Key Words
preanesthesia evaluation, pre-operative checklist, anesthetic risk, medical history, resource limited
Synopsis
Elective surgery in resource-limited countries is often performed by mobile surgical teams, either as an outreach within the country itself, or as a volunteer group from another country. These teams provide a needed service; however, they are often operating in unfamiliar settings and with limited ancillary support. Careful screening of the patients with respect to overall health and post-operative requirements is necessary to ensure maximum benefit from the surgery, with minimum risk to the patient. This chapter offers guidelines for pre-operative screening, including a targeted medical history, the medical examination, and appropriate laboratory testing. Specific concerns are outlined. Sample medical history checklist and an immediate pre-operative checklist are included.
Introduction
You are planning to do surgery in a resource-limited country. The need is great. The surgical team is willing. Your goal is to help as many people as possible. In this setting, how can you ensure the maximum benefit for your patients with the least risk? Appropriate evaluation of the site and careful screening of the prospective patients are vital to ensure patient safety and to produce good outcomes. Site requirements and patient selection will vary according to area, team expertise, and the types of surgeries planned. The following are some general guidelines and considerations to aid in the process.
Screening of the Site
When planning surgery in a new and unfamiliar venue, the site should be evaluated. The more complex the surgery and the longer the recovery, the more important are the physical environment and the services available. Guidelines for the operating room (OR) and post-anesthesia care unit (PACU) needs are discussed in their respective chapters. The following are considerations for optimal post-operative care.
Ward Needs
- •
Adequate number of beds for anticipated patient days (number of patients × length of stay per patient).
- •
Hygiene: adequate bathroom and handwashing facilities.
- •
Ability to keep surgical sites clean post-operatively.
- •
Ability to ensure patient comfort (which in turn facilitates pain control). This includes temperature conditioning (AC units, fans, heaters) and positioning.
- •
Reasonable proximity to OR and PACU to allow monitoring and ease of transport. Ramps or elevators to move between levels may be needed.
Nursing Support
- •
Adequate trained nurses to carry out any patient care and medication administration that exceed the family’s capabilities (e.g., IV medications).
- •
Staff comfortable with monitoring patients for post-operative complications (bleeding, poor circulation, poor intake, uncontrolled pain).
Ancillary Support
- •
Availability of an intensive care unit (ICU) and arrangements for transfer of care, if needed.
- •
A laboratory able to perform blood counts, routine chemistries and, when appropriate, HIV tests, sickle cell anemia screens, and malaria screens.
- •
Access to a blood bank with the ability to obtain screened blood and to perform a type and cross-match in a reasonable length of time (1–2 hours).
- •
A pharmacy in-house or within a reasonable distance that can supply medications that are needed and that were not brought into the country by the team.
Follow-Up Care
- •
A designated, willing, and available practitioner is needed for the care needs during the time period when the team is no longer present (dressing changes, graft monitoring, pins, catheters, etc.). This individual should be identified before surgery and must realistically have time available. Optimally this person will be able to work with the operating surgeons while they are on-site and communicate with them after they leave, to discuss care concerns and to provide follow-up information.
- •
Physical/occupational therapy may be needed to monitor patients and provide splinting and exercises to preserve surgical improvements. Speech therapy is ideal after the correction of a cleft palate.
These follow-up care requirements are ideal. If certain requirements cannot be met, it does not necessarily mean that surgery is not possible. It does, however, limit the types of surgery that can be safely performed at the targeted venue and in the time allotted.
Patient Selection
Initial patient selection is made taking into account the expertise of the team and the time and facilities available. Patients can then be prioritized according to need and urgency. Generally, functional corrections take precedence over cosmetic improvements; however, the adverse effect of some cosmetic defects on a patient’s life may increase the urgency of repair.
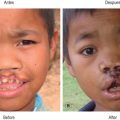
Consideration is given to timing “windows” such as early repair of cleft lips, timing of cleft palate repair for development of clear speech, and correction of strabismus or ptosis to prevent amblyopia. Expectations of the patient and the family should be explored. Families often expect the surgery to produce a “normal” appearance and function and need to understand the limitations of a procedure. In the case of multiple anticipated surgeries, the family and the surgical team together should establish priorities and the order of surgical interventions.
Finally, the ability of the patient and the environment to sustain improvements achieved by surgery should be considered. How vital is ongoing care (speech therapy, physical therapy, splinting) to the final success of the surgery, and is it available to the patient? This is a difficult judgment to make, because there are countless variables. It is, however, worth some thought. All surgery carries some risk, and the long-term benefits need to justify this risk.
Once a patient is selected for surgery, a more detailed history and examination is necessary to identify and evaluate any surgical or anesthetic risk factors. This screening is best accomplished by involving the surgeon, the anesthesiologist, and the pediatrician or internist. Each brings specific expertise and concerns to the screening process.
Patient Screening: History
A targeted patient history is the most important part of the pre-operative screening and has been shown to be the best tool for assessing anesthesia risk. Standard questionnaires have been validated as reliable tools in adults, and these can be modified for use with children. Areas covered include current health, past medical history, family history, and presence of any chronic conditions. In adults, exercise capacity has been proven to be a reliable indicator of cardiovascular status, and the threshold level for elective surgery is at least 4 METs (metabolic equivalents; 4 MET = climbing a flight of stairs or rapidly walking one block). Personal and family histories of bleeding problems are more predictive of clotting disorders than standard “screening” blood tests. Likewise, a personal or family history of anesthesia problems is a strong predictor for malignant hyperthermia or other anesthesia issues. Sample questionnaires for adults and children are included in this chapter ( Boxes 1.1.1 and 1.1.2 ).
- 1.
Is your child well today? Have they had a fever, cough, or runny nose in the last 2 weeks?
- 2.
Is the child taking any medications (including herbal medications and supplements)?
- 3.
Does the child have an allergy to any medications?
- 4.
Does the child have any chronic medical problems? Are they seeing a doctor regularly for a condition?
- 5.
Has the child had previous surgeries? When and by whom? Were there any problems?
- 6.
Has the child or anyone in the family had problems with anesthesia (requiring special treatment or a long hospital stay)? Did anyone have trouble awakening after anesthesia?
- 7.
Was the child born early? How many weeks early?
- 8.
Is the child developing normally? For school aged children: How is the child doing in school?
- 9.
Can the child run, jump, and play as actively as other children?
- 10.
Infants: Does the baby turn blue or get out of breath when nursing?
- 11.
Any heart problems? Does the child get blue lips or badly out of breath with exercise?
- 12.
Any lung problems? Asthma, bronchitis, or other trouble breathing?
- 13.
Does the child snore at night, and if so, does it awaken him?
- 14.
Has the child had seizures (convulsions) or fainting spells?
- 15.
Does the child or any family member have trouble stopping bleeding from small cuts? Do they get bruising on the face or around joints?
- 1.
Are you well today? Have you had a cold, cough, or fever in the past 2 weeks?
- 2.
Are you taking any medications (including herbal medications and supplements)?
- 3.
Are you allergic to any medications?
- 4.
Are you seeing a doctor regularly for any health problem?
- 5.
Are you a smoker? Do you use any drugs, or plants such as betel?
- 6.
Do you have any heart problems?
- •
Have you ever had a heart attack, a stroke, or chest pain?
- •
Have you ever been told that you have an irregular heartbeat or heart failure?
- •
Can you climb two flights of stairs without chest pain or breathing trouble?
- •
- 7.
Do you have any lung trouble like asthma, bronchitis or tuberculosis?
- 8.
Do you snore at night? Does it interrupt your sleep? Are you very sleepy during the day?
- 9.
Do you have high blood pressure? Is it being treated?
- 10.
Do you have diabetes? Is it controlled by diet, pills, or insulin?
- 11.
Do you have heartburn or stomach problems?
- 12.
Do you have kidney disease?
- 13.
Do you have thyroid problems? Are you taking medicine for it?
- 14.
Do you have pain, stiffness, or arthritis in your neck or jaw?
- 15.
Have you had surgery before? Were there any complications with the surgery?
- 16.
Have you or anyone in your family had complications with anesthesia?
- 17.
Have you or anyone in the family had trouble with bleeding that did not stop normally?
- 18.
Could you be pregnant?
If the provider taking the screening history is not fluent in the local language, accurate translation is vital. It is best to go over the screening questions with the translators in advance, so that they know what concerns are being addressed by each question and what answers constitute “red flags” that need further clarification. Translation of the questions into the local language/dialect may facilitate the process. The translator must be able to ask questions correctly in the patient’s language and to explain what is being asked, and must also have enough fluency in English (or the language of the surgical team) to explain the answers. A good translator can also help interpret cultural biases and local practices.
Be aware that some parents/patients may be reluctant to mention medical problems for fear that surgery will be denied. Families need to be assured that a medical condition will not automatically preclude surgery, and that accurate information is necessary to provide the best care possible.
Patient Screening: Physical Examination
A full physical examination is optimal but not always possible, particularly in a busy, crowded clinic. At a minimum, vital signs and evaluation of general appearance, airway, and heart and lungs are necessary.
- •
Vital signs (normal values for age are found in Table 1.1.1 ):
- •
Weight: For accurate calculation of fluids and medication doses and as part of the evaluation of nutritional status. Infants and small children must be undressed to avoid overestimating weight.
- •
Pulse, respirations, and pulse oximetry: As screening for unrecognized cardiac or pulmonary issues.
- •
Blood pressure: Required for ages 3 years and above to rule out hypertension.
- •
Temperature: As a screen for acute illness. Temperature >100.4°F or >38°C is considered a fever.
- •