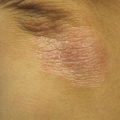
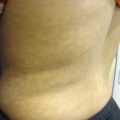
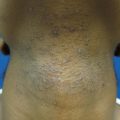
Figure 7.1
Atopic Dermatitis. Hyperpigmented scaly patches at the knees bilaterally
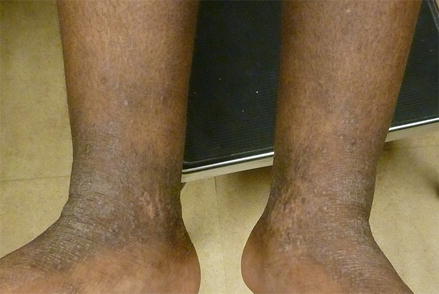
Figure 7.2
Atopic Dermatitis. Hyperpigmented scaly plaques at the ankles bilaterally
Differential Diagnosis
Based on age and clinical exam, atopic dermatitis was highest on the differential. Other forms of dermatitis such as contact dermatitis and seborrheic dermatitis were considered (Spergel and Paller 2003). Wiskott-Aldrich syndrome and hyperimmunoglobulin E syndrome are rare clinical entities but may also present with eczematous skin changes and were thus also considered, although in this case the appropriate constellation of symptoms were lacking (Dermatology atlas for skin of color 2014).
Histopathology
A biopsy was not performed in this case, as atopic dermatitis is a clinical diagnosis. Rarely, when a biopsy is performed, epidermal spongiosis and a superficial perivascular lymphocytic infiltrate with some eosinophils and melanophages is seen (Dermatology atlas for skin of color 2014; Vachiramon et al. 2012).
Diagnosis
Atopic dermatitis
Case Treatment
The diagnosis of atopic dermatitis was discussed with the patient’s family, including the characteristic locations of infantile atopic dermatitis and the potential for postinflammatory hypo- or hyperpigmentation. Various treatment options were discussed, including skin hydration, topical corticosteroids, and/or topical immunomodulators. Given that this infant’s lesions were located primarily on the face, hydrocortisone 2.5 % ointment twice daily was prescribed for a 2-week course (Eichenfield et al. 2014). The family was told that should this treatment fail to provide symptomatic relief, a stronger corticosteroid could be prescribed. For maintenance, transition to a topical immunomodulator, such as pimecrolimus or tacrolimus, could be given. The family was also instructed to apply moisturizers immediately after bathing for better skin hydration.
Discussion
Atopic dermatitis (AD/eczema) is one of the most common skin disorders seen in infants and children, with the prevalence in the United States population estimated to be approximately 17.2%(Spergel and Paller 2003). Epidemiologic studies have reported that atopic dermatitis is a condition that disproportionately affects individuals of color. Based on data collected between 1993 and 2009 from the National Ambulatory Medical Care Survey, a sampling of ambulatory care visits to U.S. physicians, showed that AD was among the top ten diagnoses for both African Americans and Asian/Pacific Islanders but was not among the top ten diagnoses for Caucasians (Davis et al. 2012). Other studies have shown that African American children are much more likely than Caucasian children to have severe atopic dermatitis, potentially due to poor access to care or delayed diagnosis (Vachiramon et al. 2012). Of note, the word ‘eczema’ is pronounced differently around the world, and amongst individuals with skin of color. Three variations can be heard; “\ig-ˈzē-mə, ˈeg-zə-mə, ˈek-sə-\” (www.meriam-webster.com).
The pathophysiology of atopic dermatitis is poorly defined but the main hypothesis relates to epithelial barrier and immune dysfunction. Mutations in the gene coding for filaggrin, a protein that helps to replace the plasma membrane in anucleated stratum corneum cells, are thought to be a factor, as filaggrin keeps the stratum corneum cohesive and affects epithelial cytokines (Dermatology atlas for skin of color 2014).
Atopic dermatitis classically appears in three sequential phases: infantile, childhood, and adult. The infantile phase is characterized by pruritic, erythematous patches and plaques that are generally located on the forehead and cheeks. The trunk or extensor surfaces may become involved with scattered, symmetrical, ill-defined patches. Affected areas tend to be edematous and fissured, often leading to secondary crusting. Pruritus is often severe, resulting in a disturbed sleep patterns. In children who are over 1 year of age, nummular lesions may accompany the erythematous patches of AD (Spergel and Paller 2003). In individuals with skin of color, erythema can be difficult to assess and thus should not be extensively relied upon. Instead, edema, warmth of the skin, and scaling in these particular distributions can help to correctly diagnose AD (Dermatology atlas for skin of color 2014).
The childhood phase of atopic dermatitis generally occurs from 2 years of age to puberty. Lesions are less likely to be exudative and are more likely to display lichenified papules and plaques more indicative of chronic disease. In children, lesions are classically seen in the hands, antecubital region, wrists, popliteal region, ankles, and feet (Spergel and Paller 2003). In African American children, a distinct clinical presentation is often seen with micropapules and perifollicular accentuation, leading to the development of monomorphic follicular papules coalescing into plaques on the trunk and extensors (Dermatology atlas for skin of color 2014; Vachiramon et al. 2012). These lesions must be distinguished from lichen nitidus, although lichen nitidus is typically located on the trunk, flexors, and genitalia and is less pruritic. In African Americans, AD lesions can also closely resemble lichen planus, although the distribution of AD lesions (extensor surfaces with limited genital and mucosal involvement) helps to distinguish (Vachiramon et al. 2012).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree