Key Points
- ▪
Intra-aortic balloon pump position is readily verified by chest radiography, because the tip is radiopaque. The tip should be located at the very distal aortic arch or proximal descending aorta.
- ▪
Percutaneously inserted ventricular assist devices are radiographically apparent, and at least in a comparative sense, their position can be verified by chest radiography.
- ▪
The positions of cannulae of extracorporeal membrane oxygenation (ECMO) systems can be verified by abdominal and chest radiography.
- ▪
The cannulae of ventricular assist devices are also radiographically apparent.
Percutaneous Devices
Pulsatile Devices: Intra-aortic Counterpulsation Balloon ( Figs. 24-1 to 24-7 )
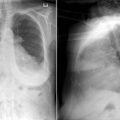
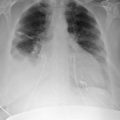
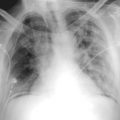
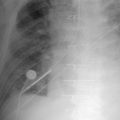
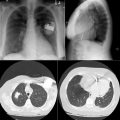
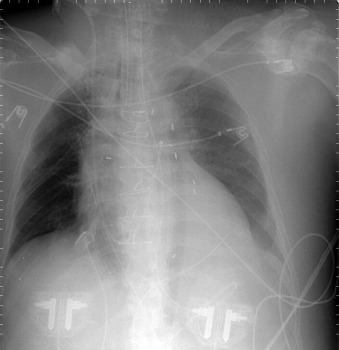
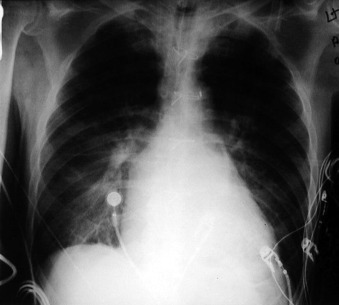
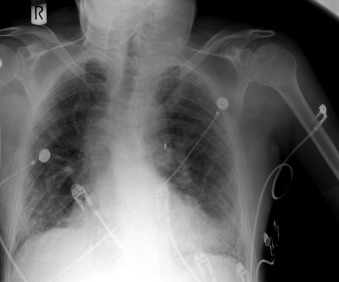
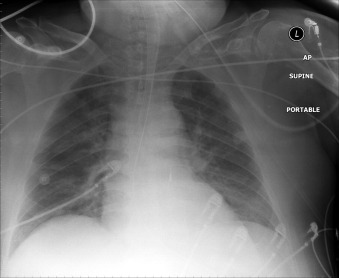
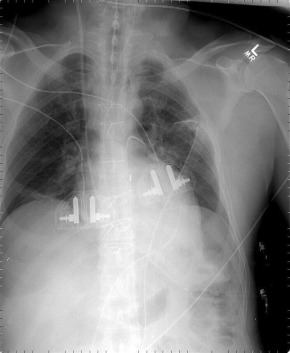
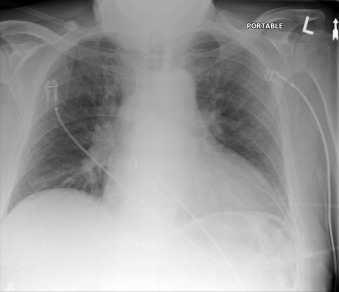
The tip of an intra-aortic balloon (which is highly visible because of its metallic marker) should be at least 4 cm below the “knuckle” of the aorta (i.e., below the left subclavian artery). The balloon appears as a cylindrical lucency if the radiographic exposure happened to be while it was inflated in diastole. Widening or haziness of the aorta suggests aortic dissection as a complication of the catheter. Incorrect insertion into the inferior vena cava is suggested by the shadow of the catheter lying to the right of the patient’s vertebral column.
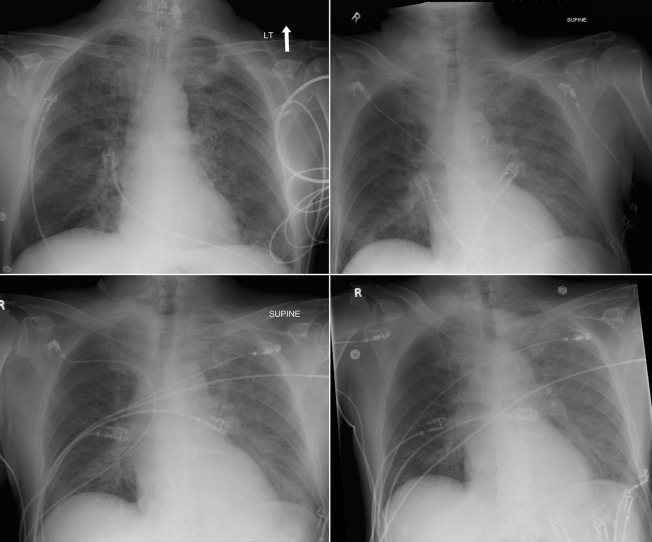
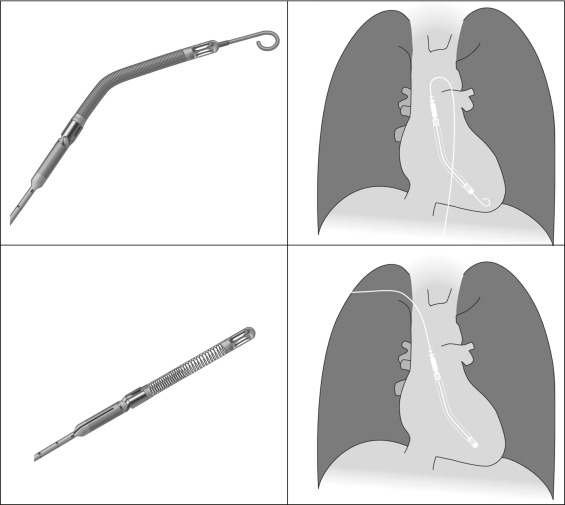
Continuous Flow Devices: Impella 2.5
The Impella 2.5 (2.5 L/minute support), a continuous flow ventricular assist device, provides continuous flow assist comparable to that of intra-aortic balloon pump. It is percutaneously inserted from the groin. Radiographically and fluoroscopically, the pigtail tips are apparent, the mechanical intake device and the mechanical output device are obvious and the conduit between the two is fairly obvious, and the more proximal catheter is marked by a faint radiopaque stripe. The pigtail tip holds the intake back from the apical wall; the intake housing draws ventricular cavity blood into it, and the output housing with the impeller pump draws blood through the intake housing and ejects it into the aortic root on the far side of the aortic valve, offloading and resting the left ventricle. On a frontal radiograph, the pigtail is directly left inferiorly and the conduit initially follows the same line before it angulates vertically or vertically/leftward up the aortic root.
Surgically Inserted Ventricular Assist Devices
There are several models of surgically inserted (left and right) ventricular assist devices with widely different designs and radiographic appearances.
Impella 5.0
The Impella 5.0 (5.0 L/minute support) is inserted by surgical cutdown or via sternotomy ( Graphic 24-1; Figs. 24-8 to 24-13 ). There are two models. The Impella 5.0 is similar to that described previously. The Impella 5.0 LD is similar but without the pigtail component.