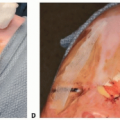
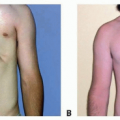
Burned Hand Reconstruction
David A. Billmire
Kim A. Bjorklund
DEFINITION
More than 80% of all severe burns involve the hand.1
These injuries may be devastating with long-term functional consequences and significant morbidity.
Burns of the pediatric hand are common and are most frequently thermal type injuries (scald, contact, or flame burns).2
Injuries tend to occur accidently as children explore their environment with their hands.
However, a glove or stocking appearance to a burn, or an injury not consistent with the history, should prompt concerns for abuse.
Hand function may be affected through tissue loss, burn scar contractures, impaired growth, and abnormal sensation.
ANATOMY
Pediatric skin is thinner and has not yet developed the thickened palmar epidermis of an adult.3
Dorsal skin is thin and pliable and provides less protection for underlying extensor tendons and bone.
PATHOGENESIS
Thin dorsal skin places underlying structures at particular risk for exposure and stiffness.
Extensor tendons are particularly at risk at the PIP joints where the central slip may attenuate or rupture with exposure, resulting in a boutonniere deformity.
Burned hands tend to assume a position of wrist flexion, MCP hyperextension, PIP flexion, thumb adduction, and interphalangeal hyperextension.4
Early elevation, splinting, and escharotomies when indicated affect postburn edema and help prevent the development of burn contractures.
Altered sensation and motor and nerve function may occur secondary to the burn.
NATURAL HISTORY
Untreated or inadequately treated hand burns frequently result in contractures and long-term functional impairment.
Early involvement of a multidisciplinary team with aggressive elevation, splinting, hand therapy, and early excision and grafting for deep burns is essential.
Hand burns that are unlikely to heal within 2 weeks of injury should undergo tangential excision and skin grafting.5
Palmar burns are more likely than dorsal burns to heal spontaneously from glabrous skin appendages and may be less likely to require grafting.
Approximately 78% of pediatric palm burns heal without the need for grafting; however, flexion contractures of the fingers and/or shortening of the thenar-hypothenar distance may occur when burns take greater than 2 to 3 weeks to heal.6,7
Secondary burn deformities may occur as a child grows because burn scars do not grow at the same rate as the rest of the child’s hand and may impede overall bone and soft tissue growth.3
Secondary burn deformities include intrinsic minus deformities (“claw hand”); palmar cupping deformity; web space deformities; hypertrophic scars and/or scar bands; finger deformities including boutonniere, swan neck and mallet deformities; and deformities of the nail.8
PATIENT HISTORY AND PHYSICAL FINDINGS
Evaluation of the location, size, depth, and previous treatment of the burn
Mechanism of injury (thermal, contact, chemical, electrical)
Previous splinting and hand therapy
Nature of the contracture (extension, flexion)
Skin and soft tissue adequacy and contracture
Tendon function—flexor and extensor
Assessment of sensation and vascular status of the hand and digits
Joint contractures—passive and active range of motion
Bony deformities and inadequate growth
Assessment of the entire upper extremity
Wrist or elbow contractures may need to be addressed to adequately position the hand in space.
IMAGING AND DIAGNOSTIC TESTS
Plain radiographs of the hands and digits should be assessed for bony deformities, joint contractures, or destruction.
SURGICAL MANAGEMENT
Surgical intervention is warranted for functionally significant contractures not improving with stretching and splinting.3
Multiple surgeries may be required as a child grows for recurrent contractures.
Thumb reconstruction
The thumb contributes up to 50% of function of the hand, and secondary reconstruction is critical in restoration of hand function.
When thumb loss remains distal to the interphalangeal joint, function is reasonably well preserved.9
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree