Secondary Neonatal Brachial Plexus Palsy Reconstruction
Joshua M. Adkinson
DEFINITION
Neonatal brachial plexus palsy (NBPP) results from injury to any brachial plexus nerve root (C5-T1) during a difficult delivery.1,2
Persistent paralysis and progressive spasticity, contractures, joint instability, and bony deformities of the upper extremity may occur in children with incomplete recovery of nerve function.
The type, severity, and manifestations of NBPP vary greatly between patients and surgical options for treatment must be individualized.
ANATOMY
Most commonly, the C5C6 roots are involved (Erb palsy), leading to deficits of shoulder abduction and external rotation (supraspinatus, infraspinatus, and deltoid), elbow flexion (biceps brachii, brachialis), and forearm supination (supinator).
C7 involvement causes paralysis of the subscapularis, teres major (TM), clavicular head of the pectoralis major (PM), brachioradialis (BR), extensor carpi radialis longus (ECRL) and brevis (ECRB), and possibly extensor carpi ulnaris and extensor digitorum communis (EDC). This leads to the classic “waiter tip” posture,3 with deficits of wrist and finger extension.
Rarely, the C8T1 roots alone are affected (Klumpke palsy), leading to weakness/paralysis in the wrist/finger flexors and hand intrinsic muscles.
Complete plexus involvement (C5-T1) leads to a flail extremity.
PATHOGENESIS
Between 50% and 92% of patients with NBPP experience complete recovery of function without primary nerve reconstruction.1,4,5,6,7,8 In those with persistent deficits, the clinical findings will vary over time.
Secondary deformities are impacted by the severity of the initial nerve injury, extent of muscle recovery, patient age at presentation, and previous treatments.
In addition to paresis/paralysis of affected muscles, co-contracture of antagonistic muscles can occur in patients with partial recovery.9 This may lead to contracture and/or joint deformity.
The most common posture in children with NBPP is internal rotation of the shoulder, flexion of the elbow, supination of the forearm, and ulnar deviation of the wrist, with variable involvement of the fingers.10 Many children also develop a limb-length discrepancy.
PATIENT HISTORY AND PHYSICAL FINDINGS
The preoperative evaluation of children with secondary NBPP deformities includes a detailed history, an assessment of functional limitations, and measurements of active and passive range of motion.
Grading function
No grading systems are universally recommended for assessment of elbow, forearm, wrist, and hand function in patients with NBPP.
Physical Examination
Function is observed, active and passive ranges of motion are documented, and muscle strength is assessed with and without gravity.
Elbow
Co-contracture of the elbow flexors and extensors are assessed. Dislocation of the radial head and proximal ulna are noted.
Forearm
Long-standing supination or pronation deformities may lead to fixed contracture of the interosseous membrane (IOM). Continued growth can then lead to bowing of the radius and ulna, dorsal dislocation of the distal ulna, and/or posterior dislocation of the radial head.
Wrist
Ulnar deviation is common because of paralysis of the ECRL and ECRB.
Hand
Limited metacarpophalangeal (MCP) joint extension is common, as is thumb instability.11
IMAGING
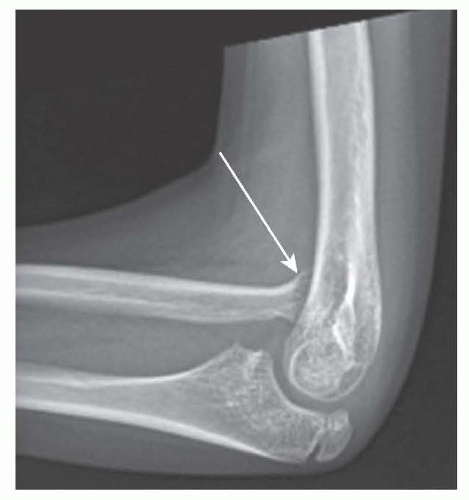
Anteroposterior and lateral radiographs of the elbow or wrist may be obtained to evaluate for joint subluxation/dislocation or articular deformities (FIG 1).
NONOPERATIVE MANAGEMENT
All patients should undergo physical therapy, with the goal of muscle strengthening and full passive range of motion of the elbow, forearm, wrist, and fingers.
Orthoses are used to maintain anatomic joint alignment and to prevent contracture.
Botox injection into spastic musculature is effective for temporary (3-6 months) muscle weakening.
SURGICAL MANAGEMENT
Surgical options include tendon transfers, arthrodeses, osteotomies, muscle/tendon releases, and functioning muscle transfers.
Secondary reconstruction of the elbow, forearm, wrist, and hand is considered in children older than 4 years with
incomplete recovery of upper extremity function after primary reconstruction or in those who present after the optimal window for nerve reconstruction.10,12,13,14,15
Restoration of elbow flexion is the priority, followed by wrist extension, thumb/finger flexion, wrist flexion, thumb/finger extension, and intrinsic hand reconstruction.
Elbow flexion contractures greater than 40 degrees are an indication for surgical release. Less significant contractures can be released, but this may cause clinically significant elbow flexion weakness.
Weak elbow flexion (less than MRC grade 3) may be addressed via Steindler flexorplasty or transfer of the latissimus dorsi (LD), PM, or triceps.
The surgical approach to the forearm depends upon the underlying deformity. Supination contractures are best treated by a biceps rerouting. If there is minimal passive range of motion, IOM release or pronation osteotomy of the radius is recommended.
Pronation deformities are treated by pronator teres (PT) release or rerouting. One must ensure good passive supination prior to PT rerouting.
Weak wrist extension can be managed by transfer of the flexor carpi ulnaris (FCU) to the ECRB or ECRL (to counterbalance an ulnar deviation force). Weak finger extension can be managed with a combination of palmaris longus/flexor digitorum superficialis (FDS)middle or FDSmiddleFDSring transfer to the extensor pollicis longus (EPL) and EDC tendons, respectively.
In patients with a total (pan-plexus) palsy, free functioning muscle transfers (eg, contralateral LD, gracilis, rectus femoris) are the procedure of choice.
Preoperative Planning
Radiographs of the affected extremity should be reviewed, if relevant.
Positioning
The patient is positioned supine on the operating room table with the affected extremity on a hand table. A well-padded tourniquet is placed high on the arm for procedures distal to and including the elbow.
For pedicled LD muscle transfer, the patient is placed in the lateral decubitus position.
The gracilis muscle harvest requires a frog leg position.
Approach
Elbow approach: The muscles causing an elbow flexion contracture (brachialis, biceps brachii, and BR) are approached via an antecubital incision.
Procedures to restore elbow flexion require a techniquespecific approach.
Forearm approach: The biceps tendon is approached through an antecubital fossa incision. The entire length of the tendon and portion of the radius under which the tendon is rerouted must be visualized.
Wrist/fingers approach: Procedures to restore wrist and finger function require a technique-specific approach. The FCU tendon may be approached through a single longitudinal incision or several stepcut incisions.
Free functioning muscle transfers to restore finger flexion require an extensile approach from the anterior upper arm across the acromion and lateral clavicle. This provides full visualization of the proposed site of origin of the transferred muscle as well the adjacent neurovascular structures to be protected and/or used for vascular anastomoses and nerve coaptation.
TECHNIQUES
ELBOW RECONSTRUCTION
▪ Elbow Release
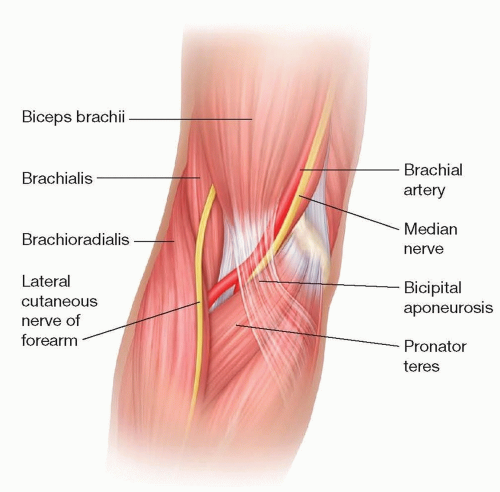
Landmarks: median nerve, radial nerve, lateral antebrachial cutaneous nerve (LABC), brachial artery, brachialis muscle, biceps brachii muscle, BR (TECH FIG 1)
Depending on the severity of the contracture, a curvilinear or Z-plasty incision is made and the lacertus fibrosus is identified and divided (TECH FIG 2A,B).
The median nerve/brachial artery is identified and retracted medially and the LABC is retracted laterally.
If fractional lengthening is indicated, then two incisions 1 cm apart are made with electrocautery at the musculotendinous junction of the brachialis. The anterior half of the BR is elevated from the humerus while protecting the radial nerve. The medial half of the biceps tendon is incised distally and the lateral half proximally to provide lengthening. The release is reinforced with 3-0 braided suture, as needed.
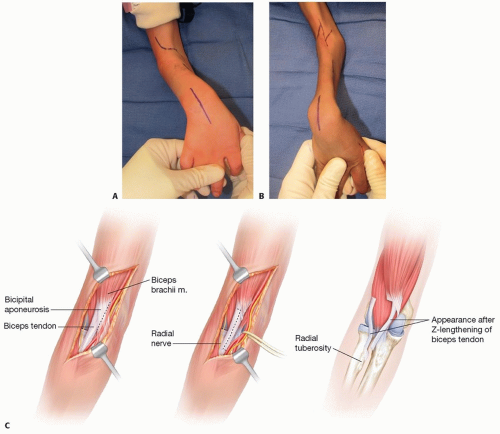
TECH FIG 2 • Approaches to elbow release. A. Curvilinear approach to the elbow. B. Z-plasty approach to the elbow. C. Steps in a biceps Z-lengthening.
If a full release is indicated, then the biceps tendon is Z-lengthened16 (TECH FIG 2C), the brachialis is divided, and the BR is completely elevated from the humerus while protecting the radial nerve. The anterior elbow capsule is incised, if necessary. In long-standing contractures, foreshortened neurovascular structures will limit full passive elbow extension.
The biceps tendon is reapproximated using 3-0 braided suture with the elbow in 30 degrees of flexion (TECH FIG 2D).
The skin is closed in layers (TECH FIG 2E).
▪ Restoration of Elbow Flexion
Steindler Flexorplasty (TECH FIG 3)
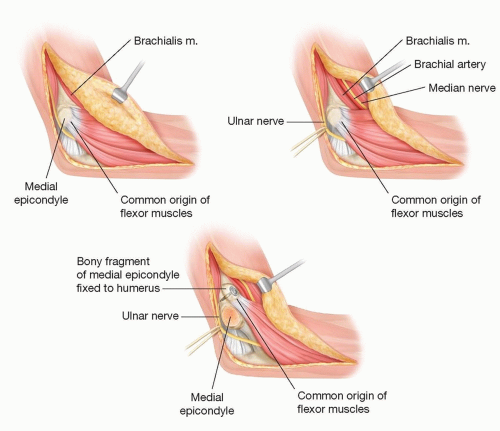
Landmarks: medial epicondyle, median nerve, ulnar nerve, brachial artery, humerus, biceps brachii muscle, brachialis muscle
Fifteen-centimeter medial elbow curvilinear incision is made, and the skin flaps are elevated above the fascia while protecting the medial antebrachial cutaneous nerve.
The ulnar nerve is retracted medially and the median nerve and brachial artery are retracted laterally.
The flexor-pronator mass is freed from osseous attachments distally. Using an osteotome, the flexor-pronator origin at the medial epicondyle is elevated with a 2-cm segment of bone.
The humerus is exposed deep to the brachialis. Approximately 5 to 7 cm proximal to the elbow joint, a bur is used to create a cortical window in the humerus.17
With the elbow in 130 degrees of flexion, the medial epicondyle/flexor-pronator mass is secured to the humeral corticotomy using a 3.5-mm compression screw over a washer.
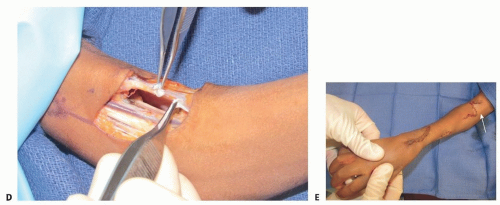
TECH FIG 2 (Continued) • D. Z-lengthened biceps tendon prior to reapproximation. E. Wound closure with a Z-plasty at the elbow (arrow).
The ulnar nerve is transposed anteriorly to prevent tethering and the muscle is closed over the exposed osteotomy site using absorbable suture.
The skin is closed in layers.
Latissimus dorsi Transfer (Pedicled) (TECH FIG 4)
Landmarks: thoracodorsal neurovascular bundle, rhomboid muscle, teres major and minor muscles, acromion, clavicle, biceps brachii tendon
Bipolar (moving the muscular origin and insertion) transfer is preferred because it increases the mechanical efficiency of the transfer and decreases the chance of vessel twisting/kinking.18
Harvest—5-cm wide elliptically oriented skin paddle (8 cm distal to the axilla) is designed over the midaxis of the muscle and incised with superolateral and inferomedial extensions.
The skin flaps are elevated off of the muscle and the arm is fully abducted and flexed.
The muscle is marked at resting tension using 3-0 silk sutures placed at 5-cm intervals.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree