Eyelids and Periorbital Area
OVERVIEW
Besides being subject to various inflammatory dermatoses such as atopic dermatitis, contact dermatitis, seborrheic dermatitis, and rosacea, the skin of the eyelids and the surrounding periorbital area is repeatedly exposed to the environment. The sun, the application of makeup, airborne substances (pollens, fragrance sprays), fingernail and toenail products that come in contact with the eyelids, and contact lenses, all have aggravating and allergenic potential in this area.
The eyelids readily swell and become edematous from internal complications, such as urticaria (angioedema). The eyelids and periorbital region may also serve as cutaneous signs of systemic conditions, such as indicators of hyperlipidemia (xanthelasma) and dermatomyositis (heliotrope sign). In addition, various benign and malignant neoplasms are seen here.
CHILDREN
Atopic Dermatitis
Atopic dermatitis (AD) (atopic eczema) of the eyelids commonly appears in children. By definition, AD occurs in association with a personal or family history of hay fever, asthma, allergic rhinitis, or sinusitis. The patient may present with itchy or irritated eyes, as well as eczematous lesions elsewhere on the body. AD frequently remits spontaneously—reportedly in 40% to 50% of children—but it may return in adolescence or adulthood, and possibly persist for life. AD typically presents early in life and is associated with an increased risk of developing asthma and allergic rhinitis. In the United States, AD has a higher prevalence in African American children.
Distinguishing Features
Habitual rubbing results in lichenification (exaggerated skin lines)
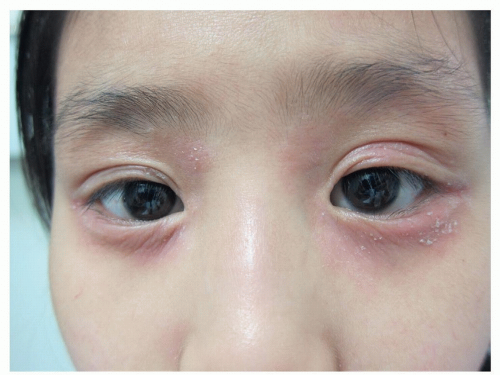
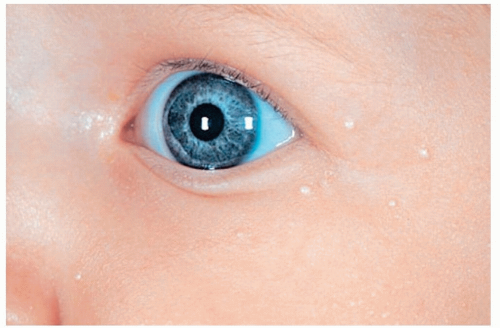
Dennie-Morgan folds are characteristic double creases that extend from the inner to the outer canthus of the lower eyelid (Fig. 4-1)
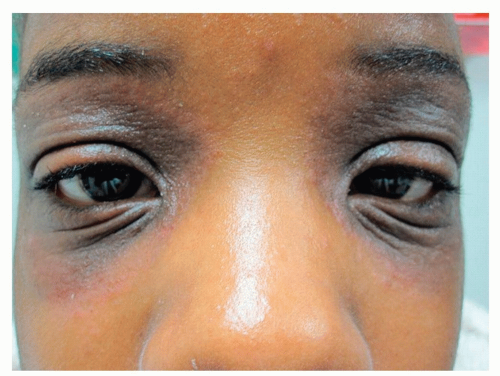
“Allergic shiners” refers to a darkened, violaceous, or tan coloring in the periorbital areas. Along with Dennie-Morgan folds, this coloring is an instant clue to atopy (the genetic tendency to develop allergic rhinitis, asthma, and atopic dermatitis) (Fig. 4-2)
Diagnosis
There are usually features of AD at other sites (e.g., flexural creases)
Personal and/or family history of atopy
Management
Topical Steroids
 Alert: It should be noted that the thin eyelid skin that protects the underlying eyes warrants extra caution and requires the least potent topical preparations (particularly topical steroids) for the shortest period of time. Only a nonfluorinated, mild topical steroid should be applied for very short periods to avoid atrophy and absorption and possible increase of intraocular pressure.
Alert: It should be noted that the thin eyelid skin that protects the underlying eyes warrants extra caution and requires the least potent topical preparations (particularly topical steroids) for the shortest period of time. Only a nonfluorinated, mild topical steroid should be applied for very short periods to avoid atrophy and absorption and possible increase of intraocular pressure.
Topical steroid-sparing agents are best used in areas of high risk where skin thinning (atrophy) tends to occur, such as the eyelids
Topical immunomodulators (calcineurin inhibitors) such as tacrolimus ointment 0.1% (Protopic) for adults; 0.03% in children; and pimecrolimus 1% cream (Elidel) are effective alternatives
Crisaborole 2% ointment (Eucrisa) is a nonsteroidal, phosphodiesterase (PDE)-4 inhibitor topical cream for mild to moderate atopic dermatitis. Crisaborole decreases the production of pro-inflammatory cytokines and is approved for infants over 3 months of age
Moisturizers such as petroleum jelly and/or barrier creams/lotions/emulsions
Ceramide-containing barrier creams such as CeraVe and Epiceram applied twice daily provide moisturization and enhance and restore the skin’s protective barrier function
Molluscum Contagiosum
Molluscum contagiosum (MC) often appears on or around the eyelids or eyelid margins. This is frequently seen in children and in patients who have human immunodeficiency virus (HIV)/acquired immunodeficiency syndrome (AIDS) (see also Forehead and Temples and Cutaneous Manifestations of HIV disease).
CHILDREN AND ADULTS
Milium
Milium (plural, milia) is most often noted on the face, especially around the eyes, eyelids, cheeks, and forehead. Milia occur at almost any age. They are very common, tiny, epidermal cysts that contain keratin (see also Forehead and Temples).
Distinguishing Features
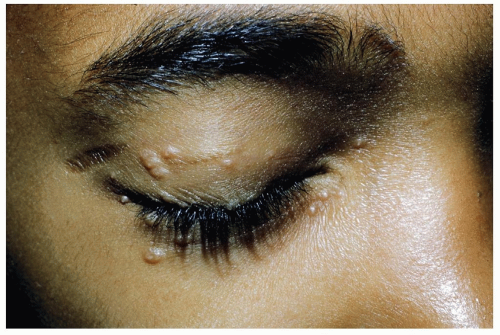
1.0 to 2.0 mm in diameter, white or yellow cysts (Fig. 4-5)
Lesions in children spontaneously resolve over time
Diagnosis
Clinical
Management
No treatment is medically necessary
For cosmetic reasons, incision and extraction (see Fig. 3-5)
Stye (Hordeolum)
A stye (hordeolum) is a common disorder of the eyelid. It is an acute focal infection (usually Staphylococcus aureus). The bacterium is often found in the nose and is transferred easily to the eye.
Distinguishing Features
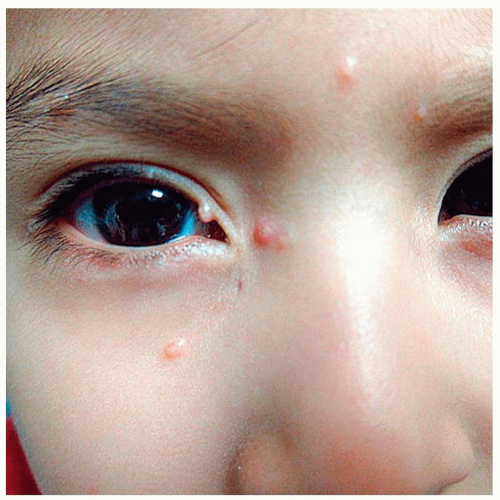
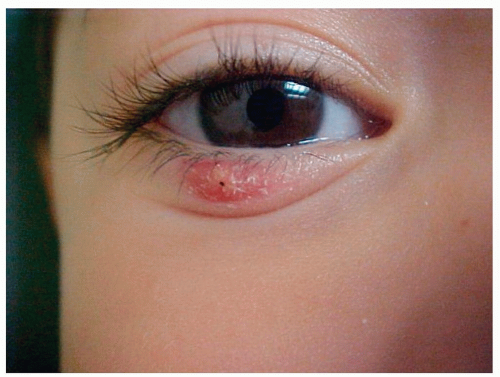
Painful, warm, swollen, red papule on the eyelid margin (Fig. 4-6)
May cause blurring of vision
Diagnosis
Clinical examination
Differentiating a stye from an acute chalazion may be difficult because they both are similar in appearance; however, styes are very tender and painful
Management
Warm compresses
Topical antibiotic ointment if the lesion is draining or if there is an accompanying blepharoconjunctivitis
Systemic antibiotics if necessary
Usually self-limited; spontaneously resolves in 1 to 2 weeks
Meibomian Cyst (Chalazion)
A meibomian cyst (chalazion) is a chronic, noninfectious granulomatous reaction. It represents an inflammatory response of either a meibomian gland or a Zeis gland. It develops because of a blockage of a gland orifice.
The resulting granulation tissue and chronic inflammation distinguishes a chalazion from an internal or external hordeolum, which is primarily an acute pyogenic lesion. Chalazia are sometimes associated with seborrhea, chronic blepharitis, and rosacea.
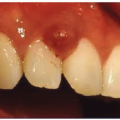
Distinguishing Features
Nontender, firm papule located deep within the lid or the tarsal plate
Lid discomfort, redness, tenderness, swelling
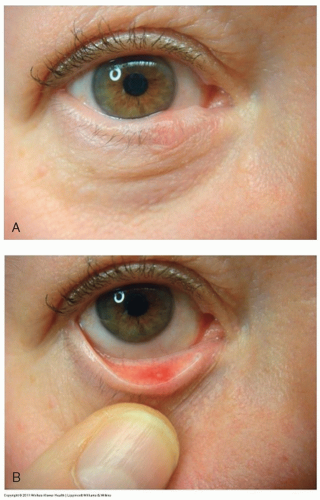
Eversion of the eyelid may reveal the dilated meibomian gland (Fig. 4-7, A and B)
Diagnosis
Clinical
Management
Small, asymptomatic chalazia may be ignored
Conservative treatment with lid massage, moist heat, and topical mild steroids can be helpful in minimizing inflammation and in reducing edema
Topical antibiotics are not effective
Systemic antibiotics if necessary
The treatment of secondarily infected chalazia (i.e., internal hordeolum) includes heat and topical and/or systemic antibiotics
Ophthalmologic surgery by incision and curettage is performed only if medical therapy fails
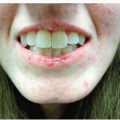
Periorificial (Periocular) Dermatitis
Periorificial (periocular) dermatitis appears in children and women between 15 and 40 years of age. Of unknown etiology, similar to rosacea, periocular dermatitis manifests as acne-like lesions surrounding the eyes.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree