Autologous fat grafting has become more and more popular among plastic surgeons in the last few years due to recent discoveries on the mesenchymal stem cells stored in the harvested fat. These cells have a great regenerative potential and have the ability to restore the damaged tissues. The authors focused their practice on the treatment of the facial scars (derived from burns, trauma, degenerative diseases, and radiotherapy) and confirm that lipofilling is an excellent solution because it is able to improve the quality of the damaged tissues in terms of better scar color, pliability, thickness, relief, itching, pain, scar vascularization, and pigmentation.
Key points
- •
Lipofilling has become an important tool for plastic surgeons in treating all the diseases resulting in scars.
- •
Fat grafting has shown to have a great regenerative potential due to the presence of the mesenchymal stem cells that allow scar remodeling and improve the quality of the scar tissue.
- •
One of the possible uses of lipofilling is the treatment of facial scars, especially if derived from burns, trauma, degenerative diseases, and radiotherapy.
Introduction
Autologous fat grafting, also known as fat autotransplantation or lipofilling, is one of the most interesting and useful techniques in plastic surgery and is now used for both cosmetic and reconstructive surgical procedures. Adipose tissue is a connective tissue full of different cells, including the mesenchymal stem cells, which have a primary role in the regenerative purposes of the autologous fat grafting. Fat stem cells are not the primordial stem cells as the ones stored in the bone marrow, thymus, or spleen. They are more likely pluripotent fibroblasts or mesenchymal cells (third-generation differentiating cells) harvested from around vessels and nerves. Similar to other stem cells, the mesenchymal stem cells possess the 2 main properties of a stem cell: self-renewal and potency (the capacity to differentiate into specialized cell types).
The concept of autologous fat grafting was first described in 1893 by Neuber and subsequently by Hollander (1912), Neuhof (1923), and Josef (1931), to treat complex congenital malformations, traumatic wounds, and postoncological demolishing procedures. One of the leaders in fat transplantation is Sidney Coleman MD, who described a new method to improve the survival of the transplanted mesenchymal stem cells in the early 1990s. Rigotti and colleagues in 1997 first used fat injection for the treatment of radiodermatitis.
Preoperative evaluation and special considerations
Before performing a lipofilling procedure, all patients need a clinical assessment and routine preoperative examination; it is important to gauge the mindset and goals of the patient and inform that the volume of the fat may fluctuate with weight loss or gain. In case of scar treatment, preoperative markings of the face are mandatory, asking the patient to note the areas of greater tension and impairment to daily life activities and joint movements.
There are multiple graft donor sites and, up to now, there are no data that support one site is better than others. After the fat is harvested and processed, it can be grafted in the face. There are multiple different areas of the face that can be treated with autologous fat grafting, such as the glabella, forehead, temporal fossa hollows, labiomental crease, lips, prejowl sulci, and even earlobes. In these areas the presence of a scar can create different grades of volume deficit that can be successfully treated with lipofilling. It is known that areas of the face that have least motion and thicker overlying tissues have the best survival of the transferred fat (cheek, nasolabial folds, and malar region). On the other side, areas under motion and thinner preexisting fat content (such as the perioral region, the lips, and the marionettes) can have variable results after lipofilling.
Nowadays fat grafting is becoming mandatory in several procedures. The reason why it has become so popular is because it is a simple, safe, and repeatable procedure that can be used to treat virtually every part of the body, including the face, for multiple clinical applications:
- •
Scar release
- •
Restoring of improving skin quality
- •
Improvement of radiodystrophic skin
- •
Volume and contour
- •
Treatment of pain syndromes
- •
Treatment of degenerative diseases
- •
Wound healing
- •
Aesthetic purposes
Surgical technique
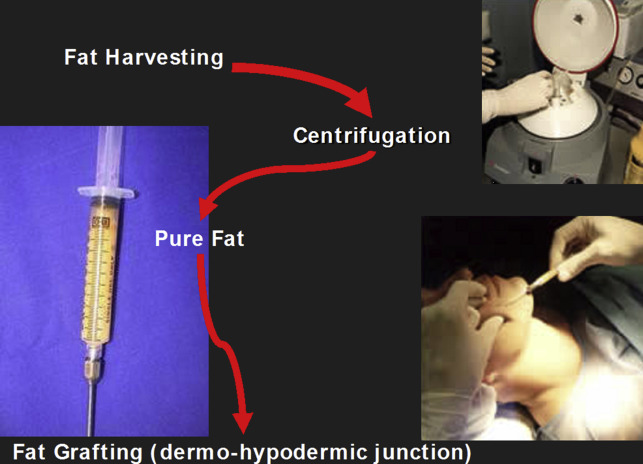
The authors’ technique, similar to the one described by Coleman, is based on the following steps: under local anesthesia and sedation, the donor areas (including the thighs, flanks, or abdomen) are incised with a 15-blade scalpel and infiltrated with a blunt cannula filled with anesthetic solution (the authors’ group uses 100 mL saline solution, 10 mL of levobupivacaine 7.5 mg/mL, 20 mL of mepivacaine 10 mg/mL, and 0.5 mL epinephrine 1 mg/mL). Adipose tissue is then harvested using the same skin incisions with blunt cannulas of 2 to 3 mm in diameter of variable length (between 15 and 23 cm). The cannula is connected with a Luer-lock syringe. After creating a negative pressure, the cannula is advanced and retracted with radial movements inside the whole donor area. The harvested tissue is then centrifuged at 3000 rpm for 3 minutes.
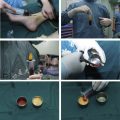
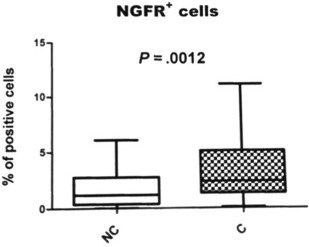
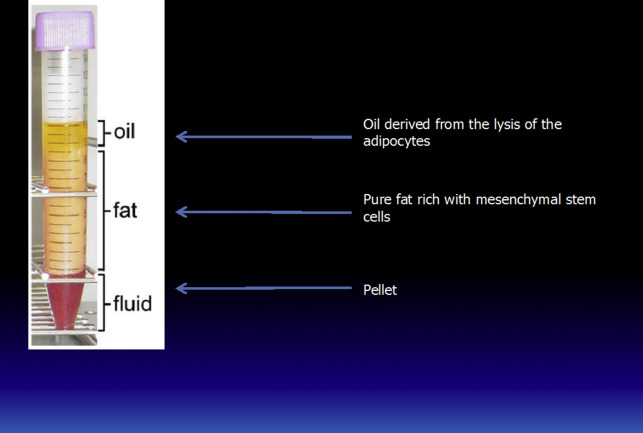
This step is extremely important because it allows the separation of the unwanted components (oil, blood, local anesthetic, and other noncellular material) from the pure fat. Centrifugation increases the content of adipose-derived stem cells, reduces the amount of proinflammatory blood cells, and concentrates a higher number of viable cells with regenerative potential. The authors recently demonstrated that centrifugation does not impair cell viability and is able to concentrate a higher number of cells ( Figs. 1 and 2 ). The purified fat is transferred into a 1-mL syringe Luer-lock that allows a good control of the amount of fat injected and better handling.
The fat can be injected using needles or blunt cannulas. In the authors’ experience blunt cannulas are not perfect instruments; their group believes that the best choice is an 18-gauge angiographic sharp needle (Cordis Corp., Bridgewater, NJ, USA) and the Seldinger technique. Using a sharp needle allows the interruption of scar tissue, obtaining a “new space” where the fat can be grafted. This technique seems to allow better fat graft survival, increase graft uptake, and minimize the possibility of oil-forming cysts. Placement of the fat in small aliquots is the key of the Coleman technique because it ensures the proximity of the injected fat to a blood supply and allows the fat to anchor to the recipient tissue. These aliquots should be placed as the cannula is withdrawn, and no more than 0.1 mL of fat should be placed with each pass. In fact, if fat is injected in a bolus, fat cells will be clumped together and only those on the periphery of the injected area will have contact with the recipient tissue and will be more likely to survive ( Fig. 3 ).
Postoperative care
The treated areas are covered with paper patches for 5 days and the patient is asked to avoid pressure and friction to limit the displacement of fat. The skin incisions in the donor areas are sutured with 4/0 Vicryl. Abdomen and trochanteric areas are usually medicated with an elastic-compressive dressing and kept in place for 5 days to prevent any risk of hematoma.
Expected outcome and management of complications
The complications of this technique are limited and rare. The most common are infections (cellulitis), prolonged swelling, intravascular injections, fat necrosis, ecchymosis, contour irregularities/asymmetries, and overgrafting. In case of excessive fat grafting, the only possible treatment is a microliposuction of the area involved.
The volume retention after grafting is unpredictable and the percentages are very different in the scientific literature. For this reason, an overcorrection of 20% to 30% should be recommended due to the expected resorption rate. The use of additives such as stromal vascular fraction and growth factors such as platelet-rich plasma may increase the predictability of fat grafting, but there are still many doubts about this. Recent studies have shown that fat grafting to the face enriched by stromal vascular fraction (SVF) can lead to a better retention, with a survival of the graft around 68%. In addition, there is evidence that the fat volume retention is improved with increase in number of cells in the SVF.
Revision or subsequent procedures
Lipofilling has proved to be a safe procedure that can be repeated several times, especially in case of unsatisfactory aesthetic or functional outcomes after the first treatment. Studies have shown that fat grafting enhances the vascularity of the involved area; for this reason, every time fat is grafted, the percentage of cells that are able to survive tends to increase. Besides, it has been seen that weight gain can cause an enlargement of the fat graft, which can lead to poor aesthetic results, especially on the face. In these situations, as in all the situations of overgrafting, a microliposuction is required in order to rebalance the excessive fat injected. Finally, in specific situations, fat grafting can be performed in association with other surgical procedures (Z-plasty, surgical scar release, scar revision) with the intent of improving the quality of the scar.
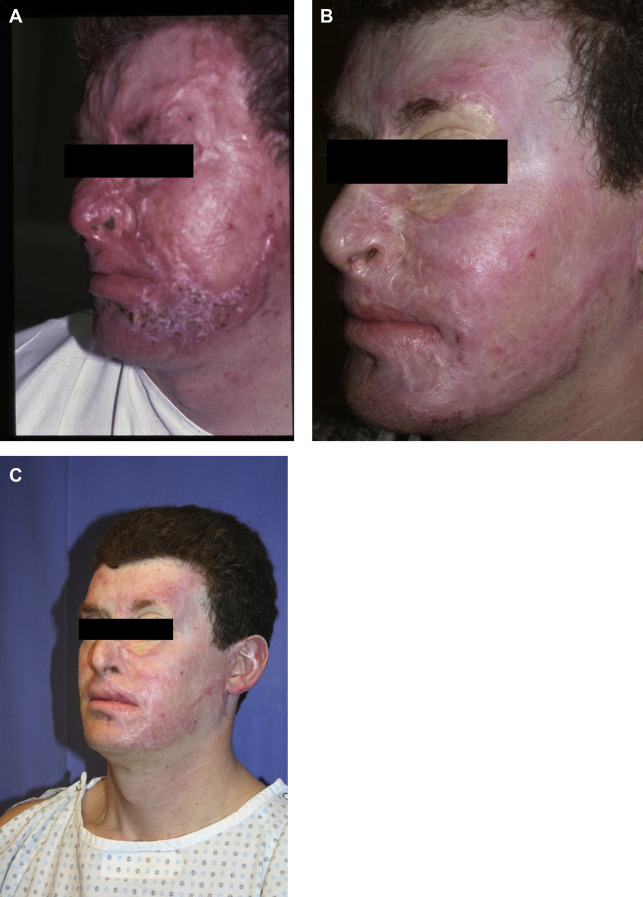
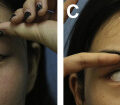
Case demonstrations
Case 1 . See Fig. 4 .