Figure 13.1
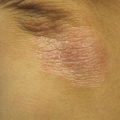
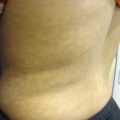
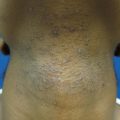
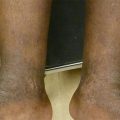
Postinflammatory hyperpigmentation. 30 year-old African-American woman with ill-defined hyperpigmented macules and patches on the chest
Clinical Differential Diagnosis
In this particular case of scattered macules and patches involving the chest, one may consider diagnoses such as pityriasis versicolor, postinflammatory hyperpigmentation (PIH) or erythema dyschromicum perstans. The former tends to present with surface scale, while the latter may have a component of erythema and a more widespread distribution. The differential diagnosis of hyperpigmentation can be vast and depends on the clinical presentation. Preceding inflammation may be subclinical in some instances, which may further complicate diagnosis. History, morphology and distribution can help narrow down potential inciting factors.
Histopathology
Hyperpigmentation on histology can be epidermal, dermal or mixed, where an excess of melanin is present in both the epidermis and dermis (Ortonne and Passeron 2005). Most cases of post-inflammatory hyperpigmentation will show increased pigmentation in basal epidermal keratinocytes; however, there may also be a dermal component, showing melanophages. Clinically, brown and blue hyperpigmentation are caused by excessive amounts of melanin within the epidermis or dermis, respectively. Focal deposition of melanin is mainly seen in PIH, which can occur after a burn, laceration, acne or any inflammation inducing insult to the skin (Davis and Callender 2010).
Diagnosis
Postinflammatory hyperpigmentation (PIH) secondary to acne vulgaris.
Case Treatment
As aforementioned, the patient did not note improvement with 4 months of twice a day use of over-the-counter hydroquinone 2 % cream. Hydroquinone 4 % cream twice a day to affected areas, along with daily broad spectrum sunscreen with at least sun protection factor 30 were recommended. In addition to addressing treatment of hyperpigmentation, the underlying causative condition, acne vulgaris, was also treated with benzoyl peroxide 4 % wash followed by topical clindamycin 1 % lotion every morning. Three months of this treatment regimen caused significant clinical improvement of hyperpigmentation.
Discussion
Hyperpigmentation is an umbrella term for a group of conditions that cause dark discoloration of the skin and includes melasma, PIH and medication-induced hyperpigmentation. Hyperpigmentation most commonly affects patients with Fitzpatrick skin phototypes IV-VI who are often patients of African, Asian, Hispanic, Pacific Islander, and/or Native Hawaiian backgrounds. There is no gender or age predilection. Considering dyschromia is one of the top five skin diagnoses in African-American patients, keen knowledge of pathogenesis, diagnosis and available treatment options for hyperpigmentation is of vital importance (Alexis et al. 2007). While considered cosmetic by some standards, dyschromias, such as PIH may have lasting psychosocial effects.
Acne-induced PIH is a particularly common occurrence in patients of color (Fig. 13.2). In a 2002 study that evaluated acne in skin of color, 65.3 % of African-American (N = 239), 52.7 % of Hispanic (N = 55), and 47.4 % of Asian (N = 19) patients acquired acne-induced PIH (Taylor et al. 2002). Atopic dermatitis, a chronic inflammatory dermatosis, has a prevalence of 10.7 % in the US, with a significantly higher prevalence seen in both the African-American populations. A common sequela is PIH (Vachiramon et al. 2012).
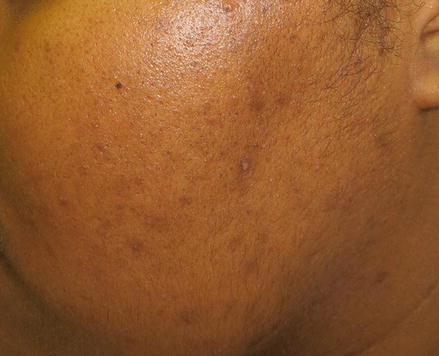

Figure 13.2
Acne induced postinflammatory hyperpigmentation. A young African-American woman with hyperpigmented macules on the cheek as a result of mild inflammatory acne vulgaris
The etiology of PIH has not been fully elucidated, however, it is hypothesized to involve inflammatory mediators, including prostaglandins (PGE2) and leukotrienes (LTC4 and LTD4). These mediators go on to stimulate epidermal melanocytes, causing an increase in melanin synthesis in the basal layer of the epidermis or release of melanin from labile melanocytes into the dermis. Elevation of melanin in the dermis in turn activates dermal macrophages (Desai 2014).
Treatment
The initial approach to treating PIH begins with identifying and treating the underlying dermatosis. Once this is achieved, the resulting hyperpigmentation may then be targeted. A crucial element in the treatment of hyperpigmentation is the use of photoprotection. Use of a broad spectrum sunscreen with a sun protection factor of 30 or higher every two hours during sun-exposure will effectively prevent the worsening of hyperpigmentation (Desai 2014). After any possible inciting causes and photoprotection are addressed, it is then reasonable to initiate topical skin lightening agents. Such agents, alone or in combination, include: hydroquinone (HQ), mequinol, azelaic acid, kojic acid, retinoids, and soy.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree