Key Points
The presence of many pericardial disorders may be suggested by the chest radiograph.
- ▪
Pericardial effusion: enlargement of the cardiopericardial silhouette (CPS)
- ▪
Pericardial tamponade
- ▪
Enlargement of the CPS
- ▪
Systemic and pulmonary venous engorgement
- ▪
- ▪
Constrictive pericarditis
- ▪
May or may not have pericardial calcification
- ▪
Atrial, especially left atrial enlargement
- ▪
Systemic and pulmonary venous engorgement
- ▪
- ▪
Pericardial cysts: cardiodiaphragmatic angle (left greater than right) or midline mediastinal rounded mass
- ▪
Pneumopericardium: air stripe and parietal pericardial stripe
Acquired Pericardial Disease
Pericardial Effusion
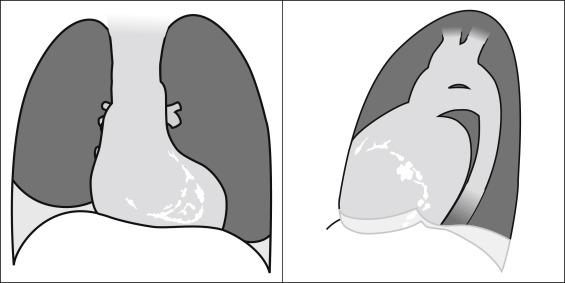
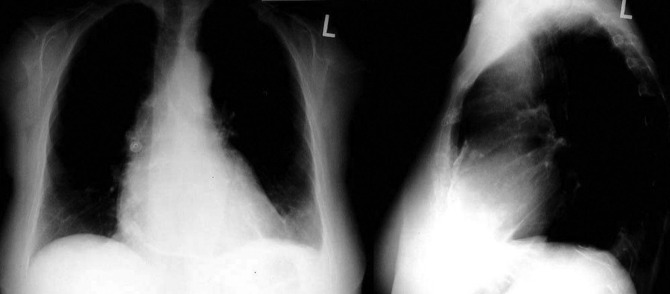
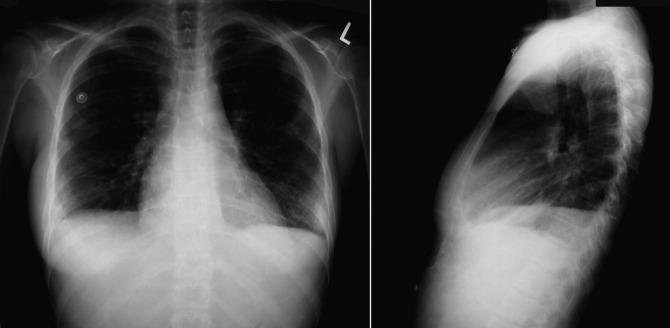
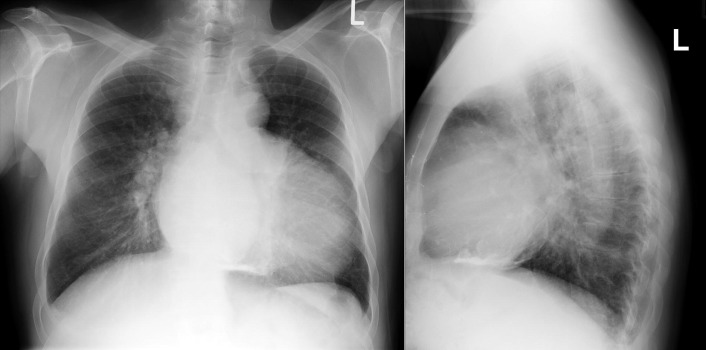
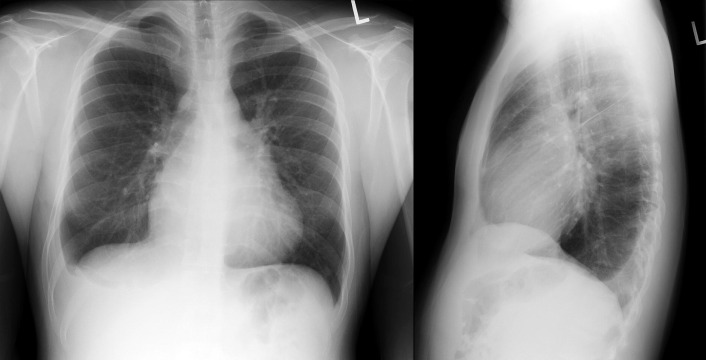
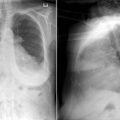
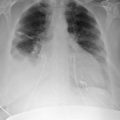
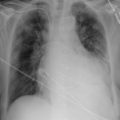
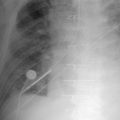
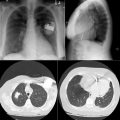
A pericardial effusion ( Figs. 16-1 to 16-15 ) is often suggested on the frontal chest radiograph by a smoothly distended, “flasklike” CPS. More than 500 mL of fluid must be present before the change in the CPS is fairly obvious. A flasklike appearance may be caused by myocardial disease as well; scrutiny of the hilar vessels may distinguish the two. In the presence of pericardial effusion, the hilar vessels are covered (the pericardium runs up onto them and obscures them). In the presence of myocardial disease, the hilar vessels are unusually prominent as they are distended under higher than usual pressure.
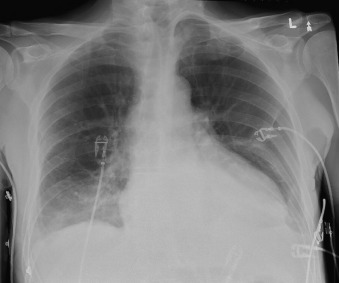
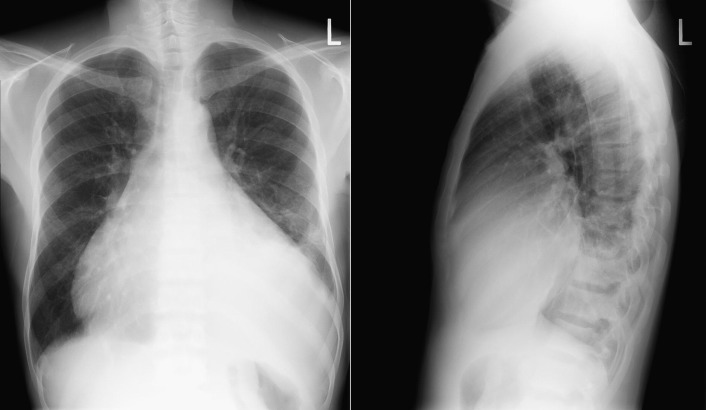
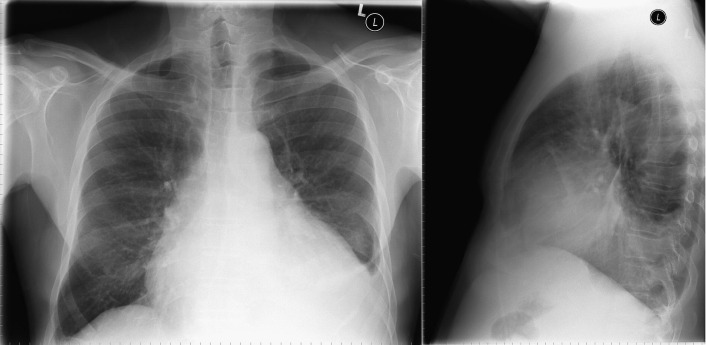
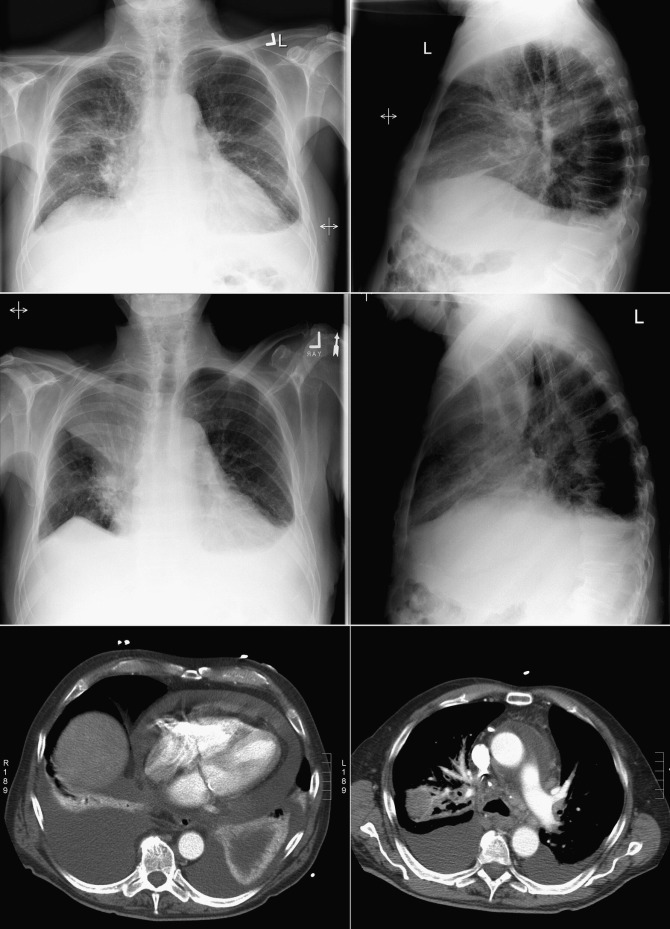
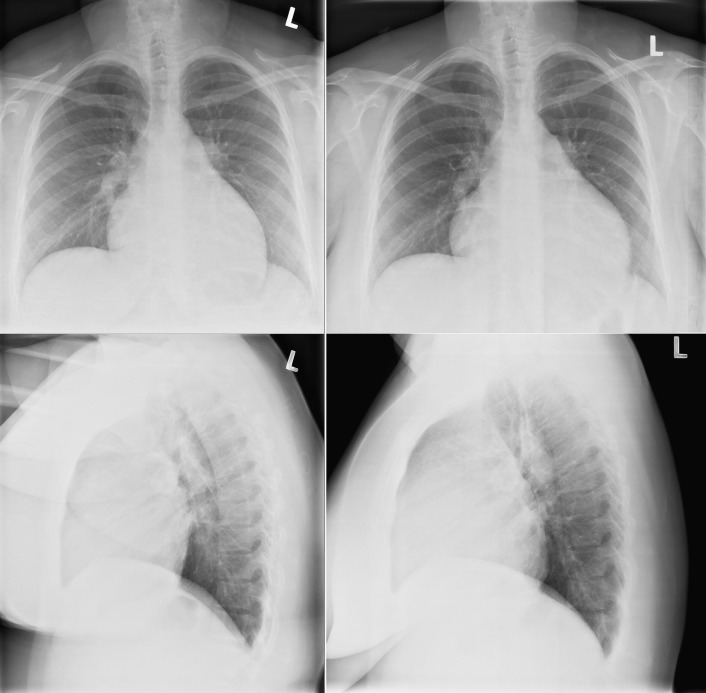
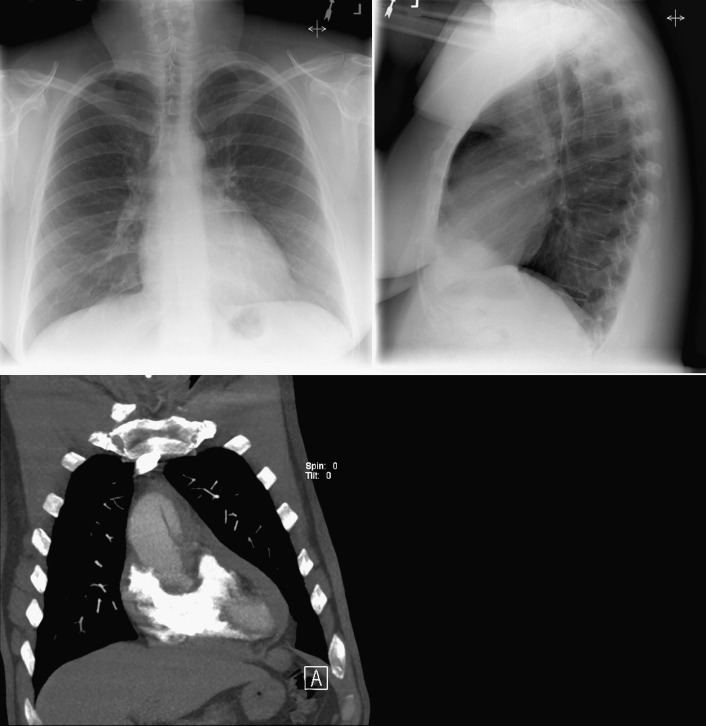
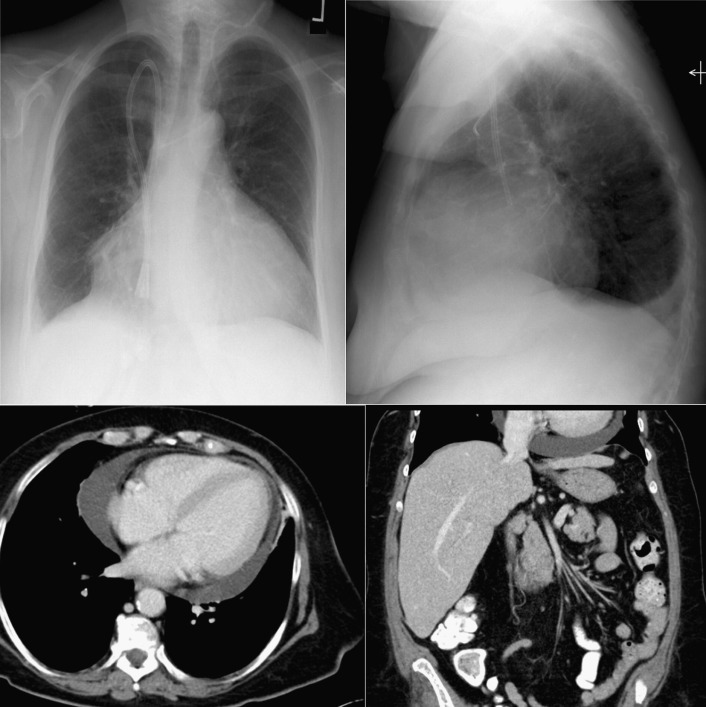
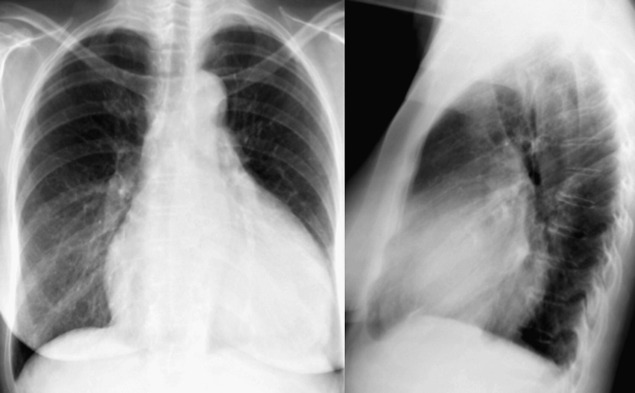
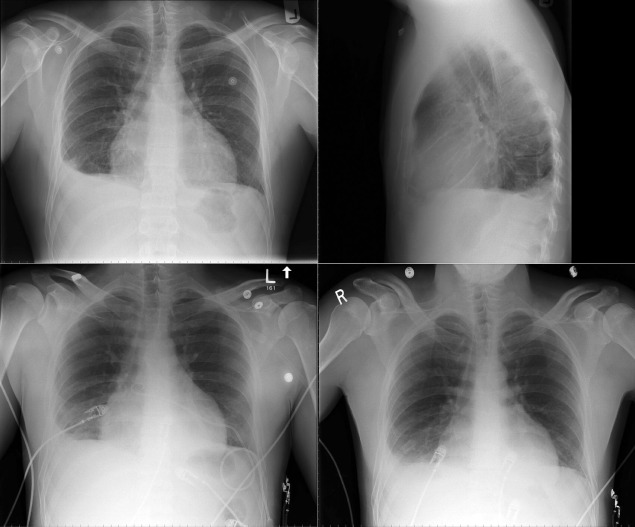
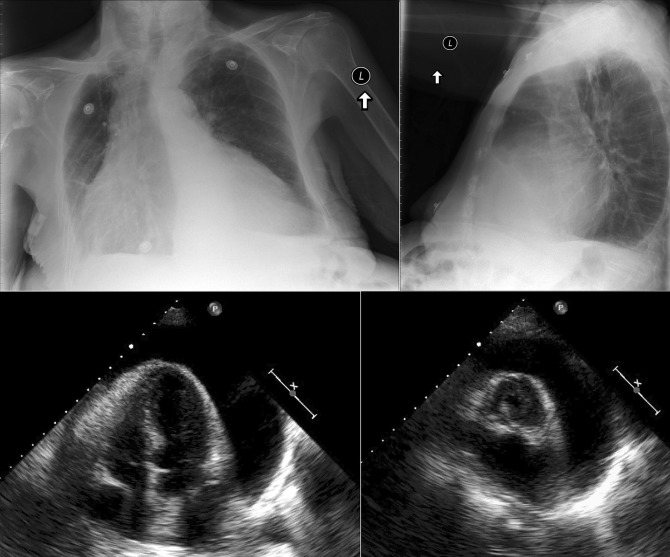
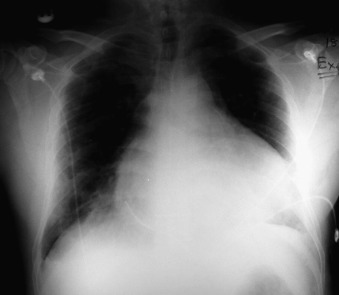
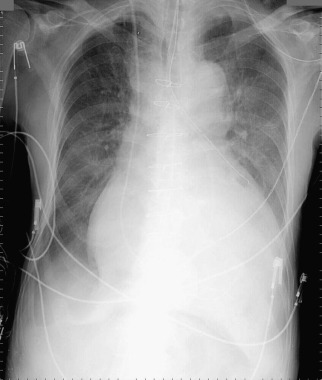
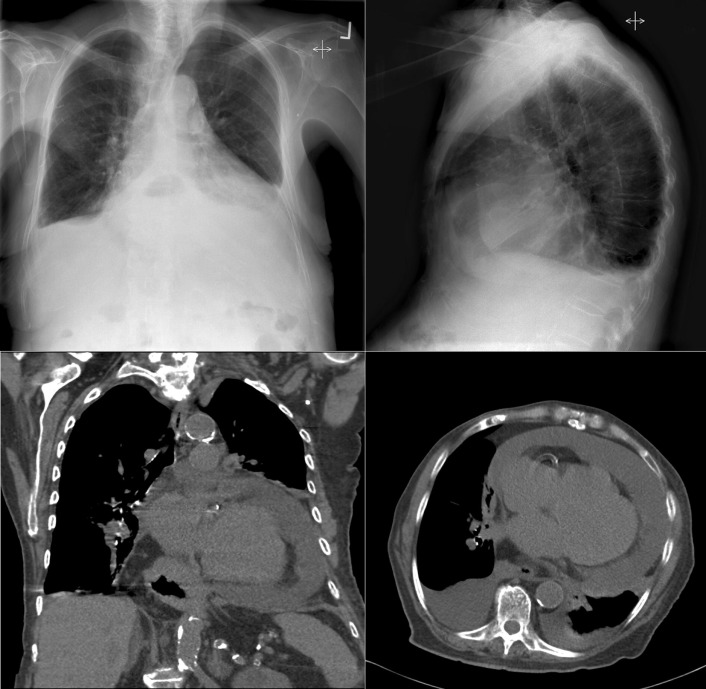
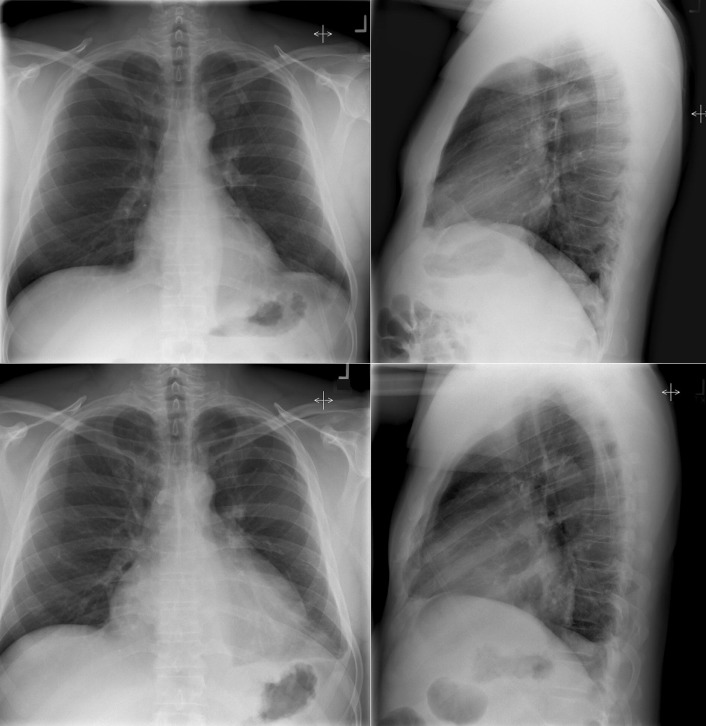
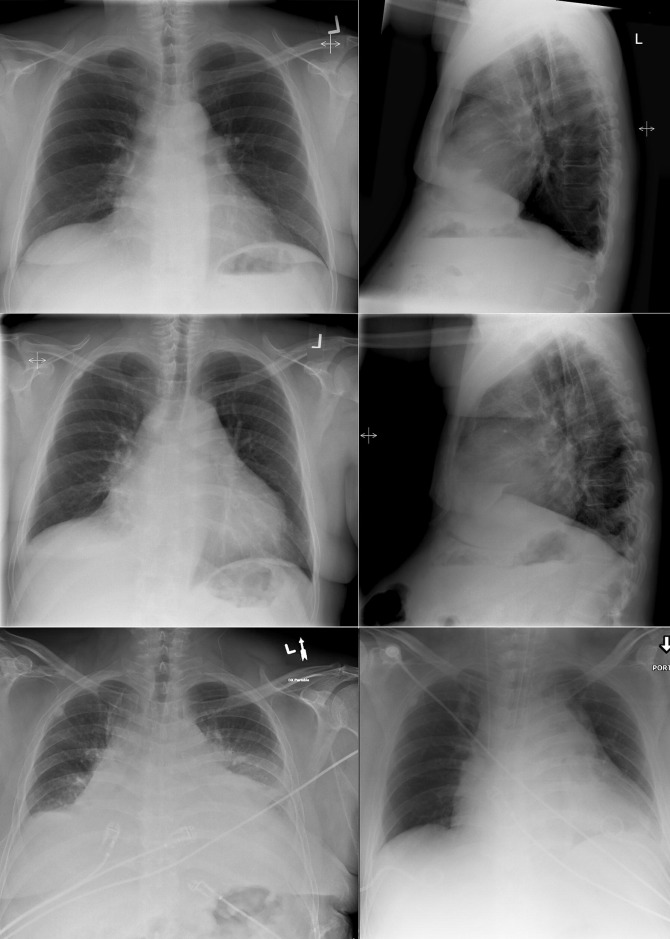
In a minority of patients with pericardial effusion, on the lateral radiograph, a stripe of radiolucent epicardial fat, a “fat line,” may be visible anteriorly, suggesting fluid in the pericardial space. A stripe greater than 2 mm is abnormal. This “pericardial stripe sign” is more easily seen in adults than children (more fat!).
A prominent azygous vein, superior vena cava, or inferior vena cava suggests cardiac tamponade.
Echocardiography is the diagnostic test of choice for the evaluation of pericardial effusions. Pericardial tamponade remains a clinical diagnosis, strengthened by supportive echocardiographic findings.
Constrictive Pericarditis
In constrictive pericarditis ( Graphic 16-1 ; Figs. 16-16 to 16-23 ) , the CPS is usually nonspecifically and mildly enlarged. Occasionally, the heart is normal or small in size. The left atrium is the most frequently enlarged chamber, because its enlargement is less restricted by pericardium. The right atrial contour on the frontal chest radiograph may be flattened. Calcification of the pericardium suggests past tuberculosis, but since tuberculosis has become uncommon at most centers, 90% of cases of constrictive pericarditis are currently noncalcified. Calcification, especially diaphragmatic, is not specific for constrictive physiology; it may be seen in the absence of cardiac compression. The apical surface is less frequently calcified than the interventricular and atrioventricular grooves. The apex seldom calcifies prominently in constrictive pericarditis; this finding suggests a calcified apical aneurysm rather that constrictive pericarditis.