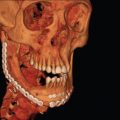
Abstract
Fractures of the condylar process of the mandible are common injuries. The treatment is controversial because they can be treated closed or open. This chapter will discuss these fractures and the methods by which they can be successfully treated.
Keywords
mandibular condylar process fractures, condyle fractures
Background
Approximately 11%–50% of all facial fractures and 30%–40%% of all mandibular fractures (MFs) are fractures of the mandibular condyle. Most are not caused by direct trauma, but follow indirect forces transmitted to the condyle from a blow elsewhere, usually in the body or symphysis region. They are often the result of rapid deceleration injuries such as when the chin of an unrestrained passenger in a car strikes the dashboard, the bicycle rider who lands on their chin, or a patient who falls on their face.
Surgical Anatomy and Clinical Presentation
The four main components of the temporomandibular joint that are important when considering condylar process fractures are the condylar process itself, the glenoid fossa of the temporal bone, including the articular eminence, the intraarticular disk, and the lateral pterygoid muscle. For purposes of this chapter, it will be assumed that the glenoid fossa and temporal articulations are uninjured.
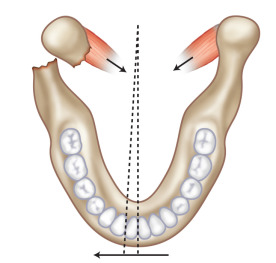
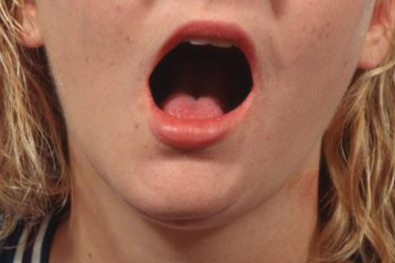
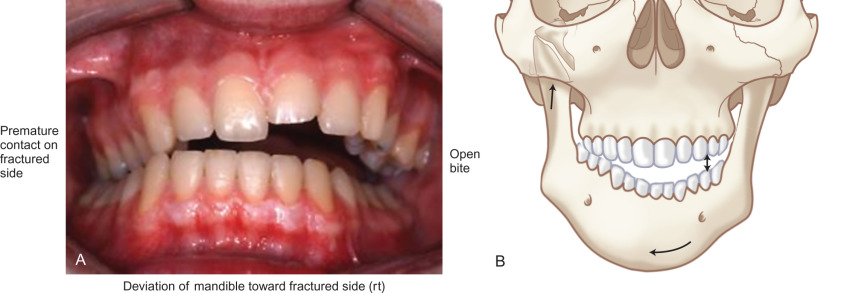
Because the lateral pterygoid muscle inserts mostly onto the pterygoid fovea of the condyle, when a fracture occurs below this level, contraction of the muscle causes the condylar fragment to be displaced anteromedially. For the same reason, condylar fractures are associated with impaired translational movement of the condyle along the articular eminence because the lateral pterygoid muscle is no longer connected to the distal portion of the mandible ( Fig. 1.15.1 ). Although rotation can occur, lack of translation produces a characteristic deviation of the chin on opening toward the side of a unilateral condylar fracture ( Fig. 1.15.2 ). Displacement of the condylar process produces a loss in the anatomic height of the ramus, which allows premature contact of the ipsilateral most distal tooth ( Fig. 1.15.3 ). The point of contact acts as a fulcrum and produces a characteristic open-bite on the side opposite of a unilateral fracture ( Fig. 1.15.3 ). Bilaterally displaced fractures of the condylar processes produce a symmetric anterior open-bite ( Fig. 1.15.4 ).
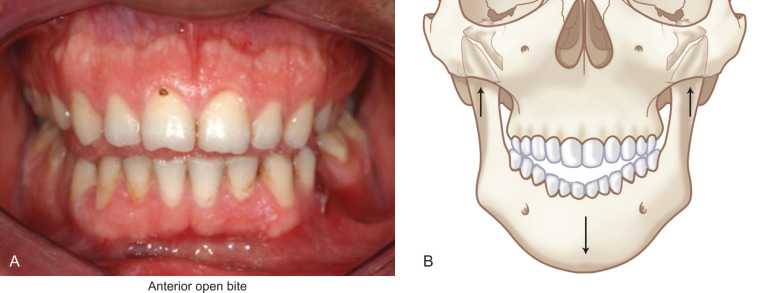
Some patients who sustain mandibular injury may present with pain in the joint and a malocclusion where the mandible comes forward on the side of the injury or they may not be able to bring the teeth together on that side and yet a fracture of the condylar process cannot be identified on imaging. In such instances, one should suspect a contusion/hematoma within the affected joint.
Radiological Evaluation
The vast majority of condylar process fractures in adults can be identified using plain radiographs. It is important to get at least two radiographs 90° to the other. For instance, the combination of panoramic and Towne’s projections offer most of what might be needed to prescribe treatment in the vast majority of patients ( Fig. 1.15.5 ). Plain films are not as useful for pediatric condylar process fractures because the bone is less dense, the condylar neck is much shorter, and often the fractures are through the condylar head, which are not revealed well with plain films. On the other hand, if the surgeon routinely treats condylar process fractures in children closed, the need for more detailed imaging (CT) may not be warranted given the need for more radiation to do so.
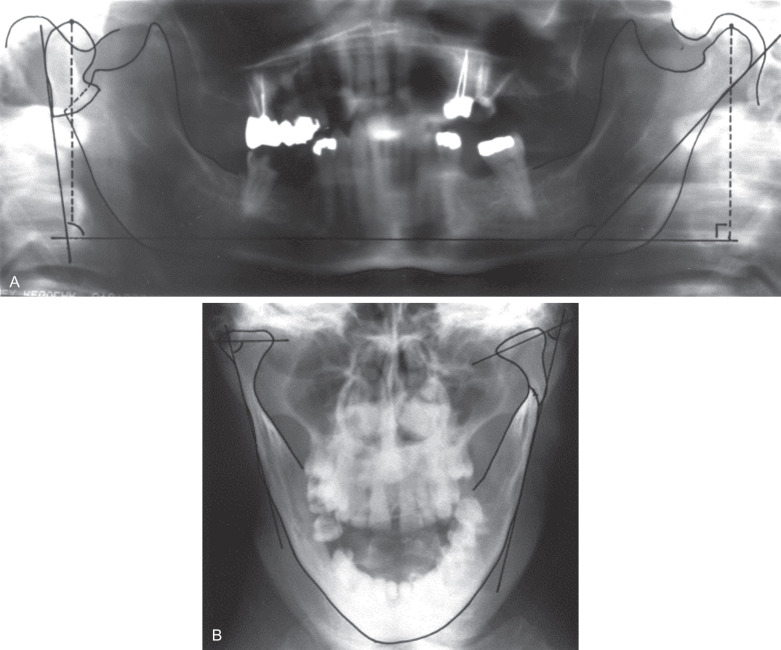
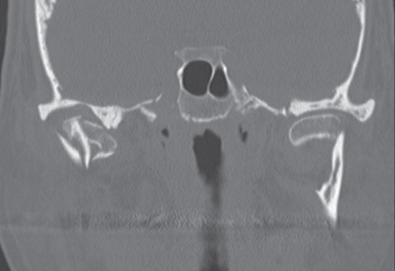
The main limitation of plain radiographs is that they do not give three-dimensional details of the fracture. Computed tomography (CT) is almost universally available today and most patients will already have a scan performed by the emergency department before a surgical consultation is made. CT gives extremely good detail of the position of the fracture(s) and the displacement of the segments. It is especially good for intraarticular fractures ( Fig. 1.15.6 ). CT scans cannot show the position of the intraarticular disk but the need to have that information available for treatment planning purposes is a hotly debated topic (discussed later). Should one desire more information on the position of the disk, a magnetic resonance imaging (MRI) scan would be needed as this is the imaging modality that provides the best view of the disk and other soft tissues within the joint.
Terminology
Controversy exists with respect to terminology and classification of condylar process fractures. Practitioners in Europe and North America may refer to the same entity with different words. For the purpose of this chapter and to clarify the vocabulary, it is important to make a distinction between the following terms:
Displacement. Displacement refers to the relationship of the fractured ends of the bones to one another. Often arbitrarily broken down into mild, moderate and severe displacement, it can be used for fractures throughout the skeleton whereas “dislocation” and “luxation” (see below) can be used only for fractures that involve a joint. The amount of displacement and its direction can be quantified by measuring the angle the condylar process makes with the ramus of the mandible in both the sagittal and coronal planes ( Fig. 1.15.5 ). A fracture that is displaced 90 degrees medially is one that is also dislocated because the articular surfaces will no longer have much contact. The relationship of the fractured ends can be further classified as those with medial and those with lateral override (displacement) of the segments ( Fig. 1.15.7 ).
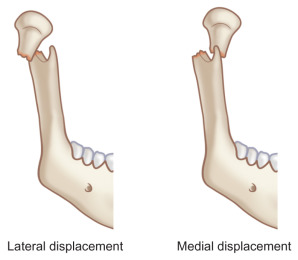
Fig. 1.15.7
Illustration showing lateral and medial displacement (override) of the fractured ends of a condylar process fracture.
Dislocation (aka Luxation). Dislocation refers to the lack of relationship of the articular surfaces to one another. It usually indicates that the articulating surface of the mandibular condyle is mostly not contacting the articulating surface of the glenoid fossa ( Fig. 1.15.8 ). To be dislocated, the fracture would have to be severely displaced (see above).
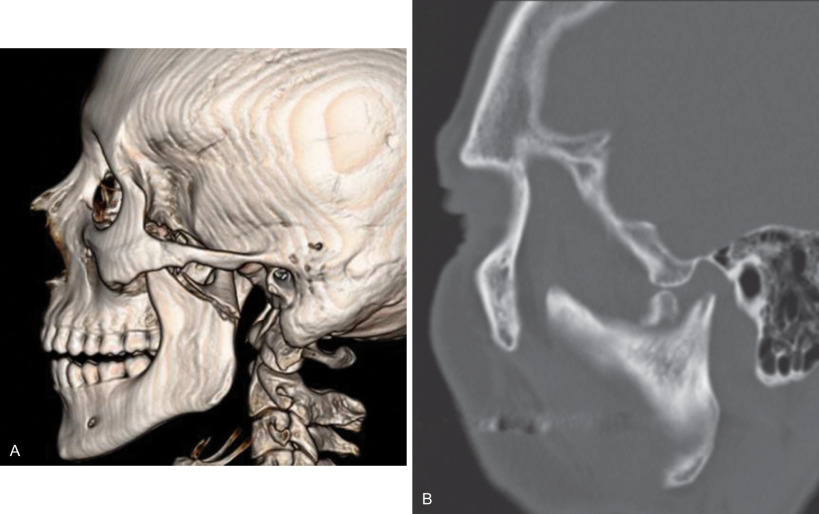
Fig. 1.15.8
CT scans of two completely dislocated condylar process fractures. Note that the articulating surface of the condyle is not in contact with the articulating surface of the glenoid fossa.
Subluxation. Sometimes the term subluxation is used to describe a partial separation of the articular surfaces but the condyle is not completely dislodged outside of the glenoid fossa. The difference between subluxation and dislocation (and luxation) is a matter of degree in that the articulating surfaces are not contacting.
Diacapitular (fractures). This is another European term that is used when the fracture line starts at the articular surface, goes through the head of the condyle and may extend outside the capsule. So it extends from within the capsule to outside the capsule ( Fig. 1.15.9 ). These types of fractures are also known as intracapsular fractures , especially in North America. However, it has been shown that in a large number of “intracapsular” fractures, the fracture extends inferior to the capsule on the medial aspect. The name “intracapsular ” therefore may be anatomically incorrect in such cases.
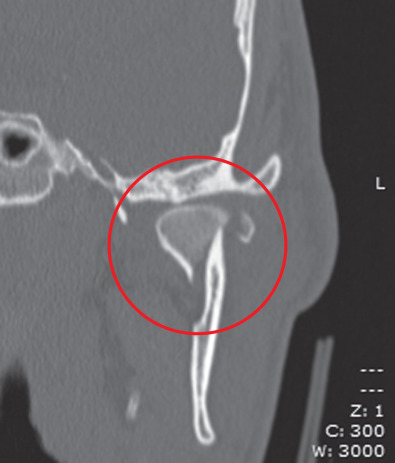
Fig. 1.15.9
CT of a diacapitular fracture. Note that the fracture line begins on the articular surface, goes through the head of the condyle and may extend outside the joint capsule on the medial side.
Classification of Condylar Process Fractures
There are many classification systems in the literature. Classification systems are used for two main purposes. One is to categorize injuries so their treatment may be studied. For this purpose, the classification system must be very complete ( Table 1.15.1 ). Unfortunately, most classification systems used to adequately classify condylar process fractures for purposes of research are complex, cumbersome, and have very little clinical usefulness. The other purpose of a classification system is to help decide between the possibilities for treatment. Such systems do not have to be as complex and the ones that are used the most today by clinicians to classify condylar process fractures are based on the level or anatomic position of the fracture(s) (i.e., head, neck, subcondylar) ( Fig. 1.15.10 ) and the magnitude and direction of displacement of the fragments ( Fig. 1.15.5 ).
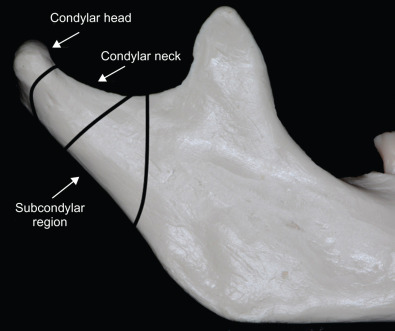
Level of the Fracture
The “level” or anatomical position of the fracture is a method of broadly classifying fractures. Although a debated issue is the exact anatomic position of the divisions, a simple method is to divide condylar process fracture into three types: condylar head, condylar neck, and subcondylar region ( Fig. 1.15.10 ). A condylar head fracture is one at the level of the joint capsule, so the fracture is essentially intracapsular or possibly diacapitular. The neck of the condylar process is from the joint capsule above to the level of the sigmoid notch below. Anything lower than that is considered a subcondylar fracture. The main usefulness of such a classification is that it directly correlates with the possibility of placing stable bone plate osteosynthesis across the fracture. For example, most condylar neck and all subcondylar fractures are amenable to stabilization with standard 2.0 mm bone plate osteosynthesis whereas intracapsular fractures through the condylar head are often not treated open by most surgeons except those skilled in temporomandibular joint surgery.
Treatment of Condylar Process Fractures
Most condylar process fractures require treatment. There are some cases, however, where observation may be indicated, for instance, a patient with a condylar process fracture that is nondisplaced or minimally displaced, but who can bring their teeth into a normal occlusion. Such patients can be placed on a soft diet and monitored. When treatment is deemed necessary, there are options that have to be considered. The main decision is whether to treat the fracture open or closed.
Deciding on Open or Closed Treatment
The age-old question is whether or not condylar fractures should be treated open or closed. This question will never be answered because it is the wrong question. What we should instead be asking is whether there are some condylar fractures that would obtain predictably better outcomes when treated open. And if that is the case, how do we identify them?
In selecting open or closed treatment, one must first understand the goals of treatment. The outcomes that are sought when treating patients with condylar fractures are the following :
- 1.
Maintenance of pretrauma occlusion
- 2.
Pain-free function
- 3.
Normal range of mandibular motion (interincisal opening > 40 mm, 9–12 mm lateral and protrusive excursions)
- 4.
Maintenance of facial symmetry
The literature is not very useful in helping an individual surgeon decide about what treatment to provide an individual patient. A fair synthesis of the entire world literature on the topic of condylar fracture treatment would be: While objective measures of outcomes vary with the level of the fracture (head, neck, subcondylar), the amount of displacement and/or dislocation, the presence of bilateral vs. unilateral condylar fractures, and whether or not they were treated open or closed, most patients with condylar fractures have few subjective complaints after treatment, irrespective of the above factors. One must keep this in mind when making treatment decisions for patients who present with condylar fractures. But knowing this may not be useful in making individual treatment decisions because each fracture, patient, and surgeon is different.
There are prerequisites to closed treatment that are important to understand.
- 1.
The patient must have a good complement of teeth, especially posterior teeth on the side(s) of the fracture(s). Without them, there will be a significant loss of posterior vertical dimension and an increase in the mandibular plane angle. The loss of posterior vertical dimension can also make future prosthetic reconstruction difficult because there will be no room between the retromolar pad and the maxillary tuberosity to accommodate the thickness of a denture base. Open treatment in patients without good posterior teeth will be better able to maintain the posterior vertical dimension and interarch space.
- 2.
The patient must be cooperative. They must wear their elastics, frequently verify their occlusion, do their functional exercises, and return often for follow-up. If one does not feel that a patient will be cooperative, then closed treatment may fail to achieve the above outcomes; open treatment might be more favored.
- 3.
The surgeon must be willing to see the patient often to assess treatment and alter functional therapy as necessary. There is no question that patients treated closed require more visits to assure the occlusion is being maintained and the physiotherapy is being performed adequately. If the surgeon is unwilling to see the patient more often, open treatment might be a more favorable option.
There are also pre-requisites to open treatment that are important to understand.
- 1.
The surgeon must be capable of safely performing open reduction and internal fixation (ORIF) of a condylar process fracture.
- 2.
Stable internal fixation must be applied to the fragments to assure no loss of stability during the postoperative healing period. If the fixation fails, loose hardware in this area will likely cause inflammation/infection for which more surgery will be needed. Therefore, one should only perform open surgery when the fragments are large enough to adequately stabilize with internal fixation devices and when the quality of the bone is adequate to maintain a stable screw–bone interface. The very young and the osteoporotic elderly female may have bone that is not capable of maintaining screw–bone interface stability.
Considerations for Open Reduction and Internal Fixation
Most condylar process fractures can be treated closed with satisfactory outcomes. This is especially true of unilateral condylar fractures that satisfy the prerequisites for closed treatment listed above. This is also true of severely displaced unilateral fractures, high or low. However, there are some conditions where open treatment facilitates the overall care of the patient. These conditions include the following:
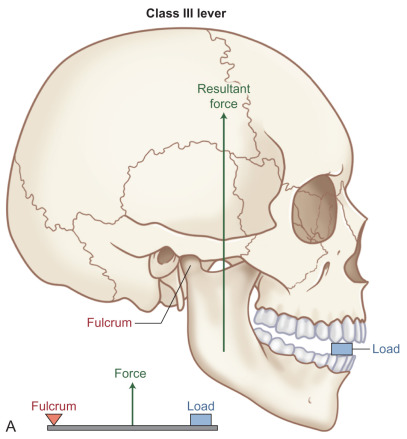
- 1.
Bilateral condylar process fractures . When a patient has both condylar processes fractured, especially when they are displaced, it will be difficult to predictably achieve the above desirable outcomes using closed techniques. The reason for this is that the biomechanics become unfavorable. If one considers that under the power stroke of mastication the mandible functions as a Class III lever system ( Fig. 1.15.11A ), when the fulcrum (condyle) is removed (by displacing the condyles), contraction of the elevator muscles causes premature contact of the terminal molars, resulting in an anterior open-bite ( Fig. 1.15.11B ). While closed treatment can often achieve the pretrauma occlusion and does so in the majority of patients, it is not predictable. Some patients obtain good outcomes, some do not. It is not possible to determine which patients will have a good outcome with closed treatment of bilateral condylar fractures and which will not. Therefore, ORIF of at least one of the condylar fractures will greatly increase the predictability of a favorable outcome.