Introduction
Breast Conservation
Increased compliance with breast cancer screening guidelines, as well as advancements in imaging technology, have led to earlier detection of breast cancer. Currently, the majority of breast cancers are diagnosed at earlier clinical stages. This should eliminate the need for mastectomy in a majority of cases as multiple randomized studies with extensive follow-up have established that breast conservation therapy (BCT) confers equivalent local control and survival as mastectomy, including the National Surgical Adjuvant Breast and Bowel Project (NSABP) B-06 study. The oncologic safety of BCT, considered when the tumor size-to-breast size ratio is favorable in selected patients, has been well established. However, there continues to be an increasing trend toward mastectomy. Recent studies show persistently high mastectomy rates, even when women are candidates for lumpectomy. Despite the extensive data showing no survival advantage with mastectomy, this has not dissuaded women from choosing mastectomy for both treatment and prophylaxis.
The topic of contralateral prophylactic mastectomy has added to the decision-making process fueling the increase in mastectomy rates in patients with unilateral breast cancer. Hypotheses explaining why women opt for more extensive surgery include fear and perceived risk in the contralateral breast, optimal reconstruction outcomes, increase in genetic testing and determination of risk profile, as well as the use of breast magnetic resonance imaging (MRI) that can detect smaller cancers. There are record numbers of prophylactic mastectomies being performed in the United States. Data show that mastectomy rates have increased in recent years with high rates of risk-reducing surgery for high-risk patients and those already diagnosed with breast cancer. Although there are general guidelines providing indications for both bilateral prophylactic mastectomy and contralateral prophylactic mastectomy, when it should be advised remains controversial. The factors associated with this phenomenon are unclear and likely involve a complex interplay of patient and physician factors. As more women opt for this type of surgical management in the high-risk and cancer management settings, the question arises as to what benchmark should surgeons utilize to advise their patients?
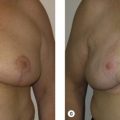
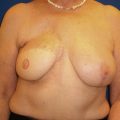
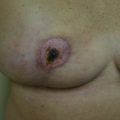
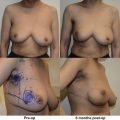
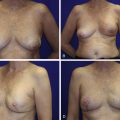
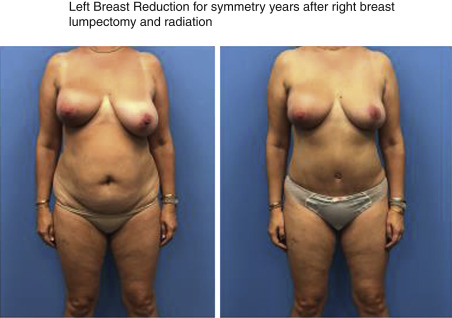
When deliberating over cancer treatment options, one concern patients often voice is the potential asymmetry after breast conservation surgery that can result in the removal of a significant fraction of total breast volume. In addition, breast asymmetry is compounded by the overall size reduction that occurs after whole breast irradiation. Whole breast radiotherapy after BCT can reduce the risk of local recurrence as much as threefold compared with surgery alone and, therefore, is a necessary component of breast conservation. Many patients after an initial satisfactory cosmetic result following breast conservation will develop a progressive asymmetry over time, prompting the need for additional surgery. This is usually a contralateral reduction mammaplasty ( Fig. 21.1 ). Therefore, symmetrization procedures done at the time of lumpectomy can be an important addition to BCT with the benefit of optimizing long-term cosmetic results and perhaps even discouraging unnecessary mastectomies. As a consequence of the advancements in oncoplastic surgery, especially among the west coast surgical oncology pioneers, oncoplastic procedures are becoming more accepted and utilized.
Outcomes after Oncoplastic Surgery
Patient Outcomes
As oncoplastic techniques increase in popularity and utilization, evidence-based analyses of surgical outcomes will be important to support further adoption. Although there is not an overabundance of literature on oncoplastic breast surgical techniques, in recent years multiple studies have been published. In the largest comprehensive literature review to date on oncoplastic breast-conserving surgery (BCS), data were extracted from 55 studies that collectively evaluated 6011 patients. Wise pattern mastopexy was the most commonly utilized oncoplastic technique, performed in 35.4% of patients, followed by the round block (14.8%) and latissimus dorsi volume replacement (9.5%) techniques. This systematic review by Cruz et al is one of the few studies to have short-term and long-term outcomes. Long-term data revealed oncoplastic surgery to have high rates of overall and disease-free survival and low local recurrence thereby confirming the oncologic safety of this procedure in patients with T1–T2 invasive breast cancers.
Of the short-term outcomes, margin status is one of the most important measures of success, and 11 studies reported specific margins for 1455 patients. Among these patients, 143 (9.8%) were classified as having positive margins, of which 113 (7.8%) had tumor on ink. Other short-term data reported included postoperative complications, including liponecrosis, skin necrosis, hematoma, seroma, delayed wound healing, nipple necrosis, and/or infection, which occurred in 14.3% of patients. Specifically, complication rates from oncoplastic BCS in this study, including liponecrosis (3.3%), skin necrosis (0.5%), hematoma (2.5%), seroma (1.0%), delayed wound healing (2.2%), nipple necrosis (0.4%), and/or infection (1.9%), closely reflected those found in a previous study that further demonstrated no statistically significant difference in the incidence of these issues among women undergoing oncoplastic and non-oncoplastic lumpectomies. However, Tenofsky et al found a higher incidence of non-healing wounds in the oncoplastic group compared with the non-oncoplastic group (8.6 vs 1.2%; p = 0.042). It is important to note that this did not prolong time to radiation within the oncoplastic group. Therefore, oncoplastic reconstruction at the time of BCS does not appear to significantly increase the risk of postoperative complications that would delay initiation of adjuvant therapy.
Cosmetic Outcomes and Patient Satisfaction
In the systematic review by Cruz et al, 25 studies also evaluated cosmetic outcomes in 1962 patients. The vast majority reported positive results with oncoplastic surgery achieving excellent, good, fair, or poor outcomes in 55.2%, 31.0%, 9.4%, and 4.4% of patients, respectively. When it comes to the literature, however, there are limited studies investigating patient-reported satisfaction and outcomes after oncoplastic surgery. Furthermore, it has been shown that there is a lack of consistent and validated measures by which these patient outcomes are reported. The majority of the studies are from Europe or South America and do not include the U.S. population. In addition, within these studies, heterogeneity exists in the definition of oncoplastic or breast conservation surgery along with their comparison group (if one is included). Overall, recent studies show positive patient-reported satisfaction with aesthetic results, breast appearance, improvement in functional return to work/activity and overall satisfaction after undergoing oncoplastic surgery compared with standard lumpectomy/mastectomy.
The majority of this data is collected from questionnaires in the postoperative period to assess patient-reported satisfaction and outcomes. For example, a study in the UK by Chand et al compared therapeutic mammoplasty (oncoplastic breast conservation surgery [OBCS]) to a latissimus dorsi miniflap and gave patients the BreastQ questionnaire to assess satisfaction. Patients who underwent OBCS felt their breasts had a more natural feel, were better in terms of size, less likely to report neck pain, and reported higher overall satisfaction. Interestingly, this was one of the few studies that asked about emotional/sexual well-being and found that there was no difference between groups, suggesting anxiety about a cancer diagnosis and treatment influences emotional well-being more than the type of surgery performed.
Some studies cite specific patient populations that OBCS may have the most benefit in, such as patients with macromastia. Kelsall et al performed a study from the UK comparing OBCS to mastectomy with immediate reconstruction. When unmatched, body image scale, breast appearance, and return to work/function were better in the OBCS group. However, when matched to case controls, women with larger breasts reported better body image scores and self-rated breast appearance, which was not seen in women with smaller breasts. Even when patients required postoperative radiation, patients in the OBCS cohort reported better body image scores compared with those with mastectomy/immediate reconstruction. Somewhat contradictory to this, a study in 2017 by Ojala et al compared aesthetic and functional outcomes 3 years after surgery and found that, overall, patients in the conventional group had better self-reported aesthetic outcomes than the oncoplastic resection group using two types of questionnaires. Of note, they found larger tumors and tumor multifocality were predictors of poor aesthetic outcomes. However, this cohort study was limited by only a small percentage undergoing oncoplastic surgery ( n = 86: 23%) compared with conventional surgery ( n = 293: 77%). Nonetheless, conventional resection may be better for certain patients. Another study in 2015 out of Brazil by Santos et al actually examined aesthetic outcomes of oncoplastic versus lumpectomy patients evaluated by a software system, specialists, and patients. Although the software and specialists reported significantly better aesthetic outcomes in the oncoplastic group, patients did not.
There is currently a large prospective trial occurring in the Netherlands comparing women who undergo BCS to evaluate cosmetic outcome, patient satisfaction, and quality of life based on the lumpectomy technique; however, it has not been completed. This will be one of a limited number of prospective trials investigating the utilization and outcomes of oncoplastic techniques compared with standard lumpectomy. Further, the investigators have a goal to use the data to create a clinical decision model to guide the use of oncoplastic techniques in the future ( Table 21.1 ).