Cutaneous Manifestations of Pregnancy
OVERVIEW
During pregnancy, hormonal shifts may result in physiologic alterations in the skin, hair, and nails. Many of these changes are seen so frequently, that they are considered to be normal. Pregnancy can also alter the course of certain preexisting skin conditions and systemic diseases that have cutaneous involvement, for example:
Systemic lupus erythematosus and scleroderma may flare.
Acne may improve, or it may worsen.
Dyshidrotic eczema may appear de novo, or a flare-up of preexisting lesions may occur.
Condylomata acuminata may enlarge considerably and may proliferate.
It should always be kept in mind that common skin diseases unrelated to pregnancy should also be considered when evaluating a pregnant patient with a skin disorder.
PHYSIOLOGIC CHANGES DURING PREGNANCY
Hyperpigmentation
Hyperpigmentation is presumed to be secondary to increased levels of estrogens and melanocyte-stimulating hormone.
Distinguishing Features
Darkening of the nipples and surrounding areolae, as well as darkening of the axillae, thighs, umbilicus, perineum, and external genitalia, may occur
Melasma (see also Cheeks). The “mask of pregnancy” (formerly known as chloasma) occurs in more than 50% of women during pregnancy. It is worsened by exposure to the sun
Darkening of preexisting freckles and nevi
Connective Tissue Changes
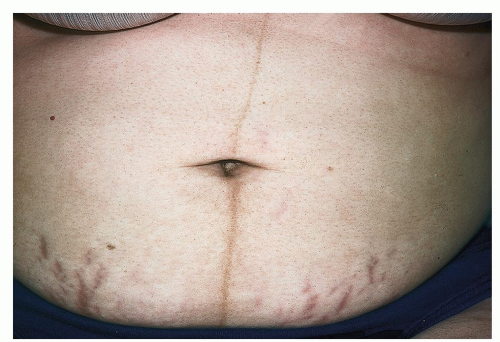
Striae gravidarum (striae cutis distensae related to pregnancy) or “stretch marks” are caused by the combination of increased adrenocortical activity and rapid tissue growth and distention, which results in the tearing of the dermal collagen matrix and a weakening of elastic fibers. Typically, striae are reddish pink to violaceous linear atrophic bands that are located on the abdomen, hips, buttocks, and breasts. The striae are permanent, but the purplish color fades with time (Fig. 23-1).
Proliferation and enlargement of skin tags, with some persisting after pregnancy.
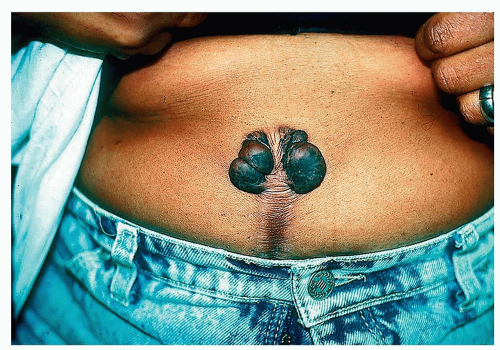
Growth of preexisting keloids. This may occur in the scars of an abdominal hysterectomy or a cesarean section (Fig. 23-2).
Vascular Phenomena
Spider telangiectasias. These can result from the high levels of estrogens in pregnancy (Fig. 23-3)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree