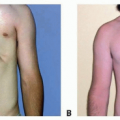
Laser Burn Scar Revision
C. Scott Hultman
Yuen-Jong Liu
DEFINITION
Mortality from burn injury has markedly decreased in the second half of the 20th century as wound sepsis, wound coverage, kidney failure, and shock have been largely overcome.
Burn injury is the result of high-energy transfer to a significant surface area of the skin or soft tissues and can be categorized by the form of energy:
Contact with high temperature solids (contact), liquids (scald), or gases (flame)
Contact with low temperatures (frostbite)
Exposure to chemicals (acids, alkalines, or other caustic reagents)
Electricity
Friction or abrasion
Burn wounds frequently heal in the form of hypertrophic scars, which hamper functional and aesthetic outcomes.
Symptoms include pruritus, burning pain, and hyperesthesia, which may be treated with antihistamines, narcotic analgesics, and non-narcotic analgesics.
Functional deficits may vary from tightness or tethering of the surrounding skin to contractures that limit range of motion.
Hypertrophic burn scars may be erythematous due to hypervascularity.
Treatments include occupational therapy, physical therapy, compression garments, moisturizing agents, sunblock, and scar massage.1,2
Evidence for the efficacy of laser therapy in the treatment of hypertrophic burn scars is now well documented in individual cohort studies,3 review articles,4 and a rigorous metaanalysis of 28 well-designed clinical trials.5
The exact biologic mechanism for improvement has yet to be elucidated, but pulsed dye laser (PDL) improves the inflammatory component of hypertrophic burn scars, which have excess pathologic vascularity, whereas fractional carbon dioxide (CO2) laser improves remodeling of dermal collagen, which is disorganized and abnormal in hypertrophic burn scars.
Best practices involve six to eight laser sessions, performed every 4 to 6 weeks, using a combination of these two lasers, plus on occasion the Alexandrite laser, to ablate hair follicles in cases of chronic folliculitis of the burn scar.
Substantial, rapid improvement in hypertrophic burn scars is now observed through objective measures, such as the Vancouver Scar Score (height, erythema, pliability), as well as subjective reports, such as the UNC 4P Scar Score (pruritus, paresthesias, pliability, and pain).6
A major benefit to both the patient and the payer is that multiple, minimally invasive laser sessions may decrease or prevent the need for more complex and more invasive surgical procedures, decreasing patient risk, reducing overall cost, and potentially achieving outcomes not previously possible.
ANATOMY
Burn scars may affect any part of the body.
Hypertrophic scars across joints may cause contracture.
Contractures on the face may interfere with competence of the eyelids or the mouth.
Burn scars are especially disfiguring on the face due to its high aesthetic importance.
Neuropathic pain may be observed in burned areas, grafted regions, and even donor sites.
PATHOGENESIS
The incidence of hypertrophic scarring after burn injury ranges from 5% to 40%, depending on anatomic location, depth of burn, method of closure, and genomic response to healing.
Hypertrophic scarring and contractures can develop in burn scars that heal by secondary intention or re-epithelialization, in split-thickness skin grafts over excised burns, along the seams of full-thickness grafts, and in donor sites that had delayed healing, due to infection of excessive depth of harvest.
Hypertrophic scars may be associated with an imbalance of collagen types 1 and 3, as well as TGF beta 1 and TGF beta 3.
Hypertrophic scarring can be viewed as an abnormal physiologic response after wound closure, in which collagen deposition and angiogenesis continue beyond their desired end points.
NATURAL HISTORY
Neuropathic symptoms, such as pruritus, searing pain, hyperesthesias, and paresthesias, are a source of frustration for the patient, can limit quality of life, and may prevent return to school, work, and social functions.
Hypertrophic scarring may cause disability ranging from minor discomfort to joint contracture.
Hyper- or hypopigmentation, erythema, and abnormal texture may cause the burn scars to be aesthetically unacceptable.
PATIENT HISTORY AND PHYSICAL FINDINGS
Complete patient history should be elicited, focusing on the type of energy delivered: scald, electrical, flame, contact, chemical, cold, friction, abrasion, or other.
Previous treatments and their effects should be noted, including skin grafting, laser treatments, topical scar treatments, moisturizing agents, sunblock, systemic medications, occupational therapy, physical therapy, compression garments, and massage.
The patient should have had no significant improvement in symptoms for at least 3 months on maximal medical therapy.
Relative contraindications to laser therapy include connective tissue disorders, utilization of systemic steroids or immunosuppressive medications, and chemotherapy or radiation therapy. Patients with moderate to severe lymphedema should also be treated with caution, as healing from ablative lasers may be delayed.
Complete physical exam should be performed, focusing on the burned area, noting whether it is a native burn scar or burn scar after skin grafting.
The burned areas should be well healed without open wounds or evidence of cellulitis.
Total body surface area of the burn injury should be noted, as extremely large areas should be staged, in terms of laser treatment.
Functional deficits should be recorded, such as loss of range of motion or loss of sensation.
Aesthetic concerns should also be considered, especially in burns of the face and the hands.
The patient’s Fitzpatrick skin type should be documented, and this will advise the initial energy settings for the laser.
Photographs are useful for insurance submission and to track progression of the scar between laser treatments.
IMAGING
Imaging is not required. However, medical photography is often needed for preauthorization from insurance companies.
For patients enrolled in a clinical trial, other imaging modalities might be helpful to measure extent of hypertrophic scarring and quantify changes:
Ultrasound to measure thickness of scar
Chroma meter to measure light-dark axis and degree of redness from erythema
Cutometer to measure elasticity of scar
SURGICAL MANAGEMENT
The patient is routinely consented for a series of laser treatments, involving selective photothermolysis with the PDL, ablative resurfacing using the fractional using CO2 laser, and either Alexandrite or diode lasers to rupture hair follicles.
A series of 6 to 8 sessions is submitted for insurance coverage at a time, though a patient may reach maximal benefit before 6 to 8 sessions or may continue to experience symptomatic improvement beyond eight sessions.
We strongly recommend maintaining a burn scar registry, which includes preoperative, operative, and postoperative data, which can be used for practice-based learning, retrospective and prospective cohort analysis, insurance preauthorization and payment, and medical-legal documentation.
We recommend working with a board-certified anesthesiologist who has completed additional specialization in pediatric anesthesia or has significant clinical experience with children and has expertise in ambulatory and office-based anesthesia.
Multimodal anesthesia has been shown to significantly decrease patient pain, need for intravenous opioids during recovery, and time to discharge from the postanesthesia care unit.7
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree