Introduction
Surgery is the key component of burn care for inflammatory source control, pain control, expedited healing, and survival. The exact operative plan needs to fit the resources available to each individual patient and institution but generally follows the same precepts:
-
1.
Early decompression and medical optimization of perfusion
-
2.
Diagnosis of injury depth and extent
-
3.
Early excision of burn wounds and source control
-
4.
Wound closure
Early intervention in the form of early burn wound excision and grafting has dramatically changed the outcome and survival of the burn patient. In our practice, integration of operative and anesthetic care can dramatically reduce patient suffering.
As discussed in chapters on the etiology of burn shock, edema, and critical care, damage-associated molecular pathways (DAMPs) and pathogen-associated molecular pathways (PAMPs) drive the inflammatory process of burn disease. Inflammatory mediators such as prostaglandins, histamine, and cytokines in the serum increase proportionally to the surface area of the burn. Hypermetabolism and catabolisms, as well as weight loss, poor wound healing, and immune depression continues until the outpouring of mediators abate. , Early surgical extirpation in conjunction with medical care can arrest or mitigate this process and improve outcomes.
Early decompression and medical optimization of perfusion
The first goal with any patient is to establish and maintain tissue perfusion and ameliorate shock. Medically, we advocate goal-directed fluid resuscitation and treatment of organ failures, which typically begin in patients with greater than 20% total burn surface area (TBSA). This is well discussed in the chapters on resuscitation and critical care. Eschar compression and compartment syndrome are two major surgically treatable diseases that compromise perfusion. These must be diagnosed early and treated rapidly.
Escharotomy
Burn eschar shrinks relative to the native tissue due to protein denaturation and increased protein hydration sites. In circumferential or large-area burns, this force can cause a compromise in blood flow by exceeding venous outflow pressure or even exceeding arterial inflow pressure. As resuscitation proceeds and edema progresses, these eschar compressions can form a feedback loop exacerbating shock. The compartment syndrome associated with eschar compression is distinct and treated differently than that typically discussed with compartment syndromes that result from excessive edema within the fascial compartments. Eschar compression creates a compartment syndrome due to an extrinsic decrease in volume of the compartment, whereas a traditional compartment syndrome is created by increased compartment volume constrained by an inelastic fascia.
Escharotomy is the surgical division of these tissues to allow sufficient diameter of the tissues and to allow perfusion. These incisions should be completely through the eschared skin and also include the investing Scarpa fascia to allow the subcutaneous fat to spread widely and fully decompress. Often this will be accompanied by reperfusion of the tissue. In doing so, tissue that had appeared full thickness may be determined to be viable ( Fig. 11.1 ). Escharotomy incisions are generally extended onto normal skin to ensure adequacy. Adequately performed incisions on the trunk or extremities will typically spread open 5 to 10 cm when relieving an eschar compression that is compromising perfusion. Although there are typically escharotomy incision locations that are described in books and internet articles, it is more important to ensure adequacy of decompression and perfusion than to focus on precise locations. As a general rule, the eschar being incised today for perfusion will be excised tomorrow for source control.
There are areas to take particular care with an escharotomy: external jugular, ulnar nerve at cubital tunnel, sternum, clavicles, tarsal tunnel on the medial ankle, and the femoral canal. These escharotomy sites are handled carefully as there are structures beneath that are difficult to cover later, so careful planning needs to start at the first incision.
Management of the defects created by escharotomies and fasciotomies vary from center to center. Care should be taken to choose a hemostatic and antibacterial material aimed at preventing bleeding, infection, fluid loss, tissue desiccation, and pain. In our center we typically use homograft, discussed later, as it achieves these goals well and is readily available in our institution.
The hands are a special area for decompression and are discussed in a separate chapter. If the hand is warm, soft, has pulsatile flow detectable by Doppler in the palmar arch and the digital vessels, and has a normal pulse oximetry signal at the tip of the digit, then flow is adequate. However, as flow becomes progressively impaired, the hand will become firm and cold, with decreased Doppler flow and loss of the pulse oximetry signal. Decompression should be performed to prevent otherwise avoidable ischemic injury because of eschar compression. Pressure measurement confirmation is generally not required if serial examinations suggest diminished tissue perfusion. In patients who are distracted with pain from burn wounds, sedated or intubated early decompression may be wise to avoid a missed ischemic injury. Escharotomy is typically performed using electrocautery. Longitudinally oriented medial and lateral incisions are made through eschar on the arm and forearm, stopping at the metacarpophalangeal joints (MCPJs) of the first and fifth digits ( Fig. 11.1 A).
(A) Arm escharotomy. (B) Hand escharotomy. (C) Finger escharotomy.
(From Fig. 61.6ABC in Green DP, Pederson WC, Hotchkiss RN, et al., eds. Green’s Operative Hand Surgery . Elsevier/Churchill Livingstone;2005:2164.)
The necessity of digital escharotomies is an issue of long-term debate. One study demonstrated a reduced incidence of amputation if digital escharotomies were performed on circumferentially burned digits. However, particularly in small children, improperly performed digital escharotomies can result in significant injury, and therefore caution must be used to avoid injury to the neurovascular bundles. When digital perfusion remains inadequate despite decompression of the arm, forearm, and hand, escharotomies of full-thickness burns of the digits should be performed. Longitudinal incisions are made carefully mid-lateral between the neurovascular bundle and the dorsal extensors, avoiding both structures. A single longitudinal incision is made on the radial aspects of the thumb and little finger and the ulnar aspects of the digits. This places the incisions on the side of the digit with the least functional importance should the digital nerve be exposed by separation of edematous tissue after escharotomy. The central digital incision can be extended proximally onto the dorsum of the hand between the metacarpals to enhance decompression ( Fig. 11.1 B). The line of incision along a given digit can be found by putting the fingers in maximal flexion, marking the lateral extensions of the flexor wrinkles and completing them to a continuous line that represents the insertion of Cleland’s ligaments, which constrain the neurovascular bundle volar to that line ( Fig. 11.1 C). Meticulous hemostasis is maintained throughout the procedure.
Escharotomy can be performed at the bedside or in the emergency department under moderate sedation supplemented with subeschar injections of local anesthetic. Some patients will benefit from general anesthesia in the operating room for the procedure to be performed appropriately. The care location is most often determined by the resourcing of the institution with priority given to establishing flow rapidly and maintaining resuscitating goals and patient comfort.
Fasciotomy
Fasciotomy is required less often in burn injuries. However, in cases of deep compartment injuries as seen in high-voltage electrical injuries, very deep thermal burns, or massive resuscitations, compartment fasciotomies are critical. Additionally, as large resuscitation volumes might be needed in larger injuries, fascial compartment syndromes may be manifested. Monitoring of clinical signs of compartment syndrome can be compromised by distracting injuries or sedation. Clinical signs of rhabdomyolysis can be a critical monitor for late compartment syndrome. As fluid volumes exceed 200 mL/kg in 24 hours, careful consideration must be taken for such syndromes, particularly in the anterior tibial compartments, even if uninjured. Upper-extremity fasciotomy may include volar and dorsal decompression, carpal tunnel release, and dorsal hand fasciotomy. A curvilinear incision is ideal for volar exposure of the compartments of the forearm.
Finally, orbital compartment syndrome must be considered, particularly in the setting of massive facial burns and periorbital edema as discussed in the ophthalmology chapter. The globe should be soft and ideally pressures measured. If there is intraorbital hypertension, or it cannot be ruled out, decompressive lateral canthotomy should be performed as a vision-preserving procedure. Lateral canthotomy should be performed in cases of OCS, described above. Structure is provided to the lids by the canthal tendons, inserting on the upper and lower tarsi medially and laterally. The lateral origin is palpable as a bony prominence at the lateral orbital rim, called Whitnall’s tubercle. Lateral canthotomy is performed by dividing the skin and lateral canthal tendon, freeing the lower lid from its bony attachment. 1 or 2% lidocaine with epinephrine is infiltrated lateral to the lateral canthus, the skin clamped parallel to the palpebral fissure, then divided with scissors anteroposteriorly. The lower lid is grasped and pulled away from the globe, placing the lateral canthal tendon on stretch, making it easier to locate and divide. The canthal tendon is divided with scissors anteriorly to Whitnall’s tubercle on the orbital rim. , A successful lateral canthotomy leaves the lower lid freely mobile and no longer apposed to the globe. Afterward, the intraocular pressure should be re-evaluated.
Diagnosis of injury depth and extent
The timing to determine the precise depth and extent of a burn injury is a moving mark that begins at the time of initial evaluation by first responders and is not complete until after definitive excision. Indeed, burn-injury depth can increase as the zone of stasis progresses to a zone of necrosis due to patient and resuscitation factors. In the immediate presentation, an answer sufficient to begin goal-directed fluid resuscitation and reestablish perfusion is good enough. When moving toward early excision, the precise depth of the burn wound becomes more important as we determine that tissue needs to be excised and to what depth. Ultimately, this is to determine the vascularity of the tissue and the viability of the dermal appendages that will reepithelialize the skin.
Clinical evaluation remains the gold standard for evaluation of burn depth, and in studies experienced surgeons are 77% accurate. Erythematous skin without epidermal separation is defined as first degree and does not need any surgical intervention. Partial-thickness burns have a loss of epidermis as noted by blistering with a portion of surviving dermis. In the clinical evaluation of partial-thickness burns, the key goal is to excise dermis with coagulative necrosis. A major difference between superficial and deep partial-thickness burns is determined by excision where the viable dermis with punctate bleeding has vessels that are able to bleed do not have coagulative necrosis. This can also be evaluated in terms of capillary refill, where blanching of tissue is indicative of tissue where patent dermal vessels are able to have the blood manually pressed out of them, then reperfusion when the pressure is released. In the setting of evaluation under tourniquet and exsanguination, tissue that remains pink is indicative of coagulative necrosis as the blood is not able to be exsanguinated from coagulated vessels. Full-thickness burns are noted to be leathery and dry or white. The underlying fat is clinically determined to be viable when a yellow glistening appearance is encountered. Dull yellow color, purple discoloration, or thrombosed vessels indicate nonviable tissues that are not suitable for grafting and require deeper excision ( Fig. 11.2 ). When excision is performed on limbs with a pneumatic tourniquet, these clinical features are particularly important. As the patient’s wounds are excised and the ultimate depth of the wounds is determined, it is important to update the patient’s diagnosis of TBSA and depth of injury to ensure appropriate treatments, patient risk stratification, and quality improvement. Total body surface area of wounds can be arrived at by Lund and Browder body surface area estimation and by direct wound measurement and division by the patient’s calculated body surface area. Both of these methods are subject to their own inaccuracies; however, it is important to remember that they are estimations and tools for planning care and predicting outcomes, not absolute numbers with immutable implications.
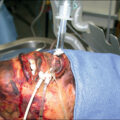
A deep flame burn on the left thigh that is in the process of being debrided. The wound has been tumesced with 1:1,000,000 epinephrine in normal saline and shows minimal bleeding. The lower part of the wound demonstrates residual dead dermis with dull appearance and staining from lysed cells. The area just above demonstrates shiny yellow, living fat and (mostly) surviving shiny white dermis with a few patches needing another slice.
There are noninvasive imaging tools available for predicting burn depth and healing time. These were generally used for research purposes but are creeping into clinic use over time. These include laser Doppler imaging (LDI), which is the current gold standard in research; infrared thermography (IRT); and spectrophotometric intracutaneous analysis (SIA). LDI uses a low-intensity laser beam to scan across the tissue surface. Laser is both absorbed and scattered by tissue matrix and the blood flow in the vessels. Flux is then determined by processing the photocurrent resulting from both absorbed and scattered light. The device generates a colored map of the wound correlating with the extent of the injury. LDI can be a useful tool in surgical decision-making in indeterminate-depth burns.
IRT uses the heat signature resulting from tissue perfusion to predict the depth of burn injury. Superficial burns retain a bright color compared with the surrounding normal tissue due to increased perfusion, whereas deeper burns appear darker in color due to decreased or lack of perfusion. , SIA is used in the diagnosis of pigmented skin lesions such as melanoma. It uses spectrally filtered images using polarized light ranging from 400 to 1000 nm. A complex set of mathematical algorithms determines the melanin and hemoglobin content of the epidermis and papillary dermis, then presents them in high-resolution images. The additional analysis of pigment available using SIA may more accurately indicate the depth of burn compared with perfusion alone.
The DeepView device is an artificial intelligence device that uses color photography to assess burn wound depth. It has been trained in a study by Phalen and Carter with 816 validated biopsy-determined burn wounds, is undergoing validation on 640 unique patients, and is demonstrating promising data in predicting burns requiring excision and grafting versus those that will heal with nonoperative management. This device-leveraging machine learning may improve diagnostic ability and allow doctors with less experience to improve their care while improving the precision of diagnosis within the burn community.
Ultrasounds with frequencies higher than 20 MHz have shown promising results in quantitative assessment of burn depth in animal models. Currently, only LDI has been validated for use in burn-depth assessment, although DeepView is moving quickly in that direction. Imaging has potential as a decision support tool for the burn surgeon, but it is not a replacement for skill and experience. Given the evolution of burn wounds over time because of patient physiologic parameters (e.g., resuscitation) and extrinsic factors (e.g., pathogens), it is unclear how generalizable these research findings will be to a broad burn population at varying sites globally. It is also unclear that the costs and added complexity of these diagnostic adjuvants will sufficiently improve care to supersede clinical evaluation by a trained and experienced surgeon.
Early excision of burn wounds and source control
Advantages of early excision
Early burn wound excision is a standard of burn care along with goal-directed fluid resuscitation. As with every form of inflammatory shock, rapid source control is a prime component of care, and in the burn patient the burn wound is the source. Early excision and skin grafting to achieve wound closure have been shown to reduce infection rates, reduce length of hospital stay, and improve survival in burn patients. Pediatric burn patients in particular have benefited from timely surgical intervention. , There has been a remarkable increase in the TBSA associated with a 50% mortality risk over recent decades. It is now usual for a child to survive burn injuries of any size, even in association with an inhalation injury ( Tables 11.1 and 11.2 ). Early prompt fluid resuscitation, appropriate critical care, nutritional support, and treatment of infections have also played a major role in this achievement.
Table 11.1
Mortality Following Burn Over Time for Different Age Groups, Shown as the Burn Size at Which 50% Live or Die
From Branski LK, Barrow RE, Herndon DN, unpublished data, 1992–2004.
| LA50 (% TBSA) | |||
|---|---|---|---|
| Age (years) | 1942–1952 | 1980–1991 | 1992–2004 |
| 0–14 | 49 | 98 | 99 |
| 15–44 | 46 | 70 | 88 |
| 45–64 | 27 | 46 | 75 |
| >65 | 10 | 19 | 33 |
TBSA, Percentage of total body surface area burned; LA50, lethal burn area for a 50% mortality.
Table 11.2
Pediatric-Specific Mortality Rates Over Time; Near-Total Early Excision Is the Basis of These Excellent Results
| MORTALITY SORTED BY BURN SIZE (% TBSA) | ||||||||
|---|---|---|---|---|---|---|---|---|
| Years | <20% | n | 21%–40% | n | 41%–60% | n | 61%–100% | n |
| 1980–1985 | <0.1% | 889 | 1% | 230 | 8% | 105 | 33% | 95 |
| 1986–1990 | <0.1% | 571 | 1% | 224 | 4% | 117 | 19% | 88 |
| 1991–1995 | <0.1% | 522 | 2% | 192 | 8% | 94 | 20% | 78 |
| 1996–2000 | <0.1% | 635 | 1% | 222 | 3% | 133 | 19% | 114 |
| 2001–2004 | 2% | 83 | 2% | 121 | 26% | 91 | ||
n, Total number of patients admitted with respective burn size in the given period; TBSA, total body surface area.
Mortality and pediatric burn patients, Shriners Burn Institute, Galveston, Texas. Unpublished data, 1980–2004.
Early operative intervention, however, remains the major contributor to this major advance in burn care. In 1974, Burke and colleagues reported on the results of total excision of full-thickness burns where allografts were applied to cover burn wounds after excision.
Improved mortality, shorter hospital length of stay, and fewer metabolic complications were noted when early excision was retrospectively compared with late excision. In another study, 32 children with an average age of 7 years and mean burn size of 65% TBSA who underwent either total excision or serial debridement were studied. Mortality, overall blood loss, and cumulative operating time were equivalent. The early excision group, however, had their length of hospital stay almost halved (97 ± 8 days vs. 57 ± 5 days). Since then, hundreds of children with burns of more than 30% TBSA treated with early excision have demonstrated a hospital length of stay of less than 1 day/% TBSA burned.
Tompkins et al. demonstrated that mortality of adult burn patients at Massachusetts General Hospital improved from 24% in 1974 to 7% in the time period from 1979 to 1984 after implementation of prompt eschar excision and immediate wound closure. This study was later expanded to include 85 patients aged 17 to 55 years. Those patients aged 17 to 30 years without inhalation injury showed significantly reduced mortality of 9% if treated by early excision compared with 45% when treated conservatively.
In children with burn injuries, Xiao-Wu et al. showed that delays in the excision of extensive burn were associated with longer hospitalization, delayed wound closure, increased rates of invasive wound infection, and increased incidence of sepsis.
Munster et al. demonstrated a statistically significant decrease in hospital length of stay correlating with a decrease in the interval between surgical interventions over a 14-year period. Other variables such as burn size, inhalation injury, and age remained unchanged during the same time period; mortality rate decreased significantly.
Elderly burn patients have also been shown to benefit from early excision. Deitch et al. demonstrated that early surgical excision in patients with an average age of 68 led to a 40% reduction in mean hospital length of stay compared with the national average and reduced mortality. Many studies show that early excision can be safely performed in the elderly with clear benefits of reducing hospital length of stay and the number of septic episodes.
Hypertrophic scar formation is common after burn injuries, with more pigmented higher Fitz-Patrick patients more prone to hypertrophic scar development. However, the most important factor in the development of hypertrophic burn scars is delayed wound healing. Deitch et al. demonstrated that in wounds requiring more than 10 days to heal, the risk of hypertrophic scarring is significant and rises to 80% if healing is delayed beyond 21 days. Operative treatment also limits the duration of pain caused by the burn wound.
In conclusion, early burn wound excision is lifesaving, offers improved cosmetic and functional outcomes, and is cost-effective.
Techniques of burn wound excision
Excision of burn wounds is at the core of modern burn care. Different methods of excision and modes of grafting are advocated based on the patient and injury. However, early debridement-based source control, pain mitigation, rapid wound healing of superficial burns, and grafting-based coverage of deep burns are widely accepted as the standard of care. How those are achieved remain an issue of debate and are driven heavily by local resources and community tolerance of patient suffering.
Excision of a small burn
Operative intervention for small burn injuries is an issue of long debate. There is a strong indication for excision of deep partial- and full-thickness burns without delay as they will tend toward significant delay in healing in greater than 3 weeks and hypertrophic scarring. Heimbach et al. noted that deep partial-thickness burns did not convert to full-thickness burns when topical antimicrobials were used to control infection. Although these wounds eventually healed after several weeks, they showed persistent blistering, pruritus, hypertrophic scar formation, and poor functional outcomes. Additionally, considerations of pain, suffering, and posttraumatic stress are not trivial, and management of these outcomes needs to be considered. These observations prompted a prospective trial of early excision and grafting versus nonoperative treatment of indeterminate depth in burns of less than 20% TBSA. Shorter hospitalization, lower cost, and reduced time away from work but greater use of blood products were seen in patients treated with early excision. Those patients treated nonoperatively required more late skin grafting to achieve wound closure and developed more hypertrophic scars. Although the advantages of early excision even for small burns are clear, a balance of patient outcomes including suffering needs to be struck with available healthcare resources.
Tangential excision
Tangential excision, as a technique, is the meticulous removal of burned skin while preserving underlying viable tissue. Body contours are better preserved with tangential excision than with fascial-level excision, which removes underlying subcutaneous fat; hence, it is the standard excision technique for burns.
Tangential excision was originally described by Janzekovic, who observed that deep skin graft donor sites could be grafted with thinner, split-thickness skin grafts taken from another area. Later, she extended this concept to partial-thickness burns by repeatedly excising thin layers of the burned skin until viable tissue was reached ( Fig. 11.3 ). She determined the heterogeneous nature of the burn injury and end point of excision as being punctate bleeding. This end point defined excision beneath the coagulative necrosis. Then, in her model, split-thickness skin grafts were immediately applied.
Schematic representation of tangential excision; sequential slices are taken until punctate hemorrhage is evident.
(From Janzekovic Z. A new concept in the early excision and immediate grafting of burns. J Trauma. 1970;10(12):1103-1108.)
The technique of tangential excision and autografting of partial-thickness burns was a major advance in burn care and remains the gold standard. Before its introduction, only full-thickness burns were excised, including subcutaneous fat and accompanying lymphatics down to the underlying layer of investing fascia ( Fig. 11.4 ). Janzekovic analyzed the results of the use of tangential excision in more than 2000 patients. She found that, compared with fascial excision, hospital length of stay, pain, and reconstructive procedures were decreased.
Fascial-level excision using cutting diathermy and an incorporated smoke evacuator.
Several different instruments can be used to perform tangential excision of the burn wound. Other steel blades such as the Norsen Debrider, Goulian knife, Watson knife, and powered dermatomes have largely supplanted Janzekovic’s original barbers’ razor. Powered surgical excision tools such as the Versajet Hydrosurgery System and the Misonix ultrasonic debrider are used for tangential excision as well ( Fig. 11.5 ). It is critical to understand that all of these are means of excisional preparation of burn wounds in preparation of skin grafting and are standards of care for surgical preparation of a wound bed for skin grafting. It is further critical to accept that additional excision may be needed over time to achieve a final excisional depth both due to clinical markers of excision and evolution of burn wounds over time.
A selection of hand-cutting dermatomes available for use for tangential excision. Most have the ability to set the aperture to the desired depth, whereas the Goulian has a large series of blade-changeable guards.
Enzymatic debridement
Since the last edition of this text, enzymatic debridement has become an increasingly available component of excisional care. For the past several decades, collagenase (Santyl) ointment has been an available topical debriding agent. Over the course of days to weeks it is able to hydrolyze burn eschar and can be an important adjuvant to nonoperative management of burn wounds. However, it is not suited as a component of operative burn wound treatment, particularly in the massively burned patient.
Anacaulase-bcdb (NexoBrid) is a bromelain-based enzymatic debriding agent that has entered practice. It completes the debridement of the wound within 4 to 6 hours depending on the care protocol. It is selective inasmuch as its activity is arrested by viable tissue. It will chemically remove the unviable tissue and accounts for the heterogeneity of burn depth throughout the wound area. Unlike in the setting of tangential excision, this does not require the end point of punctate bleeding or an experienced surgeon. Its use is curtailed by only being able to apply to areas under 20% TBSA and pain that generally requires procedural sedation or anesthesia potentially for several hours. Once the enzyme has completed its action, the digested eschar can be removed, remaining areas of the wound excisionally prepared, and the wound grafted with skin substitute.
Fascial excision
In clearly full-thickness burns, as well as some massive wounds, a fascial-level excision has clear advantages. Skin and subcutaneous tissue are excised en bloc using electrocautery in fascial excision. This involves excision of the full thickness of the integument, including all subcutaneous tissues down to the investing deep fascia. These techniques can also spare some subcutaneous fat, although this can make grafting more challenging. It is usually performed to reduce blood loss in extensive burns or in cases of severe infection to control the source of infection.
Fascial excision can limit the amount of blood loss because control of the deeper perforating vessels is achieved during the excision, bypassing the extensive capillary network present in the skin and subcutaneous tissue. Fascial excision is also required for areas where significant subcutaneous tissue has been involved in the burn injury. The advantages of this technique include speed of excision, improved graft take on fascia, and reduced blood loss.
Fascial excision is also indicated in cases of life-threatening invasive wound infection or sepsis, particularly mold infections such as Aspergillus and Mucor , and in cases of failed graft take in extensive burns in critically ill patients. Episodes of sepsis lead to ischemic necrosis of the subcutaneous fat due to poor peripheral perfusion and microvascular stasis. This represents a considerable problem in patients with extensive burns leading to late graft loss, and the ischemic areas are transformed into portals for invasive wound infection. The disadvantages of fascial excision are lymphedema due to the interruption of the subcutaneous lymphatics, difficulty with temperature regulation, poor scar pliability, and contour deformities due to the loss of subcutaneous fat. In the setting of massive burn wounds, a balance must be struck by an experienced surgeon between fascial and tangential excision. Regardless, the primacy of excisional care as the cornerstone of burn treatment is a clear standard of care.
Controlling blood loss during burn excision
Blood loss and acute blood loss anemia are an anticipated parts of burn excision given the end point of excision is bleeding. Large burns can result in considerable, even massive, blood loss. Sections in the critical care, anesthesia, and hematology chapters are dedicated to management of this anticipated challenge. Tangential excision can lead to large blood loss even with measures taken to limit hemorrhage.
The simplest measure is to operate within 24 hours of the burn injury. Vasoactive metabolites, particularly the potent vasoconstrictor thromboxane, are in abundance during this time to limit blood loss. This vasoconstriction abates by 48 to 72 hours postburn. Desai et al. demonstrated in a prospective trial of 318 pediatric patients with burns of more than 30% TBSA that early excision of burns is associated with an overall reduction in blood loss. The average blood loss per surface area excised (mL/cm ) was compared at various postburn excision time points. The total blood loss during excision performed within the first 24 hours after burn was 0.4 mL/cm 2 excised, compared with 0.75 mL/cm 2 excised if performed between days 2 and 16 postburn. The blood loss dropped to 0.49 mL/cm 2 excised if the procedure was performed after the 16th day. Overall mortality was 5% for an average burn size of 60% TBSA in the cohort. Early excision had no adverse effect on mortality. Very early excision led to a halving of blood loss for both large and small burns , ( Fig. 11.6 ).
Blood loss is almost halved by operating within 24 hours of injury.
(From Desai MH, Herndon DN, Broemeling L, Barrow RE, Nichols RJ Jr, Rutan RL. Early burn wound excision significantly reduces blood loss. Ann Surg. 1990;211(6):753-762.)
Other factors associated with increased blood loss during excision of burns are old age, male sex, larger body size, large full-thickness burns, high wound bacterial count, total area excised, and operative time.
Several drugs can limit blood loss. The homology chapter describes optimization of the coagulation cascade with blood products and factor administration, as well as the value of tranexamic acid. Tumescent infiltration with epinephrine solutions and topical application of epinephrine 1 mg/L are typical to encourage vasoconstriction. Some centers advocate up to 30 mg epinephrine per liter topically. Topical thrombin, fibrin sealant, and autologous platelet gel encourage clot formation. Immediate pressure bandaging reduces small-vessel bleeding and can allow time for coagulation to occur. These pressure wraps can be used in conjunction with topical silica such as NuStat, or cellulose-based compounds like BloodSTOP encourage clot formation and stabilization and are all critical adjuncts to reducing blood loss and enhancing graft take.
The application of tourniquets to the extremities is a very effective method of minimizing blood loss, especially for excision of burns involving hands and digits. As with tumescent infiltration, the absence of bleeding can make the estimation of the right depth of excision difficult. To counteract this, the tourniquet can be released briefly to check the adequacy of excision and then reinflated. The larger vessels are controlled by electrocautery or ligation; the wound is covered with topical hemostatic agents; and pressure is applied to allow time for the blood to be static at the wound interface on reperfusion. After the release of the tourniquet, the limb should be elevated for about 10 minutes before graft application. Alternatively, the grafts can be applied before reperfusion and secured with fibrin glue and a pressure dressing. The pressure dressing can be removed after 10 minutes of hemostatic time, and the wounds will often be hemostatic with good graft adherence. It should be noted that the longer the tourniquet is inflated, the greater the reperfusion bleeding and risk of compromising graft take.
Tumescent solution made of epinephrine containing saline can be injected into the burn wound before excision. This technique is particularly useful for burn excision of areas such as the trunk, scalp, and face; 1 to 4 mg of 1:1000 epinephrine is added to 1 L of lactated Ringer’s solution. The resulting local vasoconstriction will minimize blood loss, and one-way syringes, such as the Multi-Ad Fluid Dispensing System or a pneumatic infuser, can make the injection process easier ( Fig. 11.7 ).
An infuser device.
Assiduous monitoring of the patient’s hemodynamics by a skilled anesthesiologist is critical because epinephrine may cause tachycardia and hypertension, which can worsen bleeding. Another drawback of this technique is that the lack of bleeding from the wound bed may make the adequacy of excision difficult to assess.
Delayed definitive grafting after excision is used in many centers to limit blood loss. In case of delayed skin grafting, the wound bed needs to be kept moist and clean before skin grafting. The wound is temporarily grafted with homograft for 24 to 72 hours to allow hemostasis to be achieved fully, and the patient needs to be hemodynamically resuscitated before the additional insult of donor site harvest. This maintains a moist healthy wound bed, minimizes bacterial colonization, and encourages hemostasis. Early removal of the homograft, before full-density inosculation, prevents neovascularization of the homograft with resultant hemorrhage while allowing a second look for definitive excision before final grafting. We adhere to a hemoglobin threshold of 7 g/dL for transfusion. One study suggested a possible decrease in infection rate when compared with a more liberal transfusion strategy. Many centers will transfuse to 9 to 10 g/dL before surgery to allow a greater buffer before the onset of shock if large blood loss is anticipated.
Wound closure
Once the wound is excised, closing the wounds is the next challenge. Some centers advocate an immediate application of autograft with the notion of using every donor every time. This has been advocated for rapid closure of wounds and the philosophy that the wound has the least bacterial load immediately after excision. Other surgeons, chaper author included, advocate a more nuanced approach wherein skin substitutes are used to temporize wounds. In doing so, autograft take is generally superior with fewer wasted donors or grafting of wounds that would heal with time. ,
Skin substitutes
Skin substitutes are used to temporarily serve the protective purpose of the skin. For a more comprehensive discussion, please refer to the chapter on skin substitutes. These protective purposes include reduction of fluid loss, bleeding, pain, and bacterial burden. They can also encourage neovascularization and formation of a neodermis for the purpose of improved wound healing, graft take, and improved scarring. Over the decades there has been a proliferation of bioengineered material that achieves these goals. Thus the literature has developed a new all-encompassing term of cellular and acellular matrix-like products (CAMPs). These refer to products used on wounds that have biological effects including wound integration. This category includes traditionally defined skin substitutes. For the purposes of medical coding in ICD-10 and CPT8, burn surgeons must be able to define the products they use as skin substitutes based upon the intended use for their biological effect rather than constraining to rigid definitions espoused by third-party payers.
These CAMPs are divided into two major categories: minimally modified skin/epithelial products and bioengineered tissue matrixes. A reasonable case can be made to include certain advanced dressings within this category, with the goal being a wound-modulating effect over a simple wound dressing.
The most used minimally modified skin/epidermal product is cryopreserved cadaveric skin allograft, also known as homograft. Homograft remains an effective temporary burn wound coverage after excision if autograft skin is not available, or to temporize the wound and allow neovascularization in anticipation of autografting and to encourage the healing of partial-thickness burns. Homograft can be stored in a cryopreserved state for years, then be thawed and become adherent and vascularized when applied to a viable wound bed. This process can also serve as a test for wound-bed viability after burn excision, with immune rejection occurring 3 to 4 weeks after application. Homograft has the advantage of being inexpensive relative to most of the tissue-engineered CAMPs. In fact, it has a cost structure within the range of advanced dressings while providing excellent, time-tested biological advantages. Thus it is a critical component of the standard of burn care and the cornerstone of our care pathway.
When homografts are used as a temporary coverage for the face and genitals, they should be applied as sheet grafts. This prevents the formation of granulation tissue between the interstices, which can cause scarring and poor cosmetic outcome after secondary autografting. In our practice we prefer amniotic membrane for the face and genitals except in the rare setting of a fascial excision. Amniotic membrane is available either dehydrated or cryopreserved and has extensive antiinflammatory properties. This membrane can effectively allow reepithelialization with minimal scarring. Also, relative to homografts they do not cause engraftment with the long-term need for grafting in deep partial-thickness burns, which can have dysesthetic outcomes. Despite not reducing healing time or scarring, it provides some of the benefits of wound coverage and reduces the number of dressing changes required until healing is achieved.
Xenografts are another option for temporary wound coverage. Glycerol-preserved porcine xenograft skin is currently available for clinical use. Their main application is on partial-thickness burns after superficial debridement, as well as on donor sites. As with allografts, xenografts become adherent and provide the benefits of temporary wound coverage, such as pain control, while the underlying wound re-epithelializes, but the xenograft does not vascularize. Additionally, it is associated with worse scarring. Fish skin–based xenografts are indicated for partial-thickness burns. They have become increasingly available and marketed over the past several years, including directly to patients in social media campaigns. These xenografts are more than an order of magnitude more costly than homograft and similarly priced as amniotic membranes with no convincing advantages.
For purely superficial partial-thickness burns, there are also fully synthetic skin substitutes such as poly-lactic acid (SupraThel), Biobrane, and PermeaDerm. These CAMPs exist on a continuum between skin substitutes and dressings. At the time of the first wound treatment, all loose skin, blisters, and necrotic dermis is sharply excisionally debrided to leave a clean, moist surface. SupraThel is a bioabsorbable poly-lactic acid that maintains a moist wound environment encouraging epithelial spread, excludes bacteria, and maintains an antimicrobial acidic environment. (CITE) Biobrane is a useful dressing for smaller and more superficial wounds. Biobrane is a nylon/silicone bilaminated composite skin substitute that becomes adherent to the exposed dermis, thereby acting as a neoepidermis. Lal et al. reported no increase in infection rates using Biobrane. Infections occur rarely because of nonadherence and accumulation of fluid. Other alternatives include the use of silver-impregnated dressings with nonadherent silicone layers such as Mepilex, which provide a moist wound-healing environment and suppress bacterial growth.
The flexibility, elasticity, and strength of normal skin are provided mainly by the dermis. Excision of full-thickness burn removes the entire dermis, thus the elasticity, strength, and vascular properties of the skin are lost. Reestablishing this dermal function is the goal of a wide range of CAMPs. Originally, cadaveric homograft left to engraft in the immunosuppressed state of the massive burn filled this role, although it is associated with significant scarring. Over the past decades a number of bioengineered CAMPs have entered the market to fill these roles, ranging from minimally modified biological products to partial or full synthetics. The use of dermal replacements in the treatment of burns can provide the highly desired characteristics of normal dermis.
The first dermal replacement skin substitute to gain wide acceptance was Integra. Integra is a dermal substitute composed of a porous matrix of cross-linked bovine collagen and glucosaminoglycans providing a scaffold for cellular invasion and capillary growth. It is applied to the wound bed after burn excision, and the matrix is fully incorporated into the wound bed in 2 to 3 weeks; then, thin split-thickness autograft skin is applied. Except for a possible increased risk of infections, the use of Integra is safe and effective. Skin graft take is usually aided by the use of negative-pressure wound therapy (NPWT) ( Fig. 11.8 ).
A–C, Deep flame burn on a boy’s chest treated with early excision and Integra with vacuum-assisted closure. (D) The silicone layer being removed on day 12 ready for thin grafting with well-vascularized dermal template underneath. (E) The pleasing final result.