Forehead and Temples
OVERVIEW
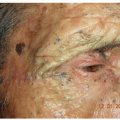
Molluscum contagiosum, flat warts, acne vulgaris, rosacea, seborrheic dermatitis, and benign neoplasms, such as various nevi, tend to appear on the forehead and temples in children and young adults. In older individuals, seborrheic keratoses, sebaceous hyperplasia, and sun-related growths, such as actinic keratoses, basal cell carcinomas, and squamous cell carcinomas frequently appear on the forehead and temples.
CHILDREN
Molluscum Contagiosum
Molluscum contagiosum (MC) is a common, self-limited, superficial viral infection of the epidermis. Spread by skin-to-skin contact and caused by a large DNA-containing poxvirus, MC is seen most often in three clinical contexts: healthy children (infants and toddlers), particularly in those who have atopic dermatitis; in the genital region in sexually active young adults; and in patients with human immunodeficiency virus (HIV)/acquired immunodeficiency syndrome (see also Genitals and Cutaneous Manifestations of HIV Disease).
Distinguishing Features
Dome-shaped, “waxy,” or “pearly” appearing papules with a central white core (umbilication); less frequently, lesions are pink to flesh-colored (Fig. 3-1)
Generally, lesions are 1 to 3 mm in diameter, but may coalesce into double or triple lesions and become so-called “giant” mollusca (more often noted in patients who are significantly immunocompromised)
Frequently grouped via autoinoculation from scratching or manipulation; lesions may be widely disseminated to trunk, extremities, and genital areas
Often involves the face, forehead, eyelids (see Fig. 4-3), conjunctiva, as well as intertriginous areas such as the axillae and inguinal creases
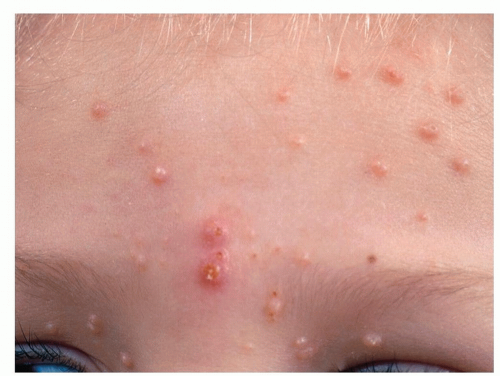
Figure 3-1 Molluscum contagiosum.
Characteristic dome-shaped, shiny, waxy papules that have a central umbilicated core. Two of the lesions are inflamed.
May appear in young children on eczematous areas (sites with decreased skin barrier integrity)
The number of lesions varies from one up to hundreds
Generally asymptomatic; may itch and become inflamed and crusted
In children, the course is most often self-limiting with lesions resolving within 6 to 18 months
Recurrences are rare in immunocompetent children
Diagnosis
Clinical
A handheld magnifier often reveals the central core
A short application with liquid nitrogen (LN2) accentuates the central core (Fig. 3-2A and B)
Shave or curettage biopsy if diagnosis is in doubt to visualize diagnostic molluscum bodies
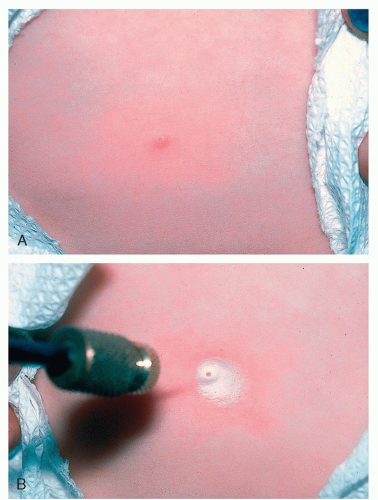 Figure 3-2 Molluscum contagiosum. A, Molluscum contagiosum. B, Molluscum contagiosum; A short application of LN2 accentuates the central core. |
Management
May resolve spontaneously
Cantharidin (Cantharone), a blister-producing agent (vesicant), is applied in an office setting. The preparation is applied to individual warts in a thin coat, using the wooded end of a cotton-tipped applicator or a toothpick. The procedure is painless. After 4 to 6 hours, the skin is washed with soap and water. The cantharidin may cause the skin under the lesion to blister, and the molluscum is then lifted off the skin
Cryotherapy with LN2
Application of 10% KOH
Electrocautery
Curettage
Home application:
Topical over-the-counter antiwart preparations such as salicylic acid in collodion (Compound W, Occlusal)
Imiquimod 5% cream (Aldara cream)
Flat Warts
Flat warts (verrucae planae) are frequently noted in children and young adults. Lesions appear on the face as well as on the arms, dorsa of hands, and the legs in women.
Distinguishing Features
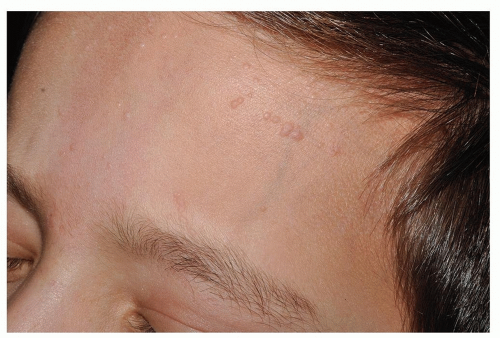
Small, flat-topped (planar), slightly elevated, skin-colored or tan papules, 1 to 3 mm in diameter (Fig. 3-3)
Lesions are subtle (side lighting may be necessary to see them)
May present in a linear configuration due to autoinoculation
Tend to resolve spontaneously but may persist
Diagnosis
Clinical diagnosis
Shave biopsy, if necessary
Management
Cautious, short applications of LN2 therapy
Light electrodesiccation Home application:
Imiquimod (Aldara cream)
Benzoyl peroxide or topical retinoids
Over-the-counter lactic-salicylic acid (Duofilm) or Occlusal-HP, a salicylic acid preparation
INFANTS, CHILDREN, AND ADULTS
Milium
Milium (plural, milia) is a very common tiny variant of an epidermoid cyst that contains keratin. Milia can occur in people of any age.
Distinguishing Features
1.0 to 2.0 mm in diameter and are white to yellowish asymptomatic papules (Fig. 3-4)
Most often noted on the face, frequently on the forehead, cheeks, and around the eyes
Diagnosis
Clinical
Management
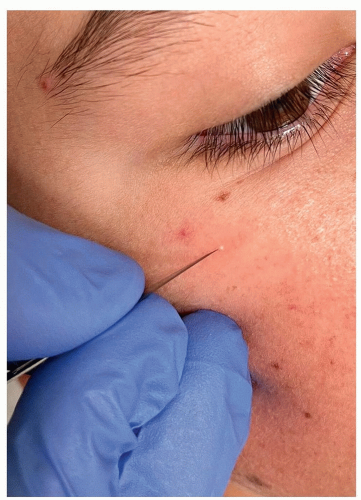
Incision and evacuation: In contrast to closed comedones (“whiteheads,” which they resemble), milia must first be incised (usually with a No. 11 blade or 20-gauge needle) before their contents can be easily expressed (Fig. 3-5).
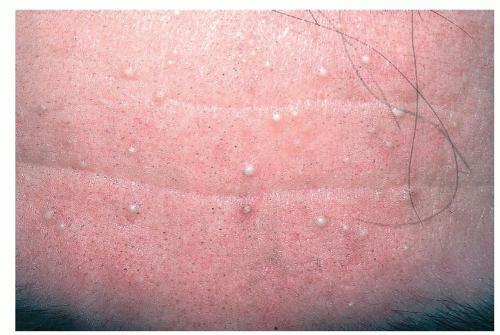 Figure 3-4 Milia. 1-2 mm smooth white cystic lesions. They are often mistaken for the closed comedones of acne (“whiteheads”). |
Melanocytic Nevus
A melanocytic nevus (MN), mole, or “beauty mark,” is a benign proliferation of nevus cells that are derived from melanocytes. Congenital nevi may be present at birth or in the neonatal period. Congenital and acquired nevi are more often seen in patients with light or fair skin than in blacks or Asians. During childhood and adolescence, acquired nevi begin to appear.
As adulthood approaches, the development of nevi tapers off, and, at middle age, many existing lesions gradually lose their capacity to form melanin, become skin-colored, or disappear completely (see also Scalp, and Nose and Paranasal Area).
Large congenital nevi are associated with a low, but real risk of malignant transformation and the development of melanoma (see Trunk).
Distinguishing Features
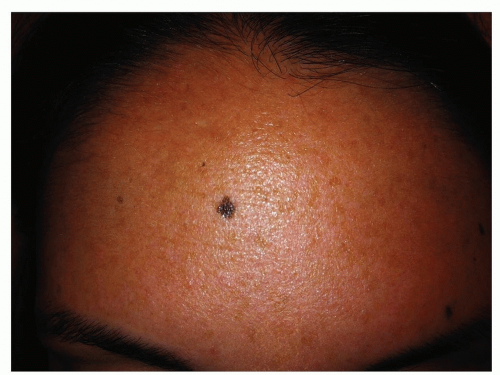
Junctional Melanocytic Nevi
Small, macular (flat), freckle-like; uniform in color (Fig. 3-6) that varies from brown to dark brown to black
Acquired or congenital; most prevalent on the face, arms, legs, trunk, genitalia, palms, and soles
Compound Melanocytic Nevi
Elevated, dome-shaped papules or papillomatous nodules that are uniformly brown to dark brown (Fig. 3-7); may contain hairs
Seen most often on the face, arms, legs, and trunk
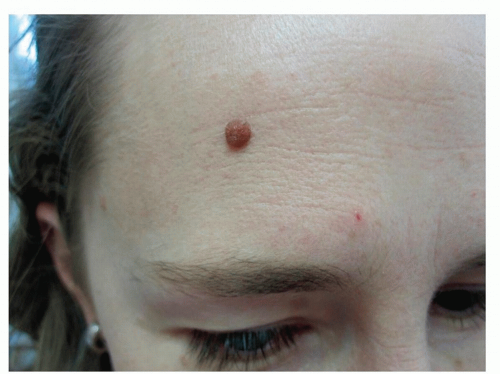
Dermal Melanocytic Nevi
May be elevated and dome-shaped, wart-like, or pedunculated
Tan, brown, or dappled with pigmentation
With age they often become skin-colored (Fig. 3-8)
Diagnosis
Based on clinical appearance or, if necessary, a histopathologic evaluation after removal
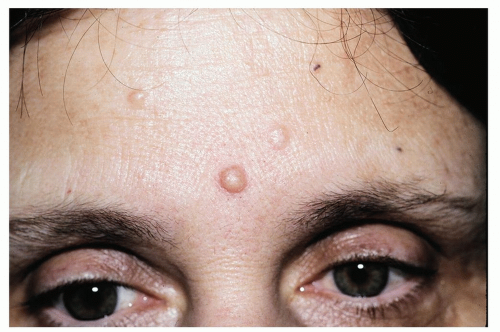 Figure 3-8 Dermal Melanocytic Nevus.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|