine system is central to coordinating the systemic response to burn trauma ( Tables 19.1 and 19.2 ). Pathologic and salutary changes are seen in the hypothalamic-pituitary-adrenal (HPA) axis, and thyroid, pancreatic, and gonadal hormonal secretions. These changes act in concert with the humoral effects of cytokines and other immunologic mediators discussed in the chapters on burn edema ( Chapter 7 ) and multisystem organ failure ( Chapter 24 ). They mediate the innate adaptive (stress) response critical to survival in patients, particularly those who recover without medical treatment. In patients receiving medical treatment, they often prove maladaptive. Understanding these fundamental responses is central to the appropriate application of critical care to burned and traumatized patients.
Table 19.1
Influence of Catecholamines on Cardiovascular, Metabolic, and Immune Response to Thermal Injury
| Physiologic Variable | Sympathetic-Mediated Change After Burn Injury |
|---|---|
| Resting metabolic rate | Increase |
| Increase | |
| Increase | |
| Increase (in vitro) | |
| Proteolysis | No change (urea production) |
| No change (protein oxidation) | |
| Decrease | |
| Glucose production and oxidation | Decrease secondary to increase in lipid catabolism , |
| No change | |
| Glycogenolysis | Increase (indirect evidence via cAMP) |
| Gluconeogenesis | Increase (indirect evidence via cAMP) |
| Lipolysis | Increase |
| Increase | |
| Increase | |
| Increase | |
| Cardiac output | Increase |
| Increase | |
| Peripheral vascular resistance | Unknown |
| Heart rate | Increase |
| Increase | |
| T-cell number and function | Unknown |
| B-cell number and function | Unknown |
| Neutrophil number and function | Decrease |
| Monocyte number and function | Increase (indirect; clonogenic potential) |
| Increase (indirect; clonogenic potential) | |
| Increase , |
Citation of studies from the current literature suggesting that sympathetic activation is involved in changing the listed physiologic variables following thermal injury.
Table 19.2
Influence of Glucocorticoids on Metabolic and Immune Response to Thermal Injury
| Physiologic Variable | Glucocorticoid-Mediated Change Following Burn Injury |
|---|---|
| Resting energy expenditure | Increased |
| Oxygen consumption | Increased , |
| Primary fuel | Lipids, glucose |
| Proteolysis | Increased in skeletal muscle |
| Acute-phase protein synthesis | Increased |
| Nitrogen excretion | Increased |
| Glycogenolysis | Increased via effect on glucagon , |
| Gluconeogenesis | Increased , , |
| Lipolysis | Increased |
| Ketone body formation | Normal |
| Triglyceride level | Increased , |
|
|
|
|
| Monocyte population | Increased transiently with corticosteroids but decreased in burn patients , , |
|
Suppressed |
|
Suppressed , |
| Bone formation | Decreased |
Citation of studies from the current literature suggesting that glucocorticoid release is involved in changing the listed physiologic variables following thermal injury.
Normal hypothalamic-pituitary-adrenal axis
The physiologic response of the HPA axis begins with the hypothalamic release of corticotrophin-releasing hormone (CRH) into the hypophyseal portal system, which mediates the release of adrenocorticotrophic hormone (ACTH) from the anterior pituitary. This, in turn, stimulates the synthesis and release of cortisol from the adrenal cortex zona fasciculata. The system is conditioned by hypothalamic afferent and efferent connections that are numerous and diverse in physiologic input and effect, respectively. The hypothalamus is the fountainhead of the autonomic nervous system, being its most rostral component. Hypothalamic nuclei originate central outflow, primarily via the dorsal longitudinal fasciculus, to numerous caudal central autonomic centers (pain modulation, heart rate, respiration, blood pressure, salivation, and the dorsal motor nucleus of the vagus) and to the intermediolateral cell column of the thoracic cord, which includes sympathetic nervous system (SNS) afferents to the adrenal glands. Hypothalamic stimulation thus initiates the release of epinephrine and norepinephrine from the chromaffin cells of the adrenal medulla, which essentially are modified postsynaptic neurons. The action of these hormones and neurotransmitters is traditionally thought to facilitate adaptation to changing conditions. As the terminal signal transducer of the global stress response, the adrenal glands function as two distinct parts: the cortex that produces steroid hormones and the medulla that secretes catecholamines. Both are critical to weathering the systemic storm and orchestrating the balancing organism response required to survive a massive injury.
The cellular and biochemical pathways through which catecholamines work these organism-level alterations are an area of active study. Here we discuss the pathologic alterations in these systems and how they relate to modern critical care and the remainder of the endocrine response.
Strong sympathetic activation after burn trauma
The catecholamine surge after burn trauma was reported in landmark papers in 1957 demonstrating marked elevations in 24-hour urine levels of norepinephrine and epinephrine proportional to burn size, highest in the first 3 days and remaining elevated for weeks. , Herndon et al. repeated these studies, finding sustained elevation in urinary epinephrine and norepinephrine levels past 35 weeks in pediatric burn patients. , Jeschke et al. subsequently demonstrated that cortisol, catecholamines, and metabolic rate are significantly elevated up to 3 years after severe burn injury. In light of the decades of evidence for sympathetic activation after thermal injury, it is critical to understand the resultant physiologic effects.
Cardiovascular response
The chapters on multisystem organ failure and shock describe the physiology of the “ebb” phase from distributive shock and myocardial changes by which cardiac function is depressed. By 48 hours postburn, the myocardium becomes hyperdynamic in a β-adrenergic–mediated manner transitioning to the “flow phase.” , Even small burns are associated with significant changes in cardiac function and possibly long-term pathologic changes.
With the onset of burn shock/postburn physiology, a sympathetic reflex arc begins when hypotension stimulates baroreceptor (carotid sinus and aortic arch) afferent nerve activity, with resultant increases in efferent sympathetic outflow. This sympathetic signal for peripheral vasoconstriction and consequent increase in peripheral vascular resistance is mediated in part by the stimulated release of adrenomedullary norepinephrine. Angiotensin II (AII) and arginine vasopressin (AVP) also act to increase vascular tone. , Additionally a complex interplay of AII and the autonomic nervous system further modulates vascular tone. Concurrently, AVP has been shown to reversibly depress myocardial function in the isolated heart. AVP, wound-derived factors including thromboxanes, and the initial catecholamine storm triggered by burn injury thus conspire with the profound and progressive fluid shifts (losses) of burn injury. This shock state is characterized by a “triple jeopardy” of increased peripheral vascular resistance, depressed cardiac contractility, and intravascular volume depletion. This combination attempts to sustain a deleterious feed-forward event and permit a potentially fatal state of burn shock during the “ebb” phase. , Painful experience has taught that survivors successfully transition to a hypermetabolic, hyperthermic, hyperdynamic, high-cardiac output flow state, whereas in the first 96 hours nonsurvivors become progressively poikilothermic and fail to exhibit the necessary increase in biochemical energetic and substrate fluxes necessary to preserve life and support tissue recovery. The progressive cooling-off of potential nonsurvivors reflects an organism-wide, cellular metabolic failure, primarily of oxidative phosphorylation and its attendant heat generation, which gives the striking appearance of the fire of a patient’s life diminishing and, if not rapidly supported, extinguishing. It is no coincidence that the subjects of this chapter are the primary systems that internally regulate metabolism and determine heat flux. Intervening to rebalance these equations preserves life through the initial phase of burn injury; is one of the great success stories of medicine in the latter half of the 20th century; is not always easy; but is possible in nearly every case. It is achieved by supporting internal temperature and permitting reasonably supranormal temperature and always preventing/treating decreases in body temperature. Heat is generated from within the organism metabolically and absorbed or lost environmentally. While insulating the patient from excessive heat loss, heat generation is supported by ensuring adequate substrate availability, which is especially important in malnourished and undernourished individuals. Flow of substrates must be maintained, which is indicated on an organism level by adequate (supranormal) cardiac index, accounting for the triple jeopardy referenced above. This may require complex inotropic and vasodilator support, in addition to exacting hourly resuscitation to maintain intravascular volume without triggering immediate or future volume overload. Bedside echocardiography can rapidly discriminate between a volume problem or a pump problem, but the latter may be due to varying combinations of inappropriate vasoconstriction (excess afterload) and myocardial depression. Other devices (PiCCO and similar), which permit monitoring of real-time parameters such as lung water, systemic vascular resistance, and contractility, can be of assistance in these situations. A useful maxim is that a normal (healthy) cardiovascular system will typically respond to correct fluid resuscitation alone, whereas cardiovascular impairment usually requires advanced, individualized intensive care unit (ICU) hemodynamic support informed by requisite monitoring.
On a tissue level, adequate end-organ perfusion is indicated by improving mental status, adequate urine output, clearance of lactate, stabilization of pH, and the absence of compartment syndromes or mesenteric ischemia. Identification of these tissue- and organ-failure syndromes is not always easy or straightforward, but like burn survival itself, perception of these critical findings is almost always possible. Finally, factors that impair cellular energy flux (usually metabolic poisons) must be identified and addressed; in the burn patient these include carbon monoxide and cyanide exposures, among others. If present, these are often the dominant cause of myocardial dysfunction, which typically will not improve until the intoxication is addressed. Viewed through the above lens, the theory and management of the early phase of burn shock is not dissimilar from the understanding and care required for bushcraft fire-making under adverse conditions; and done in a requisite manner it is similarly rewarding.
As the organism transitions to the “flow phase” around 48 hours after insult, sympathetic outflow is an important driver in maintaining supranormal cardiac function during recovery from thermal injury. In a group of burned patients undergoing visceral blood flow and metabolic measurements, the average cardiac index was 8.2 L/m 2 min. In the same study, liver and kidney metabolic and blood flow measurements were also conducted, and all were found to be elevated. These data allude to the supraphysiologic circulatory need requisite for sustained recovery from severe burn injury. Guillory and Finnerty reviewed the menagerie of animal studies demonstrating the centrality of β-adrenergic (dys)function in mediating this cardiac pathophysiology and have given mechanistic insight into the efficacy of modern burn therapy with β-blockade.
The sympathetic surge continues long after volume status is restored and baroreceptor signaling ends. Despite elevated levels of circulating norepinephrine and epinephrine, and in stark contrast with the earlier “ebb” phase, there is a paradoxical decreased peripheral vascular resistance during the hyperdynamic “flow” phase. Accompanying reduced cardiac afterload is increased cardiac preload and thus increased cardiac output. There is abundant evidence that mediators of neural, humoral, and metabolic origins are involved in driving the decrease in vascular resistance after thermal injury. The significance of β 2 -adrenergic receptors in vasodilation has been demonstrated using knockout mice, thus pointing to the importance of epinephrine. The situation is complicated in the burn patient by the increase in nerve-stimulated release of norepinephrine, which can potentially mediate vasoconstriction. However, evidence exists that the local distribution of adrenergic receptors mediating either vasodilation or vasoconstriction will determine the effect of circulating epinephrine and nerve-stimulated norepinephrine release on peripheral vascular resistance. Blood flow regulation to the burned extremity remains intact: even in legs with 85% surface burned, increasing the surface temperature causes increases in blood flow comparable to unburned legs. In addition, increased tissue metabolism has been recognized to produce metabolites that mediate increased blood flow by reducing vascular resistance. With markedly increased metabolism in major burns, these metabolites, along with abnormally catecholamine signaling, nitric oxide, and atrial natriuretic peptide (ANP), may contribute to decreased vascular resistance.
When decreases in peripheral vascular resistance (especially with superimposed sepsis) compromise tissue perfusion via maldistribution, end-organ damage can result (e.g., the urinary granular casts of tubular necrosis). In this circumstance, pressor agents may be required to maintain adequate tissue perfusion despite adequate volume status. Epinephrine is the drug of choice, providing optimal vasoconstrictor and inotropic effects. In cases of resuscitated burn shock, the additional inotropic support of epinephrine is essential to maintain tissue perfusion without overly constricting the cutaneous vasculature needed to heal burn injuries. For example, dobutamine, a β-adrenergic inodilator, is an important inotrope in select burn patients, and the novel nonadrenergic inodilator levosimendan may find utility in treating cardiac failure in burn patients.
Conversely, supplemental norepinephrine is essentially never helpful, although it may improve hemodynamics especially in sepsis, during which burned patients live or die by the success or failure of their integumentary recovery. For burn patients, norepinephrine and stronger vasoconstrictors reliably lead to conversion of partial-thickness burns to full thickness, conversion of donor sites to new full-thickness wounds, and ischemic gangrene of at-risk/healing tissue. A vicious cycle of superinfection of these areas and progressive sepsis usually heralds a fatal outcome. We do not use norepinephrine drips in burned patients; they already have an endogenous excess.
Catecholamine resistance
Acidosis is the most common cause of catecholamine resistance. Macarthur et al. described inactivation of catecholamines by superoxide anions contributing to the observed hypotension of septic shock in rat models. They found treatment with superoxide dismutase not only abrogated endotoxin-induced hypotension in anesthetized rats but also elevated circulating levels of catecholamines. These findings suggest that sympathetic signaling, which counteracts hypotension during conditions of sepsis, may be blunted by inactivation of catecholamines by superoxides in the extracellular milieu. In a conscious rat model of sepsis, superoxide inhibition enhanced plasma levels of catecholamines, increased blood pressure, and improved survival. They also found that nitric oxide reduces the biologic activity of norepinephrine without altering nerve-stimulated release. Case et al. showed increased superoxide release for T cells in a norepinephrine-stimulated manner. These findings may provide insight into why critically ill patients lose responsiveness to pharmacologic norepinephrine administration and suffer refractory hypotension.
Catecholamines and hypermetabolism
Despite myriad factors reported to promote or inhibit the development of the postburn hypermetabolic state, investigators, led by Basil A. Pruitt, have demonstrated sympathetic catecholamines (norepinephrine more so than epinephrine) to be the effector limb of the transition to and maintenance of this hypermetabolic state. Herndon et al. clearly showed this using a 50% full-thickness scald burn rodent model, with groups pretreated with thyroidectomy, adrenalectomy (± dexamethasone replacement), and reserpine depletion of catecholamines. Adrenalectomy or reserpine blunted more than half of the hypermetabolic response. Wilmore et al. demonstrated catecholamines to be the mediator of the human hypermetabolic response to thermal injury. Several key findings were generated by that study: the β-adrenergic (but not α-adrenergic) blockade reduced metabolic rate, pulse, blood pressure, and free fatty acids. Additionally, the investigators documented the “nonliving” response to thermal injury: poikilothermia, discussed earlier. Their translational research found that when burned patients were placed in cooler environments (21°C), metabolic rates generally increased, with urinary catecholamine excretions increasing in parallel, excepting four nonsurvivors who showed less catecholamine elaboration, became hypothermic, and did not elevate their metabolic rates. The reason these patients failed to develop sufficient early hypermetabolic responses to permit survival remains only partially understood, but these data suggest an inability to mount a sufficiently powerful sympathetic response.
Burned patients consistently selected a higher room temperature (~30°C) and also had skin and core temperature increases of 1.7°C to 2°C above controls. Elevations in energy requirements could be partially modulated through adjustments in environmental temperature. Burn patients treated in warm environments of 32°C exhibited reduced metabolic rates compared with those treated at 25°C, although both groups remained hypermetabolic. After injury, and concurrent with an elevated hypothalamic temperature set point and cardiac index, qualitative and quantitative changes occur in the flow of biologic energy and mass (substrate) through the patient.
Experimental studies of Wolfe and Durkot suggest that the adrenergic drive after burn facilitates lipolysis, influencing fatty acid oxidation. The importance of adrenergic drive on lipid metabolism in burns was shown in human patients through the use of stable isotopic studies, as well as adrenergic antagonists. , , The profile of the plasma lipids is dramatically changed as well. These results indicate that not only is lipolysis after thermal injury mediated by β 2 -adrenergic receptors, but they also suggest increased intracellular and extracellular triglyceride–fatty acid cycling, with resultant heat production. Elijah et al. further elucidated the effects of peroxisome proliferator-activated receptor on lipolysis and hyperglycemia in the severely burned.
Wilmore developed experimental paradigms suggesting the role of catecholamines in mediating the hypermetabolic response to thermal injury. Findings included a positive correlation of increased plasma catecholamines and whole-body oxygen consumption after thermal injury, as well as demonstrating that adrenergic blockade lowers the burn-induced increase in metabolic rate and cardiac output to control levels in animal models. ,
Experimental findings in rats suggest that the adrenal medulla, although essential for high rates of heat production after thermal injury, is not the upstream driver of the hypermetabolic response. , Animals with hypothalamic lesions did not increase metabolism after thermal injury and were chronically hypothermic, not unlike experiments in which the adrenal medulla was removed before thermal injury. These results are consistent with clinical observations of burn patients in whom reductions in heat loss were achieved with occlusive dressings and for whom elevated environmental temperatures demonstrate partial reductions in metabolic rate and catecholamine secretion.
β-blockade
Building on findings that catecholamines drive postburn hypermetabolism, Herndon et al. , demonstrated that pediatric patients could be treated with the β-adrenergic blocker propranolol to successfully reduce metabolic rate without compromising cardiovascular function. In a more recent study by this group, β-adrenergic blockade in pediatric patients for 4 weeks during recovery from severe burns reduced the elevation in resting energy expenditure and reversed the reduction in net muscle–protein balance over 80%. Such treatment also prevented fatty liver and loss in fat-free whole-body mass (measured by dual-energy x-ray absorptiometry) and provided for a more efficacious recovery in these children. , Subsequent studies extended these findings to show prolonged improvement when dosing was continued for 1 year postburn. Recent animal studies have further established a cyclooxygenase-2 role in postburn hepatocellular proliferation and histologic remodeling in the liver. Downregulation of fructose-1,6-bisphosphatase-2 mRNA has been observed in muscle tissue after treatment with propranolol; this enzyme may play a role in gluconeogenesis, although the metabolic significance of this tissue-specific transcriptional alteration remains to be determined. Propranolol leaves α-adrenergic receptors unopposed, resulting in peripheral vasoconstriction and somewhat increasing vascular resistance. Reduced blood loss has been observed, with postoperative hematocrit 5% to 7% higher with propranolol. The exercise-induced enhancements in muscle mass, strength, and VO 2 peak were not impaired by propranolol; instead, aerobic response to exercise was improved in massively burned children. β-Blockade in nonburned septic patients has become an area of active research and, based on these findings in burned patients, demonstrates value for some patients, although the overall indications and patient selection have yet to be fully elucidated.
Sympathetic influences on immune function
New data have clarified the interconnections between the immune and sympathetic nervous systems and are well reviewed by Padro et al. Understanding these interactions may be important to comprehending the implications of our pharmacologic treatments with β-adrenergic antagonists and agonists on immune function.
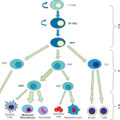
Immunohistochemical staining demonstrates substantial sympathetic innervation of all primary (thymus and bone marrow) and secondary (spleen and lymph nodes) lymphoid organs. Innervation has been shown to reach immune cell compartments of the spleen (the white pulp), periarterial lymphoid sheath, marginal zone, and marginal sinus areas, as well as the splenic capsule and trabeculae. Sympathetic nerve terminals have been described in direct apposition to T cells, interdigitating dendritic cells, and B cells.
Immune modulation by adrenergic signaling was recently reviewed by Sanders. Lymphocytes (including activated and resting B cells, naïve CD4 + T cells, T helper [T h 1] cell clones, and newly generated T H 1 cells) express β-adrenergic receptors, but they are not expressed in newly generated T H 2 cells. Furthermore, there is significant evidence that norepinephrine can modulate the function of CD4 + T cells, which in turn modulate antibody production of B cells. Sympathetic neurons suppress CD8 + T-cell receptor response and cytotoxic activity. In addition, norepinephrine can directly influence B-cell antibody production depending on the time of exposure after activation. The physiologic importance of these in vitro findings is supported by a series of in vivo experiments involving severe combined immunodeficient ( scid ) mice depleted of norepinephrine before reconstitution with antigen-specific T H 2 and B cells. These experiments demonstrate that norepinephrine is necessary to maintain a normal level of antibody production in vivo. Furthermore, other whole-animal experiments also involving scid mice provide evidence that the immune response itself stimulates the release of norepinephrine from adrenergic nerve terminals in bone marrow and the spleen, which in turn may influence antibody production by B cells in a more local manner. β-Blockade in 20 pediatric burn patients significantly reduced serum tumor necrosis factor-α (TNF-α) and interleukin-1β (IL-1β). The parasympathetic system further conditions the immunomodulatory role of the SNS. Recently it was shown that the vagal synapses trigger acetylcholine release from memory T cells, in turn reducing TNF-α through the α-7-nicotinic acetylcholine receptor. These findings suggest the potential of sympathetic/parasympathetic activation in mediating immune responses.
In animal models, blocking β-adrenergic receptors soon after injury partially restored the lipopolysaccharide (LPS)-stimulated TNF-α secretory potential of circulating monocytes lost during the course of burn injury and sepsis. Apart from adrenergic inhibition of LPS-stimulated TNF-α release in isolated macrophages, similar inhibition of LPS-stimulated TNF-α production has also been demonstrated in human mast cells, microglial cells, astrocytes, and cytotoxic T lymphocytes. In contrast with adrenergic stimulation of TNF-α release, experiments with isolated atria, , myenteric plexus, and brain tissue have proved that TNF-α can negatively affect the release of norepinephrine.
In a series of fascinating studies, Ma et al. recently demonstrated that a murine depression-like phenotype, induced by LPS injection, could be abrogated by splenic denervation before LPS administration. They showed splenic denervation prevented changes in hippocampal synapse protein expression and strikingly decreased the levels of proinflammatory cytokine IL-6. Splenic denervation did not affect levels of TNF-α. Also recently, a murine model of posttraumatic stress disorder (PTSD) termed “repeated social defeat stress” (RSDS) was shown to recapitulate the behavioral, autonomic, and inflammatory aspects of PTSD. Targeted splenic denervation did not alter antisocial or anxiety-like behaviors induced by RSDS; however, IL-2, IL-17a, and IL-22, T-lymphocyte specific cytokines, were significantly reduced. T lymphocyte T HHh H 17 polarization was also ameliorated. These and similar studies by Elkhatib et al. suggest important metabolically and immunologically important neurotransmission, likely both afferent and efferent, via splenic innervation. They allude to the tantalizing possibility of temporary interruption to aid burn/critical illness recovery and providing a deepening understanding of these intricate and interconnected regulatory mechanisms.
Although the precise mechanisms of the negative modulation of proinflammatory cytokines by catecholamines are poorly understood, it may be achieved through the ability of catecholamines to induce the antiinflammatory cytokine IL-10. Whole-animal studies involving assessment of circulating levels of IL-10, as well as studies of human whole blood and mononuclear cells stimulated with LPS in the presence of adrenergic agonists, , , support this premise. Immunomodulatory effects were further elucidated by Takenaka et al. demonstrating the effects on T-cell differentiation to CD4+ via a dendritic cell-mediated pathway. Additionally, experimental neurotrauma resulted in increased IL-10 consequent to endogenous adrenergic stimulation in the absence of LPS or other evidence of infectious challenge.
Sympathetic response to sepsis
Burn injury is commonly complicated by transient bacteremia, infection, and sepsis (see chapters on Infection [ Chapter 10 ] and Multisystem Organ Failure [ Chapter 24 ]). Infection causes a marked sympathetic response proportional to the degree of insult in which there are simultaneous and opposing forces of hyperinflammation versus immunosuppression. Sepsis is accompanied by an enormous catecholamine surge leading to changes in cardiovascular output, immunomodulatory effects, and catabolism. Propranolol has been shown to attenuate those changes. The use of an adrenergic blockade as an immunomodulator has found further utility in other traumatic injuries. Furthermore, animal models of septic peritonitis suggest that initial sympathetic activation, as measured by elevated levels of plasma norepinephrine and greater norepinephrine turnover, persists for many hours. ,
Collectively, these data clearly support a complex trophic interconnection between the SNS and immune system. Burn- and sepsis-induced sympathetic responses exert significant influence on bone marrow cellular events. Evidence for norepinephrine regulation of myelopoiesis in experimental thermal injury with sepsis is detailed in Chapter 18 on hematology.
Role of thyroid function
An early rat study showed that thyroidectomy did not alter the postburn increase in metabolism, although adrenalectomy or catecholamine depletion with reserpine did reduce postburn metabolic rates. Subsequent human studies demonstrated generally normal total triiodothyronine (T3) and thyroxine (T4), free T3 and T4, and thyroid-stimulating hormone levels in uncomplicated burn patients. However in those patients with infection or sepsis, decreased amounts of free T4 and T3 were observed. T3 replacement did not alter metabolic rate or mortality postburn but may have decreased circulating levels of norepinephrine and epinephrine. These and other studies suggest that the hypermetabolic response to burn is independent of thyroid hormones. More importantly, these data, in conjunction with more recent work by Senel et al., allude to a postburn shift in metabolic control away from thyroid signaling in favor of other mediators. Hypothalamic control is dramatically altered after burn injury and often psychological trauma alone. Raise-Abdullahi et al. have provided an updated summary of these biologic substrates and implications, although the masterful review by Wilmore, Long, Mason, and Pruitt remains as (if not more) relevant today as when it was written.
Sex steroids after burn trauma
Androgens
Release of C 19 steroids.
In the normal physiologic state, dehydroepiandrosterone sulfate (DHEAS), a weak androgen, is the major secretory product of the adrenal cortex. In burn patients, there is an increase in cortisol secretion and a distinct decrease in serum DHEAS levels owing to a reduction in synthesis. Testosterone and androstenedione levels decrease abruptly. In burn patients, subnormal testosterone levels persist for 3 to 18 months postburn, whereas cortisol levels normalize earlier. The decrease in testosterone secretion may be the direct effect of excessive cortisol levels on the testes. , Wilmore, Long, Mason, and Pruitt’s review, mentioned earlier, covers this coordinated hypothalamic response to injury.
Burned men exhibit hypogonadism and Leydig cell failure after thermal injury, resulting in depressed testosterone levels. Plymate et al. measured levels of sex hormones (e.g., sex hormone–binding globulin [SHBG] and luteinizing hormone [LH]) and thyroid hormones in the weeks after burn injury. They showed an increase in estradiol levels and a concomitant decrease in the secretion of bioactive LH after burn injury, suggesting an alteration in hypothalamic control of the gonadal axis leading to suppression of testosterone release. SHBG also exhibited significant changes, with an initial decrease and subsequent rise in concentration as compared with controls. This increase in SHBG results in a further suppression of testosterone by reducing the amounts of the unbound hormone. The levels of SHBG strongly correlated with levels of T3 and free T3 as well. This study helped elucidate the complex relationships of alterations in hypothalamic, thalamic, and gonadal regulation in the burned male. Taken together, these studies allude to a pervasive shift from normal hypothalamic function to a postinjury “mobilization” that remains but partly understood.
It appears that synthesis of C 19 steroids by the adrenals and testes is compromised as a result of enhanced production of C 21 steroids, such as cortisol. Aldosterone levels are also subnormal, despite elevated plasma renin activity. This suggests a shift in pregnenolone metabolism away from mineralocorticoid and adrenal androgen pathways toward the glucocorticoid pathway. DHEAS also has a profound influence on the immune response, and a role for DHEAS as a modulator of the immune response is now well established. Given that immunostimulatory properties of T h 1 cells are low during severe illness, DHEAS deficiency may be a contributing factor to the immune suppression in burn patients. In vitro treatment of human T cells with DHEAS increases IL-2 production (which is required for clonal expansion) and IL-2 mRNA synthesis. Interestingly, this effect was seen only in CD4 + CD8 − and not in CD4 − CD8 + cells. DHEAS-treated cells were also able to mediate a more potent cytotoxic effect than were untreated cells.
Under conditions of severe physical stress and chronic illness, dopamine levels have been shown to be elevated; , consequently, dopamine may also influence immune status and adrenal steroid secretion in burn patients. Exogenous dopamine is often used in the treatment of critically ill patients because of its vasopressor, renal vasodilator, and cardiac inotropic properties. Povoa et al. reviewed vasopressor use in septic shock and found a need for a multimodal selection of these agents. However, several other studies indicate that dopamine treatment may undermine an already depressed immune system. This effect appears to act via the suppression of prolactin release from the anterior pituitary. Dopamine suppresses serum prolactin and DHEAS levels but not cortisol levels. , In vitro, prolactin has a synergistic effect on ACTH-induced DHEAS secretion by human adrenal cells. Thus it is possible that the dopamine-induced suppression of prolactin is responsible for lowering DHEAS levels and hence suppression of the T-cell proliferative response. The in vitro proliferative response of T cells from patients on dopamine therapy is diminished, and cells treated with DHEAS mediate a more potent T-cell cytotoxic effect.
Extensive studies and clinical experiences were undertaken over the past decade with androgen supplementation using oxandrolone. Reeves and Finnerty et al., detailed the 5-year outcomes of long-term oxandrolone treatments after a 24-month administration in severely burned children. They found significantly increased bone mineral content, greater height velocity, reduced cardiac work, and augmented muscle strength. This is described in greater detail in the chapter on hypermetabolism ( Chapter 23 ). Overall, there is a hypoandrogeneric state postburn, and supplementation with the anabolic steroid oxandrolone is effective at both ameliorating hypermetabolism and shifting the patient toward anabolism.
Estrogens
The impact of xenoestrogens on mortality in burned patients has been investigated. Found in insecticides used from the 1950s to the 1970s, xenoestrogens are compounds that can act as estradiol receptor agonists or antagonists and that are stored in fat. During the hypermetabolic state after thermal injury, the xenoestrogens are released along with mobilized lipids from these fat stores. In older burn patients who were more likely to have higher concentrations of these compounds in their bodies, it was discovered that nonsurvivors had significantly increased levels of two xenoestrogens, heptachlor epoxide and oxychlordane. It was suggested that these compounds may induce the inactivation of estradiol, progesterone, testosterone, and glucocorticoids via the induction of steroid hydroxylases, as well as antagonizing estradiol receptors, which may result in decreased inflammation and cytokine release.
Adrenal cortical steroids after burn trauma
Adrenocortical response is critical to coordinating the systemic response to thermal injury. The glucocorticoid surge after burn injury has long been measured by both serum and urinary excretion markers. Regulation of glucocorticoid secretion is complex, with multiple determinants of the adrenal cortex secretion of cortisol, including pituitary ACTH, but also afferent neural control and hyperthermia, which blunts the adrenal response to ACTH. Furthermore, the usual circadian rhythm of cortisol secretion is dampened after burn injury. In 1982, Vaughan et al. showed elevated circulating and urinary cortisol, with a weak correlation to the level of ACTH. Stronger correlations were noted between cortisol and total body surface area (TBSA) burned, metabolic rate, and average body temperature. These observations in burned patients indicate that adrenal hypersecretion of cortisol is in response to temperature, circulating mediators of hypermetabolism, direct adrenal innervation, and a decrease in adrenal cortex responsiveness to ACTH. As a result, the authors concluded that cortisol may play a secondary role in permitting and promoting the changes seen in postinjury hypermetabolism. On this basis, they attributed postinjury metabolic and thermal changes primarily to sympathetic tone and circulating catecholamines (norepinephrine and epinephrine).
Danner and colleagues carefully mapped the HPA axis response to a massive septic insult in their lethal canine pneumonia model as they attempted to define the “critical illness-related corticosteroid insufficiency.” They found a massive surge in total, bound, and free serum cortisol and in ACTH. Additionally, they determined that ACTH failed to promote a further increase in cortisol and that dexamethasone did not suppress cortisol, possibly because the adrenals were already maximally stimulated. Significantly in sepsis-surviving animals, the HPA axis recovered to normal levels, whereas ACTH and dexamethasone responsiveness recovered by 10 hours compared with nonsurvivors. In contrast, the mineralocorticoid response with hyperaldosteronism remained past 72 hours and did not regain dexamethasone suppression. Thus mineralocorticoids are ACTH independent in the setting of sepsis. These data support the adrenal exhaustion hypothesis.
In a postmortem study of adrenal glands of ICU patients, it was found that the adrenocortical structure was disrupted after critical illness. These patients tended to have adrenal glands that weighed less than controls, with significantly less protein content and greater fluid content. There was also considerable downregulation of ACTH-regulated genes.
Elevated plasma-cortisol levels have been shown during critical illness, especially during an episode of systemic inflammatory response syndrome (SIRS). However, cortisol production during the day in patients with SIRS, although elevated, is less than doubled. ACTH is suppressed in these patients, implying a non–ACTH-driven response. It has been demonstrated that during critical illness clearance of plasma cortisol is significantly reduced, playing a significant role in the hypercortisolism of the critically ill stress response. Other investigators determined in the setting of septic shock that only serial hormonal measurements and provocative testing were useful for HPA axis function assessment. They further identified high aldosterone levels in a population with poor outcomes from sepsis.
Norbury et al. followed urinary cortisol levels in 212 severely burned children, finding three- to fivefold increases in cortisol excretion up to 100 days postburn. Urinary norepinephrine levels were significantly increased up to 20 days, as shown in Fig. 19.1 . Hypercortisolemia has been suggested as a driver of whole-body catabolism after severe burn. To test this hypothesis, Jeschke et al. blocked cortisol production with ketoconazole in 55 severely burned children. They found normalization of the eightfold elevation in urine cortisol in the treatment group. Counterintuitively, no change was seen in inflammatory response, acute-phase proteins, body composition, muscle protein breakdown or synthesis, or organ function. Their data suggest that postburn hypercortisolemia does not play a central role in the catabolic response.
Urinary cortisol and catecholamine excretion after burn injury in children.
(From Norbury WB, Herndon DN, Branski LK, Chinkes DL, Jeschke MG. Urinary cortisol and catecholamine excretion after burn injury in children. J Clin Endocrinol Metab . 2008;93(4):1270-1275.)
Jeschke and Herndon characterized the long-term inflammatory and acute-phase responses in 977 pediatric burn patients with greater than 30% TBSA with 24-hour urinary excretion. They found significant elevations of cortisol, catecholamines, cytokines, and acute-phase proteins for up to 3 years, as seen in Fig. 19.2 . They also observed insulin resistance, increased fracture risk, hepatomegaly, increased cardiac output and cardiac dysfunction, and impaired strength over the same period. ,
Long-term persistence of the pathophysiologic response to severe burn injury.
(From Jeschke MG, Gauglitz GG, Kulp GA, et al. Long-term persistence of the pathophysiologic response to severe burn injury. PLoS One. 2011;6(7):e21245.)
Free versus total cortisol
Glucocorticoids circulate in the body bound to cortisol-binding globulin (CBG), such as transcortin, as an inactive complex. Only 1% to 10% of total plasma cortisol circulates unbound and is responsible for the biologic activity of glucocorticoids. Free plasma cortisol is a surrogate for the difficult-to-measure tissue cortisol. , Burn injury shifts the equilibrium between unbound and total cortisol toward an elevation in the unbound fraction. Serum CBG and CBG-binding capacity are low in burn injury, severe infection, and septic shock. In burn patients, CBG levels have been shown to decrease markedly, with the lowest values occurring 48 hours after injury. Even a minor burn, such as 3% TBSA, results in a reduction of serum CBG levels by 30%, which return to normal levels 1 to 2 weeks later. The net effect of the decrease in CBG levels after thermal injury may not only result in increased levels of free cortisol but also in the amount of excreted cortisol, which is reflected in high urinary corticosteroid levels. The urinary cortisol concentration was observed to increase progressively with burn size, with the highest levels in the 60% to 99% TBSA burn groups. Additional explanations for increased levels of corticosteroids in burn patients may be due to the direct inhibitory effect of corticosteroids on the biosynthesis of CBG. Furthermore, IL-6 elevation associated with massive burns has also been implicated in reducing CBG synthesis.
Evidence exists suggesting that cortisol elevation with corresponding decreased ACTH may be driven by endothelin or atrial natriuretic peptide/hormone (ANP/H). Vermes et al. demonstrated significant elevation in both plasma endothelin and ANP levels for 8 days after hospitalization in severely ill patients with sepsis or trauma. Fittingly, endothelin has been shown to be a modulator of the sympathetic response. In addition, infusion of ANP in humans has been demonstrated to block CRH-stimulated secretion of ACTH and cortisol, whereas endothelin-1 and endothelin-3 enhance secretion of steroid hormones from the adrenal cortex. However, endothelin-3 has been reported to elevate ACTH and corticosterone levels in rats, whereas endothelin-1 results in elevated ACTH in humans. Based on this, Vermes et al. suggest that endothelin may be responsible for stimulating steroid secretion, whereas ANP’s action on the HPA axis may suppress ACTH secretion, thereby explaining the paradoxical increase in cortisol with concomitant low ACTH levels in severely stressed patients.
By precisely measuring cortisol, Cohen et al. found no significant correlation between total plasma, free plasma, and tissue microdialysis cortisol levels. Tissue microdialysis cortisol levels were significantly increased in burned patients compared with healthy controls. Furthermore, via subcutaneous microdialysis of cortisol levels in burned and nonburned tissue of severely burned patients, they discerned no significant difference in local cortisol concentrations. This indicates that local microenvironmental changes in burned tissue, such as more cortisol cleaved from CBG by the neutrophil elastase, failed to significantly affect local cortisol levels. They concluded that free cortisol demonstrated a better correlation with TBSA than total cortisol. Given the sensitivity of cortisol to pain and stress, as well as diurnal variations, Brown et al. advocate the use of salivary α-amylase as a surrogate in the setting of outpatient investigations.
Substrate cycling
Influence on metabolic pathways
Elevated energy expenditure and hyperglycemia are hallmarks of thermal injury. The heavy demand for energy stems from the increase in essential functions, such as the synthesis of proteins required for wound healing, the synthesis of acute-phase proteins, and inflammatory mediators. The increase in substrate cycling is partly responsible for the elevation in resting energy expenditure in burn patients. This occurs when enzymes catalyzing opposing reactions of the same pathway are simultaneously active. For example, in the conversion of glucose to glucose-6-phosphate and back to glucose, the demand for energy increases to resynthesize adenosine triphosphate (ATP) used in this and similar reactions. In burn patients, the rate of glucose production and glycolysis, as well as of lipolysis and reesterification of triglycerides, is elevated. This cycling of substrates generates heat through the hydrolysis of high-energy phosphate bonds in ATP, thereby contributing to thermogenesis, as well as increased energy requirements in burn patients. Muscle mitochondrial decoupling and fat browning adaptions additionally occur and further increase thermogenic capacity independent of oxidative phosphorlyation.
Hormonal determinants of glucose utilization
In 1986, glucose and alanine fluxes were studied in adult burn patients with stable isotope tracer infusions, somatostatin infusion (suppressing insulin and glucagon), and insulin + glucose replacement (isolated glucagon suppression). Insulin and glucagon levels were both significantly elevated above those in unburned individuals. Somatostatin infusion reduced both insulin and glucagon levels and induced a stable decrease in glucose production at 30 minutes with a progressive decrease in glucose uptake over the course of 30 to 180 minutes. When glucagon was selectively reduced via the reinfusion of insulin to restore basal levels in conjunction with glucose infusions to maintain euglycemia, glucose production was suppressed significantly below levels when somatostatin was infused alone, and glucose clearance was restored to preinfusion levels. This study provided evidence for glucagon control of hepatic glucose production (HGP) in the postburn state, with basal levels of insulin further suppressing HGP while exerting greater influence to increase (peripheral) glucose uptake. Glucagon reduction (via somatostatin + insulin infusion) did not alter the alanine clearance or flux rates; however, suppression of insulin and glucagon (from somatostatin infusion alone) increased the alanine flux rate, consistent with increased peripheral protein catabolism when the insulin signal is diminished. The authors noted prior observations indicating tachyphylaxis in the hepatic gluconeogenic response to glucagon. However, in the setting of hypercortisolemia (observed in these patients), prolonged HGP in response to glucagon signaling is observed.
A study of unburned adults differentiated the response to endogenous insulin infusions from the response to a proximate glucose infusion using somatostatin suppression of endogenous insulin and glucagon + insulin replacement to basal levels during the glucose infusion. This study established that glucose infusion (1 and 4 mg/kg per minute), independent of endogenous insulin effect, suppresses endogenous glucose production, stimulates alanine production, and suppresses urea production. A further analysis of data collected as part of Pruitt’s T3 replacement trial described earlier showed that the metabolic rate increased proportionally with and was independently predicted by plasma glucagon.
In the setting of an adequate, constant nitrogen intake, increasing carbohydrate feeding spared protein catabolism and mitigated negative nitrogen balance, whereas intravenous fat emulsion did not affect nitrogen balance independently. , These studies indicated the primary determinants for nitrogen excretion were carbohydrate intake and metabolic rate. Nitrogen excretion was minimized when the carbohydrate intake approximated the metabolic rate. Insulin was additively anabolic to carbohydrate intake in further decreasing nitrogen excretion when patients were provided constant and sufficient protein intake.
Glucocorticoids after burn injury
In burn patients likely to recover, plasma glucocorticoid levels are moderately elevated or in the upper-normal range, can persist beyond a month, , and return to normal as healing progresses. In contrast, patients with severe thermal injury (90% TBSA) have markedly lower levels of glucocorticoids.
Glucocorticoids and carbohydrate metabolism
Glucocorticoids contribute to hyperglycemia by enhancing endogenous production of glucose in the liver. , , , After burn, elevated glucose levels are sustained through gluconeogenesis and impaired glucose utilization. The increased plasma lactate produced by peripheral tissues after burn, as documented by Wolfe et al., is an essential substrate for gluconeogenesis by the liver. Burn injury causes intrinsic alterations in the liver, which increase the conversion of pyruvate to oxaloacetate at the expense of nontricarboxylic acid cycle sources. Efficient mobilization of glucose from glycogen and skeletal muscle amino acids for gluconeogenesis requires glucagon secretion, , which is stimulated by glucocorticoids. , , Glucocorticoids also sustain the action of glucagon and prevent the usual development of tachyphylaxis from high levels of glucagon. In addition to gluconeogenesis, impaired glucose utilization and insulin resistance can also play a role in sustaining high circulating levels of glucose in burn patients.
Glucocorticoids and protein metabolism
Protein catabolism is a part of burn hypermetabolism, resulting in negative nitrogen balance. Cuthbertson’s landmark studies were the first to suggest the important concept that nitrogen loss is a whole-body rather than a local burn wound response. The increase in proteolysis seen in burn injury is at least partly mediated by glucocorticoids. In humans and in animal models, administration of glucocorticoids enhances muscle proteolysis. Burn injury–induced muscle proteolysis can be inhibited by a glucocorticoid receptor antagonist. Amino acids mobilized from peripheral tissues are transported to the liver where, unlike in other tissues, cortisol stimulates protein synthesis. The increased hepatic protein synthesis in response to cortisol can drive the new synthesis of gluconeogenic enzymes and acute-phase proteins in response to burn injury.
The complete details of the mechanisms involved in burn-mediated alterations in protein metabolism are unknown. However, some information can be gleaned from studies on other states of excessive catabolism. In conditions such as metabolic acidosis, adrenalectomy halts muscle proteolysis and does not increase expression of components of the ubiquitin–proteasome pathway. , These effects can be reversed by dexamethasone administration. Further support for this premise is provided by in vitro studies, which show that dexamethasone-induced increases in proteolytic degradation in myocytes can be abolished by the glucocorticoid inhibitor RU486. Ding and coworkers suggest that partial inhibition of the ubiquitin–proteasome pathway may be beneficial in enhanced catabolic states. Taken together, these data suggest that interaction of glucocorticoids and the ATP-requiring ubiquitin–proteosome system may play an important role in burn-induced proteolysis. ,
Another aspect of protein catabolism after burn is the generation of gluconeogenic amino acids. Plasma levels of alanine are increased after burn. Nitrogen produced as a result of transaminating alanine to the gluconeogenic intermediate, pyruvate, is subsequently converted into glutamine and then to urea for excretion by the liver. In muscle tissue, alanine aminotransferase (ALT/SGPT) transfers an amino group from glutamine to pyruvate, forming alanine and α-ketoglutarate. Alanine is then dumped into the bloodstream, taken to the liver, and returns to the muscle as glucose (the glucose–alanine cycle). This is one reason why plasma alanine increases after burn. By contrast, in the liver, glutamine enters the mitochondria, and eventually nitrogen is processed via the urea cycle. Glutamine is one of the major participants in the translocation of amino acids from peripheral tissues to the liver for nitrogen excretion. Expression of glutamine synthase is increased to compensate for glutamine depletion in peripheral tissues. After burn injury, glutamine synthase mRNA is increased first in the lung and later in muscle. Adrenalectomy partially reduces burn-induced glutamine synthase mRNA in a tissue-specific manner, with no such effect in the kidney or liver. There is evidence suggesting that glucocorticoids may augment glutamine synthesis in lung and muscle tissues. Mobilization of protein from peripheral tissues is also indicated by the increase in phenylalanine in the blood of burn patients. Phenylalanine is the only amino acid not degraded by peripheral tissue; hence it accumulates in the circulation when uptake by the liver is compromised.
The hypermetabolic and catabolic states seen in thermal injury remain long after the burn wound completely heals , , : reduction in protein catabolism and enhancement of lean body mass have been observed to occur at 9 to 12 months after the initial injury. Therefore the postburn treatment of growth deficiency must be prolonged beyond wound healing. ,
Many treatment algorithms to modulate this growth retardation and hypermetabolism have been examined and subsequently reviewed by Diaz. Indirect effects of glucocorticoids on glucose levels in burn include modulation of insulin-like growth factor-1 (IGF-1), an important mediator of growth hormone (GH) action. , Marked depression of all components of the IGF-1 complex is seen after burn. Elevated glucocorticoid levels in burn patients may contribute to the suppression of the acid labile subunit (ALS) of the IGF-1 complex. Treatment of rats with dexamethasone results in low levels of serum ALS, as well as liver ALS mRNA. ,
In addition to amino acids released from peripheral tissue, free fatty acids are released from adipose tissue by cortisol. In burned children and adults, increased lipolysis is reflected in the elevated plasma levels of palmitic and oleic acids. , , Collectively, these effects lead to hepatomegaly and a cushingoid phenotype. Essential fatty acid deficiency can also be observed after burn injury; this usually responds to appropriate replacement.
Glucocorticoids on bone metabolism
Aside from combating the increased demand for energy, glucocorticoids also affect bone development. Abnormal bone metabolism in burn injury has been demonstrated in animals and humans. , In children, the reduction in bone mineral density persists for at least 5 years after severe burn injury (>40% TBSA) and results in permanent retardation of linear growth. , The reasons for loss of bone mineral density include increased production of endogenous glucocorticoids, the inflammatory response, immobilization, aluminum loading, and production of cytokines (e.g., IL-1 and IL-6) that facilitate bone resorption. In an animal study, Hoscheit et al. found increased markers of bone resorption, particularly RANKL, in the first 2 weeks after burn, suggesting that the decreased bone mass after burn injury results from increased resorption and decreased bone formation.
Glucocorticoids have potent effects on bone formation and resorption, resulting in loss of bone mass. Weinstein and coworkers investigated the long-term (equivalent to 3–4 human years) effects of glucocorticoids on bone metabolism in an animal model and reported a reduction in osteoclastogenesis and osteoblastogenesis leading to reduced bone turnover and reduced bone formation, respectively. Enhanced osteoclast and osteoblast apoptosis was observed in mice subjected to long-term glucocorticoid administration, as well as in patients with glucocorticoid-induced osteoporosis. In addition, glucocorticoids directly downregulate expression of type I collagen and upregulate expression of collagenase-3 in chondrocytes. On the other hand, IGF-1 enhances expression of type I collagen and suppresses the expression of collagenase-3. Thus the massive increase in glucocorticoids and the corresponding decrease in IGF-1 in burn injury have the ability to profoundly alter bone and cartilage formation.
The mechanisms by which glucocorticoids mediate bone resorption are unclear. Glucocorticoids may mediate bone resorption by their dual capacity to initially inhibit osteoclast synthesis and later stimulate osteoclast synthesis, coupled with an increase in bone resorption. Another mechanism by which cortisol may influence bone resorption is by suppression of IGF-1 or GH-induced chondrocyte proliferation. The antiproliferative effect of glucocorticoids may be mediated through downregulation of the GH receptor and binding affinity, as well as suppression of the local production of IGF-1 by these cells.
Supplementation with exogenous recombinant human GH was studied by Herndon et al. , , and was found to have a profound anabolic effect on the muscle and skin. Breederveld et al. reviewed trials of GH in burn patients, noting more rapid healing of burn wounds and donor sites, as well as reduction of hospital stay without increasing mortality or scarring. IGF-I supplementation was also examined and had an even greater anabolic effect but with less resultant hypoglycemia or hyperglycemia. However Takala et al. ascertained increased morbidity and mortality in trauma patients, and the use and further study of these hormones has since been restricted. In a subsequent study, Herndon and Voigt employed a combination treatment of oxandrolone and propranolol that significantly ameliorated growth arrest in pediatric burn patients without the risks associated with IGF-1 treatment. Rojas et al. reviewed the current pharmacotherapy for hypermetabolism in burn patients and covered these issues in detail.
Glucocorticoids on immune suppression
Severely burned patients are susceptible to opportunistic infections, and sepsis is a major cause of death associated with burns. Burn injury leaves the patient vulnerable to opportunistic infections via skin, GI, respiratory, and urinary tracts. The glucocorticoid response to thermal injury appears to play an important role in immune dysfunction, with impairment of both specific and nonspecific defenses. Corticosteroids reduce lymphocyte, eosinophil, and basophil numbers; alter lymphocyte subpopulations; depress immunoglobulin production by B cells; and suppress neutrophil and monocyte/macrophage activity.
Acute thymic involution , and a reduction of the total T cell population occur soon after burn injury. , During initial thymic involution in an animal model, there is marked depression of CD4 + /CD8 + lymphocytes. Thymic involution is a common response to various types of stress and trauma. In humans, the depression of T lymphocytes is reflected by the reduction of both CD4 + and CD8 + cell numbers. In an animal model, CD4 + CD8 − cells are reported to be more sensitive to the effects of thermal injury than are CD4 − CD8 + cells. Unsurprisingly, CD4 + CD8 − cell numbers remain suppressed during the initial 2-week period after burn injury.
Thymic changes after exogenous administration of glucocorticoids are similar to those seen in burn, , in that both noninjury exogenous hypercortisolism states and burn injury are associated with decreased CD4 + CD8 + and increased CD4 + CD8 − thymocytes. The reduction in CD4 + CD8 + cell numbers during the first 24 hours after burn is due to glucocorticoid-mediated apoptosis because burn-induced thymocyte apoptosis is suppressed by adrenalectomy or the administration of a glucocorticoid antagonist. Other factors contributing to lymphocyte dysfunction and immunosuppression resulting from elevated corticosteroid levels may include direct inhibition of T cell proliferation, IL-2 production, , apoptosis, and altered lymphocyte membrane fluidity.
Apart from these effects on lymphocytes, glucocorticoids also enhance susceptibility to infections by modifying monocyte and neutrophil function. Movement of circulating inflammatory cells to the site of infection is suppressed by the ability of glucocorticoids to reduce the cellular response to chemotactic stimuli, , , diminish neutrophil adherence, and induce a shift from marginal to circulating cells. Glucocorticoids also suppress the bactericidal activity of monocytes and neutrophils, perhaps through impairment of lysosomal function.
Although severe burns are associated with alterations in B-cell production and function, there is considerable inconsistency in the literature. For example, in rats subjected to 30% burn injury, splenic lymphocytes respond poorly to LPS, and immunoglobulin synthesis is reduced in comparison to control animals. Others have found an increase in circulating B cells early after burn injury. Administration of methylprednisolone to normal volunteers for 2 to 4 weeks also reduces serum immunoglobulin levels.
This review provides a glimpse of how the catecholamine and hormonal responses to thermal injury support compensatory cardiovascular, metabolic, and immunologic changes. Although adrenergic mechanisms are important for their ability to influence intracellular signaling pathways, their roles as modulators of gene expression are still being explored and refined. Whereas alteration of gene expressions by glucocorticoids is well described, less is known about the interplay of glucocorticoids with the complex postinjury signaling milieu seen with severe thermal injury or other forms of trauma.
Further reading
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree