Feet
OVERVIEW
The dermatologic conditions of the feet are similar to those of the hands. Inflammatory conditions such as psoriasis and eczema often mirror palmar disorders. Similarly, bacterial, viral (e.g., warts), and fungal infections are also prone to appear on the feet (see Hands and Fingers and Nails). Warts and other benign lesions must be distinguished from the rare, but potentially fatal, acral lentiginous melanoma.
Tinea Pedis
Tinea pedis (TP), commonly referred to as “athlete’s foot,” is an extremely common problem. It thrives in warm, humid conditions and is most commonly seen in young adult men. Contributing factors include hot humid climates, occlusive footwear, and hyperhidrosis. Ubiquitous media advertisements for athlete’s foot sprays and creams are testimony to the commonplace occurrence of this annoying dermatosis.
There are several clinical presentations of TP: interdigital, acute vesicular, and chronic tinea pedis. Most cases are caused by Trichophyton rubrum, which evokes a minimal inflammatory response, particularly in chronic infections. TP is also caused by Trichophyton mentagrophytes, which may acutely produce vesicles and bullae, the least common clinical variant of tinea pedis.
Distinguishing Features
Acute interdigital tinea pedis is seen predominantly in males between 18 and 40 years of age. It is most often caused by T. mentagrophytes.
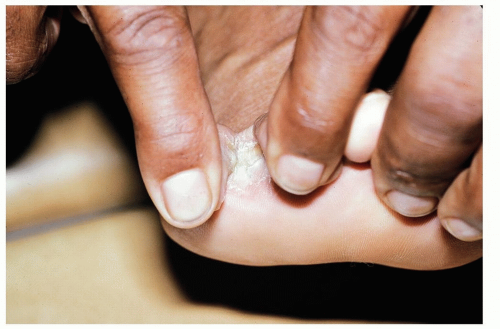
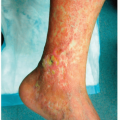
Scale, maceration, and fissures of toe webs are characteristic, especially between the fourth and fifth toes (Fig. 19-1); however, any web space, as well as the dorsal foot may be involved
Often asymptomatic; however, it may itch intensely
Marked inflammation and fissures suggest bacterial superinfection
Clusters of pruritic vesicles, bullae, or pustules on the sides of the feet, insteps, toes, or soles (Fig. 19-2)
Distinguishing Features
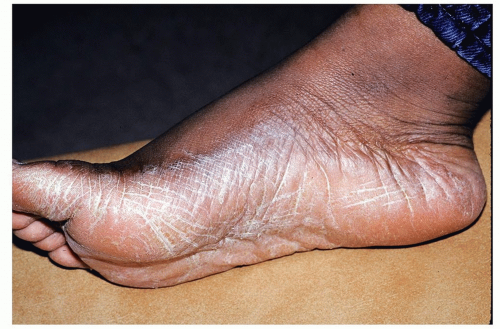
“Moccasin” distribution consists of scales covering the sole and sides of the feet (hyperkeratotic/moccasin type, usually caused by T. rubrum)
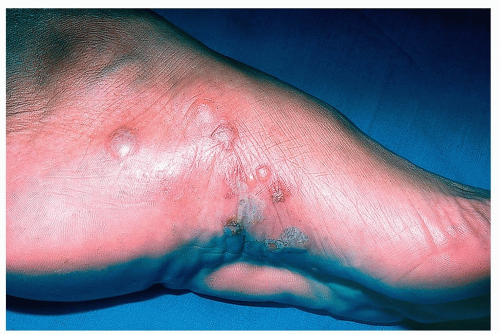
Figure 19-2 Tinea pedis, acute vesicular.
A KOH or culture specimen is obtained from under the roof of the vesicle or bulla.
The skin of the entire sole, sides of the foot, and heel is scaly, appears to be “dry,” but not inflamed (Fig. 19-3)
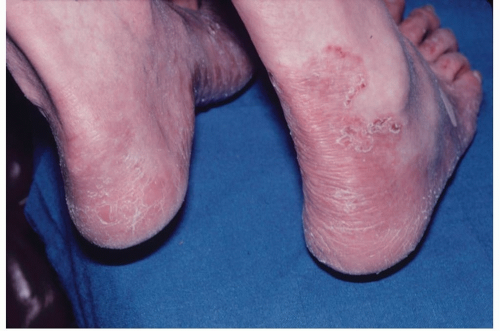
Borders are distinct along the sides of the feet and may extend to the Achilles area (Fig. 19-4)
There is often nail involvement (onychomycosis)
Symptoms are minimal unless painful fissures occur
Palmoplantar tinea can be present on one or both palms (tinea manuum), as well as on both soles (“two feet, one hand” tinea). This is pathognomonic for tinea (see Fig. 14-18)
Diagnosis
Acute vesicular tinea pedis
A specimen should be obtained from the inner part of the roof of the blister for KOH examination and/or fungal culture
A positive potassium hydroxide (KOH) examination or fungal culture is diagnostic Chronic tinea pedis
The KOH examination from the edge (“active border”) or fungal culture is positive
Management
Acute Tinea Pedis
For acute oozing and maceration, Burow solution compresses are used
Broad-spectrum topical antifungal agents such as ketoconazole (Nizoral), ciclopirox (Loprox), or clotrimazole (Lotrimin) may be applied once or twice daily
Oral antifungal agents such as terbinafine (Lamisil), itraconazole (Sporanox), fluconazole (Diflucan), or griseofulvin may be necessary if topical therapy is unsuccessful
Prevention consists of maintaining dryness in the area by:
Using a hair-dryer after bathing and targeting the involved interweb space(s)
Applying powders such as Zeasorb-AF that contains miconazole as an active antifungal ingredient
Chronic Tinea Pedis
This is the most difficult type of tinea pedis to cure because topical agents do not effectively penetrate the thickened epidermis. Consequently, systemic, as well as topical, antifungals are often necessary.
Oral antifungal agents such as the following may be prescribed:
Terbinafine (Lamisil) 250 mg once daily for 14 days or longer, if necessary
Itraconazole (Sporanox) 200 mg once daily for 14 days or longer, if necessary
Fluconazole (Diflucan) 150 to 200 mg once daily for 4 to 6 weeks, if necessary
Nail involvement may require longer treatment because nails may serve as reservoirs for reinfection (see Nails)
Prevention involves decreasing wetness, friction, and maceration. Absorbent powders, such as 2% miconazole powder (Zeasorb-AF), should be applied after the eruption clears to prevent recurrence
Not all rashes of the feet are fungal. In fact, if a child younger than 12 years has what appears to be tinea pedis, it is probably another skin condition, such as atopic dermatitis.
Plantar Warts
Plantar warts commonly appear on the soles of the feet in children and young adults. They usually arise on the metatarsal area, heels, insteps, and toes, in an asymmetric distribution.
Distinguishing Features
A loss of normal skin markings (dermatoglyphics) such as footprints and toeprints
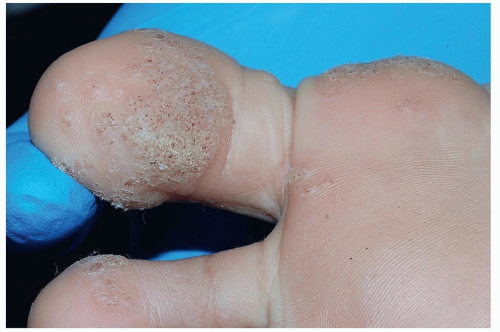
Lesions may be solitary or multiple, or they may appear in clusters (mosaic warts) (Fig. 19-5)
Can be tender and painful
Extensive involvement on the sole of the foot may impair ambulation, particularly when present on a weight-bearing surface
Diagnosis
Clinical