Introduction
The massive burn is as much a metabolic insult as it is a tissue injury. In the acute phase of burn care, a persistent, overwhelming metabolic response to thermal injury compromises the functional integrity of virtually every organ system. This response compromises wound healing capacity and negatively impacts the body’s defense mechanisms.
Large thermal injury represents a metabolic “double hit,” a nutritional challenge of both supply and demand for the injured patient. The burn wound creates drastically increased demand for anabolic metabolism for wound healing while simultaneously triggering a systemic catabolic state. The resulting mismatch between high anabolic demand and negative anabolic supply (catabolism) leads to a state of functional malnutrition which, in turn, facilitates rapid debilitation and immunosuppression that places patients at increased risk for infectious complications. Addressing these nutritional challenges is thus critical to effective care for the burn patient.
Metabolic pathology associated with burn injury
After all forms of major trauma, inflammatory and hormonal responses are activated and greatly influence metabolic pathways and mechanisms. Nutrient intake, absorption, and substrate assimilation are all affected during different stages of the stress response. Nutrient requirements increase and become more difficult to predict, and enteral or parenteral feeding is often necessary to meet vastly increased nutritional requirements.
The physiologic response to trauma leads to activation of an array of processes, many of which increase immediate energy availability as part of the fight-or-flight response. It is an evolved response to stress that assists the organism in overcoming a transient stress. However, there is no adaptive response to the kind of sustained stress state seen with massive burns because such injuries were not survivable before the development of modern medicine. By supporting patients through what would otherwise be a nonsurvivable condition, modern medical care has created a novel physiologic state characterized by a prolonged period of active injury for which there is no adapted evolutionary response. In this state, adaptive responses to immediate stress become maladaptive when sustained over a timeline well beyond those encountered in the evolutionary context ( Fig. 22.1 ).
Metabolic response to injury and trauma. Burn patients transition from the initial hypermetabolic response directly into a state of chronic hypermetabolism. (A) Classic ebb and flow phases of the acute stress response. The metabolic rate initially falls below normal and then increases to supranormal levels before returning to normal. (B) Ebb and flow revisited. In burn patients, the classic ebb-and-flow pattern is altered. Recurrent bouts of sepsis superimposed over a baseline of burn-induced proinflammatory stimuli result in a fluctuating metabolic demand, which remains chronically elevated.
(From Ball S, Baudouin SV. Endocrine disorders in the critically ill: The endocrine response to critical illness. In: Hall GM, Hunter JM, Cooper MS, eds. Core Topics in Endocrinology in Anaesthesia and Critical Care . Cambridge: Cambridge University Press; 2010:126-131.)
The hypermetabolic response to stress is particularly exaggerated in thermal injuries. The severity of the catabolic response to burn injury cannot be overemphasized. Decades of clinical and animal research have demonstrated with increasing depth and detail the ways in which burn injury alters the host organism’s metabolism to upregulate catabolic processes and inhibit anabolic processes. The net result is a substantial loss of lean body weight with an exaggerated impact on protein stores The pathophysiology of this protein wasting involves a wide array of endocrine and metabolic factors from the cellular to the organismal level.
Adrenal hyperactivity in burn patients was well documented more than 50 years ago, with massive surges in serum and urinary catecholamine levels evident within hours of injury. Inappropriate catecholamine and cortisol production has since been found to persist for weeks to months after burn injury, with end organ effects reaching the metabolic, cardiovascular, musculoskeletal, and immune systems ( Fig. 22.2 ). A sustained surge of catecholamines and inflammatory cytokines, along with massive wounds and dysregulation of thermal homeostasis, all combine and interact to yield marked increases in resting energy expenditure.
Thermal injury induces a distinctly profound metabolic shift toward proteolysis.
(From Long CL, Blakemore WS. Energy and protein requirements in the hospitalized patient. JPEN J Parenter Enteral Nutr . 1979;3(2):69-71.)
Distorted thermal regulation plays a substantial role in the increase of resting energy expenditures seen in burn patients. Destruction of a large portion of the primary thermoregulatory organ, the skin, leads to a persistent drain of body heat via decreased insulation and increased heat loss. The primary, central hyperthermia associated with the burn response compounds this energy drain. Alterations in the thalamic temperature set-point, catecholamine-induced hypermetabolism, and shunting of mitochondrial energy to heat-producing pathways all drive the hyperthermia seen within 24 hours of burn injury. As Wilmore et al. described in 1974, “Burn patients are internally warm, not [just] externally cold.” Thus the burn patient’s metabolism is taxed with the challenge of generating sufficient heat to maintain a higher body temperature with less heat-conserving resources.
Nutritional demand and substrate metabolism in burn patients
Increased total caloric demand
Thermal injury triggers a marked increase in global energy expenditure, driven by a maelstrom of catecholamines, corticosteroids, and inflammatory cytokines. , In an earlier era of burn care—before the advent of early excision, pharmacologic interventions for hypermetabolism, and modern critical care—measurements of energy expenditure in patients with large burns were reported to range from 1.5 to 2.5 times those found in nonburn controls. Although modern burn care has made significant progress in countering this hypermetabolic response, contemporary studies still report an average resting energy expenditure from 1.3 to 1.5 times those found in nonburn controls.
Substrate-specific requirements
See Fig. 22.3 for a simplified overview of the metabolic pathways involved in the systemic response to massive thermal trauma.
Simplified overview of metabolic pathways.
ATP , Adenosine triphosphate; CoA , coenzyme A; OAA , oxaloacetic acid; TCA , tricarboxylic acid.
Carbohydrates
The acute metabolic response to burn injury significantly alters carbohydrate metabolism and demands. Glucose/carbohydrate metabolism presents the burn physician with a rather vexing conundrum. On the one hand, failure to provide adequate carbohydrates results in additional compensatory protein catabolism. , On the other hand, the human body has a finite capacity for glucose oxidation. Multiple studies have demonstrated a limit to the amount of carbohydrate calories a burn patient can assimilate—approximately 5 g/kg per day in adults and 7 g/kg per day in children. , Providing glucose in excess of these limits will result in increasing hyperglycemia with resultant lactic acidosis ( Fig. 22.4 ).
Oxidative decarboxylation of pyruvate is a pivotal step in the overall oxidative metabolism of carbohydrates and fats. Overwhelmingly high levels of glucose may lead to lactate production, even in the presence of oxygen.
CoA , Coenzyme A; NAD + , nicotinamide adenine dinucleotide; NADH , nicotinamide adenine dinucleotide plus hydrogen.
(From Gore DC, Ferrando A, Barnett J, et al. Influence of glucose kinetics on plasma lactate concentration and energy expenditure in severely burned patients. J Trauma. 2000;49:673-677.)
Current guidelines typically recommend providing 50% to 60% of calories as carbohydrates in the setting of trauma or burn injury. However, as previously mentioned, large thermal injury induces massive global energy expenditure. Therefore providing 50% to 60% of calories as carbohydrates in the context of a nutritional therapy that meets the patient’s required caloric needs often results in doses of carbohydrates well in excess of the recommended limits. , , , Administration of carbohydrates in excess of the patient’s capacity for glucose oxidation only results in increasing degrees of hyperglycemia, glucosuria, and hypertriglyceridemia. In such cases the patient’s nutritional demands simply reach a point where they exceed that patient’s metabolic capacity.
There is no simple, clinically vetted solution to this challenge. A reasonable approach to this dilemma is to start by titrating enteral formula delivery up to a rate that delivers 5 to 7 g/kg per day of carbohydrates and then provide all further calories in the form of protein supplementation. Unfortunately, this typically results in a protein load that (also) exceeds the body’s capacity for metabolizing.
Fats
Although lipids are critical to effective homeostasis and wound healing, the amount of fat required to prevent essential fatty acid deficiency is remarkably small in patients with intact fat stores. Excess fat administration, on the other hand, can cause significant harm. The hypermetabolic response to thermal trauma upregulates lipolysis of circulating lipids. This surfeit of circulating free fatty acids is countered by increased hepatic esterification, with close to 70% of the free fatty acids accumulating in the liver. To minimize hepatic steatosis, the percentage of dietary calories from fat should be limited and carefully monitored. Multiple studies have demonstrated improved outcomes with lower-fat nutrition therapy in burn patients. Fat content should comprise 3% to 15% of total calories. Patients receiving total parenteral nutrition (TPN) for a short period of time (e.g., less than 10–14 days) can generally be spared lipid infusion. In those requiring sustained TPN, 0.5 to 1 g/kg given one to two times per week is sufficient. It should be noted that nondietary fat calories need to be taken into consideration as well (the fat content of a 1% propofol solution is equivalent to that found in a 10% intralipid emulsion).
It should also be noted that the preceding discussion of the role of fat alimentation in nutritional therapy reflects literature that largely predates the application of alternative fat sources (e.g., fish oil, olive oil, borage oil, etc.). In the United States, the current standard of care for both enteral and parenteral fat administration features significant components of fats that have been shown to affect inflammation. Omega-3 fatty acids are perhaps the most well-known antiinflammatory fats. , One 2018 study of 92 patients with large thermal injury found significant decreases in rates of sepsis, septic shock, and pyloric dysfunction in patients receiving omega-3 supplementation versus those who were not. A 2022 meta-analysis, however, found no benefit to omega-3 supplementation in burn patients with regard to ventilator days, length of stay, mortality, gastrointestinal complications, or infectious complications. Current research also is undecided on the role of omega-6 fatty acids. Some studies have shown that increased intake of omega-6 or precursors (arachidonic acid or linoleic acid) does not lead to an increase in inflammatory markers. , Other studies have shown that increased intake of omega-6 may inhibit the antiinflammatory effects of omega-3 fatty acids, thereby indirectly contributing to more inflammation. Taken together, these studies illustrate a need for further investigation to fully elucidate the role and interactions between fatty acids and their derivatives and inflammation. ,
Alternative fat sources have become the standard of care in Europe where intravenous fat emulsions (IVFE) have been used for over a decade. The United States has lagged behind its European counterparts but has begun to approve more and more of these formulas. Omegaven (Fresenius Kabi), SMOFlipid (Fresenius Kabi), and Clinolipid (Baxter) are three of the most recently approved IVFEs. However, more often than not, these supplements continue to be nonformulary, and they can be difficult to obtain. Although there are still insufficient data to declare these alternatives superior to the standard of care, the threshold for warranting further study has certainly been met. , As our understanding of the unique advantages and disadvantages of different fat sources matures, a reexamination of the role of fat alimentation in burn nutrition is sure to come due.
Protein
Proteolysis is the metabolic hallmark of the hypermetabolic response to thermal injury. As much as 150 g of skeletal muscle are lost per day in the absence of adequate nutritional support. If not attenuated, ongoing systemic proteolysis leads to immune dysfunction and retarded wound healing. Protein requirements of 1.5 to 2 g/kg per day in burned adults and 2.5 to 4 g/kg per day in burned children are well accepted in clinical practice. However, there are limits to the rate of effective protein assimilation. Increasing protein intake above these values can result in increased urea load and azotemia despite limited additional impact on muscle wasting.
The amino acids alanine, arginine, and glutamine play key roles in wound healing in burn patients. Glutamine plays an important role in the function of enterocytes and lymphocytes, and low plasma glutamine concentrations have been associated with increased bowel permeability and increased rates of infection. Studies in animal models of trauma and shock have shown distinct roles for these particular amino acids in recovering enteral and immunologic competence. Glutamine supplementation and other “immunonutrition” formulas featuring these key amino acids have been associated with decreased incidence of infection, shorter hospital stays, and decreased mortality in the setting of traumatic injury and sepsis. Furthermore, it has been shown that early administration of glutamine is particularly beneficial to burn patients in protecting against organ damage and minimizing the hypermetabolic response. Although the benefits of glutamine supplementation were shown in some smaller trials, more recent large-scale trials have called these conclusions into question. The Reducing Deaths caused by Oxidative Stress (REDOXS) study randomly assigned 1223 critically ill ICU patients on mechanical ventilation with multiorgan failure to receive supplements of glutamine, antioxidants, both, or placebo. The primary outcome measure of 28-day mortality was found to trend higher in the glutamine supplementation groups (32.4% vs 27.2%; P =.05). Furthermore, secondary outcome measures of in-hospital mortality and mortality at 6 months were significantly higher in the glutamine supplementation groups.
Until recently, it was thought that burn patients might show a benefit from glutamine that other critically ill patients do not. In response to this question, The Randomized Trial of Enteral Glutamine for the Treatment of Burn Injuries (RE-ENERGIZE) enrolled 1209 patients with severe burns (mean total body surface area [TBSA] 33%) and randomly assigned patients to receive 0.5 g/kg per day enteral glutamine or placebo. Recently published results did not show any difference in the glutamine supplementation group on the primary outcome measure of time to discharge alive from the hospital or mortality at 6 months . (See further discussion in the section on formulas.)
Nutritional support
In the face of the metabolic storm associated with acute burn injuries, provision of effective nutritional support is critical to wound healing, avoidance of complications, and, ultimately, survival. Failure to provide sufficient calories superimposes starvation over a state of hypercatabolism, resulting in devastating losses of lean body mass. Furthermore, there is significant depletion of the protein-energy pool available to meet the pressing needs of wound healing, mucosal integrity, and basic immunologic defenses ( Fig. 22.5 ).
Schematic representation of thermal injury-induced shifts in substrate metabolism.
Enteral nutrition
Benefits of enteral nutrition
In addition to serving as a means for systemic delivery of nutrients, enteral nutrition (EN) performs a critical function in supporting the alimentary tract itself. Enteral feeds provide direct high-concentration nutrients (e.g., glutamine, alanine), stimulate enteric blood flow, maintain barrier function by preserving tight-junction integrity, and induce production and release of mucosal immunoglobulin and critical endogenous growth factors. These functions are not replaced with parenteral nutrition (PN). After dietary ingestion, polysaccharides such as fiber and starch undergo bacterial fermentation in the colonic lumen. Bacterial fermentation provides two functions crucial to intestinal health: (1) it supports the normal flora of the gut lumen, which in turn prevents colonization and subsequent infection (e.g., Clostridium difficile ) and (2) it produces acetoacetate, propionate, and butyrate (a short-chain fatty acid). Butyrate appears to be the preferred fuel of colonic mucosa cells and is therefore essential for mucosal integrity. Both animal and human studies show that the presence of enteral feeds (in addition to or in place of PN) is associated with increased mucosal mass, mucosal oxygenation, brush-border enzyme synthesis, and villous height when compared with PN alone. , Enteral feeding also has frequently been found to improve clinical outcomes both in terms of gastrointestinal and total patient morbidity and mortality. ,
Initiation of feeds
Early initiation.
Current data support the safety and benefit of initiating EN early in the context of traumatic injury and, specifically, of burns. , In both clinical and animal studies of thermal injury and shock, early EN has consistently been shown to result in improved survival and function of the enteric mucosa as well as decreased bacterial translocation. Perhaps most importantly, early enteral feeding represents one of the most effective means of metabolic modulation in thermal injury. Studies have shown a significant blunting of the catabolic response to thermal injury associated with early feeding protocols.
Full feeds should not be delivered in the setting of marked hemodynamic instability and/or high-dose vasopressor requirements because they run the risk of inducing or exacerbating nonobstructive mesenteric ischemia. However, complete EN can be delivered safely to patients on low to moderate doses of vasopressors with stable or decreasing vasopressor requirements. , ,
In patients without hemodynamic compromise, feeding should be initiated rapidly. Although traditional practice has been to gradually titrate up enteric feeds to a goal rate over time, some literature suggests that a more aggressive approach may be warranted. Pilot studies have shown that restarting feeds immediately and at full goal postoperatively (rather than titrating) is well tolerated in burn patients undergoing excision and grafting. Furthermore, the approach of gradually restarting feeds results in significant calorie deficits accumulating over the course of care. One caveat may be patients still requiring formal resuscitation. One study found that initiation of tube feeds within 4 hours of admission to the burn ICU and acceleration to goal tube feeds within 8 hours lead to higher rates of gastric ileus compared with a more gradual titration group. However, there was no difference in clinical outcomes between groups. Early initiation of tube feeds and aggressive titration to goal within the first 24 hours may not be warranted or beneficial, but larger studies are needed to further examine this practice.
Delivering enteral feeds
PO (per Os) feeding
For the conscious patient with an intact appetite and swallowing function, direct oral intake is the preferred feeding modality. When prescribing a patient an oral diet, it is essential that the physician continuously monitor for adequate intake. In the acute surgical setting, many factors can lead to inadequate caloric intake, including high-caloric requirements because of injury, decreased appetite associated with injury response, depressed mental status, pain, or any other practical obstacles to eating such as bandages and functional limitations impacting utensil use. Should patients consistently fail to meet their caloric needs with a PO (per os, ie., oral) diet, consideration should be given to supplemental feeds via a nasoenteric tube.
In patients continuing to take food orally, careful monitoring should be maintained to ensure appropriate nutrition. Left unchecked, patients may frequently undereat or take in a disproportionate amount of calories as sugar or fat. A simple nutritional journal listing all foods and liquids consumed is often used to track intake. This journal can be maintained by the nursing staff, patient, and/or family throughout the day, and dietary adjustments can be encouraged as needed. In patients attempting to meet all needs orally (thus avoiding the need for an enteric access tube), supplemental “protein shakes” can be helpful in boosting total protein-caloric input.
Enteral access for feeding
Burn patients, particularly those suffering from larger burns, frequently prove incapable of eating sufficient quantities to meet their nutritional needs. Direct enteral feeding (“tube feeding”) is the method of choice to supplement or replace oral intake.
Either gastric or small-bowel access tubes can be used for delivering EN. Gastric feeding access allows for direct (trophic) feeding of the gastric mucosa. In the immediate postburn phase of resuscitation, though, gastric dysmotility may be present, posing a significant risk for aspiration and (particularly in children) for vagally mediated cardiac events. Thus we recommend placement of a venting nasogastric or orogastric tube for the duration of initial resuscitation.
Dysmotility does not tend to manifest in the small bowel as rapidly or as profoundly as in the stomach. Feeding using a nasojejunal tube advanced past the ligament of Treitz can be initiated within 6 hours after injury and may help in preempting the onset of starvation-associated ileus. This approach also allows continuous feeding during surgeries and physical therapy sessions. It should be noted that some authorities recommend attempting gastric feeds before resorting to postpyloric feeding, reasoning that gastric feeds may minimize the risk of gastric ileus associated with severe injury.
Nasojejunal feeding may be preferable in some settings because it does not need to be stopped before surgery to prevent aspiration. Contrary to the previously postulated protective effect of the pyloric sphincter, the largest randomized controlled trial and most recent meta-analysis of earlier studies indicate that nasogastric and nasojejunal feeds are associated with comparable rates of pneumonia.
In the past it was thought that monitoring residual stomach volumes via gastric tubes prevented aspiration pneumonia by (1) serving as a marker of enteric feed intolerance and (2) alerting the clinician to gastric distension so that feeds could be held to avert impending reflux and/or aspiration. Large multiinstitutional clinical trials have since shown that larger gastric residual volumes do not actually predict aspiration, and foregoing gastric residual monitoring altogether does not increase the incidence of pneumonia. In these studies, increasing or eliminating the gastric residual volume threshold led to significantly improved nutritional intakes.
Diet composition and enteral feed formulas
Numerous enteral formulations are available and can be classified according to their composition. Standard formulas are sterile, nutritionally complete, and intended for patients with a normal GI tract who cannot ingest adequate nutrients and calories by regular oral diets. Modular formulas consist of a singular macronutrient as a source of calories (e.g., fiber, protein) and are generally made by mixing with standard or specialty formulas ( Table 22.1 ).
Table 22.1
Composition of Various Enteral Nutrition Formulations
Data extrapolated from Nestle clinical nutrition: Enteral product reference guide. Minneapolis: Nestle, 2010; and Abbott nutrition pocket guide. Abbott Park, IL: Abbott Laboratories, 2009. From Al-Mousawi A, Branski LK, Andel HL, et al. Ernährungstherapie bei Brandverletzten. In Kamolz LP, Herndon DN, Jeschke MG, eds. Verbrennungen: Diagnose, Therapie und Rehabilitation des Thermischen Traumas . German ed. New York: Springer-Verlag; 2009:183-194.
| Formula | kcal/mL | CHO, g/L (% Calories) | PRO, g/L (% Calories) | FAT, g/L (% Calories) | Osmolality (mOsm/L) | Comments |
|---|---|---|---|---|---|---|
| STANDARD | ||||||
| Similac | 0.67 | 72 (43) | 15 (8) | 36 (49) | Infant nutrition | |
| Enfamil | 0.67 | 73 (44) | 14 (8) | 35 (48) | Infant nutrition | |
| Isomil | 0.67 | 68 (41) | 18 (10) | 37 (49) | Infant nutrition, lactose free, used in cow-protein allergy | |
| Isosource HN | 1.2 | 160 (53) | 53 (18) | 39 (29) | 490 | High nitrogen |
| Ensure Plus | 1.5 | 208 (57) | 54 (15) | 46 (28) | 680 | Concentrated calories |
| PediaSure Enteral | 1.0 | 133 (53) | 30 (12) | 40 (35) | 335 | For ages 1–13 years, with fiber, not easily digestible |
| Jevity 1.0 Cal | 1.06 | 155 (54) | 44 (17) | 35 (29) | 300 | Isotonic nutrition with fiber |
| Boost Kid Essentials | 1.0 | 135 (54) | 30 (12) | 38 (34) | 550–600 | Oral or tube feeding |
| Boost HP | 1.0 | 137 (55) | 62 (24) | 25 (21) | 650 | Oral or tube feeding, high protein |
| Promote | 1.0 | 130 (52) | 62 (25) | 26 (23) | 340 | High protein, oral or tube feeding |
| Promote with Fiber | 1.0 | 138 (50) | 62 (25) | 28 (25) | 380 | Very high protein, oral or tube feeding |
| Nutren 1.0 | 1.0 | 127 (51) | 40 (16) | 38 (33) | 370 | With fiber, decreases diarrhea |
| IMMUNE ENHANCING | ||||||
| Crucial | 1.5 | 89 (36) | 63 (25) | 45 (39) | 490 | With ARG, critical illness, major surgery, transitional feedings, hydrolyzed protein |
| Impact | 1.0 | 130 (53) | 56 (22) | 28 (25) | 375 | With ARG, GLN, and fiber |
| Impact GLN | 1.3 | 150 (46) | 78 (24) | 43 (30) | 630 | Immunonutrition, GLN, ARG, omega-3 PUFA, nucleic acids |
| Oxepa | 1.5 | 105 (28) | 63 (17) | 94 (55) | 535 | ARDS, acute lung injury, sepsis; concentrated |
| SPECIALTY | ||||||
| Glucerna | 1.0 | 96 (34) | 42 (17) | 54 (49) | 355 | For glucose-intolerant patients or patients with diabetes, low CHO |
| Nepro | 1.8 | 167 (34) | 81 (18) | 96 (48) | 585 | For CKD and patients on dialysis; concentrated |
| Osmolite 1.0 Cal | 1.06 | 144 (54) | 44 (17) | 35 (29) | 300 | Isotonic, for use in patients who are intolerant to hyperosmolar nutrition |
| Vivonex RTF | 1.0 | 175 (70) | 50 (20) | 12 (10) | 630 | Transitional feeding, low fat, easily digestible |
| Vivonex TEN | 1.0 | 210 (82%) | 38 (15%) | 2.8 (3%) | 630 | 100% free amino acids, very low fat, used for severe trauma (e.g., burns) or surgery, transitional feeding |
| Vivonex Plus | 1.0 | 190 (76%) | 45 (18%) | 6.7 (6%) | 650 | 100% free amino acids, very low fat, used for severe trauma (e.g., burns) or surgery, transitional feeding |
| EleCare | 0.67 | 72 (43%) | 20 (15%) | 32 (42%) | 350 | Prepared at 9.4 g/60 mL; amino acid-based nutrition |
| MODULAR | ||||||
| Resource Benefiber | 0.27 | 66 (100%) | 0% | 0% | — | Prepared at 4 g/60 mL; tasteless, odorless, soluble fiber, used for constipation |
| Resource Beneprotein | 0.83 | 0% | 200 (100%) | 0% | — | Prepared at 7 g/30 mL; whey protein, mixed in foods; protein-calorie malnutrition |
ARDS, Acute respiratory distress syndrome; ARG, arginine; CHO, carbohydrate; CKD, chronic kidney disease; GLN, glutamine; PRO, protein; PUFA , polyunsaturated fatty acids.
In a subset of distinctly hypermetabolic patients, the use of high-sugar, high-protein diets consisting of 3% fat, 82% carbohydrate, and 15% protein stimulates protein synthesis, increases endogenous insulin production, and improves lean body mass accretion-loss balance.
Muscle protein degradation is markedly decreased with the administration of a high-carbohydrate diet when compared with high-fat diets. This benefit stems from an increase in endogenous insulin concentration, thereby improving the net balance of skeletal muscle protein by decreasing protein breakdown. (See “ Substrate-Specific Requirements ” in this chapter for further discussion of the impact of augmenting various nutritional components.)
Immunonutrition
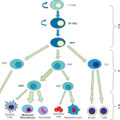
As noted earlier, immune dysfunction represents one of the most critical complications of malnutrition in burn patients. In animal and clinical studies, specific nutrients including arginine, omega-3 polyunsaturated fatty acids, glutamine, and nucleotides have been shown to positively modulate the host response with regard to immune function. Biochemically, arginine supplementation is intended to support T lymphocytes and provides a substrate for the generation of nitric oxide. Inclusion of nucleotides nonspecifically enhances immune competence. Long-chain omega-3 fatty acids decrease the production of inflammatory eicosanoids, cytokines, and adhesion molecules. This occurs directly by replacing arachidonic acid as an eicosanoid substrate, inhibiting arachidonic acid metabolism, and giving rise to antiinflammatory resolvins. This indirect effect continues on a transcriptional level with modulation of transcription factors that regulate the expression of inflammatory genes. The antiinflammatory benefits of omega-3 supplementation could be particularly helpful for those with preexisting acute and chronic inflammatory conditions ( Table 22.2 ).
Table 22.2
Effect of Omega-3 Polyunsaturated Fatty Acids on Eicosanoid Synthesis
| Metabolite | Physiologic Action | Omega-3 Effect |
|---|---|---|
| AA EICOSANOID | ||
| PGE 2 | Proinflammatory, vasodilator | ↓︎ |
| TXA 2 | Potent platelet aggregation and vasoconstrictor | ↓︎ |
| LTB 4 | Proinflammatory, neutrophil chemotaxis | ↓︎ |
| EPA EICOSANOID | ||
| TXA 3 | Mild platelet aggregation | ↑︎ |
| PGI 3 | Mild platelet disaggregation | ↑︎ |
Immune-enhancing formulas consist of nutritional components enriched with arginine, glutamine, nucleotides, and omega-3 fatty acids. Although most formulations are hyperosmolar at full strength, dilution by 25% to 50% to make isotonic and hypotonic formulas, respectively, is initially preferred to minimize the possibility of diarrhea from excess osmotic load and to facilitate absorption.
A myriad of clinical trials of immunoenhancing nutritional therapies have yielded conflicting results. Some early trials showed promise, but more recent investigations have generated concerning results. Perhaps most troublesome, as mentioned previously, the REDOXS trial examined the impact of glutamine supplementation in a large, heterogeneous population of critically ill patients. This trial found patients receiving glutamine supplementation not only exhibited no benefit but, surprisingly, also showed a trend toward increasing mortality compared with subjects treated with standard care. Furthermore, a similar large-scale study of enteral glutamine supplementation in patients with severe burns did not show any decreased hospital length of stay or a 6-month mortality benefit. Naturally, these findings have greatly dampened enthusiasm for glutamine supplementation and highlighted the importance of verifying hypothesized benefits through randomized clinical trials.
The conflicting nature of these results, and a higher number of studies that show potential benefit of immunonutrition in burn patients, highlight the need for further study. Interestingly, studies of serum glutamine levels in broad populations of critically ill patients suggest that not all patients are deficient. In the modern age of individualized medicine, there may be certain patient phenotypes, particularly among patients who are already nutrient deficient (chronically malnourished patients, those with hypercatabolic trauma, and burn patients), in which immunonutrient supplements are of much greater benefit. , , Finally, post hoc analysis of the REDOXS data suggests that the majority of the mortality risk associated with glutamine supplementation could be attributed to patients already in multiorgan or renal failure before the initiation of treatment. In light of this fact, it may be prudent to highlight more specific inclusion and exclusion criteria for glutamine supplementation candidates to avoid confounding variables.
Parenteral nutrition
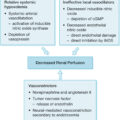
For decades, the critical-care literature has emphasized the significant morbidity and mortality risks associated with the use of PN. This emphasis led to the widespread dogma that the beneficial impact of PN can outweigh its risks only when applied to patients who are otherwise facing indefinite total starvation. More recent assessments suggest that the risk profile of PN has declined significantly most likely because of the improving efficacy of critical-care practices.
Although PN undoubtedly involves significant risks and morbidity, there is reason to believe that advances in critical care (e.g., improved glycemic control and infection control practices) have significantly mitigated these risks. Multiple large trials have evaluated the use of PN as a supplement rather than a replacement for EN, with variable results. Large multiinstitutional clinical trials in broader populations of critically ill patients have found that the use of PN either as a supplement or as a replacement for EN (i.e., TPN) no longer worsens outcomes even in patients able to tolerate EN. Perhaps most convincingly, Harvey et al. randomized 2400 ICU patients to receive either EN or PN and found no evidence of increased 30-day morbidity or mortality in the PN group. Although extremely provocative, these findings have not been tested in burn patients specifically. Such studies would be well warranted and should be encouraged.
The utility of supplemental PN (applied liberally) remains a matter of considerable debate. It is our opinion that supplemental nutrition can be quite helpful when applied selectively. Decisions regarding its use should be made based on clinician assessment of the individual patient’s metabolic needs and nutritional status. Accordingly, it is our practice to use supplemental PN in the acute phase of the burn injury response in patients unable to tolerate enteral feeds at quantities sufficient to meet (or at least approach) protein-caloric requirements. Patients who manifest enteral feeding intolerance in the subacute phase of burn injury response are typically prescribed supplemental PN only if they have evidence of preexisting malnutrition at the time of the burn. ,
Before receiving PN, patients should be hemodynamically stable and able to tolerate the fluid volume and nutrient content of parenteral formulations. PN should be used with caution in patients with congestive heart failure, pulmonary disease, diabetes mellitus, and other metabolic disorders. The significant amount of fluid and sugar may be difficult for patients to tolerate. Although there has long been debate as to the optimal timing for initiation of TPN in patients unable to tolerate adequate EN, the results of recent, randomized controlled trials suggest that early initiation of TPN is an appropriate strategy in these patients ( Tables 22.3 and 22.4 ). , , Given the particularly high energy expenditure of burn patients, it is our practice to initiate parenteral nutrition fairly early in patients unable to tolerate effective enteral nutrition.
Table 22.3
Composition of Parenteral Nutrition Formulations
| CALORIC CONTENT | ||||
|---|---|---|---|---|
| Sample Nutrition | g/dL | kcal/g | kcal/mL | mOsm/L |
| 2-IN-1 SOLUTIONS | ||||
| Dextrose | ||||
| DW 10% | 10 | 3.4 (CHO) | 0.34 | 505 |
| DW 30% | 30 | 3.4 (CHO) | 1.02 | 1510 |
| DW 70% | 70 | 3.4 (CHO) | 2.38 | 3530 |
| Amino acids | ||||
| Aminosyn RF 5.2% | 5.2 | 4 (PRO) | 0.2 | 427 |
| Travasol 10% | 10 | 4 (PRO) | 0.4 | 998 |
| Prosol 20% | 20 | 4 (PRO) | 0.8 | 1835 |
| Lipid emulsion | ||||
| Intralipid 10% | 10 | 11 (FAT) | 1.1 | 300 |
| Intralipid 20% | 20 | 10 (FAT) | 2 | 350 |
| Intralipid 30% | 30 | 10 (FAT) | 3 | 310 |
CHO , Carbohydrate; PRO , protein.
Table 22.4
Clinical Conditions Requiring Cautious Use of Parenteral Nutrition
From Mirtallo JM. In: Gottschlich MM, ed. The A.S.P.E.N. Nutrition Support Core Curriculum: A Case-Based Approach: The Adult Patient. Silver Spring, MD: American Society for Parenteral and Enteral Nutrition; 2007:268.
| Condition | Suggested Criteria |
|---|---|
| Hyperglycemia | Glucose > 300 mg/dL |
| Azotemia | BUN > 100 mg/dL |
| Hyperosmolality | Serum osmolality > 350 mOsm/kg |
| Hypernatremia | Na > 150 mEq/L |
| Hypokalemia | K < 3 mEq/L |
| Hyperchloremic metabolic acidosis | Cl > 115 mEq/L |
| Hypophosphatemia | Phosphorus < 2 mg/dL |
| Hypochloremic metabolic alkalosis | Cl < 85 mEq/L |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree