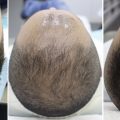
When I began performing cosmetic surgery in the 1990s the word “injectables” was not common parlance. Most practices were surgical and the only Food and Drug Administration (FDA)-accepted fillers were Zyderm and Zyplast. These were bovine collagen and patients would come in for an allergy test and a month later present for their filler injection. Certainly not an impulsive treatment! There was also a lack of longevity, as these fillers only seemed to last for several months. In 1995, it seemed quite unlikely that within a decade, injectable treatments would be a large part of my practice and the most popular cosmetic treatment in the world.
Although countries outside the USA had been using scores of various filler materials for years, the technology was slow to come to our shores. The FDA approval of Restylane in 2003 ( www.gladerma.com ) and Juvederm in 2005 ( www.allergan.com ), ushered in a new breed of cosmetic filler treatments. These new fillers were non-animal, stabilized hyaluronic acid (HA), without allergic reaction and cross-linked for longevity. Hyaluronic acid (a glycosaminoglycan) is a naturally occurring, highly hydrophilic polysaccharide found in all living cells; it attracts and binds more than 1000 times its weight in water and is chemically, physically, and biologically similar in all species, which negates allergy testing. Equally important is the fact that HA is reversible with hyaluronidase.
Natural hyaluronic acid is enzymatically degraded in 24 h and metabolized in the liver into byproducts: water and carbon dioxide. In the skin, HA is broken down by hyaluronidase and by free radicals. Proprietary cross-linking of these products makes them resistant to breakdown, thus producing longevity of the filler. The various methods of cross-linking also give the specific filler qualities such as stiffness.
These drugs (actually not classified as drugs, but approved by the FDA as medical devices) have changed the landscape of non-surgical, minimally invasive treatments. Once patients saw how easy and effective fillers and neurotoxins were, they became extremely receptive to other nonsurgical procedures and this boom became so popular that it is a requisite of all cosmetic practices.
Since almost 80% of all fillers injected in the world are HA-based, most of this chapter will focus on these products. Having said that, the basic technique for all fillers is similar but dependent on the type of filler and the anatomic region being treated. For the sake of completeness, other types of fillers are also discussed here.
At the time of writing, the most popular hyaluronic fillers include:
Galderma products ( www.galderma.com )
- •
Restylane
- •
Restylane Lyft (formerly Perlane)
- •
Restylane Silk
Allergan products ( www.allergan.com )
- •
Juvederm Ultra
- •
Juvederm Ultra Plus
- •
Juvederm Voluma
- •
Juvederm Volbella
Merz Aesthetics product ( www.merz.com )
- •
Belotero
All these products began with the generalization of “dermal fillers” and remain so in common parlance, although the injection target for each product may be different. For instance, Restylane Silk is injected in the superficial dermis, whereas Juvederm Voluma is injected in the subcutaneous tissues. Since each product has particle size or gel characteristics that are different, how and where they are placed is critical to their proper use, effect, and longevity.
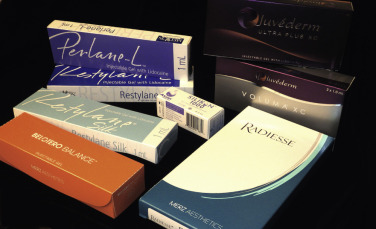
Hyaluronic acid fillers can be mono- or biphasic. Monophasic fillers (Juvederm line of fillers) consist of a cohesive gel instead of hyaluronic acid particles, while biphasic fillers (Restylane line of fillers) consist of various sized hyaluronic acid particles. This is performed in the manufacturing process where the HA is passed through different sized screens to produce small or large particles. Each company promotes their gel or particle composition as the best and, as expected, marketing and profit enter the picture. In reality, all the aforementioned fillers are safe and effective. A given surgeon or patient may have better experience with one brand or type over another, but they have all been interchangeable in my experience when comparing the same properties or composition with brand ( Fig. e10.1 ![]() ).
).
Non-Hyaluronic Acid Fillers
Popular non-hyaluronic FDA-approved fillers include:
- •
Radiesse ( www.merz.com ), an injectable filler that consists of hydroxyapatite microspheres in a soluble gel vehicle. It is resorbed over a 12-month period.
- •
Sculptra ( www.galderma.com ), an injectable implant that contains microparticles of poly- l -lactic acid, a biocompatible, biodegradable, synthetic polymer from the alpha hydroxy acid family. Sculptra is reconstituted prior to use by the addition of sterile water. The mechanism of Sculptra is different from other fillers, in that the response is not immediate, but rather the poly- l -lactic acid particles serve to initiate an inflammatory reaction and induce the production of collagen in the area. The company states that the effects may last up to 2 years but results are variable.
Permanent Injectable Fillers
- •
Silikon 1000 injectable silicone oil is a filler of historic significance that has been both praised and scorned over the past 50 years and will be discussed separately in this chapter. Silikon 1000 (which is FDA approved for retinal detachment) is injected in small aliquots and as an inflammatory response, is walled off by collagen to contain and enhance the filling. The results are permanent.
- •
Bellafill (sunevamedical.com) is designed with dual action to correct facial wrinkles: 20% precision-filtered microspheres made from polymethylmethacrylate (PMMA) and 80% purified bovine collagen. Aesthetic results are visible immediately after injection. PMMA is not taken up by scavenger cells (macrophages) and cannot be degraded by enzymes. Thus, the microspheres will remain intact beneath the creases, providing a permanent structure to support the wrinkle and prevent further wrinkling. As with all products using bovine collagen, a skin sensitivity test must be performed prior to use.
- •
Autologous fat is a “natural” filler and technique and is discussed later in this chapter.
The hyaluronic acid fillers are reversible and this is a tremendous insurance policy for both patients and surgeons, as a poor result, overfill, or change of heart can be dealt with overnight.
The above list of fillers has changed from the first edition of this text and will certainly change with upcoming editions, as this is a popular and exponentially expanding market. There are several other HA fillers that occupy a very small niche in the marketplace and are not discussed here.
Anatomic Considerations of Injectable Fillers
Over the past decade, the average cosmetic facial surgery practice has embraced the art and science of facial fillers. Whereas early filler use was two-dimensional to treat individual lines and wrinkles, contemporary filler use is three-dimensional with larger volumes being injected to enhance volume in much larger cosmetic units. Some 20 years ago, 0.5 mL of a collagen filler may have been used in a single wrinkle, whereas today it is not uncommon to inject 6 mL of hyaluronic acid filler in the midface. “Filler facelifts” (although I personally don’t like that nomenclature) may use 15 syringes to volumize the entire face.
With a long-standing appreciation for volume loss in relation to facial aging and the advancement of filler science, the contemporary cosmetic facial surgeon has new tools to perform minimally invasive facial rejuvenation. Volume loss is one of the prime factors that cause an aged look. Today’s cosmetic surgery patients are extremely savvy on the pros and cons of specific procedures. They want to look younger, not just tighter. The past emphasis from surgeons was to look tighter, and little attention was paid to volume restoration. With the new era of cosmetic sophistication, fillers (and facial implants) serve as the icing on the cosmetic cake. For younger patients, fillers can serve as a sole procedure to disguise aging. For older patients, they can be used with other rejuvenative procedures to refine the treatment results.
It is far more important how the filler is used than which filler is used. A competent injector can achieve aesthetic results from any filler if he or she knows how to use it and where to put it. Conversely, an inexperienced injector can use a premium filler and get poor results. The key to success with all fillers is correct placement in the skin and deeper tissues, and various anatomic sites have specific injection techniques. For optimum results, safety, and longevity the clinician needs to use the “right” filler in the “right” place on the “right patients.”
Most fillers are specifically designed to be placed at a certain level. The exact level of filler placement is a debatable subject. Many fillers say their intended target is the “dermis,” and some injectors describe injecting in the mid- or deep dermis. Biopsies of “dermal” fillers actually show filler in various positions throughout the dermis and subcutaneous tissue, so it is technically impossible to say a filler is monoplanar. The filler needs to be placed where its most optimum action can be exerted, including the dermis and subcutaneous planes, and sometimes on the periosteum. There is no doubt that this varies from patient to patient and is affected by skin thickness, region to be injected, amount of aging, and the specific filler composition. There are some general rules that make sense and can serve as guidelines to tissue placement. The less viscous gel fillers or those with smaller particle sizes are intended for more superficial dermal placement. The medium-particle fillers are meant for the mid-dermis, and the more robust or particulate fillers are intended for deep dermal or subcutaneous placement. Again, an experienced injector can push these boundaries. Placing viscous or particulate filler too superficially may produce contour irregularities or be visible through the tissue. Conversely, placing a small-particle filler in the deep tissue planes can result in premature resorption.
G Prime
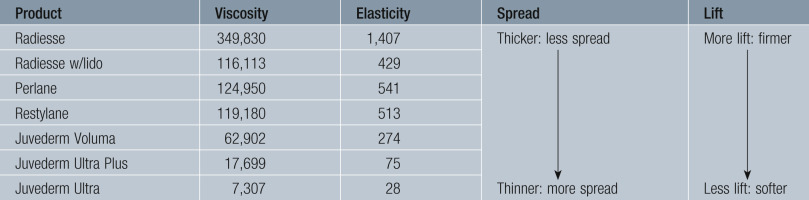
Rheology is the study of the flow of matter and G prime is a common measurement. To determine G prime, the filler is placed between two plates, which are then subjected to a lateral force. The measurement of this resistance to deformation is calculated as G prime. G prime is elastic modulus of the filler or the stiffness. To the clinician this translates as viscosity and the lower G prime fillers are less viscous and placed more superficially, while the larger G prime fillers are more viscous and placed deeper in the tissues. Low G prime fillers are used for fine lines and wrinkles and high G prime fillers are used for lifting and support such as cheek filling ( Table 10.1 ). The degree of cross-linking affects the gel hardness (G prime). Although higher G prime is frequently associated with greater ability to lift, some researchers say that this may be true in vitro but not in vivo.
The prime statement, “The key to success is placing the ‘right’ filler in the ‘right’ place in the ‘right’ patient” is often referred to in this chapter as it is so important. This means picking the correct product for the task at hand and then placing it in the proper anatomic plane(s).
Although these fillers as a group are referred to as “dermal” fillers, a common mistake of the novice injector is to place HA gel fillers too deeply or too superficially. This can produce inadequate augmentation and it dissolves faster. There is a “sweet spot” on the skin where the placement of filler produces controlled augmentation, and that differs from patient to patient. Experienced injectors know where to put the filler for maximum result, and this is a learned skill guided more by feel and visual result than by science. Placing fillers such as silicone, Radiesse, fat, and Sculptra or Voluma in the superficial dermis can produce contour irregularities. Placing fillers such as Restylane, Juvederm Ultra or Belotero in the subcutaneous tissues is a less judicious choice than their more robust larger-particle or thicker-gel counterparts.
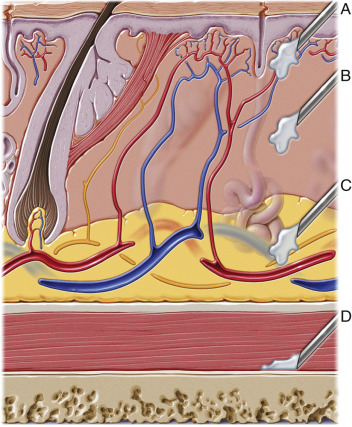
Although confusing, the tenet of intradermal placement is a good starting place for the novice injector. Injecting in the dermis is an appreciated tactile situation with contributions from the pressure of the needle entry and advancement and the syringe pressure. Again, experienced injectors can sense the correct plane. A pearl for novice injectors as to when the needle is in the dermis is observing the needle bevel upon skin entry. When the bevel of the average injection needle enters the skin and cannot be seen, this is an approximate indication that the tip is in the dermal plane. All injectors must be aware of the intended tissue plane target for various fillers ( Fig. 10.1 ). Experienced injectors will frequently layer fillers in different tissue planes to achieve results and sometimes use different fillers for the same injection. These anatomic tissue targets are discussed in detail throughout this chapter.
Injectable Fillers: Treatment Considerations
“Doctor, how long will my filler last?” This is a question asked by many patients and is not an easy one to answer. Although companies quote optimistic lengths of filler longevity, much variability exists. It depends upon the type of filler, the patient’s metabolism, the area of the face where the filler is placed, and other variables. As a general rule, fillers placed in areas of extreme motion such as the lips, will not last as long as fillers placed in a more immobile area such as the zygoma.
I never guarantee longevity, as there are too many variables and I tell patients that most HA fillers will hopefully maintain a result lasting from 6 to 12 months. Silicone may last forever; Radiesse may last 1.5 years; and Voluma may last up to 2 years. I have had patients claim that their filler only lasted 2 weeks and others say it lasted 4 years. Although the industry is pushing permanent fillers, it must be remembered that permanent fillers can cause permanent complications! In the case where the filler is not to the patient’s or surgeon’s liking, reversal is a welcome option and is discussed later in this chapter.
Due to the growing plethora of fillers, a contemporary practice must stock all the common fillers and in essence be a “filler bartender” ( Fig. e10.1 ![]() ). All injectors have their favorites, but various patients choose various products based upon their experience, the desire to try something new, and in response to the topical literature, websites, and magazine ads. Another factor that drives patient choice are discounts offered at times by various companies and their “loyalty programs,” where patients receive points or credits similar to frequent flier miles. Finally, high-volume injectors receive discounts on how much filler they order.
). All injectors have their favorites, but various patients choose various products based upon their experience, the desire to try something new, and in response to the topical literature, websites, and magazine ads. Another factor that drives patient choice are discounts offered at times by various companies and their “loyalty programs,” where patients receive points or credits similar to frequent flier miles. Finally, high-volume injectors receive discounts on how much filler they order.
Patient Selection
The rate of advancement of filler technology has proved to be confusing for patients (and some doctors) so it is imperative to “choose the right patient” for a given application. Many patients do not understand the difference between fillers and neuromodulators (neurotoxins), so education and comprehension are the two prime factors. Although fillers have broad aesthetic applications, they are not miracle treatments. Many patients present with abundant and severe wrinkling that would better be treated with skin resurfacing or facelift. Although these patients may be temporarily improved with $4000–5000 worth of filler, it is not in their best interest in the long run. Some patients may not desire surgery or not care about the filler expense, but acting in the patient’s best interest is always the first rule of medicine.
In theory, fillers can be injected anywhere on the body; however, blindness, stroke, and severe tissue loss and disfigurement is becoming more common with the increased use of fillers. The main consideration is to accurately explain what can be realistically expected as a treatment result. Showing patients a series of before and after images for specific anatomic areas is one way to provide a reasonable expectation. In addition, the injection of fillers should not be presented as a one-time procedure but as a sculpting treatment sequence to approach a result. This is especially true for HA fillers because their hydrophilic properties can cause immediate swelling in the lips, which makes judging the endpoint and symmetry difficult. One huge advantage of HA fillers is that there is no need to over-correct as with older fillers that resorbed quickly. It is also very helpful to have the patient return 2 weeks after injection to review the result. Any areas of underfill or asymmetry can be corrected and post-injection images can be taken for marketing and education. The novice injector should begin with “appetizer-sized” portions of filler and remember that there is nothing wrong with a treatment requiring multiple visits to achieve optimum results. Having patients return can be very helpful as I see patients who are happy, but I may also see deficiencies. Also, from time to time the inverse occurs where the patient is not happy but the result is adequate. Discussing all possibilities before injection is imperative as is having the proper informed consent. This is especially true with older females who may expect unrealistic results from treatment to lips or wrinkles. The best candidates for novice injectors are younger patients with small deficiencies.
Informed Consent Process
The communication that occurs before filler injection can be paramount to a success or failure in the eyes of the patient and or the law. This is the time to detail many other critical issues, including expected longevity, what the filler will or will not do, who will be responsible for the cost of revision filler, and how much filler needs to be used. Many “para filler” problems can be easily resolved by showing the patient their signed consent if post-injection problems arise. My consent is a dynamic instrument. I add to it regularly to preempt potential problems that may arise or new problems not on the current consent. Consents should be accurate and include extremely rare but possible problems such as blindness and tissue loss. “Better to have and not need than to need and not have.” Preinjection photography is also invaluable for situations where the surgeon is blamed for an existing preinjection problem. These photographs not only serve to assist in adverse situations, they serve as a teaching and learning tool for the surgeon and are invaluable for marketing.
The question of how much filler to use is always part of the preinjection discussion. Due to the high cost of a syringe of filler, many new filler patients desire to test the waters by purchasing a single syringe. For the nasolabial folds in adult patients, I almost never use only a single syringe. The problem is that a single syringe is usually insufficient to augment bilateral nasolabial folds in the older patient. The average adult could tolerate three to four syringes and would have better results if finance was not an issue. Attempting this to save money will usually produce an unhappy patient, because the result is minor and the patient can spend $600 and see no results. This can reflect on the expertise and reputation of the surgeon. When adults in the late fourth decade and beyond present for nasolabial fold or oral commissure treatment and request a single syringe, I explain the drawback to them and ask them to save their funds until they can afford the proper amount, which is usually at least two syringes.
It is important to advise patients to not expect their nasolabial folds or wrinkles to be eradicated; they will be improved, but not gone. I explain that the nasolabial fold is a valley, and the filler will make it shallower, not eliminate it. I also explain that although the nasolabial fold (or other wrinkles) may look much better in repose, they will still show upon smiling and animation. This is important because some patients will return after injection and complain that when they smile, they still see their wrinkles or folds. When treating the lips, a single syringe may be split between the lips of younger patients, but older patients, especially those with lipstick lines and perioral wrinkles, can take several syringes.
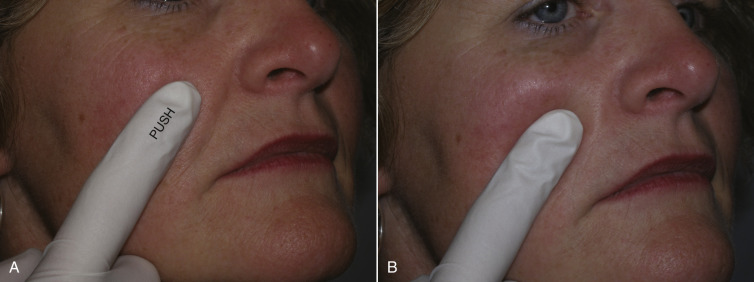
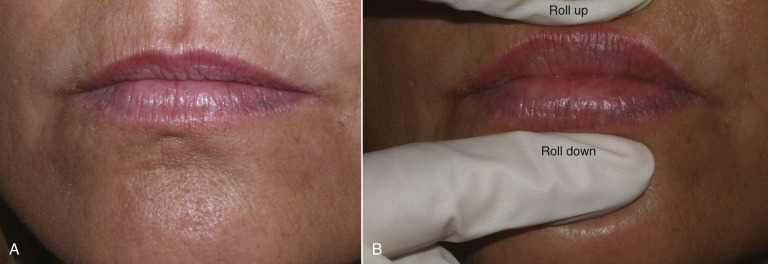
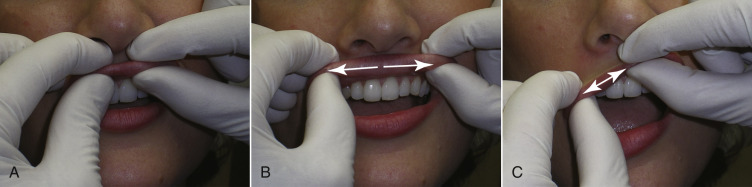
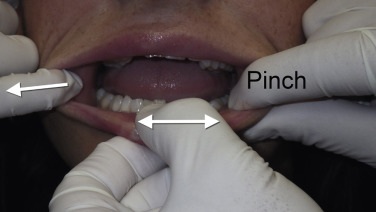
To give the patient an idea of the anticipated result, I use the following method to demonstrate an approximate goal of nasolabial and lip injections. For the nasolabial folds (NLF), I place my index finger lateral to the patient’s nasolabial fold and gently push in on the skin. This elevates the nasolabial fold, simulating an augmentation ( Fig. 10.2 ). I let them know that the fold will improve but not disappear. For the lips, I take both gloved index fingers and roll the upper lip up and the lower lip down. This allows increased vermilion show, similar to injecting filler, to increase pout and volume ( Fig. 10.3 ).
Injection Techniques
Having taught hundreds of injectors over the years, I open my lectures in jest by saying that if you can decorate a cake or caulk a bathtub, you can become proficient in filler techniques. There is actually some truth in this, since there is a distinct similarity of injection pressure and continual movement with the cake and caulk examples. Push the plunger too hard or fail to maintain a continuous motion, and you will get blobs instead of controlled lines. It is this combination of tactile pressure sensation and motion the novice injector needs to develop.
Diagnostic Decisions and Patient Expectations
Although it sounds painfully simple, the surgeon has to:
- •
Ask the patient what changes they desire
- •
Make an accurate diagnosis of the problems that exist
- •
Decide how to treat the situation
- •
Decide how much filler may be required to properly treat the situation
- •
Confirm the patient’s treatment budget.
Patient input is extremely valuable. There have been times when I was about to augment the upper nasolabial fold, and the patient was not bothered by this region but expected lower fold augmentation. The price of the treatment and the expected outcome warrant careful preinjection conversation. The first step in this communication is to hand the patient a mirror and ask them what bothers them and where. The areas are then marked with a soft Kohl eyeliner pencil. This is an invaluable marker, as it is like a grease pencil and marks very easily. It also is extremely easy to remove and can simply be rubbed off with the fingers or gauze. I have never had a tattooing problem when injecting around these marks. If the patient disagrees with the markings, then further communication is necessary.
The next thing the surgeon and patient must address is the specifics of treatment. When a patient presents for “lip filler,” the description is ambiguous. A younger patient may need a small touchup (air in the tires), whereas an older patient may need volume, outline, lipstick lines, and oral commissures treated. The treatment, expense and recovery will be very different in each of these cases. Many patients rely on the surgeon to decide what the problem and treatment will be. Astute surgeons will always make the patient take some responsibility for their diagnosis and treatment.
I begin conservatively with patients who have never had fillers and tell them before injecting them that when we are done, their lips or folds are going to look overdone due to the local anesthesia, the filler, and edema, and will settle in usually by the following day. I further explain that very infrequently, a patient may have unusual swelling that could last for days. Finally, I explain that bruising is very hard to predict; most lip filler patients do not bruise, but some will bruise significantly. I make sure they do not have important social or work plans in the following several days. It is not unusual for patients to desire filler before some event such as a wedding or reunion, and this is a slippery slope in terms of them possibly looking worse (edema and ecchymosis) instead of better. Last minute filler injections before an important function should be discouraged and rescheduled.
Prior to injection, the intended areas of injection are prepped with an alcohol pad or suitable surgical prep and all makeup removed. Makeup particles that become embedded with injection can produce inflammation or irritation.
Anesthetic Considerations
Pain control is of utmost importance. Patient comfort and easing apprehension should be kept in mind throughout the entire procedure, similar to the painless dentistry model. I see numerous patients who were treated elsewhere, had a painful injection experience, and switched offices because of their friends’ comments about how our procedures did not hurt. Never underestimate the power of marketing from painless treatment. Although most contemporary fillers contain lidocaine, I still use topical and local anesthetic injections on all patients. Undoubtedly, anesthesia care takes time and lengthens filler procedures, but this extra time spent will come back to the surgeon many times over in happy, pain-free patients and referrals. I have taken many patients from other offices that did not practice adequate pain control. In addition, a compassionate staff member that holds the patient’s hand or touches the patient in a comforting manner and voice also relaxes anxiety.
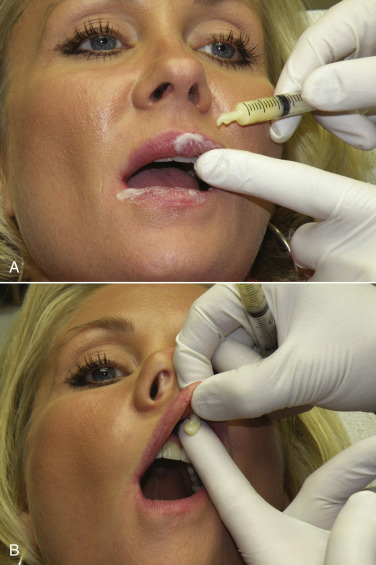
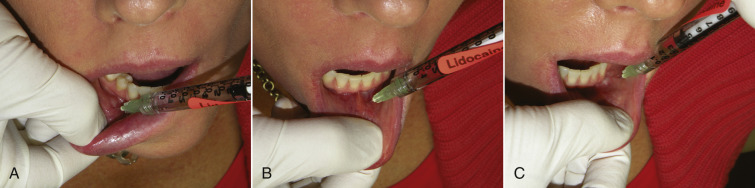
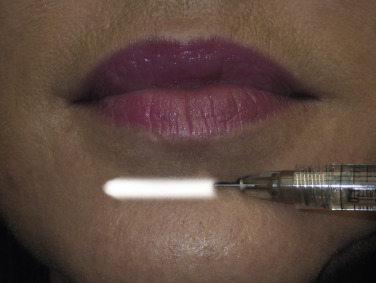
For lip augmentation, topical anesthesia is applied to the external and internal lip and sulcus and on the skin if wrinkles or folds are to be treated. A “BLT” preparation (20% benzocaine, 6% lidocaine, and 4% tetracaine) can be used as can ordinary topical dental preparations. The topical is left in place for at least 5 min. The patient is then allowed to rinse their mouth, as the anesthetic stimulates saliva and will cause numbness in the pharynx, which is disconcerting for some patients ( Fig. 10.4 ).
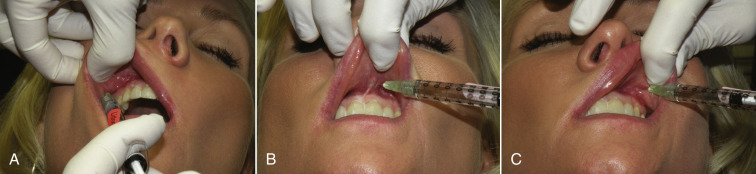
I have heard numerous high profile doctors say that “their patients don’t need supplemental anesthesia.” If that is true it is because the patient doesn’t know better. Although some surgeons employ local anesthetic blocks, I do not use them, because they are more difficult and less dependable than infiltration techniques and numb large areas of the face for hours. Using an infiltration I refer to as the “mini block” technique, a series of injections is performed across the upper and/or lower sulcus. A 1-mL syringe with a 33-gauge needle is used with 2% lidocaine and 1 : 100,000 epinephrine. The epinephrine can be omitted to reduce the longevity of the anesthesia. Lidocaine in 0.2-mL aliquots is injected just above the upper sulcus ( Fig. 10.5 ) and just below the lower sulcus ( Fig. 10.6 ). This is generally performed in four to five areas from the canine tooth on one side to the canine tooth on the other side. The patient is then allowed 5 min for the anesthetic to take action. The local anesthetic will affect lip animation and this is another important reason for marking the patient prior to local anesthesia so landmarks are not lost or distorted. In addition, some of the wrinkles that existed with animation may not be visible if the lip is not moving normally.
Lip-Enhancement Techniques
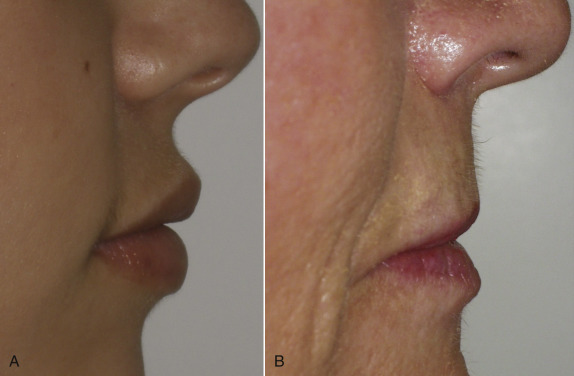
Treating young patients without significant photodamage is usually straightforward. They may simply need a small amount of volume to plump up the lips or some basic vermilion outline for definition. Treating the senescent lip, on the other hand, can be very challenging. The youthful lip is shorter, curvaceous, defined, and volumized ( Fig. 10.7A ). The aging lip lengthens for numerous reasons, including volume loss from skin, muscle, minor salivary gland and fat changes ( Fig. 10.7B ). Loss of tooth structure (attrition) also contributes to postural differences of the lips.
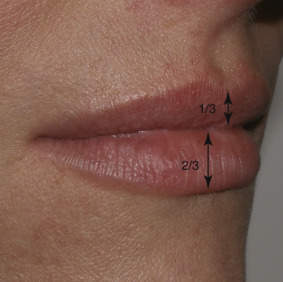
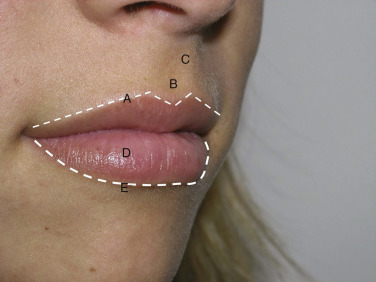
A successful injector is a student of lip form and function and needs to be cognizant of the differences between youthful and senescent lips. In youth, the upper lip constitutes about one-third of the total lip volume, and the lower lip constitutes about two-thirds of the mass. This applies to the “golden ratio” of 1 : 1.61 for the upper and lower lip, respectively. This varies among patients and ethnicity ( Fig. 10.8 ). The youthful perioral region is defined by numerous anatomic components that undergo changes with aging. The astute injector is aware of normal lip volume, outline, philtrum, and philtral columns ( Fig. 10.9 ).
As with many other body parts, some patients exhibit outstandingly aesthetic lips. These patients may exhibit three distinct prominences or tubercles in the upper lip and two in the lower lip. On the upper lip, one “pillow” lies centrally and one is present on each lateral region. On the lower lip, the two prominent tubercles lie on each side of the midline. Some injectors strive to duplicate these prominent regions. My experience is that this looks good on some patients, but most patients feel that the discontinuous tubercles look less aesthetic than simply having full, contiguous lips.
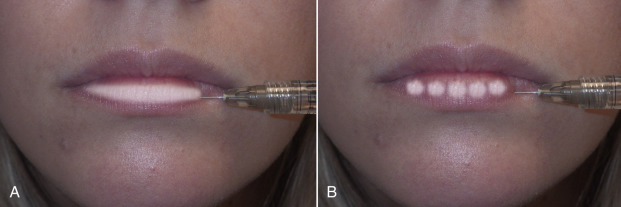
Every practitioner has his or her specific filler injection techniques. The two most popular are linear threading and serial puncture ( Fig. 10.10 ). Linear threading involves inserting the needle and injecting the filler in a straight line while continuously moving in a backward direction. This process would be analogous to placing a line of toothpaste on one’s toothbrush, laying down a seam of calking, or decorating a cake. Although I personally inject while withdrawing, other injectors advocate injecting antegrade to push structures out of the way. I feel that the latter can be more prone to vascular injection. The other injection method is known as the serial puncture technique. This involves placing small boluses of filler with multiple punctures along the lip or wrinkle. In reality, many instances call for a combination of both techniques.
Lip Outline
Each patient is evaluated for specific areas of filler enhancement. Some patients (young and old) lack the specific outline of a “Cupid’s bow” or “white roll.” The Cupid’s bow of the upper lip is a lazy-“M” shape, and the corresponding vermilion/cutaneous border (VCB) of the lower lip is curvilinear. In patients with well-defined lip borders, a pleasing light reflex is visible and contributes to maximum aesthetics. If a patient has adequate lip volume, they may only need border outline, but some patients need both volume and outline as well as vertical rhytid injection.
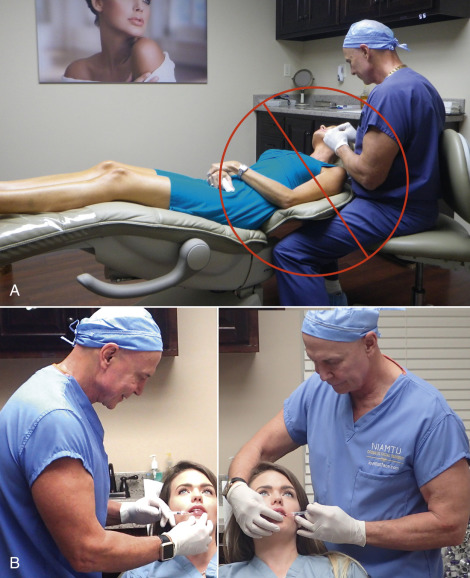
It is important to inject patients in an upright position; gravity will distort a supine patient’s normal anatomy ( Fig. 10.11A ). In addition, many doctors only inject from one side of the chair and this can lead to unrealized asymmetries. It is important to rotate around the patient and inject each side independently for the most accurate results ( Fig. 10.11B ).
While performing any injection of any product in or around the face, the injector should have expertise on vascular anatomy and injection techniques. As stated earlier, intravascular injection can and has caused blindness, stroke, and severe tissue loss.
Creating the Vermilion Outline
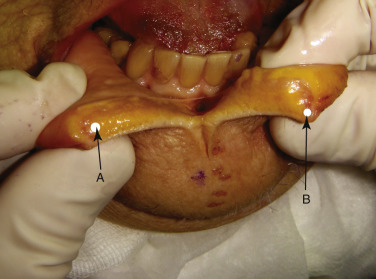
When injecting the lip borders for outline, needle placement is critical. A potential space exists between the mucosa and orbicularis oris muscle, and this space is the target of border outline ( Fig. 10.12 ).
Injecting in this target space is both visual and tactile. When the needle is in the correct plane, the filler will visually flow both antegrade and retrograde. This can be seen and also palpated by the non-injecting hand. By pinching the border between the non-injecting thumb and index finger, the injector can feel the free-flowing filler, as well as confine the filler to stay within the border. If the needle is in the correct plane (the described potential space), the filler will flow freely with minor syringe pressure. This is confirmed by observing the border being properly created. If the needle is too deep, no distinct outline is seen. If the needle is too superficial, the filler will not flow but instead “ball up,” and the syringe pressure will increase. In this case, the needle must be redirected into the proper potential space.
When augmenting the vermilion border for outline or white roll enhancement, I begin with the central “V” of the Cupid’s bow. The finger and thumb contain the filler and assist in palpation of the augmentation ( Fig. 10.13 ). If the patient does not have a well-defined Cupid’s bow, it is drawn with a marking pencil before the injection to serve as a guide for filling. Care is used to form crisp, angular contours in the downward legs of the lazy M in the area of the central lip.
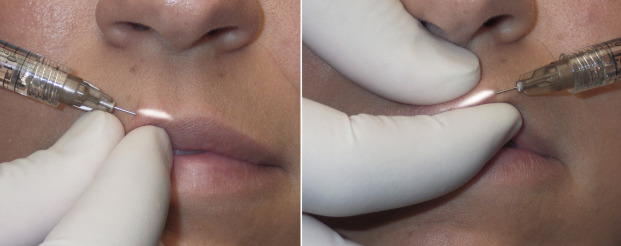
The next step is to continue the vermilion outline augmentation laterally across the entire upper lip ( Fig. 10.14 ). Some patients require the white roll to extend all the way to the commissures while others only need this augmentation more centrally and gently tapering several millimeters short of each commissure. The needle is inserted all the way to the hub, and the filler is injected with even syringe pressure upon withdrawal. Most filler needles are half an inch long, and the border is augmented at half-inch intervals, taking care to not leave a gap between needle insertion points.
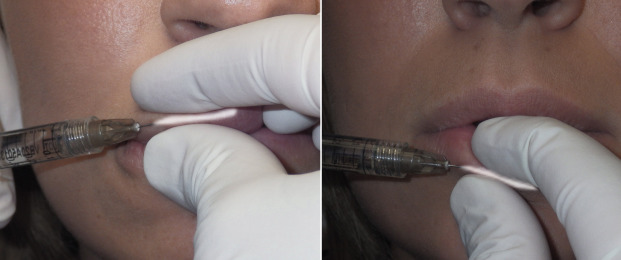
The white roll is similarly created in the lower lip, which is more curvilinear than in the upper lip ( Fig. 10.15 ). Reestablishing the light reflex accentuates the lip form and outline, especially in women that wear shiny lip gloss.
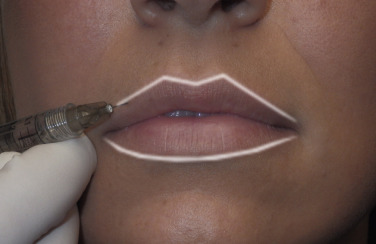
A single syringe is usually more than adequate to outline the vermilion on both lips. The lower-lip central vermilion outline is a small but powerful augmentation. Outlining the vermilion border in both lips as described is sometimes all a patient needs for lip enhancement, especially those who do not desire larger lips. Many patients also require “plumping” by adding volume to the central lip.
Increasing Lip Volume (Pout)
Although vermilion border augmentation is a powerful means of enhancing the lip, many patients have adequate outline and a defined white roll or Cupid’s bow and do not require outline. The most common presentation in my practice is the patient who presents with the desire for more lip volume. These patients request plumper, fuller, pouty, and more voluptuous lips. Many are younger and already have adequate vermilion border. These patients will benefit from deeper fill that will increase the general lip volume and pout. By augmenting the deeper portion of the lip, the actual lip will roll out and produce increased pout. The target for volumizing the lip is basically the center of the lip. This is deep to the muscle and contains connective tissue, minor salivary glands, and fat ( Fig. 10.12B ). For younger patients with minor volume loss, I describe this as “putting a little air in the tires.” A single syringe split between both lips can reestablish youthful volume. Older patients will require more filler and it is not uncommon to use two syringes for plumping.
When volumizing, the needle is inserted at the wet/dry line, deep into the central lip. The center of the lip is generally a safe plane, because the labial artery lies at the posterior third of the lip. The target for injection when performing deep volumization is the central lip. Central lip refers to the deep tissues midway between the outer mucosa and skin and the intraoral mucosa, literally the center of the lip when considering the lip in cross-section, as shown in Fig. 10.12A . The needle and filler is anterior to the labial artery and is generally a safe zone (see Fig. 11.1 ). The needle is inserted to the hub and slowly withdrawn while continuous, steady injection is performed (linear threading). In this area, the goal is to produce a “tube” of filler to enhance the volume ( Figs. 10.12B and 10.16 ). As noted earlier, some injectors reproduce the prominent lip tubercles seen in some aesthetic lips, and instead of a continuous tube of filler, the tubercles are reconstructed by placing three boluses in the upper lip and two in the lower lip. Some patients have atrophic lips that require projection of the region from the nose to the vermilion. This region can be injected with filler to increase the pout in conjunction with conventional lip fill, as described above.
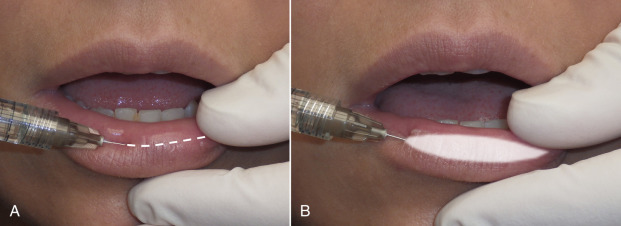
After filler is injected, the region is inspected for symmetry and fill. I strongly believe massaging the injected filler is a critical (and often overlooked) step in obtaining natural and aesthetic results. Most fillers have the consistency of soft gels or paste and when injected, will not always be homogenous. Massaging the filler more evenly distributes and forms it and produces a smoother, more homogenous result ( Fig. 10.17 ). In addition, the injector can actually level out an area of excess by moving the filler through the tissues. My assistant keeps a small bolus of petroleum jelly on the back of her glove during all filler injections, and I dab this and coat the lip and skin just prior to massage.
Some injectors carry vermilion and deep volume injections all the way to the corner of the mouth, but I generally do not. In my opinion, one of the most common unnatural filler results is the “ducky” lip, due in part to an eversion of the lateral lip reminiscent of the familiar rubber duck bath toy, which is unfortunately visible on many female celebrities ( Fig. 10.18 ). This can be a variable decision, as some patients benefit from mild to moderate fill all the way to the commissure and others do not.

Lip Injection Cannula Technique
Another convenient means of deep lip volume augmentation is using a specially designed blunt rounded injection cannula instead of the standard half-inch needles that are supplied with filler. Numerous companies produce disposable, flexible 4-cm, blunt cannulas with the orifice set proximal to the tip. These cannulas have a standard Luer Lock connection and are packaged with an “entry” needle of the same gauge ( Fig. 10.19 ). They are blunt and therefore less traumatic, flexible for better negotiation, and can be used in virtually any filler application as conventional needles. Many injectors have switched to using cannulas only. I prefer a 23-gauge cannula for most filler applications.
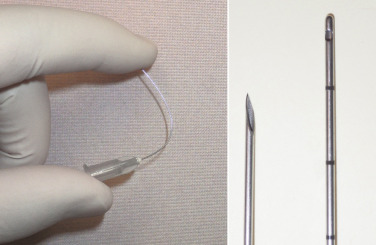
Many clinicians feel that cannulas have numerous advantages over needle injection. The tip is blunt and easily moves through the lip without lacerating tissues and vascular structures and therefore produces less bruising and swelling. This type of blunt cannula may reduce the chance of intravascular injection, but this has still been reported with cannulas. In addition, this technique only requires a single puncture. The cannula is passed through the entirety of the lip, negating the need for multiple needlesticks. The size of the cannula and orifice allow a larger deposition of filler with minimal syringe pressure, making the injection process much faster. Since the cannula is blunt, an entry point is first made with a supplied half-inch 22-gauge needle at the lateral lip ( Fig. 10.20 ). The cannula is inserted into the puncture and threaded through the center of the entire lip ( Fig. 10.21 ).
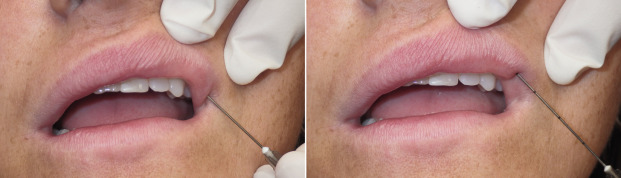
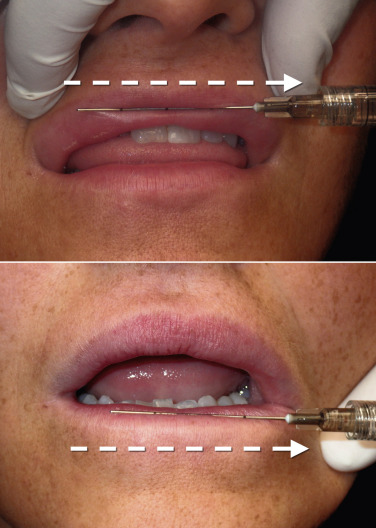
The filler is then injected in a single smooth action while simultaneously withdrawing the cannula. Since more filler is deposited in the center than at the lateral border, the syringe pressure is increased as the midline is approached to deposit more filler, and then backed off as the cannula approaches the puncture insertion point. This forms a natural taper from one side across the center to the other side ( Fig. 10.22 ). The same procedure is performed on the other lip in most cases. Some patients require increased pout and this can be accomplished by injecting filler (with cannula or needle) in the cutaneous portion of the lip (the area under the nose and above the vermilion). This cutaneous augmentation can produce an extremely aesthetic lip, especially in the lateral view.
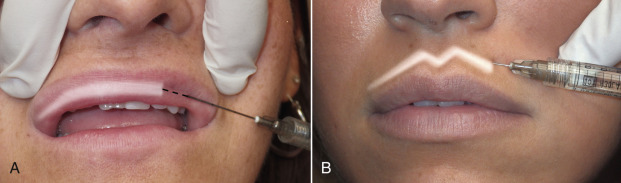
The final step is to massage the filler. Since a puncture hole was made one commissure, it is important to pinch this hole when massaging, so the filler is not expressed out of the hole when massaging toward that side. It is helpful for the assistant to place their little finger in one commissure to stretch the lip, which facilitates the massage ( Fig. 10.23 ). As noted, having a dollop of petroleum jelly on the back of the assistant’s hand is convenient for lubricating the mucosa and skin for massage, without interrupting the process. Some injectors also use the cannula for vermilion outline as well as deep volume injection.
Perioral Filler Techniques
Philtral Columns
Although the lips are frequently the requested region of improvement, there are numerous perioral indications that can make patients look younger as well as enhance the result of the lip augmentation. Philtral column enhancement is one of the most overlooked aspects of lip rejuvenation. It may never occur to many injectors to address this region, and others may be intimidated. The philtrum is a subcolumellar depression with well-defined columns on either side . In youth, this complex is angularly defined and contributes to youthful aesthetics. As we age, the architecture of these structures frequently changes, and the central upper lip becomes devoid of this pleasing topography. In treating this area, the injector can enhance existing philtral columns or create new ones.
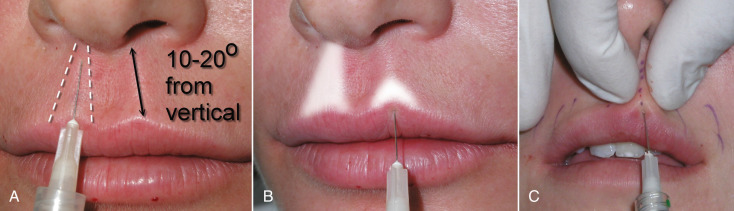
The philtral columns are not vertically straight but rather at a 10–20 degree angle from vertical; the base of the column is lateral to the tip ( Fig. 10.24A ). There are numerous ways to augment the philtral columns. A very simple technique is when treating the lips, conserve the last bit of filler in the syringe and simply place a small peak at the vermilion cutaneous junction at the base of the existing column. This filler is injected in the dermis while the other hand pinches the skin to allow a triangular deposition. This technique does not extend superiorly up to the nostril, but rather becomes a small peaked extension of the angular Cupid’s bow. It only takes a small amount of filler to create this peak and in younger patients it gives the semblance of normal anatomy without treating the entire column. For older patients or those with no defined philtral columns, a more complete reconstruction can be performed. The goal is to replicate the normal angled, conical-shaped philtral column. This is merely a bigger version of the previously described technique but more aggressive; it extends to the nostril just lateral to the columella on both sides. It is important to keep the column tapered and angled 10–20 degrees to appear natural. Pinching the upper portion of the skin helps create the taper ( Fig. 10.24B ).
Vertical Lip Rhytids
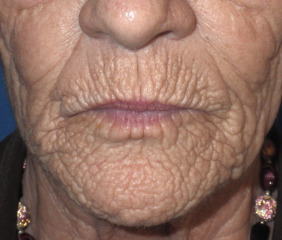
Vertical lip rhytids (lipstick lines) bother women significantly. This is one of the most commonly requested perioral procedures and one of the more difficult conditions to remedy. These vertical lines are problematic from the standpoint of aesthetics and due to the fact that applied lipstick will leech out and follow the lines onto the skin. These lines are perpendicular to the orbicularis oris muscle and are largely a result of this muscle’s function over the years. Lip rhytids can be vertical, angular, and radial ( Fig. 10.25 ). It is suggested that men are less affected because they have more and denser hair follicles in the lips. Smokers and chronic drinking from a straw probably accelerate formation.
I personally feel that vertical lip rhytids represent one of the greatest challenges of lip rejuvenation. Patients must understand that the wrinkle can be improved at rest but is usually better but visible during animation. To truly improve vertical lipstick lines they are injected in conjunction with lip volumization or vermilion outline. One commonly encountered problem is that many older women have lipstick lines but do not want “bigger lips.” They refuse any other filler except treatment of the actual lipstick lines. This ties the hands of the injector, as it is difficult to improve the entire situation with only localized wrinkle injection.
Patients with severe lines are best treated with combination therapy, with Botox, filler, and laser resurfacing. Patients must understand that these lines will not be eradicated, but rather mitigated. Although lines can be individually injected, this procedure has the liability of creating a series of “speed bumps” or ridges across the lip.
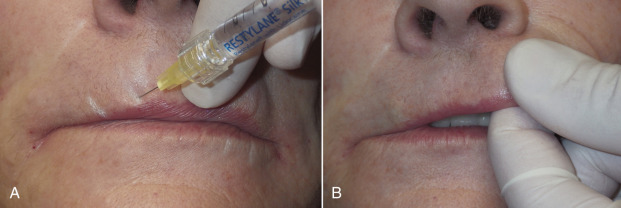
My preferred method for treating vertical lip rhytids is to first volumize the lips with deep fill and outline. Virtually all patients who have enough aging to have lipstick lines also have generalized volume and vermilion border loss. It is explained to the patient that by restoring volume and border to the lip, the skin will stretch and improve the appearance of perioral lines. After the lip is plumped and the white roll reestablished, the lipstick lines are injected. Low G prime and less viscous fillers such as Restylane Silk, Volbella, and Belotero perform well in this area as their target is superficial dermis. The needle is inserted barely into the dermis and a small bolus of filler injected. This bolus is then massaged over the length of the vertical wrinkle, which smooths it ( Fig. 10.26 ).
Figs. 10.27–10.32 show before and after images of lip augmentation with injectable fillers.
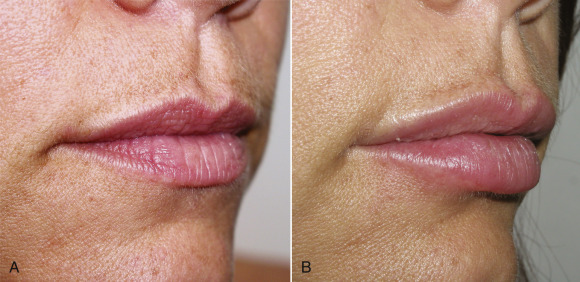
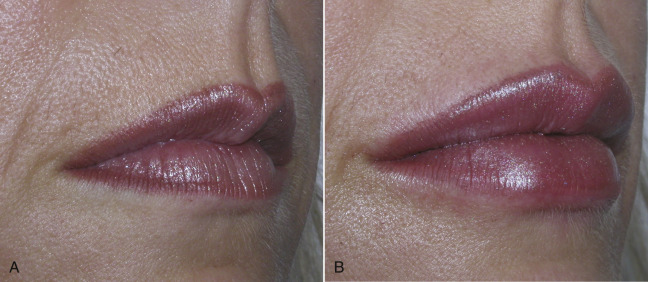
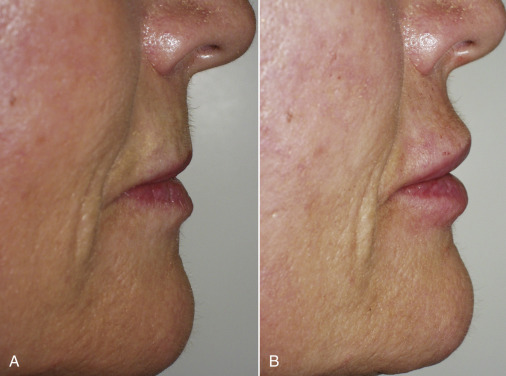
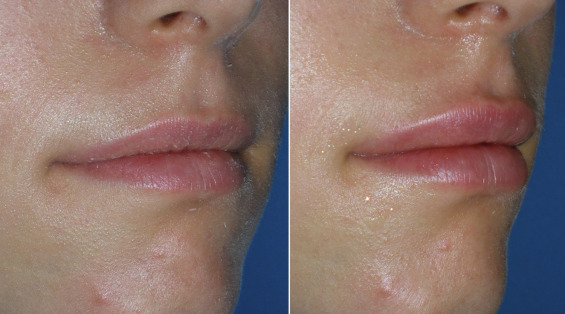
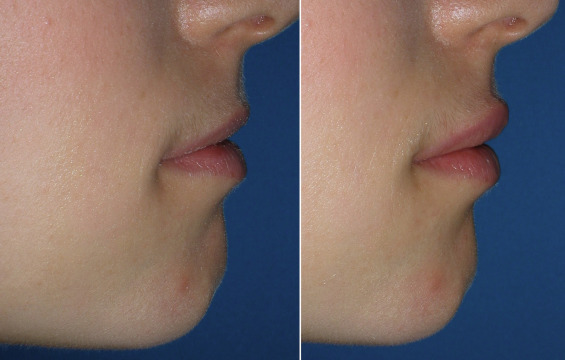
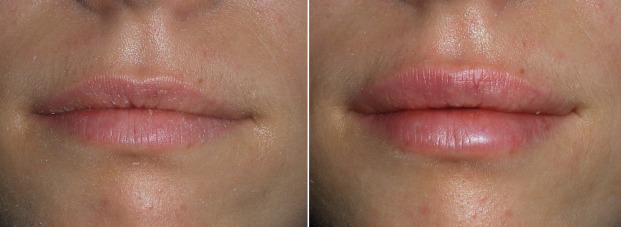
Most patients with lipstick lines also have melomental (marionette) lines, downturned oral commissures, and generalized volume loss of the lips along with photodamaged skin. To improve these more severe cases, a significant amount filler can be required, but frequently, this age group is averse to spending a lot of money to correct this region.
Oral Commissure Injection (Downturned Corners of the Mouth)
When addressing the perioral region for filler rejuvenation, the corners of the mouth are a commonly requested treatment area. This can be a difficult region to enhance and can be a “black hole” for filler, requiring a lot of product. Due to the numerous muscles merging at the modiolus, this is a complex anatomic area. Many patients also have a dimple in this region that is accentuated upon smiling. It is important for these patients to realize that although the commissure may be improved in repose, the dimple and hence the depression may still be visible when smiling or animating. Most young patients have crisp, tight, horizontal, or upward-turning oral commissures. As patients age, tooth structure is lost, which decreases the vertical dimension of the jaw. Tooth attrition also causes overclosure of the jaws, which increases the perioral soft tissue drape and in part results in downturned oral commissures ( Fig. 10.33 ). Also contributing to this aging is muscle atrophy, loss of fat, photoaging of the skin, and jowling. Older patients with heavy jowls can have very deep melomental folds (or marionette lines) and be under the impression that the filler will lift and improve the jowl. It is imperative to explain to the patient the best and worst case scenario for treatment result, so they can have a reasonable idea of what to expect. One of the most hated aging changes is “permafrown” or downward turning corners of the mouth. This is one aging change that can be dramatically improved with neurotoxins and fillers.
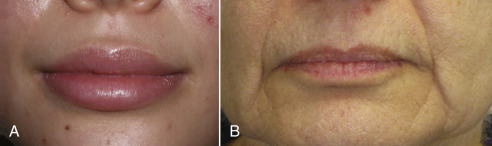
Patients with severe tooth wear or dentures may need to have their vertical dimension increased by a restorative dentist or have dentures remade to lengthen the intermaxillary space.
Combining neuromodulator (neurotoxin) treatment of the depressor anguli oris muscle with injectable fillers in the area can be symbiotic. When injecting the commissure, it is important to control the flow of the filler, as it has a tendency to spread laterally in this region. If the injector is not cognizant of this, lateral pouches can form, which worsens the deformity ( Fig. 10.34 ).
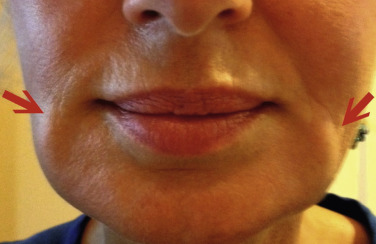
Numerous injection techniques are used to treat the oral commissures or the melomental folds and in my opinion, both regions need simultaneous treatment for maximum improvement. Some patients may present with a downturned commissure but without deep melomental folds and just the corner of each lip can be treated. More often, a “hockey stick” configuration is formed by the horizontal commissure and the vertical melomental fold; treating both of these regions simultaneously is the key to improving them separately ( Fig. 10.35 ).
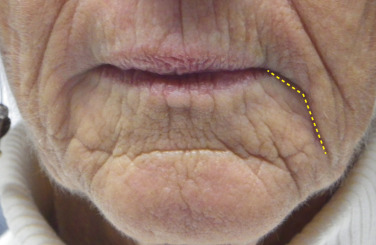
In the described dual deformity the melomental fold is treated first to establish a base or pillar to support the sagging commissure. As stated earlier, filler can have a tendency to migrate laterally, so the injector must carefully control the deposition. To create a base, a broad band of filler is placed in the deeper subcutaneous tissues under the fold. A second layer is placed in the mid-subcutaneous layer and a final layer is placed in the dermal layer ( Fig. 10.36 ).
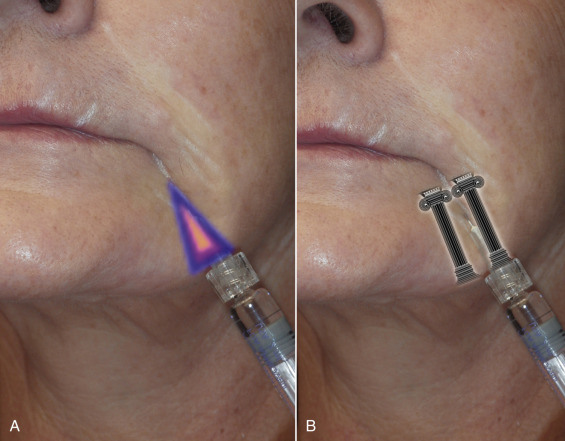
The nasolabial fold and melolabial fold can also be treated with a flexible blunt cannula. Some patients can be treated solely with the cannula ( Fig. 10.37 ). Extremely deep folds may also require intradermal injection with a needle. The cannula can be used to create the base and the needle used to finish the augmentation intradermally.
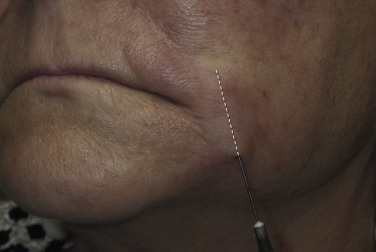
Once the melolabial fold has been addressed, the depressed or downturned commissure is treated. A small amount of filler can be injected directly into the fold in the commissure but this is a region where the filler can move laterally, so only a small amount is injected. The goal is to fill this crevice and upturn the corner of the mouth without creating a puffy appearance.
After a small amount of filler is placed directly in the commissure, the distal corner of both lips are filled at the commissure. It is important to have a distinct angle at the commissure and this also helps elevate the mouth corners ( Fig. 10.38 ). Fig. 10.39 shows a patient with severe aging of the commissures and melolabial regions before and immediately after injection. These techniques of establishing the melomental pillar and filling the lip corners are used to elevate the commissures. It is important to stop after filling the first side and show the patient the result ( Fig. 10.40 ). The reason this is done is to they can appreciate the difference. If both sides are treated before the patient looks in the mirror they may not be able to note the significant difference. Figs. 10.41 and 10.42 show actual cases, where I stopped on the first side to show the patient the difference.
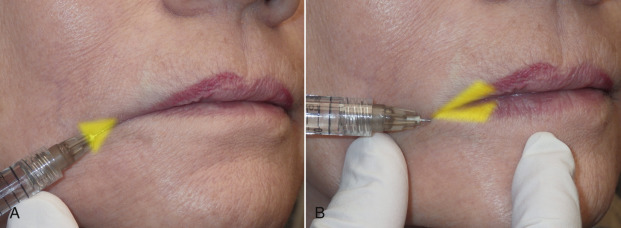
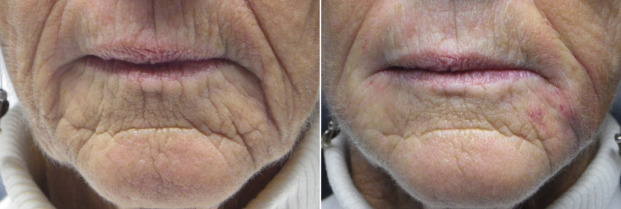
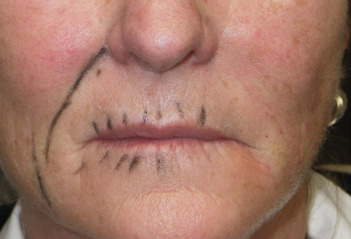
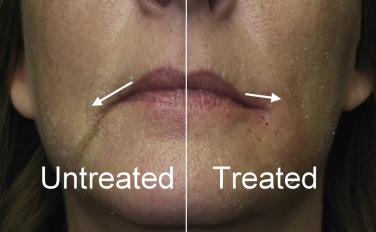
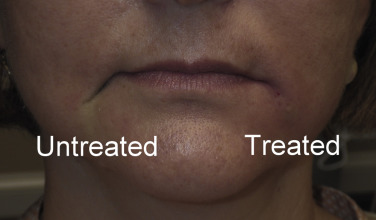
Although most filler injection is performed solely for aesthetic reasons, there is a functional application for commissure and melomental fold treatment. Filler in this region can improve or sometimes prevent Candida albicans infection. Angular cheilitis (also called “perlèche”) is a common irritation/infection in the oral commissure area and can extend into the melomental folds. This occurs when “drool lines” form and entrap saliva, which causes irritation and creates a “yeast-friendly” environment. This is especially common in older patients who have skeletal and dental tissue loss that collapses the soft tissues. This is treated with antifungal medications, but in the presence of deep or redundant soft tissue, it can be very resistant.
By filling the crevices, there is less moist, deep, and dark yeast-friendly areas. Fig. 10.43 shows a before and after filler injection for perioral rhytids that were associated with angular cheilitis. The condition cleared within 1 week after filling.
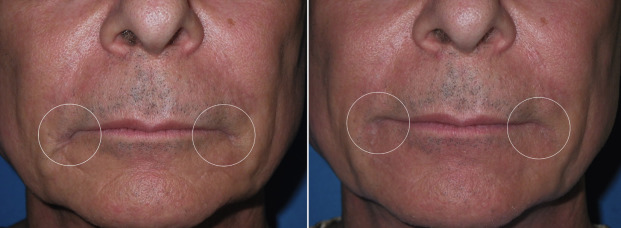
Filler Injection for Facial Balance
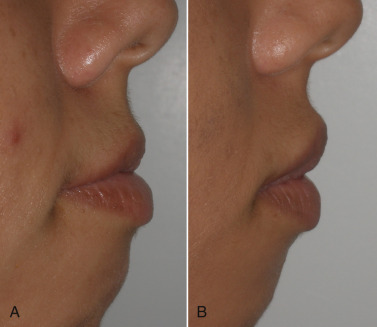
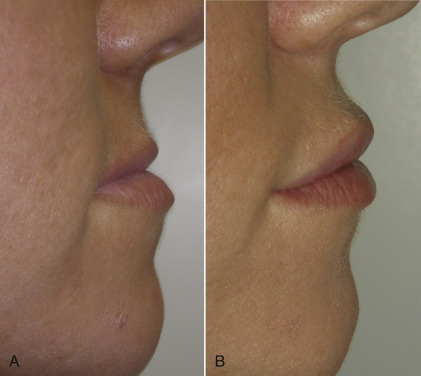
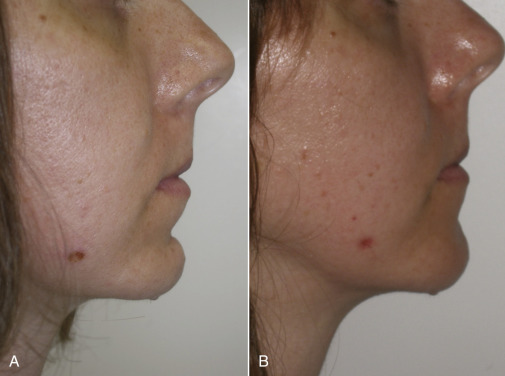
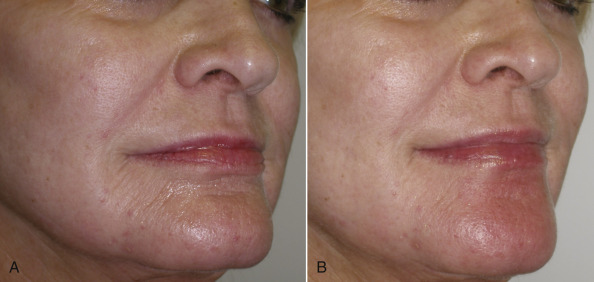
Facial fillers can be used to balance minor facial disharmonies such as mandibular prognathism or maxillary hypoplasia. This is accomplished by enlarging the deficient region. Besides augmenting the vermilion, the skin above the lip is also injected to improve projection (see Fig. 10.22B ). Figs. 10.44 and 10.45 show before and after results of patients with a deficient maxilla and the upper lip posterior to the lower lip before and after correction.
All lip injections (and all filler injections) are immediately treated with ice after augmentation, and the patient is encouraged to ice the area for several hours. A commercial crushed ice machine is one of the best investments I have made in my practice.
Augmenting the Mentolabial Fold
The mentolabial fold represents the region below the lower lip and above the chin. In youth, this fold has a pleasing S curve that deepens with aging. In addition, this fold is greatly affected by the position of the jaw, chin, and teeth. In patients with microgenia, retrognathia, or lower facial vertical-third height deficiency, this fold can be very deep, with an overhanging lower lip. Some patients present with a simple deepened fold from aging and, as in any other facial fold or wrinkle, the region is augmented with filler ( Fig. 10.46 ). A deep fold can take several syringes to correct or improve. The first injections are placed in the deeper subcutaneous regions to buttress the augmentation, and the remaining injections are layered in the mid-subcutaneous layer and finally in the dermis. This layering support can significantly improve the depression, lift the ptotic lip, and give an appearance of increased lower facial third vertical height ( Figs. 10.47 , 10.48 ).
Midfacial Filler Treatment
Filler Augmentation of Nasolabial Folds
The nasolabial folds (NLF), which are sometimes called the melolabial folds, are very popular injection options and treatment is faster and has fewer nuances than the lips. The nasolabial folds are a complex anatomic structure caused in part by the merging of various tissue planes from skin to bone. The descent of the malar fat pad, decades of facial animation, and numerous other factors influence the deepening of the NFL.
Before treating this area, it is important to give the patient an accurate idea of what to expect and an opportunity to provide their own input, as to how they want the fold changed. In most adults, the fold extends from the lateral nasal region and can merge with the melomental folds (marionette lines). Other patients exhibit anatomy where the NLF merges with the “smile dimples” lateral to the oral commissures. Some patients desire augmentation high on the fold to correct the paranasal depressions, whereas this region does not bother other patients, whose desire may lie in augmentation lower on the fold or even in the perioral region. I explain that the NLF will not “go away”; our goal is to soften it. I further explain that the NLF is a valley, and we want to blunt the fold, not eliminate it. Finally, I never inject an adult with a single syringe of product. In reality, most adults in their fifth decade could easily accommodate three or four syringes. Filler is expensive and it is only natural for patients to want to economize. The pre-filler consult and communication can be as important as the final result.
When treating the NLF, all makeup is wiped off with alcohol, the folds are marked, and topical anesthesia is applied to the skin. I am an absolute proponent for painless injections and I use local anesthetic infiltrations for all filler injections. The anesthetic technique for the NLF is simple. A 1-mL syringe with a 33-gauge needle (same set up as neurotoxins) is used with 2% lidocaine with 1 : 100,000 epinephrine. We keep a container of these filled syringes in each treatment room, since we use them for many procedures. When using local anesthesia for folds or wrinkles, it is important to inject it deep to prevent distorting the anatomy of the fold or wrinkle, which can affect the accuracy of the result. I generally inject 0.1 mL of local anesthetic at several points along the fold. The first injection is in the area of the nasal ala (a painful region to inject filler), another injection is placed in the mid-fold, and frequently a third injection is placed at the inferior portion of the fold. I make a point to the patient that pain control is very important in our practice and this has paid off many times over in new referrals. The skin does not need to be totally numb, only enough to take the edge off the discomfort.
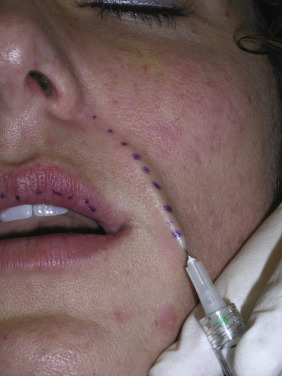
Patients should not be positioned supine for filler injections because gravity will significantly affect the anatomy of the fold, making accurate treatment difficult. I use a combination of the two methods of linear threading and serial puncture for treating the NLF. Needle position is important, as injecting too deep will not improve the fold and injecting too superficially can produce a bumpy or unnatural appearance. In younger patients, an intradermal injection plane is acceptable to improve a shallow fold ( Fig. 10.49 ). In patients with moderate aging changes, a deep dermal/subcutaneous and superficial dermal layer may be warranted. In older patients with deeper folds, I prefer to layer the filler in three planes. I first perform a deep subcutaneous layer to provide a base, then more superficial subcutaneous injections to create midlevel support, and finally dermal injections to fill the surface layer ( Fig. 10.50 ). The combination of this layering improves longevity and result, as it addresses the fold in multiple layers.
Some patients have paranasal depressions on the lateral nose at the superior portion of the fold and request treatment in this area as well. This is a normal anatomic contour, even in young people, so complete filling is not usually advisable. Older patients, denture patients, or patients with maxillary deficiency may benefit from filling this area. It can be filled as an isolated area but more commonly in conjunction with the entire fold ( Fig. 10.51 ).
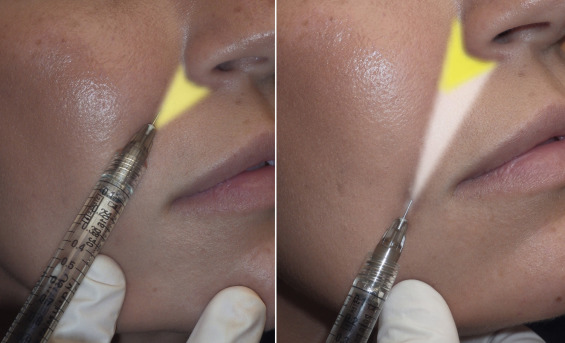
A huge pearl to remember when treating the NLF (or any fold or wrinkle) is that if you cannot see immediate improvement, the needle is probably in an incorrect plane. Many novice injectors place the filler too deep and it does not plump out the fold. If immediate noticeable improvement is not seen, the needle needs to be positioned more superficially. Due to the unique anatomic planes of the NLF, even while injecting in the center of the crease, the filler can migrate laterally and create a lateral ridge ( Fig. 10.52 ). This can actually make the NLF bigger. If the filler migrates laterally during the injection, the needle is directed more medially before continuing the injection. Remember with this, what you see is what you get.
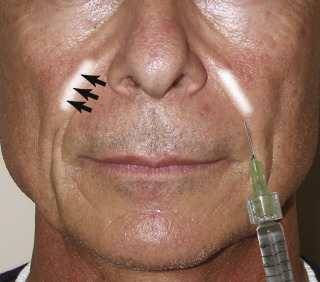
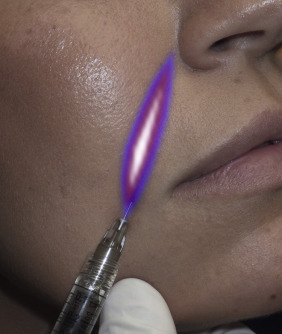
Another means of facilitating NLF filler is to put the cheek on stretch with the non-injection hand. This tension will turn a curvilinear structure into a straight line, making it easier to inject ( Fig. 10.53 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree