Summary
Facial anatomy is highly complex and intricate. A strong knowledge of facial anatomy is the foundation for performing facial plastic surgery. This in-depth knowledge and understanding of facial anatomy is necessary to safely perform facial plastic and reconstructive surgery. Therefore, this chapter thoroughly reviews facial anatomy.
3 Anatomy
3.1 Introduction
As facial plastic and reconstructive surgeons, our goal is to provide the highest level of care and safety to our patients. An in-depth knowledge and understanding of facial anatomy is necessary to avoid complications when performing facial plastic surgery procedures. The objective of this chapter is to examine the face by region and discuss the anatomy relevant for safely performing facial plastic surgery procedures.
3.2 Skin Anatomy
3.2.1 Epidermis
Layers
The epidermis is divided into five layers. From superficial to deep, the outermost layer is the stratum corneum which represents the terminal differentiation of keratinocytes into anucleate, flattened keratinocytes. 1 The stratum lucida is an eosinophilic acellular layer beneath the stratum corneum in acral skin (palms and soles). 1 The stratum granulosum contains deeply basophilic keratohyalin granules important for the cornification of the stratum corneum. 1 The stratum spinosum layer contains polygonal cells with abundant eosinophilic cytoplasm named for small, spiny intercellular desmosomal attachments seen under light microscopy. 1 The deepest layer is the stratum basale. This is a single mitotically active layer of cuboidal to columnar-shaped basophilic keratinocytes that attach to the basement membrane by hemidesmosomes and give rise to the more superficial epidermal layers. 1
Composition
The epidermis contains keratinocytes, melanocytes, Langerhans cells, and Merkel cells. 1 Keratinocytes make up 80% of the epidermal cells and originate in the basal layer. 1 Melanocytes are neural crest derived, pigment-producing, dendritic cells found in the basal layer. 1 They produce melanin to protect the mitotically active basal keratinocytes from UV radiation. 1 Langerhans cells are bone marrow–derived antigen-processing and antigen-presenting cells found mainly in the stratum spinosum layer. 1 , 2 These cells are characterized by intracytoplasmic tennis racket–shaped structures called Birbeck granules. 1 Merkel cells are mechanoreceptors of neural crest origin involved with touch sensation. 1 , 2 They are found in the basal layer of palms, soles, oral and genital mucosa, nailbeds, and the follicular infundibulum. 1
3.2.2 Dermis
Layers
The dermis is composed of two layers: the papillary dermis (superficial) and the reticular dermis (deep). The papillary dermis is thinner than the reticular dermis. The dermis is organized into upward projecting papilla that intercalate with the downward projecting rete ridges of the epidermis. 1
Composition
Collagen is the primary structural component of the dermis. 1 Collagen is synthesized by dermal fibroblasts and provides tensile strength and elasticity. 1 The majority of dermal collagen is type I (80–90%). 1 Dermal elastic tissue is composed of multiple substances including elastin protein, microfibrillar matrix with fibrillin, and a glycoprotein. 2 Ground substance of the dermis includes proteoglycans, glycosaminoglycans, and filamentous glycoproteins. 1 The cellular components of the dermis include fibroblasts, phagocytic cells (monocytes, macrophages, and dendrocytes), and mast cells. 2
Vasculature
The skin has two vascular plexuses connected by communicating vessels. The superficial vascular plexus is in the superficial reticular dermis and receives its vascular supply from the deep vascular plexus. 2 It gives rise to the capillary loop system in the papillary dermis. 2 It abuts the epidermis and provides nutrients by diffusion. 2 The deep vascular plexus is at the junction of the dermis and subcutaneous fat and receives its vascular supply from the musculocutaneous arteries perforating from the subcutaneous fat. 2 Arterioles from the deep vascular plexus supply the epidermal appendages and the superficial vascular plexus. 2
3.3 Forehead Anatomy
3.3.1 Central Forehead and Glabella
Topography
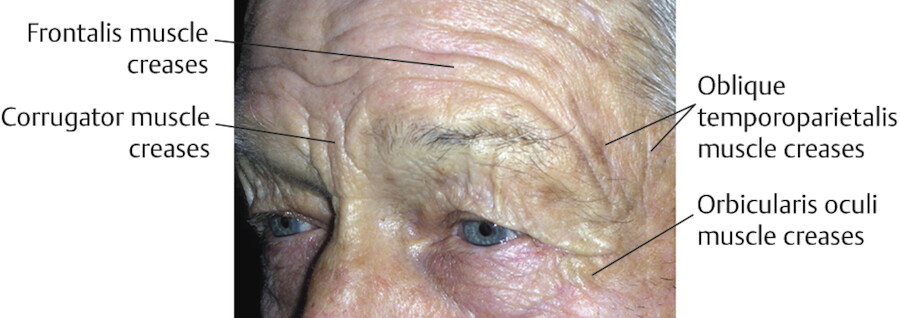
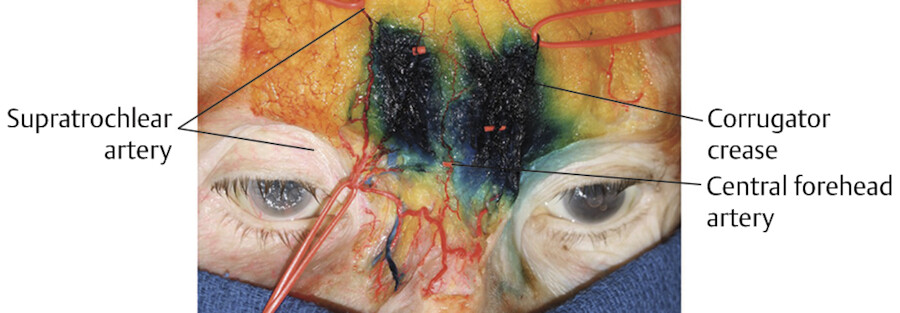
Presenting as early as the 20s, the central forehead can develop dynamic horizontal lines due to underlying frontalis muscle contraction and creasing of the forehead skin (Fig. 3.1). Likewise, the glabella develops vertical lines (corrugator creases) related to repeated creasing of the skin from underlying corrugator contraction (Fig. 3.2) and horizontal lines from underlying procerus contraction. The corrugator crease is a landmark for the vertical course of the supratrochlear artery, which supplies the soft tissue of the central forehead (Fig. 3.3).
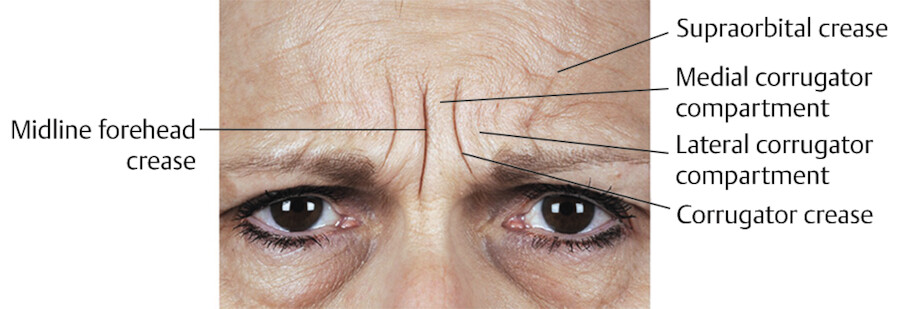
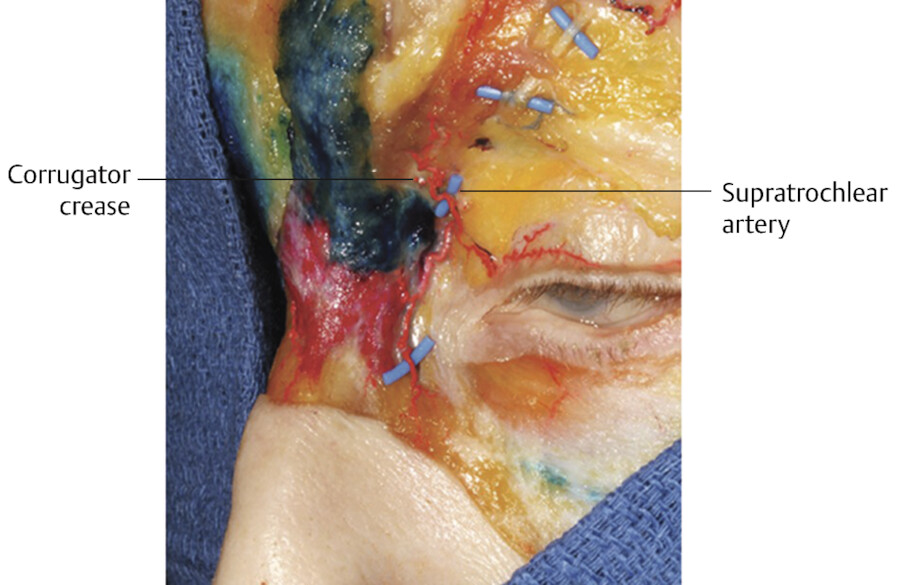
Soft Tissue
The scalp is composed of five soft tissue layers: skin, subcutaneous tissue, galea, loose areolar tissue, and periosteum. 3 The skin of the forehead is the thickest of the face. The galea aponeurotica of the scalp divides into a superficial and deep layer to envelope the frontalis muscle. 3 , 4 The deep layer of the galea attaches to the supraorbital margin. 5 Between the deep galea plane and periosteum is a plane of loose areolar tissue. 4 The periosteum and galea fuse approximately 1 cm above the supraorbital rim. 3
Muscles
Frontalis
The frontalis muscle is the primary brow elevator with a central attenuation. 4 The frontalis originates from the galea aponeurotica of the scalp, penetrates through the overlapping orbicularis muscle, and inserts into the subcutaneous tissue deep to the eyebrows. 6 Medially, it becomes confluent with the vertical procerus muscle. 3 The lateral frontalis margin stops or markedly attenuates over the temporal line. The frontalis muscle is firmly fixed to the overlying dermis by transverse-oriented fibrous septae. 6 These are thought to play a role in the transverse forehead furrows that occur across the forehead. 6
Corrugator Supercilii
In the medial canthal area, the bulky corrugator supercilii is located deep to the frontalis. 7 It originates from the nasal process of the frontal bone and extends obliquely over the supraorbital rim where it interdigitates with fibers from the frontalis and orbicularis muscle and inserts into the dermis of the forehead skin behind and just superior to the middle one-third of the eyebrow. 4 Medially the corrugator is congruent with the procerus. 7 Its action is to pull the eyebrow in an inferomedial direction.
In cadaver dissections by Pessa, the corrugator muscle was identified with two muscular bellies, a transverse and an oblique (Fig. 3.4). 8 The thickest portion of the muscle is at the medial canthus. Substantial bulk was still present at the midpupillary line, but no distinct corrugator fibers were detectable at the lateral canthus. 7
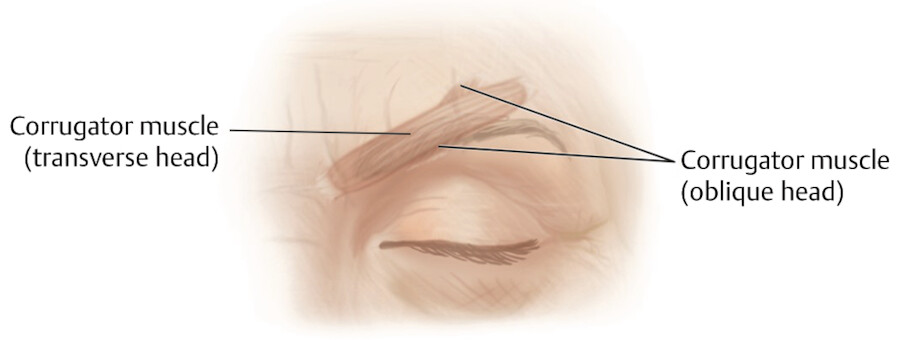
Depressor Supercilii
The small, vertically oriented depressor supercilii muscle originates on the medial orbital rim, near the lacrimal sac, and inserts on the medial aspect of the bony orbit, inferior to the corrugators (Fig. 3.5). It acts as an accessory depressor of the medial eyebrow. 6 Of note, not all reports have identified this muscle.
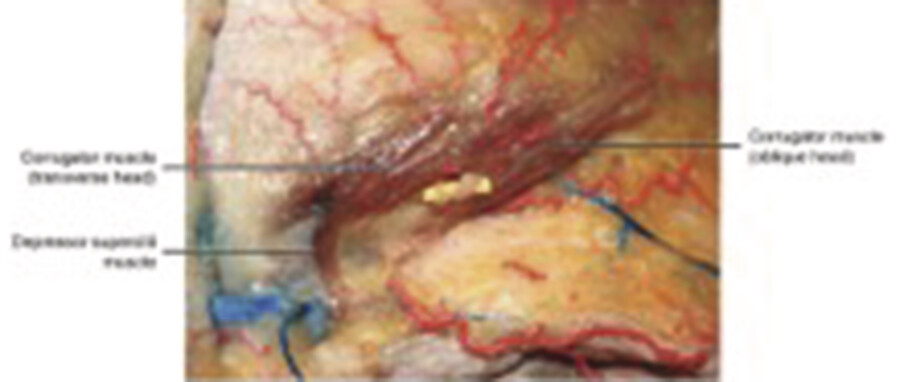
Procerus
The procerus is a small, thin pyramidal muscle arising from the fascia of the inferior portion of the nasal bone and the upper lateral nasal cartilage. 6 It inserts into the glabellar skin, between the paired bellies of the frontalis. 6 The procerus draws the medial angle of the eyebrow downward. The procerus is inferior to the corrugator supercilii. 6
Innervation
The ophthalmic division of the trigeminal nerve (V1) gives off the supratrochlear and supraorbital branches and provides sensation to the forehead and scalp. The supraorbital nerve supplies sensation to the upper eyelid and forehead skin except for a midline vertical strip which is supplied by the supratrochlear nerve. The supraorbital nerve has two divisions: (1) a superficial (medial) division that passes within and over the frontalis, providing sensory supply to the forehead skin and the anterior margin of the hair baring scalp and (2) a deep (lateral) division that runs between 0.5 cm and 1.5 cm medial to the superior temporal line between the galea aponeurotica and the periosteum as a sensory nerve to the frontoparietal scalp. 3 , 9 The supraorbital nerve leaves the orbit via a notch in the supraorbital rim in approximately two-thirds of patients and through a foramen in one-third of patients (Fig. 3.6). 3 The supratrochlear nerve exits the orbit by passing through the corrugator supercilii muscle. 3
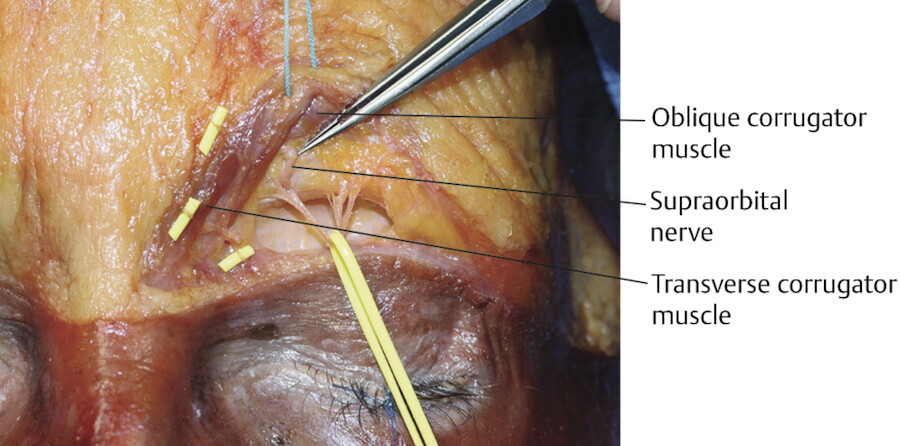
Vasculature
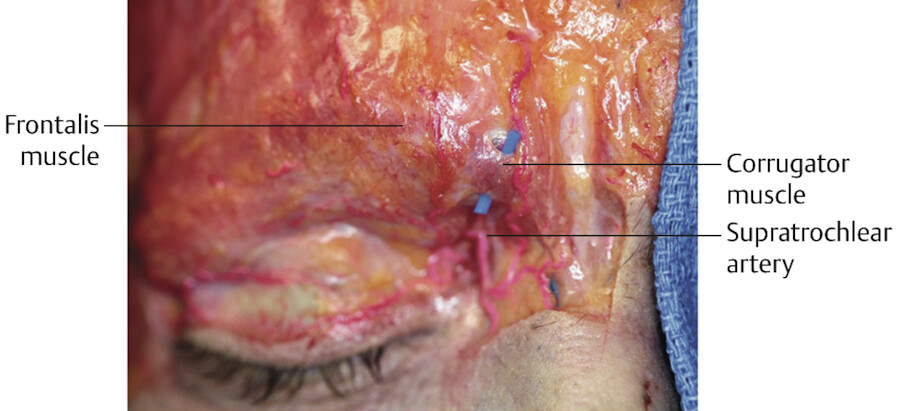
The internal carotid artery gives off the ophthalmic artery which gives off the supraorbital and supratrochlear arteries. The supraorbital and supratrochlear arteries, which travel with similarly named sensory nerves in a neurovascular bundle, are found deep to the corrugator muscle and frontalis muscle, until approximately 1 cm above the supraorbital rim where they pierce the frontalis to emerge superficially in the subcutaneous plane and supply the skin of the central forehead (Fig. 3.7). 8 The central forehead artery is superficial in the glabella area and is likely responsible for vascular complications from superficial filler in the glabella (Fig. 3.8). 8
3.3.2 Temporal Fossa
Soft Tissue
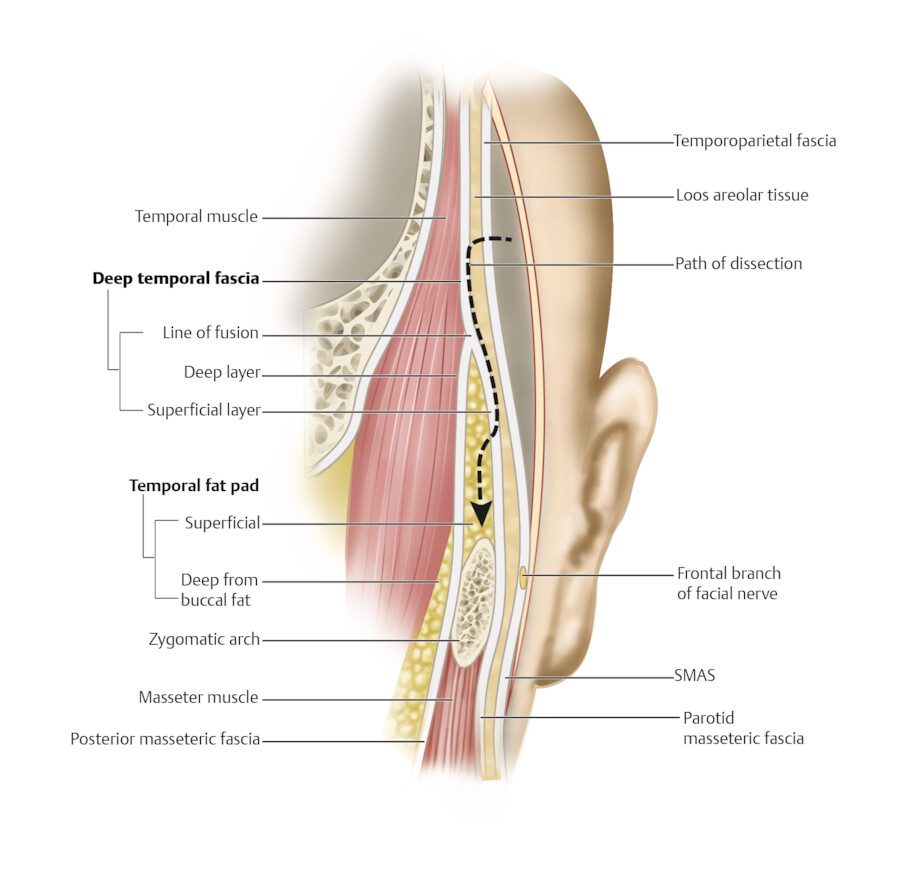
The temporal fossa contains a complex layering of soft tissues. From superficial to deep, the outermost layers are the skin and subcutaneous tissue. Next is the temporoparietal fascia (superficial temporal fascia). This fascia consists of three distinct layers. 4 The temporoparietal fascia is continuous with the superficial musculoaponeurotic system (SMAS) in the midface and merges in the central forehead with the galea. 10 The frontal branch of the facial nerve lies deep to the temporoparietal fascia (Fig. 3.9). Next, the temporalis fascia is a dense layer of shiny white fascia that splits around the temporalis muscle, creating a superficial and deep layer. 4 The temporal line is the convergence of the deep and superficial layers of the temporalis fascia with the frontal periosteum. The temporal line meets the lateral margin of the galea to form the conjoint tendon. 10
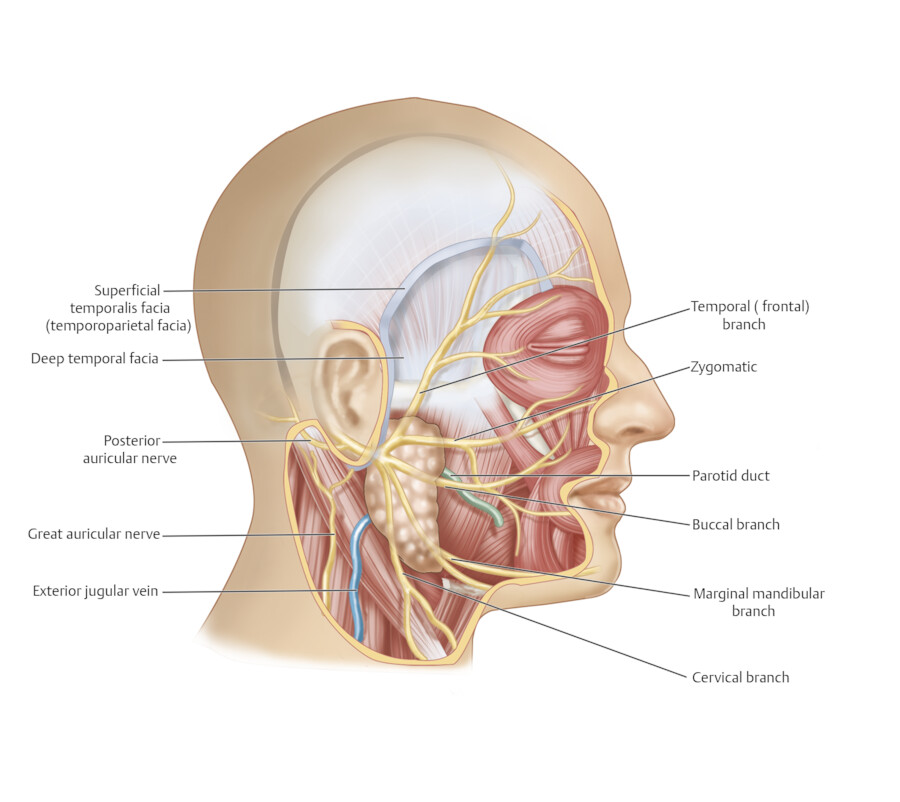
Muscle
The temporalis muscle sits in the temporalis fossa. It originates from the temporal fossa and inserts onto the coronoid process of the mandible, medial to the zygomatic arch. The temporalis is a muscle of mastication.
Fat Pads
The temporal fat pad is divided into a superficial and deep fat pad. 11 The superficial fat pad is immediately superior to the zygomatic arch between the superficial and deep layers of the temporalis fascia (Fig. 3.10). 11 The deep fat pad is deep to the deep layer of the temporalis fascia and superficial to the temporalis muscle. 11 This fat pad is posterior to the zygomatic arch and is continuous with the buccal fat pad. 11
Innervation
The maxillary division of the trigeminal nerve (V2) provides temporal sensation by the auriculotemporal and zygomaticotemporal branches. 10 Cranial nerve V innervates the temporalis muscle.
Vasculature
The superficial temporal artery and vein are found within the temporoparietal fascia. The sentinel vein is the key venous anatomy in browlifting. The sentinel vein runs superficial to the temporalis fascia near the region of the frontozygomatic suture. 10 The location of this vein is a marker for the frontal branch of the facial nerve which runs superficial to the sentinel vein. 10 Identification of this vein, particularly in endoscopic approaches indicates the inferior extent of dissection.
3.4 Periorbital Anatomy
3.4.1 Upper and Lower Eyelids
Topography
The palpebral opening in adults is 10–12 mm vertically and 28–30 mm horizontally. 6 The palpebral opening has a slight superior cant, with the lateral canthus about 2 mm superior to the medial canthus. 6 In adults, the upper eyelid covers 1–2 mm of the superior cornea and the apex of the upper lid margin is nasal to a vertical line drawn through the center of the pupil. 6 In Caucasians, the crease is 7–8 mm above the lid margin in men and 10–12 mm in women. 6 The lower eyelid margin sits at the inferior limbus of the cornea with a slight crease that is 2 mm below the lash line medially and 5 mm laterally. 6
Soft Tissue
The upper and lower eyelids are divided into an anterior, middle, and posterior lamella. The anterior lamella is the eyelid skin and underlying orbicularis muscle. The middle lamella is the orbital septum. The orbital septum is an extension of the arcus marginalis, a band of thickened periosteum at the orbital rim. The posterior lamella includes the tarsal plate, eyelid retractors, and conjunctiva. The tarsal plate is a dense connective tissue structure along the margin of the upper and lower eyelid. The tarsal plate attaches to the periosteum of the orbital rim by the medial and lateral canthal tendons. Medially, the canthal tendon has a deep attachment to the posterior lacrimal crest and a superficial attachment to the anterior lacrimal crest. 6 Laterally, the canthal tendon has a deep attachment 3 mm posterior to the orbital rim at Whitnall tubercle. 6
Muscles
The orbicularis oculi is a circular muscle that surrounds the eye. It is divided into an orbital, preseptal, and pretarsal section based on the anatomy beneath these sections. It functions to blink, squint, and forcefully close the eyelid, and its orbital component is a depressor of the forehead. 6 The orbital section arises from the medial canthal tendon, arches along the orbital rim, and meets laterally at the zygoma. 6 The orbital fibers of the orbicularis muscle interdigitate superiorly with the frontalis muscle fibers, pulling the skin of the forehead and eyelid downward, while elevating the cheek toward the eye, resulting in dynamic “crow’s feet.” 6 The preseptal fibers overlie the orbital septum. The pretarsal fibers are firmly adhered to the tarsus and travel in an elliptical path around the palpebral fissure.
Upper Eyelid Retractors
The upper eyelid retractors are responsible for elevation of the upper eyelid. The main retractor is the levator palpebrae superioris muscle. The levator arises from the orbital apex. The muscular portion is 40 mm in length with a terminal tendinous sheath that extends for 14–20 mm, called the levator aponeurosis. 12 The muscle transitions to the tendon at Whitnall ligament. The central portion of the levator aponeurosis joins the orbital septum and together they insert into the overlying eyelid skin and orbicularis forming the eyelid crease (Fig. 3.11). The levator continues inferiorly and inserts onto the superior tarsal surface. The levator palpebrae superioris is innervated by CN III. 6
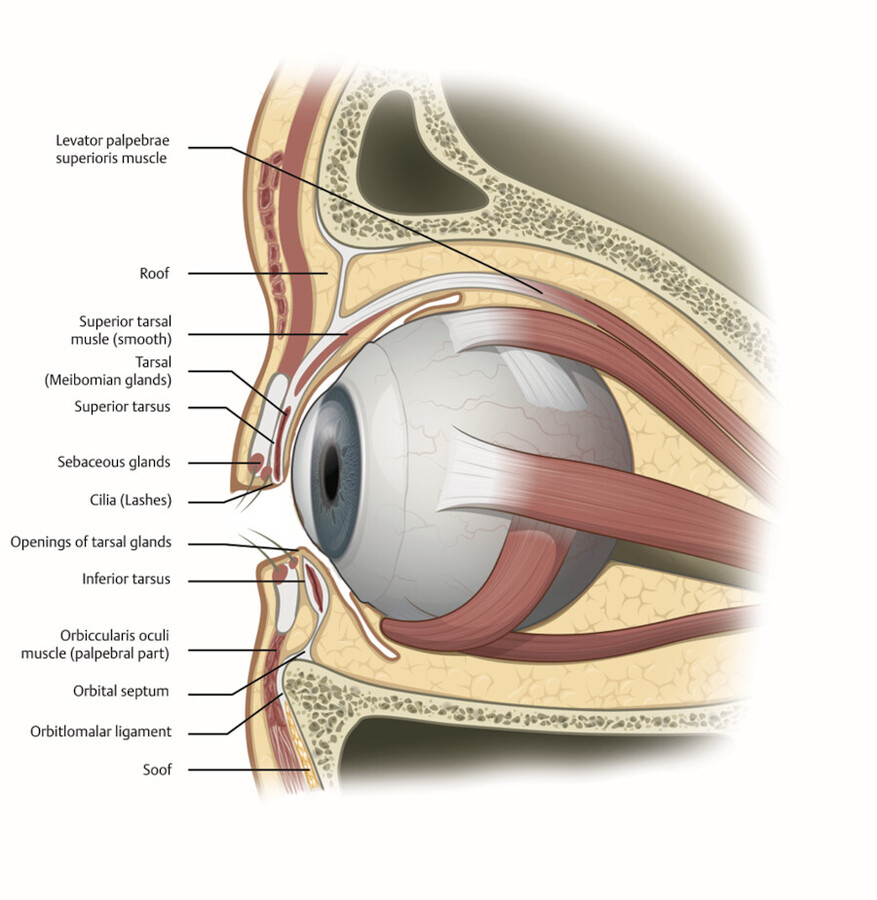
Müller muscle is an accessory upper eyelid retractor. It is a smooth muscle that is posterior to the levator and firmly attached to the conjunctiva deep to it near the superior margin of the tarsus. 6 Unlike the levator palpebrae superioris, Müller muscle is sympathetically innervated. 6 It contributes about 2 mm to upper eyelid retraction. 6
Lower Eyelid Retractors
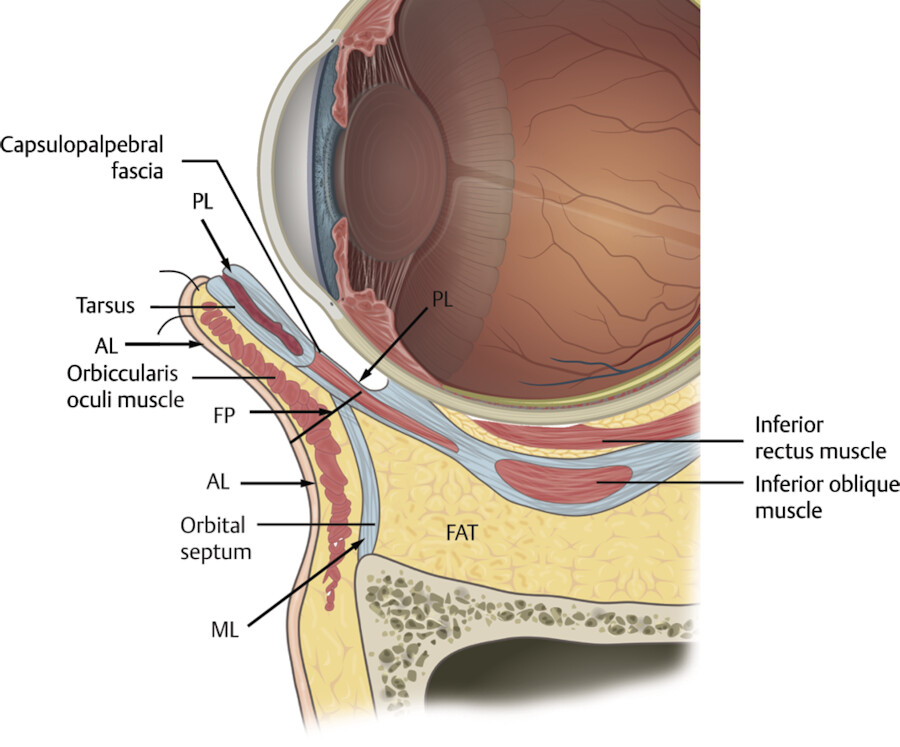
The lower eyelid retractors are the capsulopalpebral fascia and the inferior tarsal muscle. They correspond to the levator aponeurosis and Müller müscle in the upper eyelid, respectively. The capsulopalpebral head originates from the fascia of the inferior rectus muscle and then envelopes the inferior oblique muscle to become the capsulopalpebral fascia, inserting on the inferior tarsal border with the orbital septum (Fig. 3.12). 6 The inferior tarsal muscle has sympathetic innervation and is located posterior to the capsulopalpebral fascia. 6
Fat Pads
Upper Eyelid
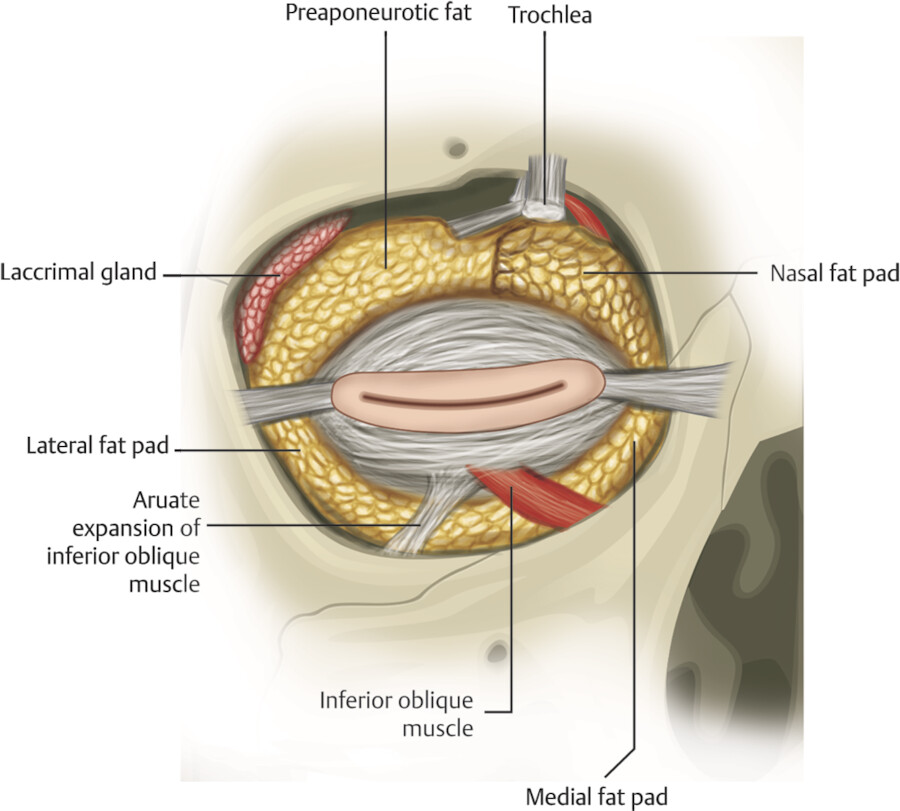
Two orbital fat pads are found posterior to the septum:the medial (nasal) fat pad and the central (preaponeurotic) fat pad (Fig. 3.13). The medial fat pad is whiter than the yellow central fat pad. The central fat pad is just anterior to the levator aponeurosis. The lacrimal gland is found posterior to the septum in the lateral space. The central fat pad is encased in a thin membrane which harbors small blood vessels and is innervated by terminal branches of the supraorbital nerve. 13 The trochlea of the superior oblique muscle separates the medial and central fat pads (Fig. 3.13).
Lower Eyelid
There are three postseptal fat pads in the lower eyelid complex: medial, central, and lateral. The inferior oblique muscle divides the medial and central fat pads while its arcuate expansion divides the central and lateral fat pads (Fig. 3.13). 14
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree