Gastroschisis and Omphalocele
Jamie C. Harris
Fizan Abdullah
DEFINITION
Gastroschisis
Gastroschisis is the most common congenital abdominal wall defect in the newborn period. This results from failure of the intestines to return back into the abdomen during development around week 10 of gestation.
The abdominal wall defect is usually less than 4 cm in diameter and is more commonly located to the right of midline.
Omphalocele
Omphalocele is the second most common abdominal wall defect, 1/5000 live births.
This is characterized by a large defect, greater than 4 cm, and is covered by a membrane of peritoneum.
This can contain intestines, as well as liver, spleen, and gonads. Unlike gastroschisis, omphalocele has a high rate of associated anomalies, including chromosomal abnormalities and cardiac defects.
DIFFERENTIAL DIAGNOSIS
Ruptured omphalocele can be distinguished from gastroschisis based on the size of the defect (greater than 4 cm), as well as contents other than intestines in the defect.
An umbilical cord hernia will be smaller than omphalocele, and does not contain abdominal organs.
Pentalogy of Cantrell is a rare constellation of ectopia cordis, omphalocele, sternal cleft, anterior diaphragmatic hernia, and intracardiac defect.
In ectopia cordis, the defect is located at the midline of the sternum and contains the heart.
Patient History and Physical Findings
Prenatal history
Often, abdominal wall defects are diagnosed on prenatal screening. Maternal serum and amniotic fluid demonstrates elevated alpha fetoprotein (AFP).
Amniotic fluid demonstrates elevated acetylcholinesterase.
There is a higher specificity of elevated AFP for gastroschisis compared to omphalocele.
Postnatal history and physical (FIG 1)
For both defects, birth history as well as patient stabilization from a cardiopulmonary standpoint should be completed first.
Initial inspection should be done to determine:
The presence of a covering membrane (indicating omphalocele) (FIG 1A).
The viability of the intestines, evidence of necrosis, atresias, or perforation.
Contents in the defect, including liver, gonads, and other intra-abdominal organs.
If these are seen without a covering membrane, ruptured omphalocele should be considered.
Full cardiopulmonary exam should be done to determine if there are audible murmurs appreciated, which suggest an underlying cardiac defect.
Examination of the rest of the body to examine for any associated anomalies should be done.
Omphalocele is associated with multiple different syndromes including Beckwith-Wiedemann (omphalocele, macroglossia, and gigantism), and trisomy 13, 18, and 21.1
IMAGING AND OTHER DIAGNOSTIC STUDIES
Prenatal ultrasound
Gastroschisis
Prenatal ultrasound will demonstrate intestines within the amniotic fluid, outside of the abdomen.
This is most commonly seen around 20 weeks of gestation.2
Anomalies, most commonly intestinal atresias, can also be identified on prenatal ultrasound. Bowel dilatation greater than 14 mm is predictive of atresias.1
Omphalocele
Intestinal contents will be seen outside of the abdomen.
The sac can be visualized on ultrasound, helping distinguish from gastroschisis.
Additionally, liver can be visualized in the defect.
This is seen around 18 weeks of gestation.
Evaluations of other associated anomalies, including cardiac, can be done on prenatal ultrasound as well.
Postnatal echocardiogram
The rate of cardiac anomalies in omphalocele is higher (14%-47%) than in gastroschisis (3%-33%).3
Common cardiac anomalies that are seen are ventricular septal defect, atrial septal defect, and tricuspid atresia. A complete cardiac evaluation for omphalocele should be done in the perinatal period.
SURGICAL MANAGEMENT
Preoperative Planning
Gastroschisis
There are two management strategies for gastroschisis:
Delayed closure with silo placement, allowing for reduction of the abdominal contents over the following days
Immediate reduction with closure at birth
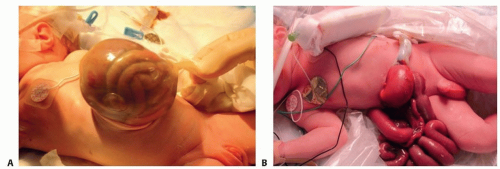
FIG 1 • A. Omphalocele presents with a membrane covering and the umbilicus originating from this membrane. B. Gastroschisis presents with a defect in the abdominal wall without a membrane covering the extruded intestines.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree

 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access