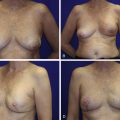
The surgical management of breast cancer has evolved significantly over recent years, commonly trending away from radical procedures, toward those with less extensive resections and decreased patient morbidity. Such types of breast conservation therapy have also been accompanied by simultaneous reconstructive procedures to the breasts, allowing maintenance of ideal aesthetics to preserve the breast mound. These joint oncoplastic procedures have allowed for improved aesthetic outcomes and quality of life for patients, while still ensuring oncologic safety.
A variety of techniques have been described for oncoplastic partial mastectomy reconstruction, including local tissue rearrangement, reconstruction through reduction mammaplasty or mastopexy approaches, and transfer of local/regional flaps. The individual procedure is chosen based on the preoperative breast size and ptosis, percentage of breast parenchyma excised, location of tissue removal in the breast, and potential need for adjuvant chemotherapy or radiation. The rapidly expanding body of literature on outcomes following oncoplastic surgery has shown numerous benefits to this reconstructive approach, including improved aesthetic outcomes, better control of tumor margins, high patient satisfaction, and the ability to extend the option of breast conservation for previously unfit candidates.
With such techniques, potential complications must be considered by the reconstructive surgeon and discussed with both patients and oncologic surgeons. Although some potential risks apply to all oncoplastic procedures, some are unique to individual procedures performed in this setting.
Acute Complications Following Oncoplastic Reconstruction
Overall complication rates for oncoplastic reconstruction range from 15–30%. The complications unique to this type of surgery include skin/flap necrosis, nipple and nipple–areolar complex (NAC) necrosis, seroma, hematoma, infection, wound dehiscence, and fat necrosis. The most common complication in Wise pattern techniques is delayed healing of the T junction. Although wound-healing complications may delay time to adjuvant radiotherapy, this is a rare occurrence in all series reported to date. These procedures do have longer operating times than wide local excision alone, which should be taken into consideration when evaluating patients to ensure they are appropriate candidates for oncoplastic reconstruction.
For individual complications, the most commonly reported rates apply to hematoma/seroma (6% range), wound dehiscence requiring management (4% range), and breast asymmetry requiring revision (5% range). These rates apply to all types of oncoplastic procedures and are within similar ranges to most types of post-mastectomy breast reconstruction options. The undertaking of a bilateral oncoplastic reconstruction has not been shown to result in higher complication rates when compared with unilateral procedures.
Although these quoted complication rates are higher than those for breast conservation without reconstruction, the aesthetic outcomes must always be considered when considering risk. Without oncoplastic reconstruction, any contour deformity will likely require future revisionary surgery. Furthermore, if the patient receives adjuvant radiation, the postoperative contour deformity will become magnified, and the surgical options for correction will be limited. When attempts are made at correcting deformities following breast conservation and radiation rather than upfront with oncoplastic surgery, the reported overall complication rates are in the 40–50% range.
Local Tissue Rearrangement
Local tissue rearrangement is an essential component of many oncoplastic procedures. This may shift the defect to a less conspicuous location by taking advantage of healthy breast parenchyma, subcutaneous fat, and skin elsewhere in the breast, regardless of breast size. These approaches often involve raising of skin/subcutaneous flaps to allow for mobilization of the underlying glandular tissue to fill the glandular defect. Glandular flaps may allow defects in all areas of the breast to be filled, even in the difficult-to-repair upper inner quadrant defect, provided there is sufficient tissue.
The complication rates following local tissue rearrangement are the lowest reported for any method of oncoplastic surgery. The most frequently reported are seroma (12% range) and local infection (7% range). And although these may require further invasive treatment, the majority can be successfully treated with aspiration, drainage, and antibiotic therapy. In the event of a hematoma, management usually requires operative exploration, especially when acute. The use of a surgical drain is not preventative but may be diagnostic and prevent excessive tension on the incision and NAC. Seroma management is usually achieved with observation or aspiration. If the seroma interferes with the delivery of radiation, surgical management or placement of an indwelling catheter by the interventional radiologists may be appropriate. Delayed healing is usually managed by local wound care; however, if extensive, surgical excision may be necessary, especially if the timing of radiotherapy will be impacted. Local infection can be in the form of cellulitis or an abscess. Cellulitis is usually successfully treated with intravenous or oral antibiotic therapy. Abscess management requires incision and drainage.
When compared with partial mastectomy alone, the use of immediate local tissue rearrangement is not an independent predictor of overall complications. In either cohort, the independent predictors of overall post-surgical morbidity are body mass index (BMI), American Society of Anesthesiologists (ASA) class 3 or 4, bleeding disorder, chronic obstructive pulmonary disease, and greater operative times.
Oncoplastic Reduction Mammaplasty
Reduction mammaplasty is an ideal treatment option for breast cancer in women with macromastia. Based on tumor location, a skin pattern and NAC pedicle are designed preoperatively to allow for resection of the tumor within the typical resection pattern for the specific reduction technique and filling of the planned tumor defect with the remaining breast tissue. Once the amount of required tissue resection is determined on the ipsilateral side, the contralateral breast can also be reduced to match. Furthermore, this technique can be applied to tumors in other areas of the breast by shifting tissue and rotating the reduction pattern and pedicle location.
The most commonly employed oncoplastic reduction technique is the inverted T pattern with inferior pedicle reduction mammaplasty. The orientation of the pedicle ultimately depends on the location of the tumor and the area of excision. When the tumor is located in the upper pole of the breast, a wide upper pole tumor excision with glandular resection followed by parenchymal rearrangement will often result in an improved aesthetic outcome for the large or ptotic breast. The incision pattern maintains viability of the skin flaps while providing adequate access and exposure for the partial mastectomy. Whenever possible, it is prudent to maintain perfusion to the NAC on a dermoglandular pedicle.
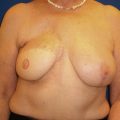
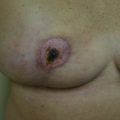
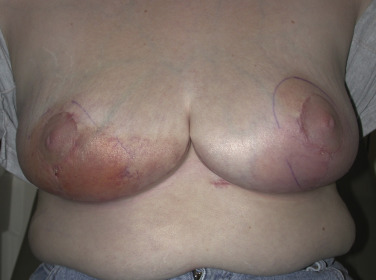
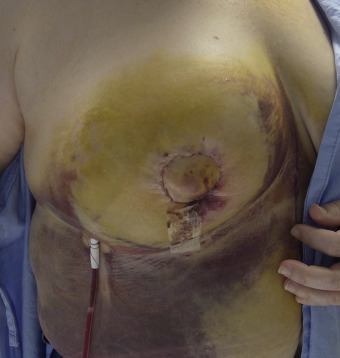
For these techniques, the most commonly reported complications include delayed wound healing (10% range), infection (5% range), and symptomatic fat necrosis (1.4% range). Other less commonly reported complications of these techniques include seroma (1% range), symptomatic fat necrosis (1–2% range), and nipple necrosis (1–2% range). The most common area for delayed healing is the trifurcation point associated with the inverted T pattern ( Fig. 17.1 ). This is an area of relatively poor vascularity and increased tension. Management is usually achieved by local wound care; however, if delayed healing interferes with radiotherapy timing, surgical debridement and secondary closure is considered. Delayed healing of the NAC is also a risk and usually managed with local wound care ( Fig. 17.2 ). Excision is reserved for cases with total necrosis of the NAC ( Fig. 17.3 ).
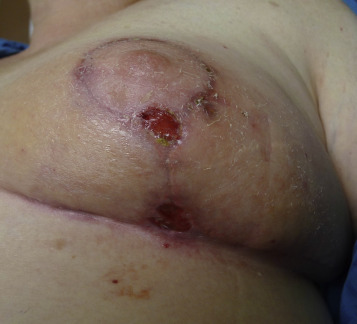
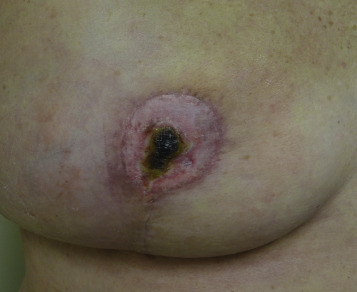
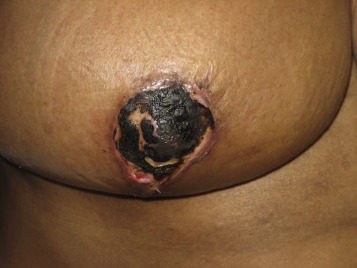
Fat necrosis is another potential complication associated with oncoplastic surgery and more problematic in women with mild to moderate hypertrophy associated with a moderate volume partial mastectomy ( Fig. 17.4 ). Parenchymal rearrangement can be pushed to the limits of vascularity and result in less perfusion to the parenchymal flap, resulting in fat necrosis. When palpable, options include ultrasound and fine needle aspiration for diagnosis and either observation or surgical excision. When extensive, additional rearrangement may not be an option, and a local flap such as a latissimus dorsi may be necessary.

Cellulitis and hematoma following oncoplastic reduction mammaplasty is an uncommon event and usually amenable to conservative management ( Figs. 17.5 and 17.6 ). Most infections are preventable by using copious irrigation techniques and prophylactic intravenous antibiotics. Postoperative antibiotics are considered in some patients dependent upon native risk factors. Hematoma occurrence is rare and usually preventable with good hemostasis following the ablative and reconstructive portions of the operation. Postoperative hematoma will usually require operative evacuation, especially if the bleeding is active and associated with severe swelling. A preoperative coagulation profile and avoidance of aspirin products is recommended.
When assessing aesthetic outcomes and patient satisfaction, oncoplastic reduction techniques have been shown to carry a significant positive effect, thus again outweighing the risk of complications in the majority of patients. Validated patient satisfaction surveys administered to patients following these procedures have shown significant improvements in postoperative patient assessment (relative to preoperative) with emotional health and acceptance of the patient’s own body after surgery. Furthermore, comprehensive patient satisfaction surveys have not illustrated a decrease in postoperative self-assessment of any factors related to the breasts by patients, including physical appearance, emotional well-being, confidence, and sexuality.
There is also been a clear benefit from the standpoint of complication reduction to performing immediate oncoplastic reduction at the time of partial mastectomy. Large series have shown that patients undergoing immediate oncoplastic reduction for reconstruction exhibit an approximately 20% overall complication rate. When the oncoplastic reduction is delayed, oftentimes until after adjuvant radiation treatment has been completed, the complication rate rises to the 60% range ( Table 17.1 ). The largest differences seen in specific complications when comparing immediate versus delayed oncoplastic reduction are seen with infection rates (3% vs 16%), fat necrosis (0.9% vs 8%), and asymmetry of the breasts (8.5% vs 24%). Thus, experience indicates that there is a significant benefit to proceeding with immediate oncoplastic reduction from the standpoint of complication/morbidity reduction.
| Timing and Outcomes for Oncoplastic Reconstruction | |||||
|---|---|---|---|---|---|
| Overall | Immediate | Delayed immediate | Delayed | P -value | |
| Patients | 160 | 117 | 18 | 25 | |
| Complications | 28.1% | 20.5% | 33.3% | 60% | 0.001 |
| Infection | 5% | 3.4% | 0 | 16% | 0.019 |
| Fat necrosis | 1.9% | 0.9% | 0 | 8% | 0.047 |
| Mean satisfaction | 69.8% | 72.8% | 68% | 61.8% | NS |
| Mean aesthetic outcome | 62.5% | 63.9% | 54.6% | 58.8% | NS |
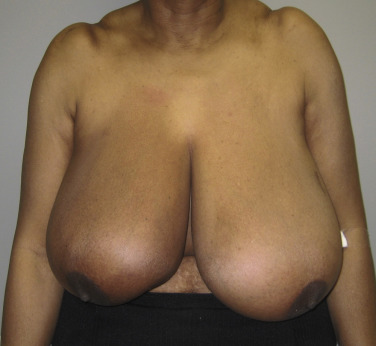
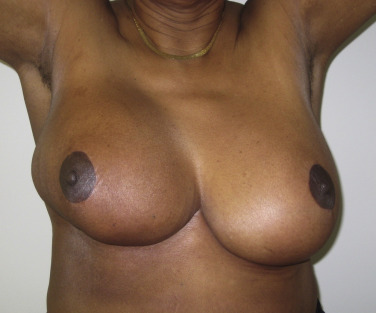
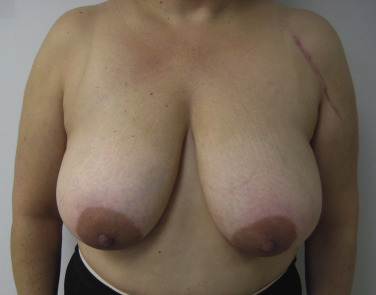
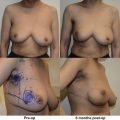
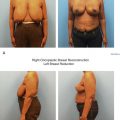
When reduction mammaplasty is requested following breast conservation, there are two schools of thought. The first is that reduction mammaplasty should be avoided because the complication rate is so high, and a mastectomy should thus be considered. The other is that it is acceptable to proceed with a reduction mammaplasty; however, there are several tenants that must be considered. The first is patient selection. If the skin is severely damaged and fibrotic, reduction should be avoided; however, if the skin is relatively soft, then reduction can be considered. Undermining should be kept to a minimum to maintain adequate perfusion. Wedge excision of the parenchyma using a sharp scalpel rather than electrocautery is advised. Free nipple graft should be considered. Although, this will not guarantee a complication-free operation, the complications can be reduced. Figs. 17.7 and 17.8 illustrate a patient with severe mammary hypertrophy following right breast conservation therapy. Following the reduction mammaplasty, distortion of the inferolateral aspect of the breast was noted with arm elevation. Figs. 17.9–17.14 illustrate a patient following oncoplastic reduction mammaplasty complicated by a positive margin on final pathology.