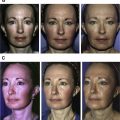
Reversing structural changes in aging skin gained potential after the therapeutic use of adipose-derived stem cells was described. Nanofat is a highly concentrated solution of progenitor cells without viable adipocytes. Nanofat grafting creates striking skin quality improvement. The availability of adipose-tissue combined with straightforward mechanical protocol to process fat brings regenerative and antiaging medicine into real-life clinical practice. Association with other cofactors (hyaluronic acid, botulin toxin, and vitamin C) and therapies (microneedling and drug delivery) provides better outcomes. This article describes the techniques and the authors’ experiences in nanofat grafting, and its potential new applications in regenerative medicine.
Key points
- •
Nanofat has no filling capacity. It is a highly concentrated solution of progenitor cells and has no viable adipocytes.
- •
The mechanical protocol for nanofat preparation is essential. It consists of a 2-step emulsification technique followed by filtration.
- •
Striking improvement on the skin quality is perceived 6 to 8 months after nanofat grafting. Association of hyaluronic acid, botulin toxin, and vitamin C provides shorter-term enhancement of the skin quality.
- •
Grafting can be performed by a nanofat intradermal injection or by a microneedling delivery system. Nanofat cream is used as an adjunct after the procedure to further maximize benefit and to moisturize the skin during initial healing.
Video content accompanies this article at “ http://www.plasticsurgery.theclinics.com ”.
Introduction
During the past 20 years, lipofilling has emerged as a fundamental component in a facial rejuvenation procedure ( [CR] ). Currently, facelifts and lipofilling can be almost considered inseparable: facelift techniques address the sagging process, whereas the lipofilling focuses on the deflation. First described in 2001, adipose-derived stem cells (ADSCs) and their therapeutic potential may be the tool researchers and clinicians were looking for to address the third component of the aging process: the structural changes of the skin. For the past decade, these fat tissue cells have shown not only biocellular regenerative potential in vitro but also striking improvement of the quality of skin in clinical cases. Adipose tissue is easily harvested by minimally invasive liposuction and a large number of mesenchymal stem cells are obtained in the lipoaspirate. The wide availability of adipose tissue combined with the straightforward mechanical protocol to process the fat into a highly concentrated solution of progenitor cells brings regenerative medicine into real-life clinical practice. In 2013, Tonnard and colleagues described the procedure to produce so-called nanofat out of harvested microfat by a simple mechanical emulsification.
The mechanical protocol consists of emulsification of the harvested microfat, followed by filtering. The result is a whitish liquid with no viable adipocytes but with a large number of good-quality mesenchymal stem cells. Although adipocytes represent 80% to 90% of the volume of the harvested fat, they only represent 25% of the cell count. The remaining 75% is called the stromal vascular fraction (SVF). This contains a large amount of ADSCs, as well as endothelial cells, monocytes, macrophages, granulocytes, and lymphocytes.
The regenerative mechanism by which nanofat works is still not completely understood. Studies suggest that the multiple cell types in the SVF might work in combination to provide a microenvironment where numerous markers come together and trigger the regenerative capacity of the stem cell and of the tissue itself. Recent research has shown that the mechanical shear stress imposed on the fat during preparation of nanofat generates an upregulation of signaling pathways to enhance multipotent and pluripotent stem cells’ capacity to regenerate. The results of these complex intercellular crosstalking reactions were reported to range from enhanced collagen deposition and skin elasticity to formation of new blood vessels, tissue remodeling, thickening of the dermis, and downregulation of melanogenic activity. This wide range of regenerative properties brings nanofat grafting into focus for both cosmetic and reconstructive surgery.
This article describes the techniques and the authors’ experiences in nanofat grafting, as well as its potential new applications in regenerative medicine.
Preoperative evaluation and special considerations
With the clinically perceived benefit of nanofat and its applications, the authors are presently offering it to all our patients in whom at least 1 of the following items is present:
- 1.
Trophic skin changes associated with age and photodamage
- •
Thin dermis
- •
Fine wrinkles
- •
Craquelé surface (ie, neck, décolleté, perioral)
- •
Mucosal aging (ie, dry lips, genital)
- •
- 2.
Pigmentary conditions
- •
Pigmentary changes (ie, face, hands)
- •
Dark circles under the eye in cases of thin dermis associated with increased melanin pigment deposits
- •
- 3.
Scarring and atrophy
- •
Scars
- •
Radiodermatitis.
- •
There are no specific contraindications of its use and only transient yellowish staining is sometimes seen in the first postoperative week, followed by a mild inflammation that can last up to 3 weeks.
Nanofat does not have filling capacity. Thus, the idea in nanofat grafting is injecting regenerative cells and extracellular elements to promote tissue regeneration and remodeling. Clinically, nanofat grafting can be done alone or in association with other rejuvenation procedures (ie, facelift and lipofilling). Indications for nanofat extend beyond facial rejuvenation procedures; areas such as the neck, décolleté, and hands can also benefit from its use. Overall improvement of the quality of the overlying skin can be perceived after 6 to 8 months. Reported changes range from improvement in elasticity, pigmentary conditions, texture, and fine wrinkles. Its versatility, simplicity, and safety made nanofat an integral component of the authors’ clinical practices.
Surgical procedure
Harvesting
After infiltration of modified Klein solution (1:1.000.000), microfat is harvested under full-force vacuum aspiration into a sterile canister. The use of a fine 2.4-mm cannula with 20 1-mm sharpened holes (Tulip Medical, San Diego, CA, USA) was associated with an increased rate of ADSCs in the microfat when compared with conventional harvested fat. The lipoaspirate is then rinsed with saline or Ringer’s lactate over a sterile nylon cloth with 0.5-mm perforations mounted on a sterile canister. After removal of fibrous remnants with a mosquito, the obtained microfat is transferred to 10-mL Luer-Lok syringes.
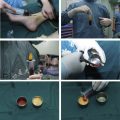
Nanofat Preparation by Intersyringe Shuffling
The mechanical protocol of nanofat preparation consists of a 2-step emulsification process followed by filtration. The first step is performed by vigorous shifting of the microfat from a full 10-mL syringe to an empty one through a 2.4-mm female-to-female Luer-Lok connector (Tulip Medical, San Diego, CA, USA). After 30 passes, the same process is repeated with a 1.2-mm female-to-female Luer lock connector for another 30 vigorous passes. This progressive emulsification process is important to guarantee that all adipocytes are destroyed. At the end of this emulsification process, a whitish discoloration of the fat is seen. The fat is now passed through a double 400-micron or 600-micron filter (disposable filter or permanent strainer cartridge) to remove connective tissue remnants (Tulip Medical, San Diego, CA, USA). When nanofat needling is planned, for every 10 mL of nanofat obtained, 1 mL of hyaluronic acid (HA) filler (cost ± €80), 100 mg of vitamin C, and 50 units of botulin toxin (cost ± €60) are added and mixed together. Preparation of the nanofat cream consists of mixing equal volumes of cream and nanofat.
Preparation of Recipient Site
When performed under local anesthesia, nanofat injections and nanofat needling to the face are well-tolerated after facial nerve blocks using lidocaine 1% (supraorbital, supratrochlear, infraorbital, and mental nerves). For neck and décolleté treatment, topical anesthesia (lidocaine 5% cream applied for 40 minutes before procedure) is usually sufficient. Under general anesthesia, no extra infiltration or block is needed. Marking from the earlier microfat grafting is removed before the needling to avoid transcutaneous tattooing.
Combining Treatment Modalities
Clinically, improvement of the quality of skin after nanofat grafting can be perceived after a minimum of 6 to 8 months. In an attempt to provide a shorter term enhancement of skin quality, the authors used a novel delivery system and used microbotox, skin booster HA, and vitamin C in our clinical practices, with obvious immediate results.
Microneedling
The authors first described the method of delivering nanofat through intradermal injection using 27-gauge needles. Although this approach is very effective for small areas, such as upper lip and eyelids, addressing bigger areas is time-consuming and it may be difficult to deliver the nanofat emulsion evenly throughout the area. Full-face treatment, as well as neck and décolleté treatment, benefit from a different delivery method.
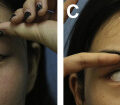
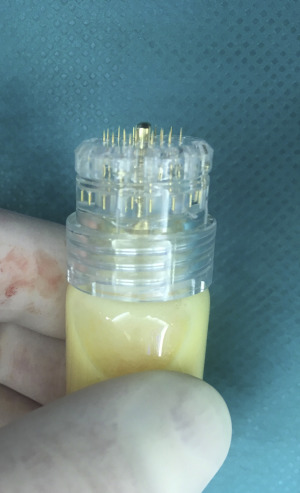
Verpaele and colleagues recently described a novel method of nanofat delivery using a microneedling device ( Fig. 1 ), the Hydra Needle 20 (Guangzhou Ekai Electronic Technology Co Ltd, Guangzhou, China). This method not only allows uniform delivery of nanofat in the created microchannels but also associates with the benefits of the microneedling itself. Microneedling is a well-established skin treatment that works by percutaneous collagen induction trough activation of a series of growth factors. Combining the regenerative capacity of the nanofat with the additional stimulus of collagen production and scarless healing provided by the needling may work synergistically to optimize results. The device contains 20 1.5-mm needles and is used by repetitive tapping motions to create the microchannels. The papillary dermis is reached as reflected by the punctuate bleeding obtained. The pump system in the needling device delivers the content of each bottle (up to 8 mL each) in thousands of tiny droplets of nanofat into the dermis. Needling is normally performed for 20 minutes, the time to empty the 8 mL vial.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree