and Frank Hölzle2
(1)
Department of Oral and Maxillofacial Surgery, Klinikum rechts der Isar, Technische Universität Munich, Munich, Germany
(2)
Department of Oral and Maxillofacial Surgery, University Hospital of RWTH Aachen University, Aachen, Germany
Electronic supplementary material
The online version of this chapter (doi:10.1007/978-3-319-53670-5_2) contains supplementary material, which is available to authorized users.
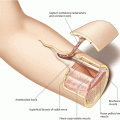
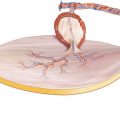
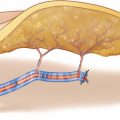
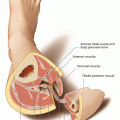
Since the RFF is drained by a deep and a superficial system, there is still a debate as to which system is more reliable for anastomoses. Anatomically, the superficial system of the RFF is largely represented by the cephalic vein, which collects the blood from the dorsal venous arch and courses along the dorsolateral border of the radius toward the antecubital fossa, where it communicates with the median cubital vein, the basilic vein, and also with the deep venous system of the RFF via a perforating vein. The vein then further ascends to the deltopectoral fossa, traveling within the groove between the biceps and brachialis muscles, where it perforates the clavipectoral fascia to drain into the axillary vein. According to an anatomic dissection by Reid and Taylor [430], the cephalic vein was absent in 2 out of their 50 specimens. The average diameter of the cephalic vein is about 5 mm (1–12 mm) [275].
The communicating vessel between the cephalic vein and the deep system was first noted by Soutar et al. in 1983 [511], followed by a number of more detailed anatomical and clinical descriptions. Tahara et al. [523] found this vein to be present in all but one of their 188 patients, and despite the complex procedure to dissect the pedicle up to the brachial vessels, they emphasized to include this vein because it allows to drain both venous systems with only one anastomosis. Whereas a similarly high reliability of this communicating vein was also described by Valentino et al. [566], Thoma et al., who classified the branching pattern of the deep and superficial system into five different groups, could find the communicating vein in only 62% of their cases. Of these cases, the median cubital vein either split into the cephalic or median basilic vein (group 1) or did not bifurcate (group 2). In 18%, both deep veins merged and formed a sizeable common trunk, but did not anastomose with the superficial system, and in the other two groups, both deep veins did not merge, but had a suitable caliber for anastomoses (5%) or were different in size with one vein significantly larger than the other (15%).
According to a review by Medard de Chardon et al. [363], there are supporters of performing anastomoses to either the deep [118, 242, 243, 510, 570] or the superficial veins [246, 339, 400], because they believe those veins represent the dominant drainage system. Other authors consider both systems to have an equal capacity to drain the flap [136, 268, 557], but they prefer the superficial system because the veins have a larger diameter, making anastomoses easier. Other authors state that the deep veins are more adequate to drain the distal part of the skin paddle [243, 370] or believe it to be more reliable than the superficial system in elderly patients [118]. Moreover, the superficial veins were proposed to serve as a backup in case of the need for revision surgery [370].
The question of whether to perform a single or double venous anastomosis was discussed extensively in the literature. Again, a very useful summary was provided by Minoun et al. who could identify authors suggesting only one venous anastomosis, whether it is superficial or deep [154, 268, 510], because they considered a single venous outflow to be sufficient. Moreover, when performing a second anastomosis, this would lead to an increased operating time and reduction of venous blood flow, which could increase the risk for thrombosis. A significant decrease in flow velocity was also confirmed by a study by Hansono et al., who therefore argued against two venous anastomoses. To evaluate the efficacy of the cephalic vein, it was proposed to temporarily clip the deep veins and to anastomose the flap to the superficial system only if there were no signs for venous congestion [429]. On the other hand, many other authors recommend performing two venous anastomoses routinely [61, 198, 247, 306, 543, 566] preferably one from the deep and another from the superficial system [244]. Using the double anastomoses technique, failure rates between 0% and 1% were reported in primary reconstructive procedures [5, 443]. This was confirmed by a systematic review and metaanalysis including almost 7000 free flaps by Riot et al. [439], who found a significantly lower failure rate for double venous anastomosis. This finding was also evident for most of the studies focusing on the RFF [244, 446, 490, 530].
Beyond the relevance of the cephalic vein to drain RFF in free-tissue transfers, it can be left attached to the donor site after extended dissection up to the clavicle, if a long venous pedicle is required in cases of vessel-depleted necks or during salvage maneuvers [188, 275, 634]. With this technique, the cephalic vein is exposed along its course at the arm directly or via endoscopic guidance and together with the flap tunneled subcutaneously over the clavicle into the defect, so that only an arterial anastomosis is necessary, and the dissection of the cephalic vein is possible in less than 30 min [422]. Moreover, the vein is a useful source for vein grafts because of its large caliber, superficial location, and ease of handling [188] (◘ Figs. 2.1 and 2.2).
2.1 Flap Raising
2.1.1 Patient Positioning and Flap Design
Like in the standard flap-raising procedure, the arm is disinfected including the fingers and brought in an abducted position. Blood flow in the cephalic vein is checked by occluding it distally and milking the vein proximally. If there is no refill or if the vein is fibrotic following multiple-catheter insertions, it cannot be used to drain the flap. To allow for approaching both sides of the arm, which might be necessary if the cephalic vein runs far dorsally, the whole forearm and hand must be accessible for flap elevation. When designing the flap, its radial margin must be extended toward the dorsum of the forearm so that the cephalic vein is safely included into the skin paddle. Moreover, like in the standard flap design, the skin must cover the lateral intermuscular septum to include the radial vessels. Normally, the ulnar margin of the flap is outlined along the flexor carpi ulnaris tendon, and distally, a distance to the flexor crease of 2–3 cm is kept. The use of a tourniquet is not necessary for flap elevation. For pedicle dissection, the incision line is marked between the flexor carpi radialis and brachioradialis muscle (◘ Figs. 2.1 and 2.2).
Exposure of Flexor Carpi Ulnaris
The skin is incised along the whole ulnar flap border, the deep fascia is exposed and completely cut, and the flexor carpi ulnaris muscle and tendon are exposed. Care is taken not to overlook a superficial ulnar artery which, if present, mostly runs directly deep to the fascia (◘ Figs. 2.3 and 2.4).
Distal Exposure of Cephalic Vein, Radial Vessels, and Superficial Nerve Branches
The deep fascia is taken by a hook, elevated, and the dissection proceeds underneath the deep fascia and without touching the paratenon of the flexor muscles until the flexor carpi radialis tendon has been reached. Next, the radial artery is palpated, the skin incision is extended dorsally, and the first superficial branch of the radial nerve is identified. Close to this sensory nerve, the cephalic vein and the second branch of the radial nerve are carefully exposed (◘ Fig. 2.5).
Ligation of Vessels
Flap raising now proceeds from distal to proximal. For this, the radial vessels and the cephalic vein are ligated, always maintaining their contact to the skin paddle. Other than the vessels, the superficial nerve branches are carefully dissected away from the skin until they form a single nerve branch (◘ Fig. 2.6).
Raising the Flap from Distal to Proximal
At the same time, the radial vessels are elevated together with the lateral intermuscular septum as part of the deep fascia. Consequent hemostasis is performed when tracing the pedicle. If present, side branches of the cephalic vein crossing the lateral and inferior border of the flap are ligated. Both pedicles, the radial vessels and the cephalic vein, are closely attached to the flap via the deep fascia and the subcutaneous fatty tissue, respectively (◘ Figs. 2.7 and 2.8).
Dissecting the Cephalic Vein and Radial Vessels
The proximal incision is now carried out down to the deep fascia without injuring the cephalic vein. The fascia is opened between the brachioradialis and flexor carpi radialis muscles, and the radial vessels are followed as far as necessary for a tensionless anastomosis. The skin covering the cephalic vein is uplifted, and the vein is traced the same length as the radial vessels. It is clearly seen that the cephalic vein has a large caliber and that its superficial position makes dissection quick and easy. Before completely raising the flap and ligating the vessels, the venous return is tested in the superficial system. If there is strong venous backflow from the cephalic, it can be used as the single venous drainage of the flap (◘ Fig. 2.9).
Finishing Flap Raising
When using the cephalic vein as the only draining vessel, it is important to maintain the subfascial plexus within the adipose layer. Although this is also possible in the suprafascial flap-raising approach, protection of the fine vascular connections between the skin, cephalic vein, and radial vessels is the easiest when harvesting the flap conventionally together with the deep fascia (◘ Fig. 2.10).
Checking Venous Return
The capacity of either the superficial or deep system to drain the flap can be estimated by observing the backflow, but the most reliable method to provide a safe venous drainage is performing anastomoses to both, the cephalic and one of the deep veins. Further dissection of the vessels to the point where both systems are connected via a perforating vein might be associated with a risk of kinking and twisting a too long pedicle (◘ Figs. 2.11 and 2.12).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree