Fat grafting is one of the most prevalent fields in facial rejuvenation at present. The procedures include the evaluation of recipient and donor areas, as well as fat harvesting, processing, and reinjection. Inappropriate treatment of each link may affect the final effect on the whole. The authors believe that understanding of facial anatomy and personalized therapy are the key to successful operation.
Key points
- •
Preoperative communication with the patient, management of expectation, careful evaluation, and marking of the operation areas are critical to postoperative satisfaction.
- •
The infiltration of tumescent solution to recipient areas could decrease incidence of intraoperative hemorrhage, fat embolism and postoperative hematoma.
- •
Asians are characterized by depressed midface and wide facial contour, with fat grafting in the shape of a “T”.
- •
Fat is mainly placed in the upper layer of periosteum and submuscular layer for structural support; a moderate amount of subcutaneous fat grafting forms a transition area with the surrounding tissue.
•The skin texture and color can be improved by microfat grafting for the subcutaneous and intradermal layers.
Video content accompanies this article at http://www.plasticsurgery.theclinics.com .
Introduction
Fat grafting has been widely used in facial rejuvenation in recent years. It can be applied to facial cosmetic alone or in combination with other facial lifting surgery. With age, the skin relaxes with a decrease in elasticity, and sags caused by the relaxation of supporting ligaments, accompanied by the volume loss and redistribution of the deep and superficial fat compartment, as well as the absorption of the underlying bone, all of which contribute to the senility of the facial morphology, such as facial hollowness and wrinkles. In the past, the applications of facial skin and superficial musculoaponeurotic system fascia lifting surgeries were expected to achieve facial rejuvenation, but often did not produce satisfactory results. With the understanding of changes in facial fat pad of facial aging, and the studies of tissue regeneration of the adipose cell and adipose-derived stem cell, plastic surgeons gradually realized the importance of treating facial aging by restoring the volume of soft tissue and improving the texture of skin through fat grafting.
However, owing to the unpredictable absorption of the fat, plastic surgeons expect to obtain better results through overgrafting, which often result in complications such as fat necrosis, oil cysts, calcification, or overcorrection. For the past 10 years, the authors have treated a large number of patients with facial rejuvenation by autologous fat grafting, acquiring satisfactory and long-lasting results without any severe complications. In this article, the authors introduce their preferred techniques of fat grafting for facial rejuvenation in Chinese patients.
Preoperative evaluation and special considerations
It is crucial to communicate with the patient in detail to identify the patient’s concerns and expectations. The patient should be made to understand the principles of fat grafting, therapeutic effects and complications to avoid unrealistic expectations and disappointment postoperatively.
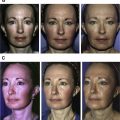
The facial features and aesthetic standards of Asians are different from those of Caucasians. Asians have a low forehead, flattening midface, collapse of nose, and retraction of chin. For aesthetic appreciation, a full forehead and a raised nose and chin are considered to be a symbol of charm and glamour; the smoothness and softness of the curves on lateral face are more emphasized. The zygomatic arch and mandibular angle should not be protruding. Consequently, the sites for facial fat grafting are formed a region of a “T”, aiming to create an inverted triangle on the face ( Fig. 1 ).
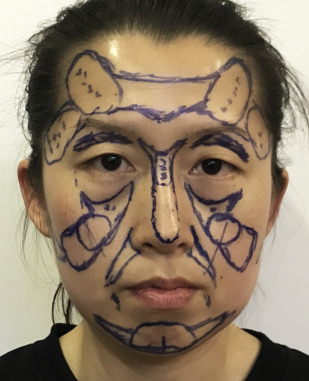
In the youth (<35 years), fat grafting aims at the correction of the middle face congenital depression, while improving the outline of lateral face to form soft curves. For those greater than 35 years, the skin texture can be improved through the regeneration of microparticle fat grafted into the superficial layer of the face. Therefore, individualized design of the distribution and amount of graft is performed according to gender, age, facial contour, skin texture, and degree of relaxation.
Surgical procedure
Donor Site Selection and Assessment
All fat deposits can be used as donor areas ( [CR] ). The purpose of surgery for some patients is not only to get facial rejuvenation, but also to improve body shape. Therefore, the patient’s expectations can be used for reference in the selection of the donor areas. If only rejuvenation is sought, the authors usually prefer to select the abdomen or thigh as donor site for the following reasons. First, liposuction and facial lipofilling can be performed in the supine position without changing posture. Second, fat grafts can be obtained relatively easily in these areas. In addition, it has been reported that there are greater concentrations of adipose-derived stem cells in the lower abdomen and medial thigh. It is a useful technique to assess the thickness of fat by skin grasping.
Fat Harvesting
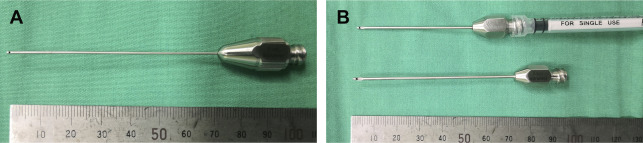
The operation is generally carried out under intravenous or local anesthesia (if less fat is needed). The incisions of liposuction should be concealed. The incision is made 2 mm long with a No. 11 blade after anesthetized with 2.0 mL of 1% lidocaine and 1:100,000 epinephrine. A 2.0-mm diameter 9-hole cannula is used for infiltration anesthesia ( Fig. 2 A), and tumescent solution (490 mL normal saline, 10 mL 2% lidocaine, and 1 mL 1:1000 epinephrine) is infiltrated into the deep and superficial layers of the subcutaneous fatty tissue as the cannula moves forward and backward. In this way, the tumescent solution can penetrate uniformly and the fibrous connective tissue can be loosened, which is helpful in the subsequent liposuction. We adopt the tumescent technique for liposuction and the ratio of tumescent solution to fat harvested is 3:1, waiting for at least 15 minutes before beginning liposuction to attain adequate anesthesia and hemostasis.
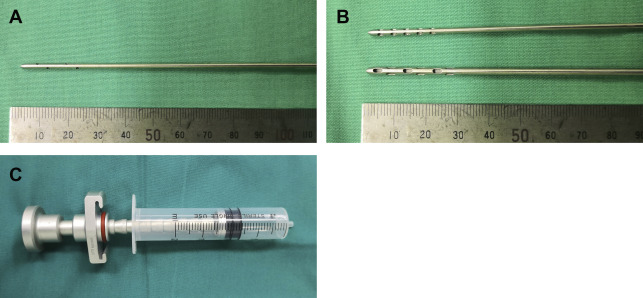
Lipoaspirate is harvested through the same incisions previously made for infiltration of tumescent solution. There are 2 kinds of liposuction cannulas with the same diameter of 2.5 mm and 9 side holes, the hole sizes are 3.0 mm × 1.0 mm and 1.0 mm × 0.8 mm, and can be used to obtain fat parcels of different sizes ( Fig. 2 B). The macrofat is used to fill into the deep layer as structural support and volume augmentation, and the microfat is used precisely in the superficial layer to counteract the effects of skin aging.
The liposuction cannula connected to a 20-mL syringe is inserted into the incision and fat grafts is harvested with anterior and posterior movements ( Fig. 2 C). To ensure minimal mechanical trauma to the fat parcels, the plunger is pulled back gently at 2 to 4 mL to minimize negative pressure and maintained by locking. In general, the amount of fat harvested should be at least twice as much as anticipated to ensure that there is an adequate quantity for grafting.
Fat Processing
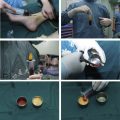
The authors are more inclined to adopt mesh/gauze for fat processing owing to its ability to remove more oily components and tumescent solution. It was reported that the fat obtained by the mesh/gauze technique contains more functional adipocytes and has a greater volume retention than that of the Coleman centrifugation technique.
The obtained lipoaspirate is transferred into 60-mL syringes through a connector. After simple precipitation, the aqueous portion is discharged and an equal volume of normal saline is brought into the 60-mL syringe containing 25 mL of precipitated fat twice for rinsing to remove blood, cellular debris, and any tumescent solution. After that, the fat is dumped on the metal filter with thick cotton pad below for 15 minutes to absorb any aqueous and oil components by capillary action. Meanwhile, the coarse fibrous tissues are manually removed to avoid cannula blockage. The purified fat is collected by 20-mL syringes and carefully transferred into 1-mm syringes through a connector. The fat should then be grafted immediately to minimize air exposure.
Preparation of the Recipient Site
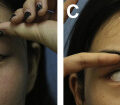
An anesthetic block (usually including the supraorbital nerves, infraorbital nerves, and mental nerves) with 1% lidocaine and 1:200,000 epinephrine is particularly effective in reducing discomfort and pain while the patient is awake. The recipient areas are infiltrated with tumescent solution (0.04% lidocaine with 1:1000,000 epinephrine) using an 18-G pointed needle and a 3-hole cannula with a length of 7 cm and a diameter of 1.0 mm ( Fig. 3 A). We need about 50 mL of tumescent solution to infiltrate the entire face. The infiltration of tumescent solution can promote vasoconstriction to decrease the risk of a vascular embolism; the concomitant decrease in bleeding is beneficial to the survival of the fat because it decreases the inflammatory response. During the procedure, it should be emphasized that the areas just infiltrated should be pressed by the palm to mitigate the effect of swelling on the surgeon’s judgment in the fat grafting process.