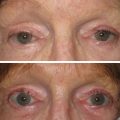
Rhinoplasty, the quintessential “nose job,” is considered to be the most complex and challenging cosmetic procedure that exists in aesthetic surgery today. Nevertheless, it remains an extremely popular surgery for men and women. Its popularity has steadily increased over the years, nearly as rapidly as procedures such as liposuction or aesthetic breast surgery.
Surgeons that elect to make rhinoplasty part of their repertoire must be dedicated to continual learning and improvement, which takes considerable dedication. It is a surgery that deals in micrometers versus inches and involves a structure that is strategically placed in the middle of the face, where any mistake can be extremely obvious. To make matters more challenging, there is unquestionably no single method or technique that can work for all noses. It is essential to have a systematic method for evaluating the nose and treatment planning. A completely dogmatic protocol is impossible to create, since the nose is made up of a mixture of various skin types, cartilaginous shapes, and bony deformities that can challenge the most experienced surgeon. Another diagnostic challenge is the fact that many patients seeking rhinoplasty or revision rhinoplasty may have some degree of body dysmorphic disorder (BDD). The most notable to be mindful of are those who fall into a well know acronym category called SIMON – Single Immature Male Obsessive Narcissist. Unfortunately, many patients such as SIMONs and other BDD patients can appear relatively normal during the consultation phase. Still, all efforts should be made to discover mental issues and unrealistic expectations before any surgery is performed.
An isolated chapter dedicated to rhinoplasty will without doubt be only an overview and hopefully create a good basic general knowledge, but in no way can give the breadth of knowledge required to be an expert in rhinoplasty. There have been many giants in the field of rhinoplasty that have dedicated their lives to understanding this exciting procedure such as Dean Toriumi, Gilbert Aiach, Jack Sheen, Jack Gunter, Eugene Tardy, Rod Rohrich, and John Tebbetts, all of whom have multiple publications on rhinoplasty that are worth reading. This chapter seeks to give a basic understanding of classic rhinoplasty, along with an anatomic basis for typical techniques shown in a somewhat step-by-step fashion. Classic more advanced maneuvers are also reviewed here, particularly when it serves to improve or preserve a functional outcome in addition to the cosmetic enhancement. There is also a section on cosmetic rhinoplasty in the older cleft lip and palate patient.
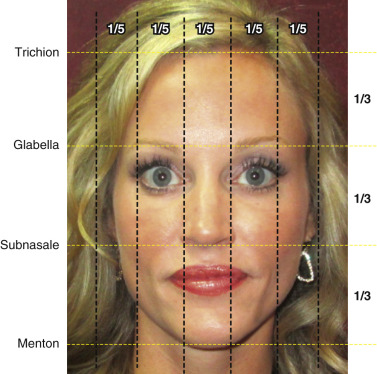
Great rhinoplasty surgeons would likely agree with Leonardo Di Vinci who, 500 years ago, demonstrated how important facial proportion is to beauty. Nowhere is it more important than in the middle of the face, where the proportion of the nose is absolutely critical to the success of an operation. Understanding correct proportion and how to achieve this related to all subunits of the nose and how this relates to the face, is an absolute necessity prior to taking on the nuances and details of rhinoplasty itself ( Fig. 6.1 ). The extraordinary mix of suspended cartilages that make up the lower-half to two-thirds of the nasal structure is immeasurably key for achieving the desired aesthetic outcome. Nasal cartilages typically make up the majority of manipulation during rhinoplasty. Cartilage and/or bony manipulation are generally necessary to achieve a harmonious structure of the nose that is both aesthetically pleasing and functional. An absolute comprehension of nasal anatomy is paramount to appreciate the minutiae of rhinoplasty.
Anatomy
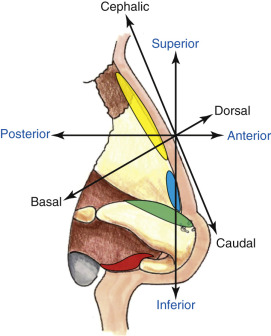
Terminology of surgical anatomy can be confusing for the novice rhinoplasty surgeon, particularly because the standard terms for direction ( superior, inferior, anterior, and posterior ) are not used to the same degree as the terms cephalad, caudal and dorsal/basal ( Fig. 6.2 ). The terms cephalic, dorsal and caudal, to describe positioning during rhinoplasty surgery is more specific due to patient positioning. Surgeons can use terms interchangeably and there are many other anatomic terms when describing the nose that may differ between surgeons such as using the word “nasal tip” versus “nasal lobule,” although most would describe the nasal tip as being the most projected point of the nose that is positioned between the two domes as well as between the supratip break and infratip break points. The tip of the nose is probably the most important area because of its location and all of the finer details that make up its shape ( Fig. 6.3 ). The ill-defined nose, which is often one with an amorphous tip, is simply one that has lost its tip-defining points. This may be due to genetic cartilage that is ill-defined, previous surgical damage, or thick skin that is hiding (camouflaging) the cartilaginous structure ( Fig. 6.4 ).
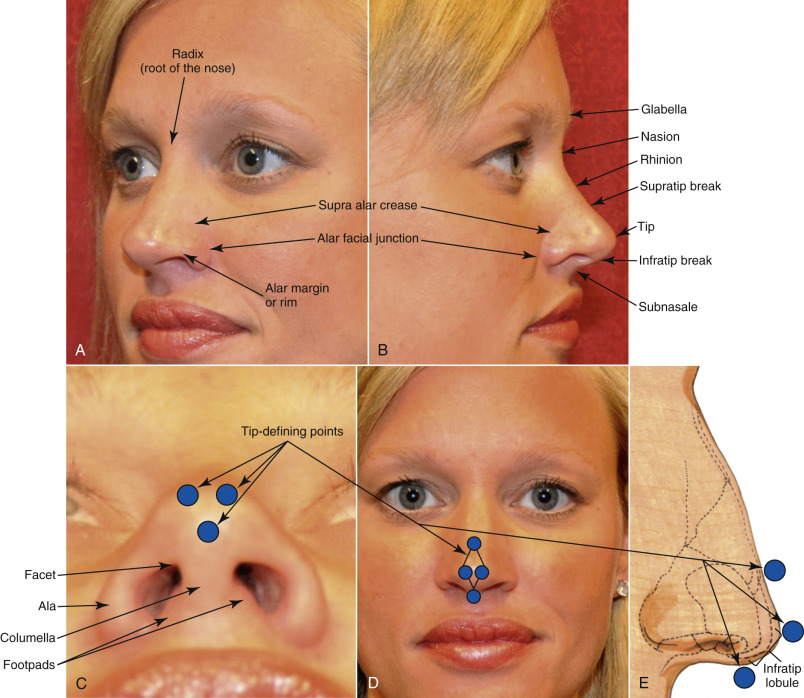
Skin thickness is an essential part of the nasal anatomy that must be recognized preoperatively. Typically, the thickness of the skin differs along the dorsum compared with the rest of the nose and nasal tip. In the root of the nose or Radix, the skin is comparatively thick and somewhat mobile. The thinnest skin of the nose is classically over rhinion, which is in the mid-dorsal region and is also quite mobile. The skin becomes thick again in the tip region where it is most adherent and typically more sebaceous in nature. The sebaceous nasal tip skin does not heal well from external scars. For instance, an external incision on the nasal tip for removal of a mole or because of injury often leaves an inferior quality scar compared with thin skin. Fortunately, the columella has minimal sebaceous glands compared with the tip and it heals nicely from an open transcolumellar rhinoplasty incision.
Nasal Musculature
The layer below the very thin subcutaneous level contains the nasal muscles. The muscles of the nose can be thought of as an extension of the SMAS (superficial musculoaponeurotic system), which is a fibromuscular layer that involves not only the muscles of the nose but extends laterally into the other facial musculature and is regularly used during facelifting. There is some argument whether or not a true SMAS exists or if it is simply a histologic diagnosis because of the thin nature of this fibrotic tissue investing the muscle. The muscles that make up the nose do function in facial expression and help with the function of breathing and animation during smiling. The muscles can be divided into elevators, depressors, compressors, and dilators of the nose. Typically, the muscles are paired and are extremely thin and much more superficial than the other muscles of the body ( Fig. 6.5 ).
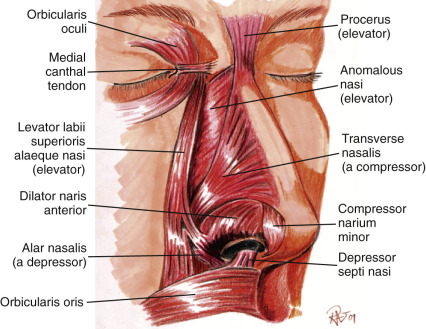
Because a good portion of the blood vessels course into the muscular layer, surgical dissection should be below the muscular layer that covers the bony and cartilaginous structures. Staying well below the nasal musculature helps prevent damage to vessels, nerves, and lymphatics. It also limits unnecessary bleeding that may lead to excessive ecchymosis, edema, and scarring.
Certain muscles do occasionally require surgical treatment. An overactive depressor septi nasi muscle can create a major ptotic displacement of the nasal tip when the person smiles. Transection of this muscle is easily accomplished to noticeably improve this deformity. Similarly, the dilators of the ala including the ala and nasalis muscle may occasionally be treated if excessive alar widening is noted on high smile. In general, the nasal muscles are avoided, particularly to prevent excessive bleeding and unwanted fibrosis.
Nasal Blood Supply
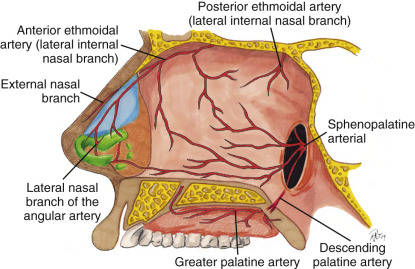
The blood supply to the nose and septum is extremely rich and comes from multiple sources. The most common nosebleed, for example, comes from Kiesselbach’s plexus on the septum, which is an area where there is convergence of three arterial sources: one from the branch of the superior labial artery, one from the branch of the sphenopalatine artery, and the other from the anterior ethmoidal artery ( Fig. 6.6 ).
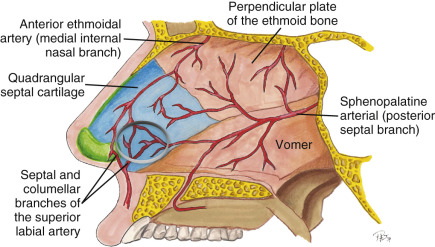
The rich vascular supply allows the nose to heal well with a very low risk of infection, as with most aesthetic surgeries of the face. A specific local anesthetic technique to help cause vasoconstriction of this rich blood supply during cosmetic rhinoplasty is critical to allow for a relatively bloodless field because of the delicate nature of the surgery.
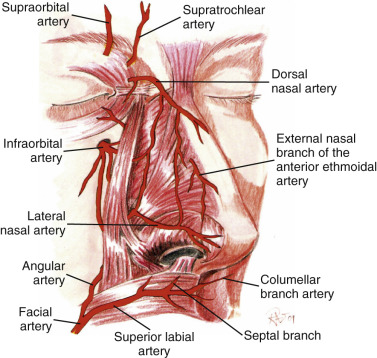
The robust blood supply to the lateral and external nose comes from both internal and external carotid arteries. While there are branches of the ethmoidal and superior labial artery extending to the nasal tip, the lateral nasal artery has an even stronger blood supply that supplies the nasal tip, which allows for transection of the columella without fear of ischemia at the nasal tip ( Fig. 6.7 ).
The significant plexus of the vessels arising from multiple sources have a venous and lymphatic network that is largely the same ( Fig. 6.8 ). Many believe nasal edema may be less from a closed rhinoplasty, although arguments can be made that there are adequate channels of lymphatic and venous drainage for open or closed rhinoplasty. Therefore, postoperative edema from rhinoplasty may be similar since postoperative drainage should be adequate for either technique if performed carefully.
Nasal Bone and Cartilage Anatomy
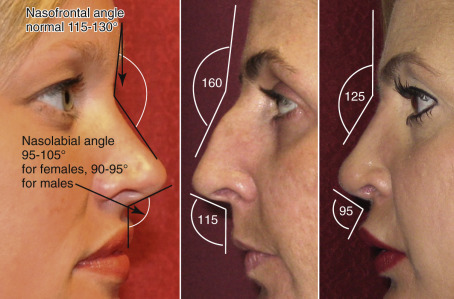
The bony vault at Nasion (nasofrontal suture) is the thickest and most solid portion of the nasal structure. It is made up by the paired nasal bones as well as the frontal process of the maxilla. The nasofrontal angle is an important clinical landmark as well as anatomic position for the junction of the frontal bones and nasal bones ( Fig. 6.9 ).
The nasal bones extend various lengths caudally to connect with the upper lateral cartilage and can overlap the cartilages by several millimeters.
At the root or base of the nose, the nasal bones are the most adherent. The bones thin significantly as they extend caudally toward the upper lateral cartilages. This root of the nose, where the bone is thickest, is a common area for rasping to lower a nasal dorsal hump in the cephalic portion. A very large nasal dorsal hump may require the use of a Rubin or other osteotome to reduce the bony dorsum ( Fig. 6.10 ).
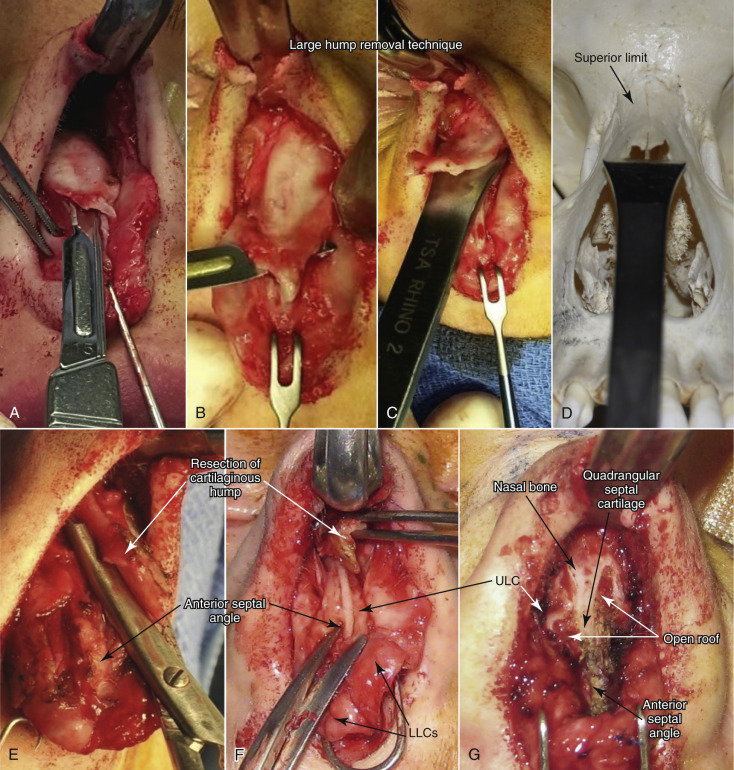
Ideally, rasping alone is enough to lower the bony hump on the majority of patients with average to small dorsal humps. The area of the cartilaginous hump most likely to be missed is the anterior septal angle (ASA) area. Inadequate reduction of the ASA, especially combined with over-resection or lack of tip support, can lead to a very unaesthetic “Polly Beak” deformity ( Fig. 6.11 ).
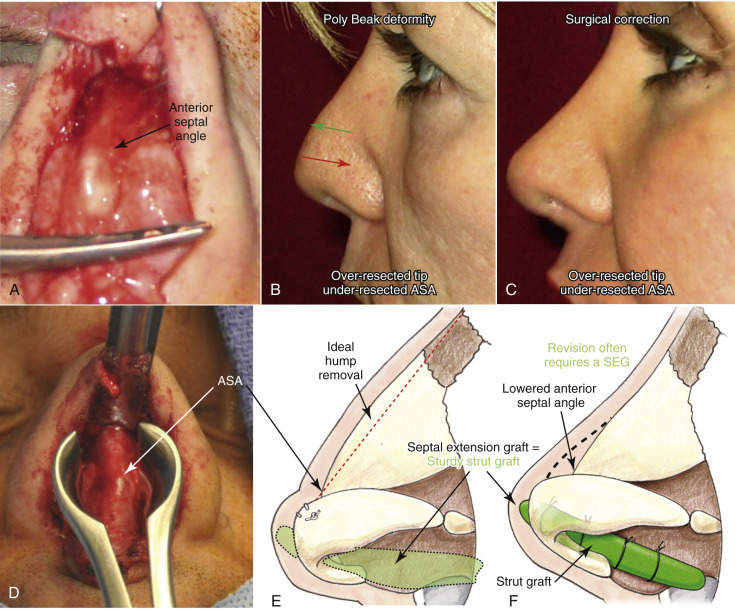
The cartilage and bone making up the nasal hump are quite variable in thickness as well as actual length. Patients with short nasal bones may be more at risk for internal nasal valve collapse ( Fig. 6.12 ). Valve issues occur more in this scenario because the middle nasal vault formed by long upper lateral cartilages have less bony support, thereby relying on less rigid cartilage.
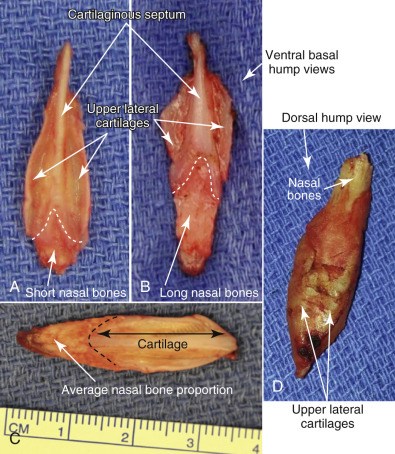
The nasal bones connect caudally to the paired upper lateral cartilages. There is a very firm attachment to the nasal bone and upper lateral cartilages, particularly along the medial edge adjacent to the septum. The upper lateral cartilages that can be found extending just over 5 mm beneath the nasal bones to allow for a more firm attachment. Extreme rasping with a coarser aggressive rasp can potentially dislodge the upper lateral cartilages from the nasal bone insertion creating a significant deformity if unrecognized. The upper lateral cartilages provide the majority of support in the middle-third of the nasal pyramid along with the anterior border of the nasal septum. The lateral cartilages continue along the anterior border of the septum with perichondrium covering both the superficial and deep surface.
The portion of upper lateral cartilages that connect to the nasal septum in the mid-vault region makes up a landmark, termed the “internal nasal valve” ( Fig. 6.13 ). The valve area is an extremely important region with regard to breathing compromised potentially before and after rhinoplasty surgery. The action of the dilating muscles on the lateral portions of the upper and lower lateral cartilages play a role in maintaining at least a 10- to 15-degree angle of the nasal valve to maintain adequate airflow. Compromise to the internal nasal valve can compromise breathing, whether it is from damage to the dilating muscles or from direct damage and scarring in the valve itself. Scarring in the valve from over-aggressive resection of overlying lateral cartilages is the most common culprit. Patients with classic high narrow vault to begin with are more at risk for nasal vault problems following rhinoplasty and must be noted in the consultation. A patient with a high narrow vault requiring significant hump reduction may require spreader grafts placed between the resected dorsal septum and upper lateral cartilages to prevent valve compromise after surgery. Caution must always be used when resecting any portion of upper lateral cartilages to avoid breathing problems or cosmetic problems from middle vault collapse.
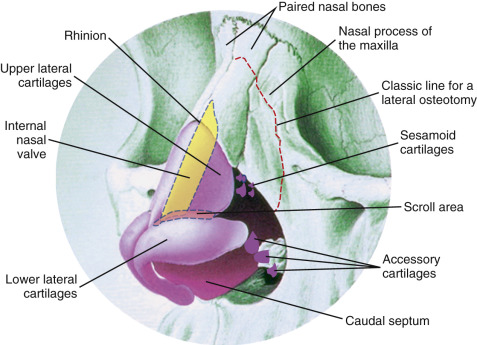
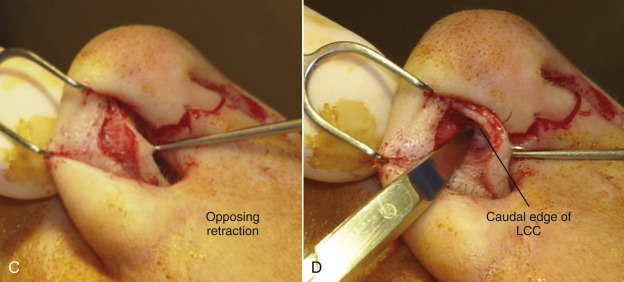
The anatomy of the lowest portion of the upper lateral cartilage can be quite variable where the upper lateral cartilages connect to the lower lateral cartilages. This area is considered the scroll region. The upper lateral cartilage and lower lateral cartilage connection has been described by different authors, but one of the most common descriptions shows the cartilages connect by interlocked shape 52% of the time, overlapping 20% of the time, “end-to-end” 17% of the time, and opposed 11% of the time ( Fig. 6.14 ). The scroll area provides significant support to the nasal pyramid particularly the tip.
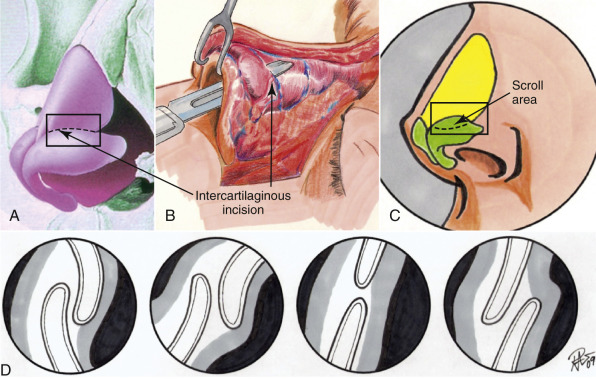
The lower lateral cartilages form the majority of the nasal tip and make up the majority of patient complaints with regard to the shape of the nose. The nasal bones and upper lateral cartilages create the classic nasal dorsal hump, whereas, the lower lateral cartilages are what create the common complaint of a bulbous or boxy nose deformity. The structures of the lower lateral cartilages involve a medial, intermediate, and lateral crus. They not only create the nasal tip appearance but help in function. The thickness and elasticity of the lower lateral cartilages play a major role in the external nasal valve, as well as overall tip support. The lower cartilages, particularly the intermediate crus, help make up the dome ( Fig. 6.15 ).
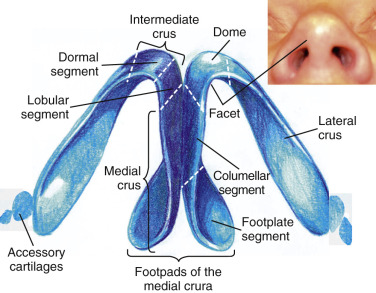
The angulation of the lower lateral cartilages themselves can vary tremendously from patient to patient. The axis of the lateral crus can be very oblique or positioned more medially. In addition to varying positions of the axis, the cartilage can actually be concave in shape versus the more common convex shape. Often the lateral crus will also have a somewhat irregular distorted appearance simply as a congenital anomaly. The relationship of the caudal edge of the lateral crus adjacent to the anterior septal angle makes up the very important supratip region ( Fig. 6.16 ). The various morphologies of the medial, intermediate, and lateral crural cartilages can dramatically change the appearance of a nasal tip, which explains why the vast majority of grafts placed in the nose are used in this region.
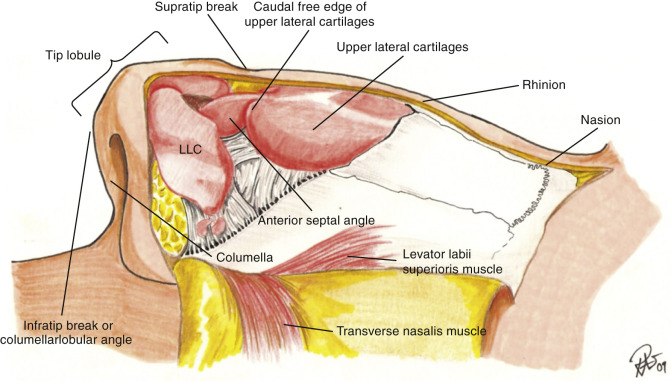
The nasal septum, which connects to all of the previously mentioned structures (nasal bones, upper lateral cartilage, and lower lateral cartilage) provides a very significant amount of support to the nose throughout its entire length and plays a big part in not only a nasal dorsal hump but actual tip projection and support as well. While the medial crural cartilages make up a portion of the columella, the caudal septum itself is classically a more sturdy type of cartilage compared to the medial crural cartilages and must be addressed for problems such as hanging columella and almost any other type of major tip projection issue. The nasal septum is made up of bone and cartilage, the perpendicular plate of the ethmoid, vomer, and the quadrangular cartilage ( Fig. 6.17 ).
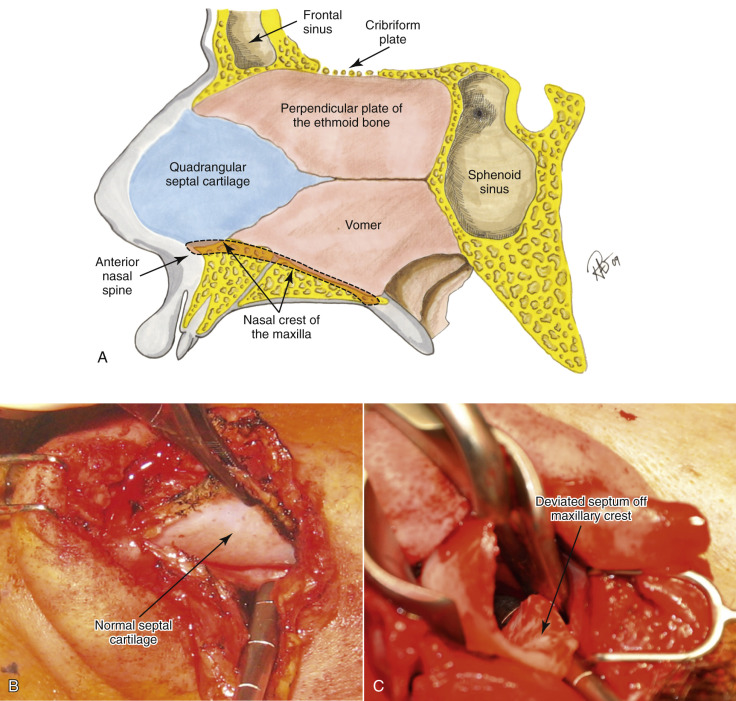
It also has a rich blood supply as previously described and can have various shapes when it connects to the maxillary crest along with multiple deformities and deflection types. An asymmetric nose is basically impossible to treat without addressing the septum, which inevitably plays a major role in a crooked shape or asymmetries. Also, the nasal septum is one of the best sources for cartilage or bone for grafting the tip or dorsum in reconstructing defects. The classic description of cartilaginous sparing during septal resection recommends leaving a 1-cm caudal and dorsal strip to provide adequate cartilage to prevent tip ptosis or a saddle nose deformity. While the 1 cm rule is certainly a good basic guideline, multiple other factors play a role in the amount of septum to leave behind. Thickness of residual bones and upper and lower cartilages as well as additional grafts all affect the strength of tip projection. The key is to realize that the septum has a major function in aesthetics of rhinoplasty surgery, particularly with support of the nose, and is invaluable as a source for tissue grafting. The inferior turbinates are often a source for nasal obstruction in addition to septal deviation and must be evaluated before and during rhinoplasty. Enlarged inferior turbinates can be treated in a number of ways, including partial anterior resection or out-fracturing. Over-resection has been known to create chronic problems such as nasal dryness.
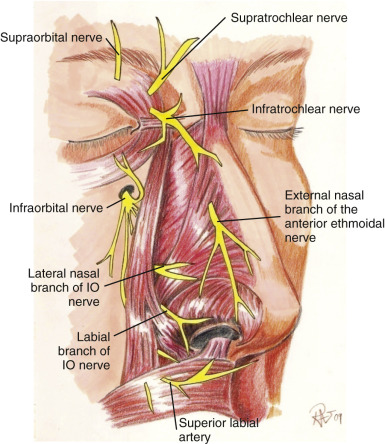
Finally, the nerve supply to the nose comes from sympathetic sensory divisions of the ophthalmic and maxillary branches of the trigeminal nerve (cranial nerve V) ( Fig. 6.18 ). Branches of the supratrochlear and infratrochlear nerves supply the upper half of the nose, while the infraorbital nerve and external nasal branch of interior ethmoidal nerve supply most of the lower half of the nose.
Examination and Consultation
As with any general clinical exam, this is the chance to get to know the patient and find out their chief concerns. As always, the first question should be what bothers them most of all, i.e., what is their chief complaint. Having the patient look in the mirror while they are describing their chief complaint can be very helpful and if the patient does not mention it specifically, they must be asked if they have any breathing problems currently or in the past or if they have had any history of trauma. Despite the fact that the patient may not mention past surgery on an evaluation form, verbally asking again if they have had any previous nasal surgeries is extremely important. Also, a history of any seasonal allergies or periodic episodes of nosebleeds is important to note. Once all of the patient’s complaints have been recorded on an appropriate film or diagram, a detailed exam is performed in a systematic method, assessing skin quality, as well as general shape and support of the nose along with any external and internal nasal deformities or lesions.
During the entire consultation, an assessment of the patient’s mental status must be evaluated to be sure that there is no evidence of possible BDD or any other worries that may create problems in the postoperative period. The young male rhinoplasty patient is often one of the more challenging patients to achieve a result that they will be completely happy with on a long-term basis. Classic signs of potential problems are patients who bring in magazines of movie stars with a particular shape of nose, while some may still be realistic, a more in-depth evaluation of this patient must be undertaken. Ideally, you hope to only operate on a patient once because secondary surgeries are always more challenging and difficult. In addition to the routine workup for medications and history of surgery, it is important to rule out any history of chronic use of nasal spray such as Afrin ® or a possible history of cocaine use, especially if large unexplained septal perforations are noted on the exam.
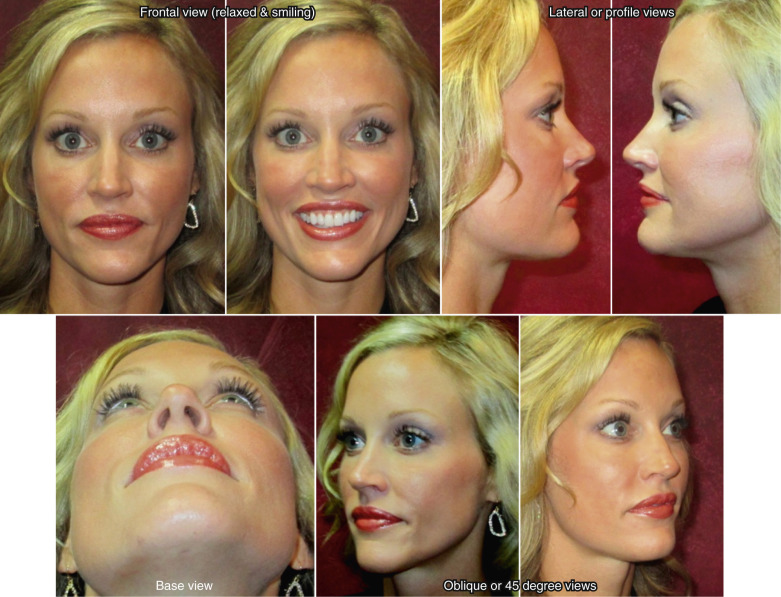
Taking photographs is an important part of record-keeping that can be invaluable for treatment planning. It is important to take quality photographs using six standard views, which are frontal (full face), two lateral views, and two 45-degree (oblique) views, along with a basilar view ( Fig. 6.19 ). Other photographs may occasionally be necessary such as relaxed frontal as well as high smiling frontal and lateral views, to evaluate nasal tip displacement from an overactive depressor muscle. Standardization of the photographs is critical for follow-up and for evaluating your own results over time. Since it may take a year or more to see the final number of changes that can occur after rhinoplasty, photographs are invaluable.
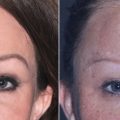
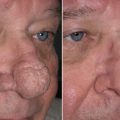
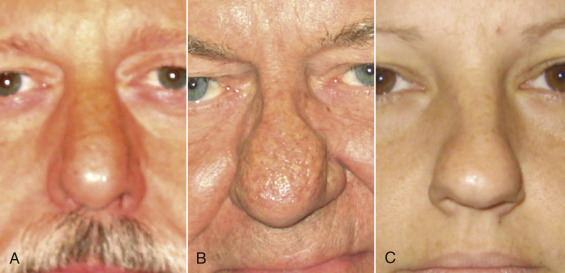
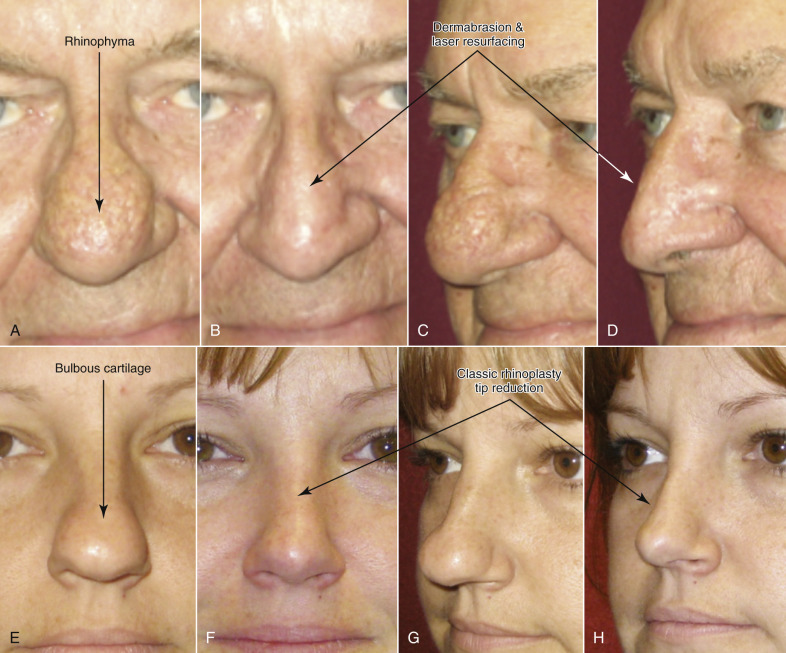
Initial assessment of the skin thickness should be noted throughout the upper and lower nose along with the amount of sebaceous type nasal skin. Also, the elasticity is noted by a simple pinch test and stretching of the skin over the nose along with palpation, particularly in the nasal tip, to assess the amount of support over the nasal tip itself along with a good sense of possible irregularities that cannot be simply visualized. Thin-skinned patients have the potential for a very nicely sculpted nose but are also at risk of showing every flaw. On the other hand, patients with bulbous tips but very thick skin may not get the result they hoped for because the thick skin limits the amount of shrinkage that can safely be achieved by standard rhinoplasty. Rhinophyma, which is an overgrowth of sebaceous glands secondary to rosacea, can be treated by addressing the outer skin alone ( Fig. 6.20 ). African-Americans as well as certain other ethnicities tend to have thicker nasal skin requiring special techniques to give the patient the results they hope to achieve. Limitations must be discussed.
Evaluation of proportion of the nose particularly related to the face is critical. Using classic methods that were developed by Leonardo Di Vinci, and others, are commonly performed to gain an appreciation for proportion of the nose, as it relates to its own subunits and the face itself. For example, the width of the alar base compared with the intercanthal distance is an easy assessment and can quickly give an idea of proportion, along with simply measuring the distance and recording the base of the nose. The length of the nose is also assessed from the radix to the nasal tip and must be based on proportion to the rest of the face. In addition to the nasal length, the angulation from the lateral view is extremely critical, particularly in the nasal frontal angle and the nasolabial angle. The ideal nasal frontal angle is between 115–130 degrees and is slightly more obtuse in females (see Fig. 6.9 ).
It can appear very different when a nasal dorsal hump is present and also from a significant amount of bossing in the glabellar and frontal region or even a deepened or shallow radix area. The depth of the radix can also be assessed by evaluating the distance from the pupil to the nasion from the lateral view and should be in the range of 4–9 mm on average. Reporting the amount of nasal dorsal hump or possible saddle nose deformity is important, along with whether the patient feels as though they have a large hump, a small hump, or none at all. The patient should also be asked whether they prefer a straight nasal dorsum or like the appearance of a more “scooped” look to assess what the patient would ultimately be happy with. Performing computer simulation can be helpful in particular patients that may not have a realistic expectation of what can be performed. Surgeons vary in whether they like this idea, since the result may not ultimately end up like the prediction. If using computer simulation, it is critical to inform the patient that this is only a simulation and the results may vary and that it is simply a tool to try and help with the surgical planning and to assess if the patient is realistic in what can be achieved.
Nasal Tip Clinical Evaluation
Evaluation of the nasal tip is essential to rhinoplasty surgery. Beyond the skin texture and thickness, the general shape of the nasal tip should be evaluated where it is bulbous, pinched, twisted, asymmetric, boxy, overly projected, or under-projected. The general definition related to tip defining should be assessed in whether or not there is a good supratip break, infratip break, or if the nose is amorphous in shape with limited or no tip-defining points or visible architecture of the lower cartilages. Following general shape, noting the nasolabial angles as well as the amount of supratip break or whether there is a Polly Beak deformity (reverse of supratip break) created from prominence of the anterior septal angle is vital to document.
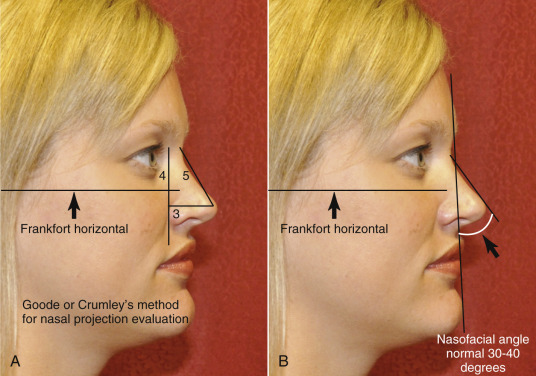
The tip projection and support is assessed based on palpability and visualization. Assessment of the nasal tip projection is difficult because occasionally, the amount of projection can appear as though there is more there than in actuality, such as in a case with a ptotic tip with a nasal dorsal hump. Often, once the other portions of the nose are addressed, the amount of projection changes. The Goode method of assessing projection is one of many, where RT is the distance between radix and the pronasale ( Fig. 6.21 ). The ideal tip projection is 0.55–0.60 of RT. It can also be measured from the nasion to nasal tip (0.55–0.60 of N–NT). Another method is Crumley’s method, which is based on measurements of a nasal triangle that proportionately equals 3–4–5 based on lines perpendicular and parallel to Frankfort horizontal (3 AP–NT (alar point to nasal tip), 4 N line to AP, 5 N–NT). In other methods, the amount of nasal projection is generally related to the dorsum or the anterior face.
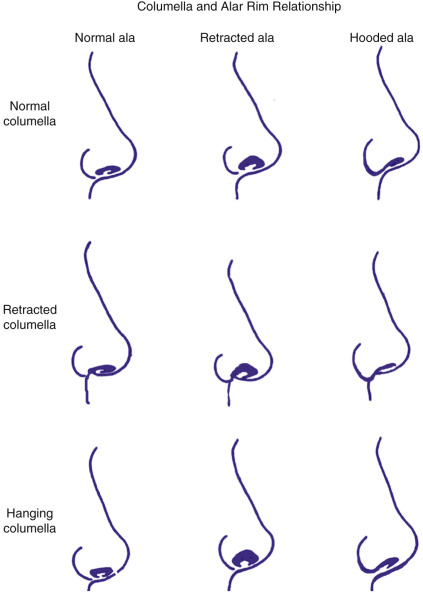
The columella must also be assessed and practically has 2–4 mm show from a lateral view. Not only should there be 2–4 mm of alar show from a lateral view, but in relation to the columella. The ala must be assessed along with the position of the anterior nasal spine and the amount of skin in the base of the columella that can be visualized directly at the nasolabial angle itself. A retracted columella can be very unaesthetic and may be due to inadequate tissue support over the anterior nasal spine but also from simply an enlarged ala that gives the illusion of a retracted columella. The relation of the columella to the alar rim ( Fig. 6.22 ) can be a mix of situations as described by Toriumi and Becker (see Further Reading ). The nasolabial angle is a very important measurement to note and is classically just over 90 degrees in men and 95–110 degrees in women. The nasolabial angle can be affected by not only the amount of tip rotation and amount of caudal septum, but also by the amount of anterior nasal spine projection or even the effects of the entire maxilla and upper incisor teeth. Over-zealous cartilage resection can create a nasal tip that is too short, over-rotated and a nasolabial angle that is too obtuse.
In assessing the overall projection of the nose and proceeding downward to the anterior nasal spine, it is important to evaluate the face as a whole, since problems requiring orthognathic surgery such as maxillary deficiency along with mandibular problems can indirectly affect the shape and appearance of the nose. The classic situation where a patient has a nasal dorsal hump along with microgenia creates a circumstance where the patient should be informed of the proportional discrepancy in order to fully explain to them what may be creating the unaesthetic appearance that they are concerned with. Often, placement of a chin implant on someone who has microgenia with a nasal dorsal hump will clinically make the nose more appealing and even appear smaller because of a more proportionate face overall. Patients requiring orthognathic surgery who have maxillary hypoplasia along with malar hypoplasia may have other problems that contribute to the aesthetics of the nose; therefore, achieving the patient’s overall desire may require more than a simple rhinoplasty. Simultaneous orthognathic surgery and rhinoplasty can be performed but one must understand that major tip changes may occur when the entire maxilla and its anterior nasal spine in moved. A strut is placed for tip refinement and support following resection of a large amount of surrounding cartilage. To prevent deflection from maxillary impaction, the anterior nasal spine is reduced as well. Easy access for septal cartilage harvesting is one advantage of a simultaneous LeFort osteotomy and rhinoplasty ( Fig. 6.23 ).
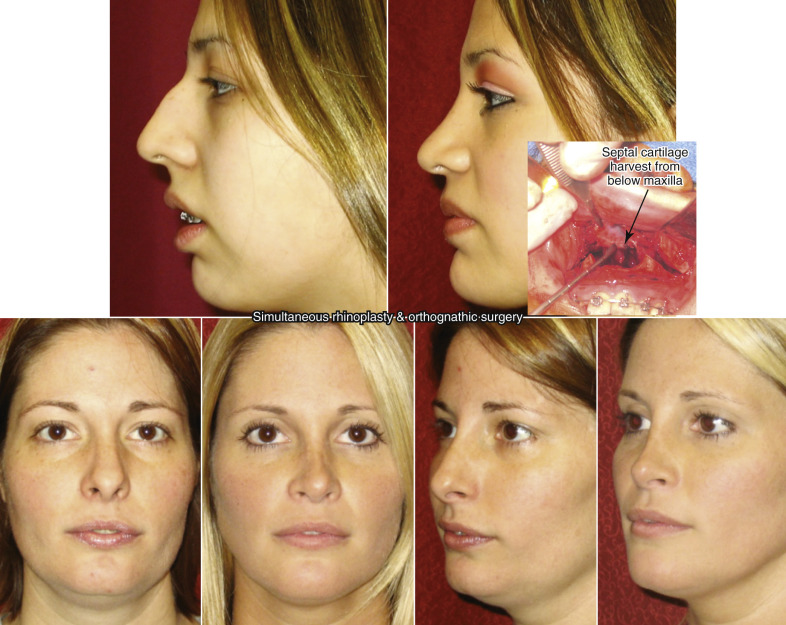
In addition, the nasal base must be controlled with intraoral alar base cinch sutures, since releasing the periosteum at the pyriform rim allows the nasal base width to widen. As with any aesthetic surgery of the face, proportion is key in attaining a harmonious and natural appearance, keeping in mind that good function is absolutely critical. Cleft palate patients are similar to orthognathic patients, in that they often have major bony defects around their nasal defect that must also be corrected to fully improve their rhinoplasty results. An example is augmentation of their deficient pyriform rim by cleft to correct alar asymmetries projection ( Fig. 6.24 ).
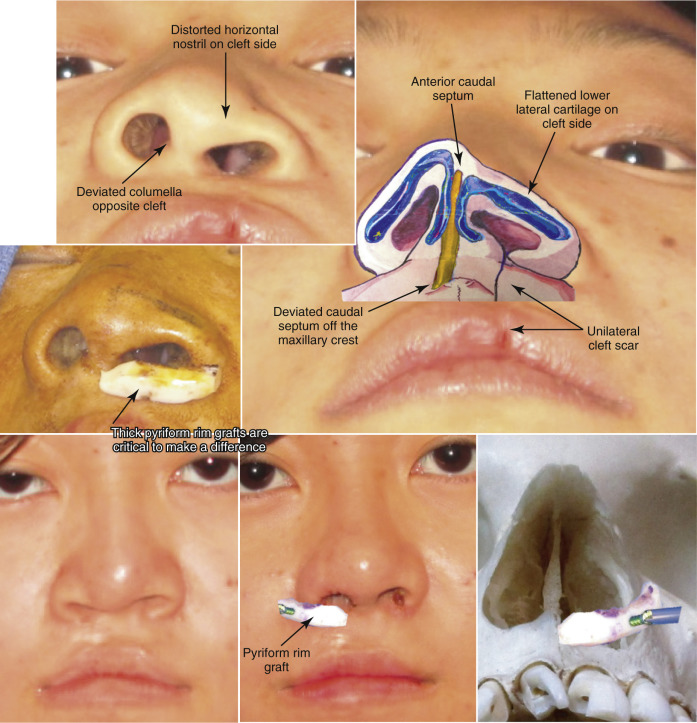
Function of the nose can be assessed by several methods, including simply having the patient take deep breaths in, while holding the nose closed on each side. Other tests involve cotton-tip applicators placed just inside the nose or a caudal test with a finger pulling on the skin on the outside of the nose to assess internal valve problems. Noting valve problems beforehand, both internal and external, can help prevent an unhappy patient postoperatively. It is much easier to prevent these problems with spreader grafts performed during the primary surgery if indicated, rather than performing reconstructive surgery on an operated nose that has significant scar tissue (see Fig. 6.74 ).
Patients who have already undergone previous nasal surgery may have external nasal valve collapse from over-resection of the lower lateral cartilages. External nasal valve collapse can also be seen in a thin or narrow nose, a very aged nose, or even in patients with some facial paralysis. Internal nasal valve collapse that may have been created by scarring from previous rhinoplasty surgery often requires spreader grafts to correct. The Cottle test, for diagnosis of nasal valve collapse, is performed by using your finger to pull laterally on the cheek and lateral wall of the nose in order to open the nasal valve. Classically, patients breathe much easier when this test is performed (positive Cottle sign). The Breathe Right strips that are regularly used by athletes and have an adhesive that allows for the device to act as a temporary spreader graft, function in the same way. The splints open the internal nasal valve from the skin side and allow at least temporary increase of nasal airflow whether nasal valve collapse exists or not. Actual inspection inside the nose with a nasal speculum can help identify any major perforations that could be caused by pathology or even a history of cocaine use. The speculum exam will also note any major deflections of the septum as well as enlargements or asymmetries of the turbinate. The state of the nasal mucosa, such as inflammation from allergies, should be noted during an intranasal exam.
Treatment Planning
A good treatment plan prior to rhinoplasty surgery is an absolute necessity. It is critical to plan for possible problems requiring additional procedures such as graft harvesting from behind the ear, rib, hip, or other location. Pre-surgical photographs (see Fig. 6.19 ) along with possible radiographs, such as cephalometric radiographs, may be helpful in deciding on a sequence for the surgery as well as a detailed plan. Many surgeons will also use waxed paper overlays to mark out exactly what they are hoping to achieve, which can be invaluable when beginning a rhinoplasty surgical career. A logical treatment order should be planned and followed. Most surgeons will developed their own comfortable treatment outline and follow the general treatment order each time.
External vs Endonasal Technique
The argument for or against an open or closed rhinoplasty will likely exist for at least a few more decades to come, and can be easily argued either way. Certainly, there is no one technique that maintains clear superiority over the other. The advantages of an open or external rhinoplasty are obvious, in that it has superior visualization and, in most surgeons’ hands, the ability to place grafts or reduce cartilage can be performed more precisely. The argument for a closed technique involves the possibility of less disruption of blood supply and lymphatics leading to possibly less postoperative edema. The other obvious advantage is the fact that no external scar would be present. Also, some feel that it may be faster in their own hands and is less disruptive to some of the attachments that may allow for better support of the nose. While I personally use both techniques, depending on the particular situation, the external open rhinoplasty is certainly an easier approach and allows for teaching purposes. The main benefit for open rhinoplasty is the ability see everything without distortion for more precision placing of tissue grafts and for tissue resection. Fortunately, the external transcolumellar scar, if placed well and meticulously closed, has rarely ever an aesthetic complaint and in the vast majority of cases, it is nearly invisible after prolonged healing ( Fig. 6.25 ). It is critical to understand nasal base proportions and where to ideally place the external incision, just above the medial footpads to allow for the best healing.
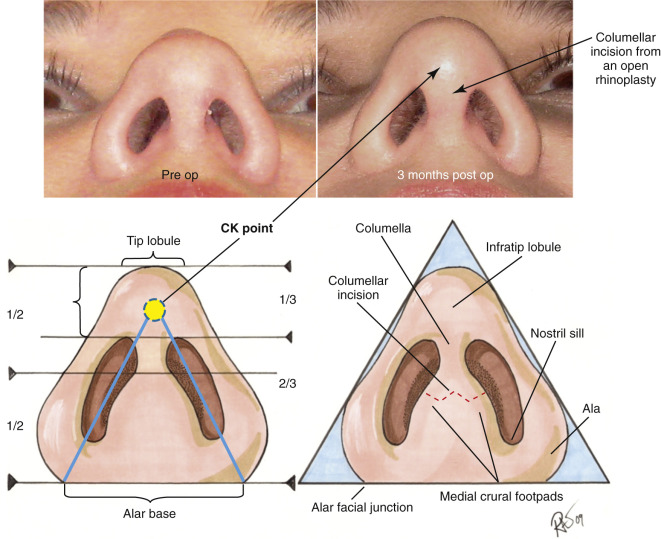
The argument and debate over closed versus open rhinoplasty will go on possibly indefinitely. As with any surgical procedure where multiple techniques exist, the best technique is actually the one that works best for you. The typical patient will simply be happy if their surgery goes smoothly and the results are all that they had hoped to achieve, regardless of the incision type chosen.
General Anesthesia or IV Sedation
Another debate with regard to rhinoplasty surgery is the type of sedation or anesthetic used during surgery. Local anesthesia, without a doubt, is required for vasoconstriction, but the type of sedation varies among providers. In my own practice, all of our rhinoplasty surgeries are performed under general anesthesia for complete control of the airway. Rhinoplasty surgery is a technique that may easily lead to significant blood in the nasopharynx and oropharynx. Major problems with airway management are increased with sedation techniques, where the airway is not protected. Also, simple problems such as coughing or movement during surgery can create a nuisance during a poorly controlled intravenous (IV) sedation. Many surgeons today still perform the procedure under IV sedation and that can work very well but must be carefully managed to avoid airway compromise.
Incision Options
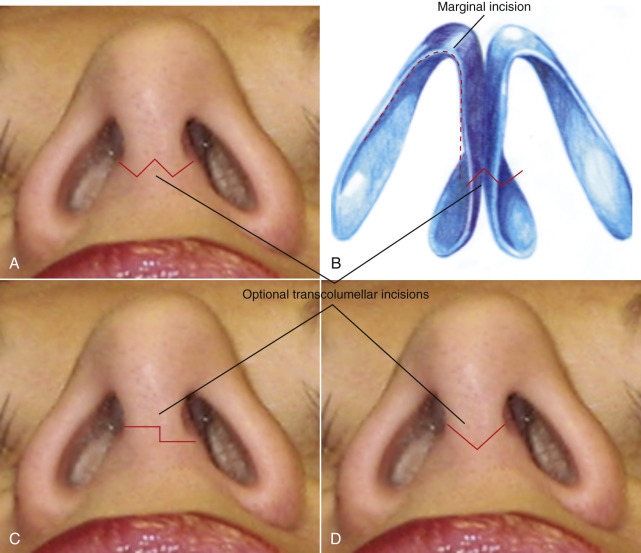
Multiple incision options exist for various rhinoplasty techniques; however, the external rhinoplasty has the most standard incision, which involves a transcolumellar incision that is blended into a marginal incision. The marginal incision is one that can be used for both an open or closed technique. A marginal incision is an intranasal incision that essentially hugs the caudal margin of the lower lateral cartilages, while the caudal margin of the lateral crural cartilage typically follows just along the entire extent of the lower lateral crus ( Fig. 6.26 ). As the incision approaches the facet or internal crus, it often can be made 1–2 mm more cephalic than the actual margin of the cartilage, in order to help prevent alar retraction. Also, the marginal incision along the medial crus can be made further cephalically than the actual margin, if significant treatment of the medial crus or placement of a strut is indicated. This allows for more exposure of the medial crural cartilages than would be attained if the incision was truly at the marginal edge.
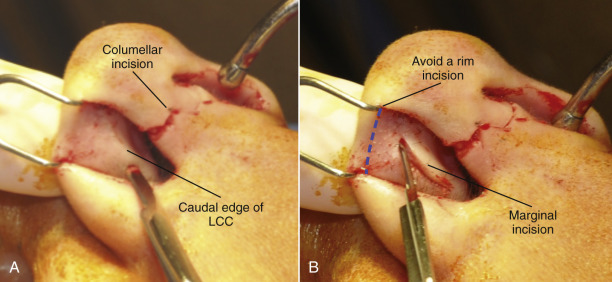
For the transcolumellar portion of the external rhinoplasty, the incision should be made with a No.11-blade scalpel to create precise edges and distinct corners in which reapproximation can be made easily and predictably. The incision should preferably be placed in a location that would be at least visible postoperatively, typically approximately one-third of the distance from the alar base extending up toward the nasal tip. This also typically corresponds with the top of the nasal footpads of the medial crural cartilages. The actual shape of the incision is variable. A straight line incision should be avoided because this would leave the most notable scar and possibly some notching laterally. Various shapes and techniques have been used to perform this transcolumellar incision, with the most common being either a stair-step technique vs a “W” or inverted-”V” type of incision ( Fig. 6.27 ). The key to having an incision that looks nearly invisible postoperatively, is meticulous surgical technique where tissues are not crushed or compromised by inappropriate retraction. The tissue in the columellar area can be very thin and rough manipulation of this can create poor healing postoperatively. Care must be taken in elevating this flap to prevent crushing the tissue or excessive stretch with retractors. Finally, closure of the columellar incision must also be meticulous using interrupted sutures in a precise fashion to ultimately achieve a very well-hidden scar during open rhinoplasty.