Introduction
Oncoplasty is a popular technique for managing partial mastectomy defects that continues to gain momentum among plastic surgeons and oncologic breast surgeons alike. It is now widely accepted as a superior approach for reconstructing partial mastectomy defects, especially in the setting of postpartial mastectomy radiation. The advantages are that oncoplasty expands the candidacy for breast conservation therapy to patients with larger tumors who would otherwise require a mastectomy. Oncoplasty reduces the chances of having positive margins by increasing surgical exposure and allowing for a larger more comprehensive resection. The reconstructive component of oncoplasty significantly improves the cosmetic outcomes compared with lumpectomy or partial mastectomy alone. Larger defects can be reconstructed with local breast tissue to obliterate any dead space created by the partial mastectomy. This creates a stable breast mound that can better tolerate external beam radiation.
By expanding the role of breast conservation therapy, oncoplasty provides patients with a less invasive option. This option eliminates the need for an overnight stay in the hospital and decreases both the operative time as well as the time for recovery. There is no need for either an external breast prosthesis or an internal breast implant that might be required for a mastectomy reconstruction. Oncoplasty also often allows patients to maintain nipple sensation following their reconstruction. These characteristics all contribute to the popularity that oncoplasty has gained as a successful reconstructive option.
There are a variety of methods by which oncoplastic breast reconstruction can be performed. These include volume replacement techniques as well as volume displacement techniques. Volume replacement methods include the use of remote flaps such as the latissimus dorsi or the thoracodorsal artery perforator flaps and are usually performed in women with smaller breast volumes. Volume displacement methods include the use of adjacent tissue rearrangement, mastopexy, and reduction mammaplasty, and are usually performed in women with moderate to large breast volume.
Reduction mammaplasty is arguably the most common form of oncoplastic reconstruction and can be performed in a variety of ways. Although standard reduction mammaplasty techniques are diverse and can be performed using a variety of pedicles, oncoplastic reduction is different in that the orientation of the pedicle will depend on the location of the partial mastectomy defect. In other words, a superior defect is usually repaired with an inferiorly based pedicle. This chapter will review the fundamental principles and concepts associated with oncoplastic reduction mammaplasty.
Patient Assessment
When a patient is diagnosed with breast cancer, they are usually given two treatment options: either a partial mastectomy in conjunction with external beam radiation or a mastectomy that may or may not require radiation based on lymph node involvement. Most patients who opt for the partial mastectomy or lumpectomy choice are candidates for oncoplasty. Evaluating these patients typically amounts to three key factors:
- 1.
Tumor location and characteristics
- 2.
Need for adjunct therapy
- 3.
Goals and overall health of the patient
Once these three factors have been evaluated and discussed with the patient and the treatment team, then a successful oncoplastic plan can be formulated.
Tumor Location
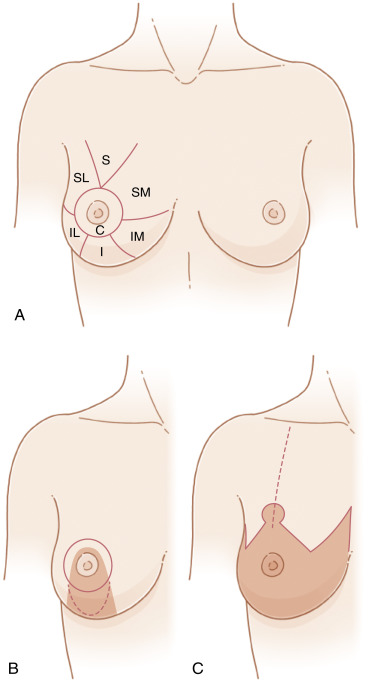
The location of the tumor or the area needing resection is key to designing the best approach to reduction mammaplasty oncoplasty. For strategic purposes the breast can be divided into seven areas as shown in Fig. 8.1 . Preoperative magnetic resonance imaging is extremely useful to determine the extent of the tumor in the breast or if there is any other underlying pathology, like ductal carcinoma in situ (DCIS), in another area of the breast that would also benefit from resection. Once all the areas that require resection have been delineated and pathology has been confirmed or ruled out by core needle biopsy, then the extent of the defect can be categorized to one or more of the seven areas.
Need for Adjuvant Therapy
Once the diagnosis of breast cancer is made and the patient is determined to be a candidate for breast conservation therapy, then there are other tumor characteristics that can affect the timing and extent of the resection and subsequent oncoplastic reconstruction. For example, in the setting of triple negative breast cancer, the tumor is typically highly sensitive to chemotherapeutic agents. In this scenario, it is often helpful to proceed with neoadjuvant chemotherapy first to shrink the tumor down before resection. This strategy allows the treatment team to validate that the chemotherapy is effective against the tumor and also reduces the size of the resection. In smaller breasted patients, this can be helpful to preserve as much breast tissue as possible to maintain a stable breast mound through postpartial mastectomy radiation without compromising oncologic principles.
Another important consideration following oncoplastic reduction mammaplasty is the need for postoperative radiation therapy. The rationale behind this is, although a partial mastectomy is likely to eradicate the bulk of the tumor, microscopic cells may remain, and therefore radiation therapy is recommended. The type of radiation will vary based on the tumor and breast characteristics as well as the recommendations of the radiation oncologist. Options include intraoperative radiation therapy, brachytherapy, partial breast irradiation, or whole breast irradiation. A more detailed explanation is provided in the chapter on oncoplasty and radiation therapy.
Goals of the Patient
Oncoplastic breast reconstruction is no different from any other plastic surgery procedure where it is paramount to understand and account for the goals of the patient. The ideal candidate for a reduction mammaplasty approach to oncoplasty is a patient who would benefit from a reduction mammaplasty alone. In this regard, the reconstructive surgeon can offer the patient a treatment option with benefits that extend beyond breast cancer therapy. It might be that the patient has always wanted to reduce the volume of her breasts and this clinical situation provides an opportunity, albeit unplanned, for this to happen. Patients have the option of performing an ipsilateral oncoplastic reduction alone or choosing to have a contralateral reduction mammaplasty for symmetry. The majority of patients choose the latter to minimize the number of future operations.
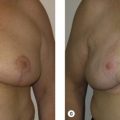
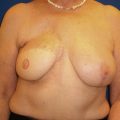
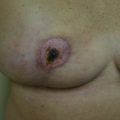
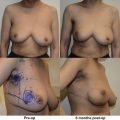
It is important that the patient understands the amount of reduction that will take place with the resection and subsequent radiation so that they can truly make an informed decision. Patients with smaller breasts who prioritize breast volume may not be well served with a reduction-based oncoplastic operation. However, patients with macromastia who hold nipple sensation to be a priority will likely benefit from this approach. Having an in-depth conversation about the expected outcomes and reviewing before and after photographs of the procedure will increase patient understanding and likely increase patient satisfaction. It is therefore important to thoroughly review the risks and benefits of these procedures and discuss the potential complications. Complications include but are not limited to bleeding, infection, and scarring as well as fat necrosis, delayed healing, loss of sensation, and asymmetry.
Operative Technique
Reduction mammaplasty techniques for oncoplastic breast reconstruction are based on volume displacement. These techniques utilize advancement, rotation, or transposition of the remaining breast tissue following a resection to obliterate the dead space created by the resection. Conceptually, it is a strategic breast reduction where the part of the breast that is normally discarded contains the pathological breast tissue needing resection.
Numerous reduction mammaplasty techniques have been described in the plastic surgery literature, and they are all certainly applicable in oncoplasty. For the purposes of this chapter, it is helpful to simplify the approach to the skin pattern and distill down the reduction mammaplasty techniques to three approaches that can be utilized successfully in almost every partial mastectomy. If the requirements for resection and reconstruction cannot be met by these techniques, then the patient is likely not a good candidate for oncoplasty and would be better served with a mastectomy.
One of the most important considerations when performing oncoplastic reduction mammaplasty patterns is an appreciation of the vascularity of the breast. There are several dominant sources that can perfuse the breast in a segmental fashion. The vascularity to the breast is primarily derived from the internal and lateral mammary perforators as well as the thoracoacromial trunk, intercostal perforators, and thoracoepigastric systems. The primary blood supply to the nipple–areolar complex is via the fourth intercostal, aka artery of Wuringer, that courses through the horizontal septum. The third and fourth perforators derived from the internal mammary system will also contribute to the vascularity when a superomedial or medial-based pedicle is used.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree