Prominent Ear
Akira Yamada
Arun K. Gosain
DEFINITION
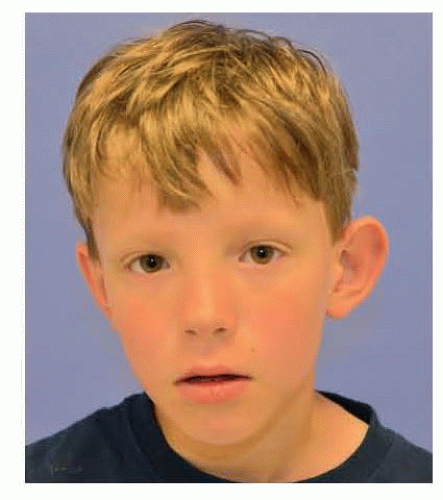
Prominent ears are a common abnormality, affecting about 5% of children. When observing other people’s faces, the first thing we pay attention to is the facial triangle, eye-mouth-eye. The auricle is usually not the primary area of attention. However, if the auricle is projected more than 25 mm from the head, it tends to catch the attention of human eyes as “prominent.”
ANATOMY
The main components of the prominent ear are (1) loss of antihelical fold, (2) concha scapha angle greater than 90 degrees, and (3) conchal cartilage excess (FIG 1).
PATHOGENESIS
The most common etiology of the prominent ear is effacement of the antithetical fold. Also a deep conchal bowl (greater than 1.5 cm) frequently contributes to the overall pathogenesis. Combination of these two is very common.
PATIENT HISTORY AND PHYSICAL FINDINGS
Five parameters should be assessed systematically to ensure that all components of the prominent ear deformity are recognized: (1) auriculocephalic angle, (2) scapha-conchal angle, (3) relationship of the antihelix to the helix, (4) horizontal distance from the most lateral aspect of the helix to a point perpendicular to the skull, and (5) depth of the conchal bowl.
NONOPERATIVE MANAGEMENT
If the patient presents in infancy, preferably less than 1 month of age, ear molding techniques may be indicated. Success of ear molding progressively diminishes after the first month of life, and after age 2 months, surgery is the only reliable option to correct the prominent ear.
SURGICAL MANAGEMENT
If the distance from the head to the top of helix at any point is over 25 mm, it is considered to be a prominent ear.
Because the prominent ear could be the target of bullying and ridicule during school age, the most popular timing of surgery is before the start of primary school.
There seems to be a slightly different prominent ear concept among different cultures. Generally speaking, Asian countries are more tolerant to prominent ear, because the “big ear” is a good sign of luck and wealth.
Preoperative Planning
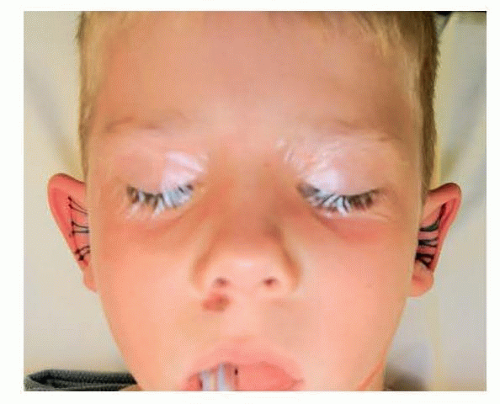
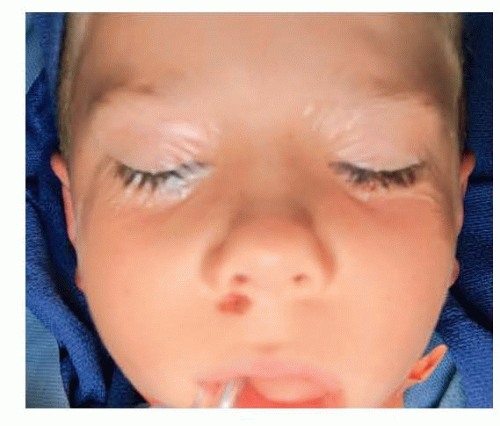
Preoperative anthropometric measurement of the auricle is extremely important to achieve symmetry of the projection of the auricle postoperatively. The direct measurements also help to assess the nature of prominence. For example, if the patient has more prominence in the lower pole (25 to 30 mm), it is likely that conchal hypertrophy exists. To assess the degree of projection, the authors recommend measuring at least three points (eg, upper, middle, and lower) from the head to the top of helix. An otoplasty grid provides objective data of projection from the top to the tail of the helix (FIG 2). In case of unilateral prominent ear, otoplasty grid taken from normal data can be used as an intraoperative template to achieve symmetry (FIG 3).
Prediction of the Projection Reduction
20 mm distance from the mastoid to the peak of helix is acceptable projection, especially in Asian countries. In the United
States, somewhere between 15 to 20 mm is the reasonable goal to achieve. The trend of ear projection in the patient’s family is a good indicator for the targeted height of projection.
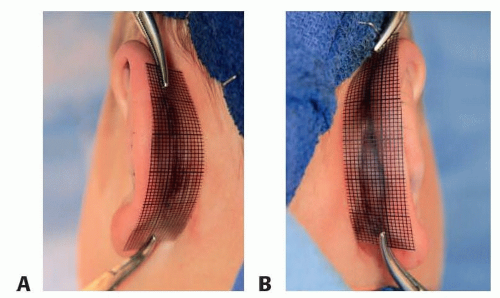 FIG 3 • Otoplasty grid is used to assess the postop helix-mastoid distance on the (A) left and (B) on the right. |
Preoperative Quantification of Prominence by Otoplasty Grid
After determining the goal of projection, the authors create a customized otoplasty grid for the patient, with a planned projection from the mastoid to the peak of the helix (15 mm in FIG 2). Upon placing the grid at the back of the auricle, one can visualize the amount of reduction needed for surgery.
Positioning
Approach
Most cases need a combined approach to correct the deformities. Among numerous techniques reported in the literatures, Mustardé mattress sutures are the most commonly used method to create the antihelical fold.3
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree