Introduction
The type of reconstruction used for partial mastectomy defects depends on (1) the size of the resection, (2) the size of the breast, and (3) the location of the tumor. Tumor location on the breast and relative to the nipple–areolar complex is critically important. A recent study of 350 patients demonstrated that the maximal volume of tissue resected with lumpectomy without resulting in unacceptable aesthetic and functional outcomes of decreased quality of life were 18–19% in the upper-outer quadrant, 14–15% in the lower quadrant, 8–9% in the upper-inner quadrant, and 9–10% in the lower inner quadrant. Tumor location not only can predict the potential for a cosmetic deformity, but it also can help determine the type of reconstruction required to fill the partial mastectomy defect. Women with smaller breasts are more often amenable to flap type volume replacement reconstructions, whereas women with larger or more ptotic breasts are better candidates for volume displacement techniques. Adhering to strict algorithms is difficult because every case is different. Being familiar with the various reconstructive tools will allow reconstruction of almost any partial mastectomy defect. The oncoplastic reduction and mastopexy techniques can reconstruct a tumor in any location. Although principles are essentially the same for any breast defect, the type of pedicle and type of skin pattern might differ depending on the tumor location. Flaps can also reach any tumor location; however, some flaps are better suited for certain locations than others.
Problem Areas in Oncoplastic Reconstruction
Partial reconstruction works well in lower quadrants of the breast. These areas are adjacent to suitable volumes of breast parenchyma that can be transposed or rotated into a nearby defect. The upper and superomedial quadrants of the breast are relatively volume deficient and are often not close to suitable pedicles that may be used as volume fillers. The supra-areolar area from the upper anterior axillary fold laterally across to the manubriosternal junction medially is often challenging to reconstruct. This area often requires local flaps or autoaugmentation techniques to fill the defects. Central defects can also be challenging because they potentially interfere with blood supply to the nipple–areolar complex and, when not filled appropriately, will lead to nipple retraction and resultant deformity. It is important to keep in mind that when the defect is extensive with little remaining breast tissue, completion mastectomy and immediate reconstruction is often the more appropriate option.
- 1.
Volume Displacement Techniques
Breast-reshaping procedures all essentially rely on advancement, rotation, or transposition of an area of the breast to fill a small- or moderate-sized defect. This absorbs the volume loss into a smaller breast. In its simplest form, it entails mobilizing the breastplate from the area immediately around the defect in a breast flap advancement technique. These procedures are indicated in women with small- to medium-sized breasts where the resection does not lead to any significant volume alteration that might cause breast asymmetry. A contralateral symmetry procedure is typically not required.
Perhaps the most popular and versatile breast-reshaping options are the mastopexy or reduction techniques. The ideal patient is one where the tumor can be excised within the expected breast reduction specimen in medium to large or ptotic breasts where sufficient breast parenchyma remains following resection to reshape the mound. This means that any tumor location within the standard Wise pattern resection tissue is ideal for this approach. Kronowitz et al describe seven areas or zones of the breast that can be used to determine pedicle location. The most difficult locations to treat are superomedial areas, where lack of adjacent breast volume tends to limit reconstructive options; women with large lower poles and cleavage are easier to manage in this area. High upper pole tumors can also be problematic unless a flap of breast tissue can be incorporated into an inferior pedicle as a pennant flap rotated up into the defect from below.
Lower quadrant tumors in women with larger breasts are ideally suited for the oncoplastic approach. Some of the original descriptions of oncoplastic reduction techniques were in tumors located inferiorly. Quadrantectomy type resections are possible, removing skin and parenchyma from this location, reshaping the breast using a superior or superomedial pedicle ( Fig. 16.4 ). Inferior and midline tumors can be reconstructed using the vertical pattern in smaller- to moderate-sized breasts. A superiorly based pedicle can be used to reposition the nipple, and this then results in a very familiar defect because it is the location where tissue is resected in a vertical pattern breast reduction or mastopexy. The medial and lateral pillars are then plicated to fill the defect and lift the breast with a similar pattern being performed on the other side. The breast surgeon will often have the luxury of removing skin along with the tumor resection if this falls within the proposed preoperative markings ( Fig. 16.1 ).
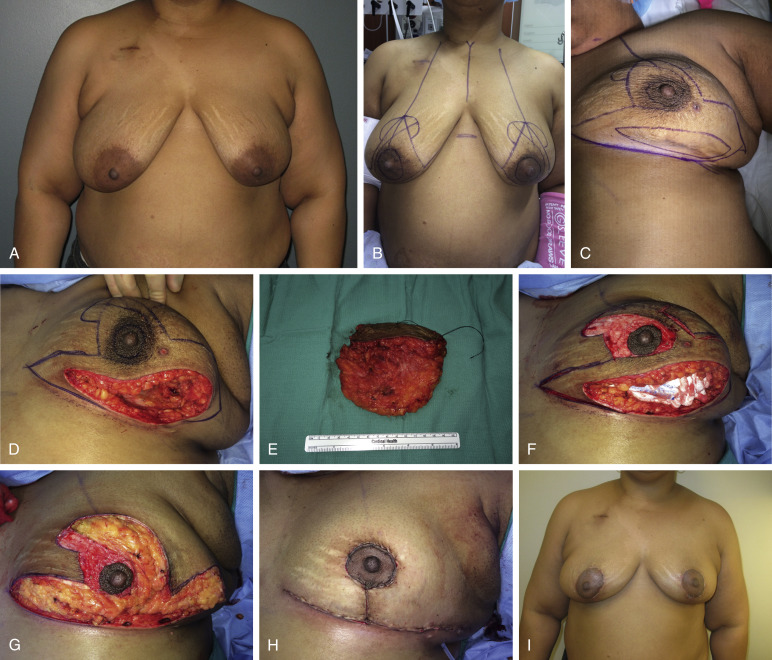
If the inverted T or Wise pattern reduction or mastopexy is planned, the technique is similar. Resection is performed either with or without skin within the Wise pattern markings. The nipple is then moved up on a superiorly based pedicle, and the remaining dermatoglandular tissue is resected from around the lower pole, and the oncoplastic reduction is completed. If additional tissue is resected from around the tumor defect, it is important to mark the specimen because this will then become the new margin. If significant ptosis exists, and the tumor is inferior and a superiorly based pedicle is not possible, then this becomes more challenging. Autoaugmentation techniques are often not required for central lower pole defects because the nature of these techniques will often have sufficient remaining breast tissue to fall into place filling the defect without having to rearrange parenchyma.
Inferolateral tumors are best closed with a superomedial pedicle incorporating an accessory flap of inferior central tissue to rotate into the lateral defect if indicated. If a superiorly based pedicle is not possible due to significant ptosis, then an inferior or centrally based pedicle can be used and shifted medially to enhance perfusion to the nipple. True inferolateral defects often do not require autoaugmentation techniques, but when they do, extended superomedial pedicles can be used to rotate and fill an area of volume void when indicated. The nipple pedicle is extended and the glandular tissue is de-epithelialized and rotated laterally.
Inferomedial tumors are also often very amenable to superior or superomedial pedicles. The defect will often lie in the Wise pattern markings, and completing the reduction will reshape the breast mound. If an inferior pedicle is needed, it can also be shifted laterally and used to move the nipple and fill the defect. Autoaugmentation techniques are similarly not often needed but can be performed using an extended superolateral pedicle if indicated.
Upper quadrant tumors result in defects that can be more challenging to reconstruct. These defects are outside the Wise pattern markings, which makes skin and parenchyma removal difficult. The vast majority will be lumpectomy type defects and are often best filled with an inferior or central pedicle ( Fig. 16.2 , upper). When sufficient glandular tissue remains above the nipple–areolar complex on an inferior pedicle, this can be used to fill the central upper defects. If not, it will be important to mobilize some upper pole tissue to fill the defect and provide upper pole fullness. The higher the tumor on the chest wall and the thinner the patient, the more difficult this becomes. If there is a paucity of available tissue, glandular “wings” of parenchyma from the lateral and medial upper quadrants can be mobilized to help close the defect. This is often not possible, and subsequently autoaugmentation techniques are used to fill the dead-space and maintain shape. Extended superomedial pedicles in women with medium-sized and ptotic breasts and upper or upper-outer quadrant defects will often provide good reconstruction. A vertical reduction technique is performed creating medial and lateral pillars. The lower pole breast tissue is kept as an extension of the superomedial pedicle and transferred to fill the upper or outer quadrant defect. The breast is then shaped by closing the pillars inferiorly. A similar technique can be performed for upper-inner quadrant defects using an extended superolateral pedicle.
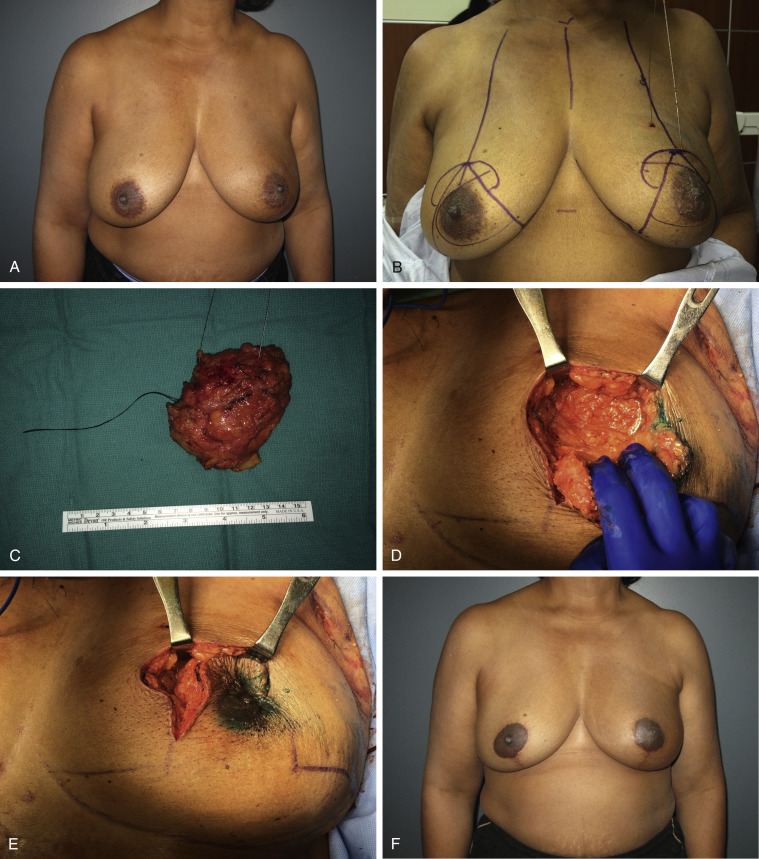
These upper-outer quadrant defects in women with large breasts who undergo a Wise pattern reduction can also be filled using the secondary dermatoglandular pedicle. If a superomedial pedicle is used to reposition the nipple, and volume is needed to fill an upper-outer defect, then a secondary inferolateral pedicle can be created to fill the defect. The pedicle is fashioned to fit the defect and made smaller or larger depending on the demands. This is often safer than extending the primary pedicle as it preserves better perfused dermatoglandular tissue with less risk of fat necrosis.
Larger quadrantectomy defects, especially above the nipple, can be incorporated into a batwing mastopexy or elliptical-type incision and provide preservation or improvement of shape and elevation of the ptotic breast along with the tumor resection. A similar mirror image resection is often performed on the opposite side for symmetry. Additional mastopexy options exist for oncoplastic breast conservation. The donut mastopexy allows a breast segment to be removed through a periareolar incision and is useful for segmentally distributed cancers in the upper or lateral portion of the breast. The batwing mastopexy involves a full thickness excision of lesions deep within the breast centrally or adjacent to the nipple–areolar complex. The two similar half-circle incisions with angled wings on either side of the areolar allow advancement of the fibroglandular tissue to close the defect. Because this removes sufficient breast tissue and skin to alter the size of the breast and nipple position, a similar contralateral lift is occasionally required to achieve symmetry. Additionally, if the patient is a candidate for breast conservation therapy (BCT) and has multiple areas that need to be resected, as long as sufficient tissue remains, remodeling techniques can be used in a similar fashion.
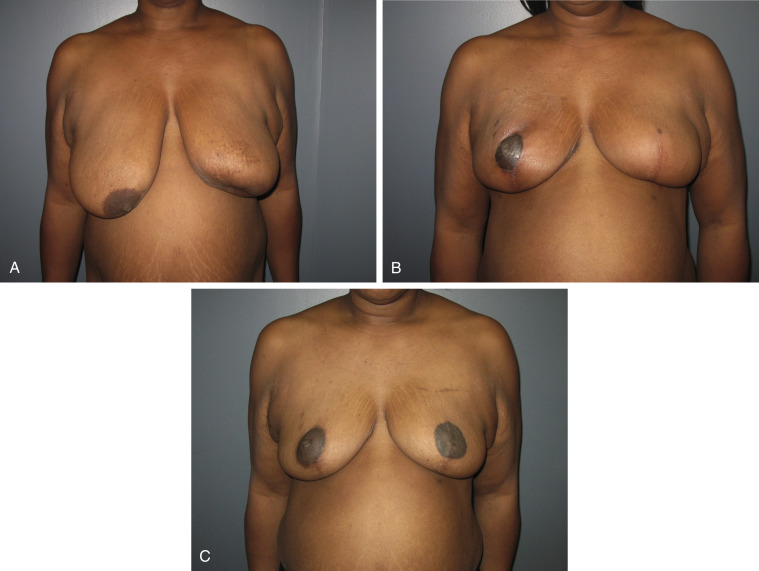
Central tumors have in the past been considered relative contraindications to BCT; however, with the oncoplastic approach in women with macromastia, the tumor and nipple–areolar complex can be widely excised and reconstructed using a variety of techniques. The mound can be remodeled in the inverted T-closure pattern, similar to breast amputation reduction techniques. The nipple is then reconstructed later using the reconstruction technique of choice ( Fig. 16.3 ). Another option if the tumor is located more superiorly or lateral is to perform a central elliptical excision of skin, nipple, and parenchyma, and mirror image contralateral reduction for symmetry. A third option includes creation of a skin island on a dermatoglandular pedicle to rotate into the central defect to allow for shape preservation and nipple reconstruction ( Fig. 16.7 ). The breast is marked preoperatively for an inverted T or a vertical approach depending on breast size, and the skin island is brought in from inferior or medial ( Fig. 16.4 ).