Eyelid Coloboma
Adam R. Sweeney
Christopher B. Chambers
DEFINITION
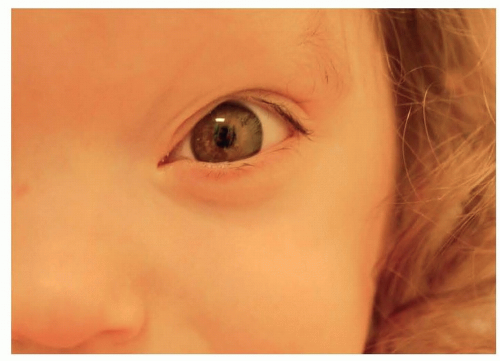
Eyelid coloboma (plural: colobomata) is a congenital anomaly arising from developmental interruption of the eyelid folds causing an eyelid cleft in either the upper or lower eyelid.
ANATOMY
The classic description of an eyelid coloboma is a full-thickness defect of a segment or an entire eyelid including absence of the conjunctiva, tarsus, orbicularis muscle, and skin.
The term “pseudocoloboma” may be used to refer to a partial-thickness defect of the lid, usually involving the deeper structures with intact superficial layers.
There is considerable variability in involvement including only a slight lid indentation to complete lid absence with underlying ocular abnormalities.
The majority are found in the medial third of the upper lid.
PATHOGENESIS
The etiology of eyelid colobomata is not fully understood and likely varies.
Variability in the formation of the eyelid folds early in embryogenesis vs later disruption of eyelid fusion/fissure may implicate the location of a coloboma defect and any associated facial clefts.2,4
Attributed etiologies include intrauterine amniotic bands, abnormalities in vitamin A metabolism, intrauterine inflammation, decreased placental circulation, hamartomas, abnormal fetal vasculature, failure of eyelid fold fusion, or abnormal fetal migration of the neural crest cells.5-7
Colobomata may occur in conjunction with Goldenhar syndrome (oculoauriculovertebral dysplasia),1,8 Treacher Collins syndrome (mandibulofacial dysostosis),3 frontonasal dysplasia, and Delleman syndrome.9 Goldenhar syndrome is associated with unilateral upper lid coloboma, whereas Treacher Collins is associated with lower eyelid coloboma or pseudocoloboma.2
NATURAL HISTORY
Untreated, an eyelid coloboma may lead to neonatal exposure keratopathy with corneal ulceration and perforation.
A small coloboma associated with the appropriate amount of superior rotation of the eye upon eye closure, known as a Bell reflex, may be asymptomatic requiring only cosmetic surgery later in life.
PATIENT HISTORY AND PHYSICAL FINDINGS
Careful physical examination should be performed to assess the thickness and extent of eyelid loss in both upper and lower eyelids of both eyes. Attention should be given to the degree of skin laxity for anticipated donor lids, integrity of anchor sites on the involved lid, and skin color/thickness.10
Fornices of eyelids should be meticulously examined for adhesions (symblepharon) that may hint at underlying diagnosis of cryptophthalmos.
Full ophthalmic examination with cycloplegic refraction, eye motility examination, external examination, slit-lamp examination and dilated fundus examination should be performed to identify other regions of adverse development.
Both eyes should be closely examined.
The most common finding is an upper eyelid medial fullthickness abnormality. The defect is typically a triangular or quadrangular lesion with the base toward the eyelid margin (FIG 1).1,6,11
The defect may vary in severity from a small indentation to the full eyelid length.
If present in the lower eyelid, partial-thickness defects are more common.
DIFFERENTIAL DIAGNOSIS
Associated syndromes:
Goldenhar syndrome (epibulbar dermoids, preauricular appendages, blind pretragal fistulae, hemifacial atrophy, vertebral anomalies)1,8
Treacher Collins syndrome (lower eyelash irregularities, absence of lower puncta, iris coloboma, microphthalmos, midface hypoplasia, lateral downward slant of the palpebral fissures)3
Delleman syndrome (orbital cysts, intracranial cysts, skin appendages)9
Other facial clefting syndromes affecting the eyelids; as described by Tessier, facial clefts
Eyelid trauma
Entropion
Cryptophthalmos
NONOPERATIVE MANAGEMENT
A small eyelid coloboma with mild corneal exposure may be treated with lubrication, bandage contact lenses, or moisture chambers with surgery deferred until 6 months of age or later when pediatric eyelid tension has relaxed.3
SURGICAL MANAGEMENT
Surgical correction is the preferred method of treatment.
Surgery is required and urgently indicated in cases where exposure keratopathy is present or imminent.
Preoperative Planning
General anesthesia is recommended for pediatric cases.
Review the facial photos and examination including size, location, and shape of the lid defect to help determine the appropriate technique.
Positioning
The patient is positioned supine on a surgical table with an adjustable headrest lowered to give the surgeon the best access. The patient should be prepped and draped leaving the full face exposed.
Approach
Upper or lower eyelid lesions involving ¼ of the eyelid or less may be amenable to direct closure.
Upper or lower eyelid lesions involving a quarter to half the eyelid are treated with Tenzel semicircular flap.
Large lesions with significant tissue loss involving ½ or more of the eyelid may be managed via a one-stage graft technique involving a tarsomarginal graft from the ipsilateral lower intact lid or from the contralateral intact upper eyelid.12
For lesions with greater than ½ eyelid tissue loss and not amenable to a one-stage closure, a two-stage lower lid rotation to the upper lid via a Cutler-Beard technique may be employed.13
The vast majority of large colobomata involving greater than ½ of the eyelid involve the upper eyelid; thus, techniques specifically addressing upper eyelid repair are described below. One-stage and two-stage grafting for lower eyelid closures are routinely performed and described for other conditions; however, these are out of the scope of this chapter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree