Key Words
burn, contraction, contracture, axilla, shoulder, skin graft, fasciocutaneous, flap, perforator flap
Synopsis
Burn injury to the axilla is caused by flame or direct contact. Ignition of clothing is the most common cause. Burns that will not heal within 2 weeks should be excised and skin grafted to prevent progressive scar contraction that will directly affect shoulder motion. Pain during acute burn management will limit abduction of the arm. The supple, concave quality of the axilla offers reduced resistance to burn contraction, subjecting the patient to potential long-standing painful, restricted motion.
Reconstruction of the burned axilla should be considered early as a pattern of functional loss of motion develops. The choice of reconstructive procedure depends on the extent of axillary involvement as well as on the quality of the peripheral tissue. Surgical treatment should reduce pain and maximize shoulder motion. Analysis of tissue deficiency, contraction patterns, and quality of tissue to be used for replacement will identify the proper treatment for each individual patient. As the contracture increases in complexity, knowledge of composite tissue transfer is essential to produce the best outcome while minimizing complications and recurrence.
Clinical Problem
The axilla is the area of skin and soft tissue underlying the shoulder joint. It is a supple, concave area defined by an anterior and posterior skinfold. The anterior fold is bordered by the lateral edge of the pectoralis major muscle; the posterior fold by the subscapularis, teres major, and latissimus muscles. The superior border consists of the first rib, clavicle, and scapula. The lower portion of the axillary skin is contiguous with the thorax. The contents of the axilla, deep to the subcutaneous tissue, include the axillary vessels, the brachial plexus, the long thoracic nerve, and axillary lymph nodes and lymphatic vessels. The skin of the axilla is of variable thickness. It is thinner at the cupola and thicker at the anterior and posterior folds. The density of hair follicles at the axillary cupola can be a potential source of increased healing by epithelialization in more superficial burn injuries to that protected area.
Burn injury to the axilla is often part of a larger chest/back burn in which loose clothing has caught fire, very often in cooking-related fires with direct injury to the torso and the outstretched arms. In regions where open, unprotected cooking fires are used in the home, burn injury to the axilla may be more common, especially in small children, who may fall or roll into the open fire. Explosions of stoves and ceramic cooking vessels are also a source of burns to the torso, upper extremities, and axillary areas.
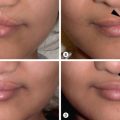
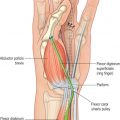
Acute management of the axillary burn requires the assessment of burn depth and area of involvement. If third-degree burn is found over the majority of the axillary surface, early excision and grafting should be planned ( Fig. 4.6.1 ). Given the supple quality of the skin and the degree of concavity of the axilla, significant scar contraction will occur if the full-thickness burn is not excised. The resulting burn scar creates a skin deficiency that will limit motion of the shoulder. If partial-thickness injury is present and the expectation of healing by epithelialization is anticipated, conservative management with dressing changes may be considered ( Fig. 4.6.2 ). Splinting the arm in abduction both pre-operatively and post-operatively will be essential to reduce the potential for contraction. Early motion during the post–skin grafting or epithelializing period is extremely important.
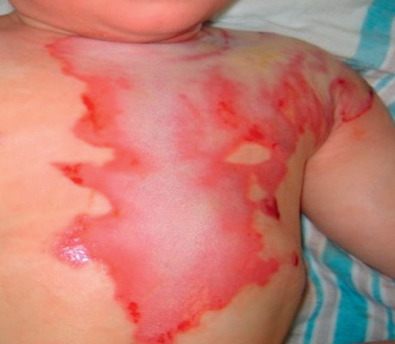
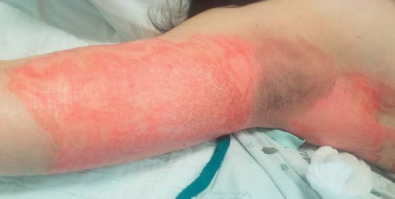
Burns of the axilla and shoulder are painful. Early excision of the deep burn with skin graft resurfacing replaces the anticipated contracting burn scar with better-quality tissue essential for early range-of-motion exercises. Axillary contractures and limitation of shoulder motion will be functionally significant in all deep axillary burns that go untreated. Even with optimum burn excision, skin grafting, or quality epithelialization in lesser-depth burn injuries, 27% of the patients will show axillary contractures when the scars have matured.
After healing of the grafted or epithelialized axillary burn, the surgeon will initiate a therapy plan to include scar massage, passive motion, and progressive stretch. Gains in abduction are maintained using splints between exercise periods and especially at nighttime. Splints and exercises opposing contraction are continued until scar maturation is complete and improvement in scar restriction occurs. Motion exercises are essential in preventing periarticular fibrosis of the shoulder joint. Limited shoulder motion is associated with a high degree of axillary contracture post-burn.
Continuous range-of-motion and stretch exercises of the shoulder after acute burn injury and resurfacing are essential to minimize contraction during the scar maturation period. As improvement of shoulder motion plateaus, identification of specific developing axillary contracture patterns will define the reconstructive stage of axillary burn management. Burn scar is synonymous with tissue deficiency. An appreciation of scar tension, direction of contraction, and timing of procedures associated with axillary contracture is important for the burn surgeon. Early intervention will be of great benefit to the patient.
Pre-Operative Management
In the acute burn to the axilla and shoulder, correct assessment of burn depth is critical. If the etiology of the burn is flame from ignited clothing or direct contact with fire, burns are likely to be third-degree in depth. The shape of the axilla is concave, which reduces all resistance to burn scar contraction. Early excision of the burn is indicated as soon as deep second- or third-degree depth is appreciated. Replacement of all burned tissue with healthy skin graft, followed by an exercise regimen, is the ideal course. Prioritizing areas of excision will depend on total extent of body surface area burn, with more critical and larger areas undergoing excision and grafting first. The injured axilla should not be ignored because of the small area of burn. The shoulder is the most mobile joint in the body, and any restriction of supple tissue in the periphery will quickly decrease its range of motion.
The optimum timing for management of the acute axillary burn corresponds to the clinical appreciation of full-thickness injury. This usually occurs by the second to third day after the injury. Pre-operative testing is dependent on the overall extent of body surface area burn. Dehydration secondary to third space burn swelling and a reduced level of hemoglobin expected in larger burn injuries must be corrected.
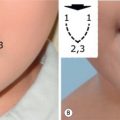
From the reconstructive perspective, late burn scar contracture of the axilla after scar maturation is classified based on local anatomical conditions. The classification chosen facilitates reconstructive planning based on the expected amount of tissue deficiency. Specific procedures will be indicated based on the expectation of long-term improvement of shoulder motion and the probability of recurrence of contracture. The classification scheme guiding reconstruction uses four progressively increasing scar deformities:
Type I: Linear scar contracture web at either axillary fold with minimal adjacent scarring.
Type II: Scar contracture at either axillary fold with adjacent skin scarring.
Type III: Linear web at both anterior and posterior fold; cupola spared.
Type IV: Axillary folds, hair-bearing skin, and entire axilla are obliterated.
Surgery
In surgery, an amount of clysis solution (1 mL epinephrine 1 : 1000 in 1 liter of saline, final epinephrine concentration of 1 : 1,000,000) is injected into the subcutaneous tissue below the burn, reducing bleeding during the tangential or full-thickness excision. The injection of this fluid also brings the depth of the axillary skin into a more manageable position for excision. The clysis injection can also be used below the donor areas, reducing the total amount of blood loss during the acute burn excision and grafting. A dermatome is used for skin harvest, set at a moderate depth of 0.012 inches. A widely pie-crusted sheet or 2 : 1 meshed graft will contour nicely into the axilla once full hemostasis is obtained. Positioning of the arm is important during the surgery; abduction beyond 90 degrees must be well controlled and limited to short periods of time only. This will prevent brachial plexus stretch and resultant post-operative paresthesia.
Acute excision of the axillary burn is followed by immediate skin grafting if hemostasis is complete. Shearing of the graft is the greatest mechanical complication in the immediate post-operative period. A well-designed and secured tie-over dressing will permit the graft to drape well into the configuration of the axilla and provide even contact with the depth of the excision, optimizing engraftment. The post-graft splinting protocol abducts the arm to approximately 90 degrees of abduction with external rotation of the shoulder. Comfort in the splinted position and the absence of distal paresthesia are important for splint compliance.
As soon as skin graft take is apparent, therapy begins with both active and passive range of motion and stretch of the shoulder region. Use of splinting for a minimum of 5 days will provide an improved opportunity for graft take. Range-of-motion exercises with splinting between exercise periods and at night will help to maintain position. Exercises and abduction splinting will add resistance to the contraction process. Splints are maintained until the patient can easily overcome the tension of the healing skin graft. The use of a trapeze attached to the bed or overhead bars from which patients can use their body weight to complement resistive stretch is also desirable.
After a burn to the axilla, range of motion of the shoulder becomes painful. The unsplinted arm will remain adducted against the torso with shoulder rotation depending on the extent of the axillary and torso burn involvement. If early excision is planned, the position of the shoulder should accommodate dressing changes comfortably. Abduction splinting to 90 degrees begins immediately after (if not before) excision and grafting. This places the arm in an advantageous position to begin range of motion once the graft has taken and therapy begins. The splint stabilizes the arm/axilla, allowing optimal graft take and reducing the risk of graft loss complications. Splinting protocols vary between authors. A greater area of burn excision and grafting and the late onset of therapy were associated with a worse outcome of shoulder range of motion after discharge.
The reconstructive phase of axillary burn contracture begins when the patient has reached the maximum improvement of shoulder motion possible, opposed by significant limitations secondary to scar restriction. Long-standing principles suggest delaying contracture release until the burn scar has softened and matured. A more practical approach, however, suggests early intervention for release and reconstruction when the surgeon and therapist identify progressive loss of shoulder motion with low expectation of further improvement. Greenhalgh and colleagues have shown that there are no adverse outcomes from performing scar release and reconstruction of the axilla before complete scar maturity is present. An earlier return to improved range of motion benefits the patient.
Surgical reconstruction of the burn-contracted axilla will vary based on the classification of axillary deformity. The following outlined procedures suggest greater complexity as the burn scar and tissue deficiency become more pronounced. Successful outcome of the axillary release and reconstruction will be based on available peripheral tissue, patient compliance, and reduced complications.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree