Management of the Open Abdomen
Alexander F. Mericli
Charles E. Butler
DEFINITION
The phrase “open abdomen” is used to describe a defect in the abdominal wall that exposes the viscera.
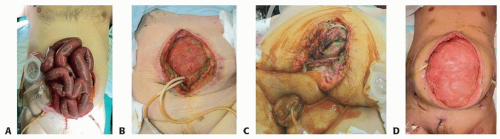
There are several challenging clinical scenarios that can necessitate leaving the abdominal cavity opened or that can result in an open abdomen (FIG 1):
Damage control laparotomy after trauma
Excessive visceral edema as seen in severe abdominal sepsis
Following a decompressive laparotomy for management of abdominal compartment syndrome
Strategies involving a planned relaparotomy (second look for intestinal ischemia)
Staged abdominal wall reconstruction after fascial dehiscence and evisceration
The central tenant of open abdomen management is the construction of a temporary abdominal closure until definitive abdominal wall reconstruction can be performed.
When one is confronted with a clinical situation that requires an open abdomen or results in an opened abdomen, there is a number of reasons why it may be prudent to stage the abdominal reconstruction with a temporary abdominal closure:
Decreases tension on the musculofascial abdominal wall and prevents abdominal compartment syndrome
Reduces risk of evisceration
Facilitates regaining access to the abdominal cavity
Reduces lateral retraction of the skin, subcutaneous tissue, muscle and fascia
Ideally, it facilitates a delayed primary abdominal wall closure.
ANATOMY
The abdominal wall is a layered structure consisting of muscle and fascia.
The paired rectus abdominis muscles comprise the central portion, ensheathed in the fascia of the anterior and posterior rectus sheaths.
The rectus muscles are flanked on either side by the oblique family of muscles: the external oblique, followed by the internal oblique, followed by the transversus abdominis.
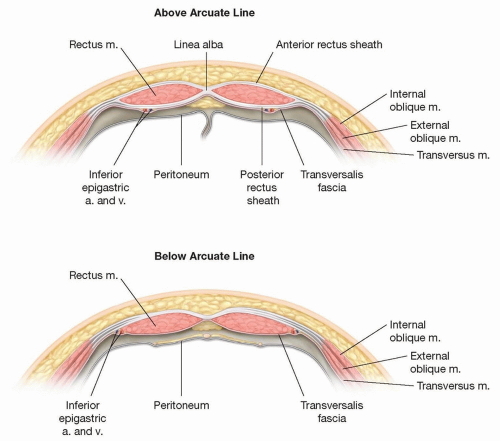
Above the arcuate line (approximately at the level of the anterior superior iliac spine), the anterior rectus sheath is made up by contributions from the external oblique aponeurosis and internal oblique; the posterior rectus sheath is made up by the internal oblique, transversus, and transversalis fascia.
Below the arcuate line, there is no posterior sheath, only transversalis fascia is below the rectus muscle (FIG 2).
PATHOGENESIS
The scientific rationale for the creation and maintenance of an open abdomen is centered on the phenomenon of intestinal edema and decreasing the impact of the inflammatory cascade.
The intestine is a highly vascularized structure with a rich network of arteries, veins, capillaries, and lymphatic vessels. In pathologic states, such as after an abdominal trauma, after abdominal surgery, or in abdominal sepsis, a decrease in clearance of fluid from the extracellular space can result in swelling of the intestinal wall several times the normal diameter, potentially interfering with perfusion of the bowel.
Multiple inflammatory cells are present within the bowel wall and peritoneal membrane.
In the postsurgical abdomen, the trauma abdomen, and in abdominal sepsis, there is a profound local inflammatory response, which quickly progresses to systemic inflammatory response syndrome (SIRS), which can easily contribute to multiple organ dysfunction syndrome (MODS).
Premature closure of the abdomen can exacerbate the inflammatory response and accelerate these syndromes as well as contribute to abdominal compartment syndrome.1
Abdominal Compartment Syndrome
Abdominal compartment syndrome is a syndrome of uncontrolled intra-abdominal hypertension. Any factor that raises intra-abdominal pressure can contribute to abdominal compartment syndrome, including free blood and clots, bowel edema, vascular congestion, excessive crystalloid resuscitation, intraperitoneal packing, and nonsurgical bleeding, acidosis, hypothermia, and postoperative ileus.
Normal intra-abdominal pressure is 0 to 5 mm Hg and can easily be quantified by measuring bladder pressure.
Abdominal compartment syndrome is defined as a sustained bladder pressure of 20 mmHg or greater with dysfunction of 1 or more organ systems (ie, heart, lungs, kidneys, neurologic, etc.) OR a sustained bladder pressure of greater than 25 mmHg without organ dysfunction.
Once diagnosed, emergent abdominal decompression is indicated. Typically, organ function returns to normal after decompression, but a mortality rate of 50% has been recorded, secondary to ongoing MODS.6
NATURAL HISTORY
There are numerous physiologic changes that accompany an open abdomen. These changes are not insignificant and can contribute to substantial morbidity; however, the potential for morbidity of an intentional open abdomen is outweighed by the possible complications that could ensue, should the abdomen be closed prematurely.
Fluid balance
A significant amount of peritoneal fluid is lost through an open abdomen, typically 1 L/h for a 70 kg person.
If a closed suction system is used as part of the temporary abdominal closure, such as negative pressure therapy, then this fluid loss can be quantified and therefore accurately replaced.
Maintenance of normothermia
The large cutaneous defect oftentimes present with an open abdomen impairs the body’s thermoregulatory system.
The loss of peritoneal fluid exacerbates heat loss through convection.
Frequent temperature monitoring, forced air warming blankets, and a warmed room are all techniques that can be employed to counteract this effect.
Protein loss
Peritoneal fluid is protein rich, with 2 g protein/L.7 This must be replaced through diet or enteral feeds in order to maintain nitrogen balance.
Fistula
With the open abdomen, the bowel is at risk for injury. Patients with a fresh bowel anastomosis are at greatest risk.8
Whenever possible, the viscera should be covered by the omentum for an additional layer of protection.
Loss of domain
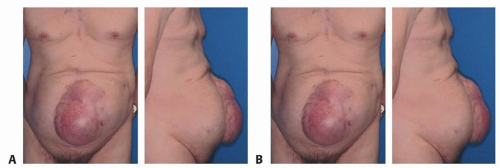
The creation of an open abdomen places the patient at risk for losing abdominal domain as the musculofascial abdominal wall retracts laterally over time (FIG 3).
Methods of temporary abdominal closure are designed to prevent this situation by keeping the fascia as medial as possible.
PATIENT HISTORY AND PHYSICAL FINDINGS
Although it is most commonly the decision of the general or trauma surgeon, it is helpful for the plastic surgeon to understand the factors that are involved in deciding whether a patient should be managed with an open abdomen.
Trauma/damage control
Preoperative predictors: penetrating torso trauma with hypotension, need for resuscitative thoracotomy, blunt abdominal trauma with intraperitoneal hemorrhage, and hypotension
Intraoperative predictors: development of a coagulopathy, intraoperative exsanguination requiring greater than 10 units of packed red blood cells, pH less than 7.2, base deficit greater than -6 in patients older than 55 years or greater than -15 in patients younger than 55 years, temperature less than 34°C, and/or estimated blood loss greater than 4 L2.
Abdominal compartment syndrome
Patients with sustained intra-abdominal pressure greater than 20 mm Hg with onset of new organ dysfunction
Patients with acutely increased intra-abdominal pressures greater than 25 mm Hg without acute organ dysfunction should be considered for prophylactic decompression.
Patients at high risk for development of abdominal compartment syndrome: those requiring greater than 15 L crystalloid or 10 units of packed red blood cells, patients with increased peak inspiratory pressures greater than 40 mm Hg upon fascial closure.2
Planned relaparotomy
Management of intestinal ischemia potentially requiring repeat bowel resections
Severe abdominal sepsis necessitating repeated debridements, such as in pancreatic necrosis or intra-abdominal abscesses
Acute postoperative evisceration
Fascial dehiscence in the acute or subacute postoperative period can result in evisceration. Given that this often occurs during the inflammatory stage of wound healing, visceral edema and friable, inflamed abdominal wall soft tissue may preclude immediate fascial reapproximation.
IMAGING
Computed tomographic imaging of the abdomen and pelvis are imperative for surgical planning and preoperative evaluation. FIG 4 demonstrates images from a patient with an open abdomen and associated lateral musculofascial retraction (loss of domain) (left) as well as a patient with an incisional ventral hernia after laparotomy (right).
SURGICAL MANAGEMENT
A variety of surgical techniques for temporary abdominal closure are available, ranging from a skin-only closure to the more sophisticated ABThera System (KCI, San Antonio, TX).
The ideal temporary closure contains the viscera, minimizes skin maceration and damage to the underlying bowel or fascia, and facilitates durable fascial reapproximation. Although there are advantages and disadvantages to each technique (Table 1), the method of temporary abdominal closure is largely dependent upon surgeon preference.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree