Abstract
At its most fundamental level, suction lipectomy involves a rigid cannula connected to a suction device and direct lipectomy involves a thorough understanding of cervicofacial anatomy with a discerning eye for facial contouring. We are in an exciting time in aesthetic medicine where there are many tools available for cervicofacial contouring. The authors believe in a multimodal approach using volume augmentation, soft-tissue redraping, and liposculpting for the best and most natural appearing results. This chapter provides preoperative guidelines for proper patient selection, reviews options for anesthesia, highlights necessary equipment, and outlines salient technical points.
Keywords
Cervicofacial lipectomy, Liposculpture, Suction lipectomy
History
Cervicofacial lipectomy, performed by liposuction or direct fat excision, is a powerful tool in lower face and neck rejuvenation. Lipectomy may be useful in younger and older patients to remove unwanted deposits of fat, contour the corpulent face, and as an adjunctive treatment of the aging face. Since its introduction into the United States in the early 1980s, liposuction has become the most commonly performed aesthetic procedure . Liposuction has been used from head to toe with reproducible results and minimal complications. Although the initial experience stemmed from its applications in body sculpting, suction lipectomy has become a powerful method to remove undesirable adipose tissue and contour the cervicofacial region. There is a wealth of literature documenting advances in techniques and instrumentation used in liposuction, and a review of the history of this technique is important to understand its fundamental principles and provide a context for evolving applications .
The earliest references to adipose tissue removal date to the 1920s in France . In 1921 Dujarrier removed fatty tissue from a ballerina’s leg using a uterine curette; this resulted in amputation secondary to vascular injury and gangrene. Initial catastrophic results such as this discouraged further attempts at lipoextraction for several decades. A more practical approach to lipoextraction was developed in the mid-1970s by Fischer and Fischer, who designed a cannula attached to a suction device to facilitate tissue removal . A similar approach was independently developed by Kesselring, who advocated suction-assisted lipectomy .
Although the addition of a suction device proved to be a major advance, problems with sharp-edged curettage instruments and large cavities created by wide tissue undermining persisted. Most of these problems were solved with the advent of the blunt technique, still in use today. Inspired by the Fischers’ work, Illouz in Paris reported his 5-year, 3000-case experience with suction-assisted lipolysis using a new blunt-tipped suction cannula . His “wet” technique included injection of the aspiration site with a hypotonic saline solution, theoretically to rupture the adipocytes. The blunt-tipped cannulas were connected to a high-power suction machine and were used to create tunnels in a fan-shaped manner to aspirate fat.
Fournier made further technical refinements on Illouz’s technique . He advocated a “dry” technique without preinfiltration of hypotonic solution as he did not believe that infiltration with hypotonic solution was necessary. Furthermore, Fournier proposed taping the suctioned areas to collapse the aspiration tunnels and advocated the idea of syringe liposuction as an alternative to suction pumps.
American surgeons visited France and learned the techniques of liposuction. In 1977 the first American to visit France was Field, a dermatologic surgeon . Other American surgeons followed, and in 1980 Martin, an otolaryngologist, visited Illouz and began to perform liposuction in Los Angeles in 1981. Soon, symposia and training courses were held to disseminate the techniques of liposuction. The American Society of Plastic and Reconstructive Surgeons was primarily under the tutelage of Illouz, whereas Fournier was largely responsible for encouraging participation and teaching physicians from all specialties. The first American course in liposuction was given by Newman, an otolaryngologist and cosmetic surgeon, and Dolsky, a plastic surgeon, in Philadelphia in 1982. Since that time, there has been great intellectual dialogue and innovation, leading to significant advances in cannula instrumentation, aspiration methods, and anesthetic techniques .
With advances in understanding of facial and cervical anatomy, surgeons have expanded on classical techniques and engaged in direct excision of submuscular fat previously thought to be inaccessible by liposuction. Historically, fat removal deep to the platysma was avoided because of concerns regarding neurovascular complications . More recently, however, Feldman and others have emphasized the importance of submuscular fat removal in appropriate patients to optimize results following necklifts . Still, most surgeons agree that subplatysmal fat is not conducive to liposuction, and if removal is warranted, should be approached with caution under direct visualization.
The buccal fat pad is another submuscular location that is best treated with direct excision. In 1732 Heister first described the buccal fat pad as a glandular unit, and in 1802 Bichat was the first to recognize that this glandular unit was predominantly fatty . The buccal fat pad was further described as having multiple extensions, and in 1997 Matarasso described pseudoherniation of the buccal fat pad as a new clinical entity . In addition, it is important to recognize that similar to periorbital and subplatysmal fat, the buccal fat pad behaves differently to subcutaneous fat and persists through times of emaciation. Indeed, following significant weight loss and reduction in subcutaneous fat, people will commonly have persistent buccal fat .
In the last two decades, facial sculpting techniques have allowed surgeons to contour both subcutaneous and submuscular fat with efficacy and minimal complications.
Personal Philosophy
Liposculpture has revolutionized aesthetic surgery of the face and neck by allowing surgeons to contour and improve anatomic regions not adequately addressed by lifting and redraping procedures; indeed, cervicofacial lipectomy has become an integral technique in the successful rejuvenation of the face and neck. The authors recognize that many excellent surgeons differ in the nuances of their lipectomy techniques. This chapter does not attempt to provide an impartial treatise on cervicofacial lipectomy, but rather provides a practical strategy born of significant clinical experience to produce optimal results.
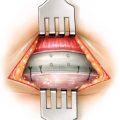
Within the overall population, the authors find that only a select group of patients benefit from primary cervicofacial liposuction alone. Such primary liposuction procedures are reserved for younger patients with localized adipose tissue and good skin tone, which allow for adequate skin contracture and redraping. In the authors’ practices, liposuction is frequently used in conjunction with other rejuvenation procedures of the face and neck (e.g., mentoplasty, plastysmaplasty, or rhytidectomy), and is most effective in recreating an acute cervicomental angle and helping to delineate a smoother jawline. The authors use both the tunneling technique to remove adipose collections in the submental region as well as the “layer” technique, in which a skin flap is elevated before aspiration ( Fig. 24.1 ). The authors find that the layering technique facilitates skin redraping without the risk of dimpling and skin irregularities from septal attachments inherent in the tunneling technique.
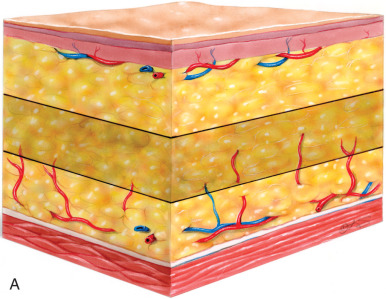
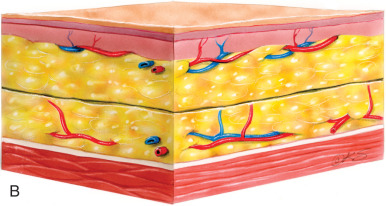
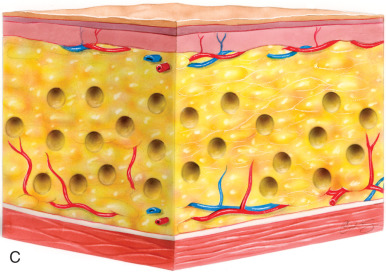
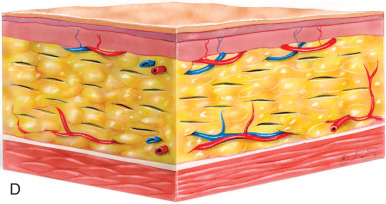
In the last decade the authors have noted a shift from the classic techniques and have engaged in more direct excisional lipectomy procedures in select patients to provide improved facial reshaping. This is in part based on sound anatomic studies, advances in surgical technique, and time-proven efficacy and safety. With this increased understanding and experience, the boundaries have expanded to allow optimal results in cervicofacial contouring. We advocate that a judicious mixture of both liposuction and direct fat excision in appropriate patients may be necessary for optimal results.
In all surgical endeavors, the authors strive for straightforward and safe techniques. For many aesthetic procedures, new instruments, equipment, and technology are being introduced to facilitate use, improve results, and minimize complications. However, these advancements need to be evaluated with a critical eye. At its most fundamental level, suction lipectomy involves a rigid cannula connected to a suction device and direct lipectomy involves a thorough understanding of cervicofacial anatomy with a discerning eye for facial contouring. We are in an exciting time in aesthetic medicine where there are many tools available for cervicofacial contouring. The authors believe in a multimodal approach using volume augmentation, soft-tissue redraping, and liposculpting for the best and most natural-appearing results. This chapter provides preoperative guidelines for proper patient selection, reviews options for anesthesia, highlights necessary equipment, and outlines salient technical points.
Anatomy
A thorough understanding of facial anatomy is critical to the successful application of lipectomy techniques. A comprehensive review of the head and neck is beyond the scope of this chapter, but it is important to highlight the anatomic structures relevant to facial liposculpture.
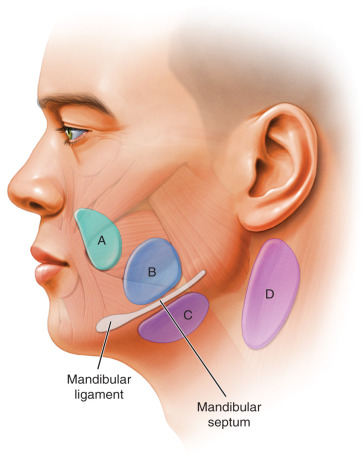
Fat in the area of the jowls and neck is highly compartmentalized . Fascial borders are encountered between the different zones of fat, and these borders originate in the superficial fascia and insert in the dermis of the skin . Dye injection studies have distinguished discrete superior and inferior subcutaneous fat compartments of the mandible . The superior jowl compartment is an inferior extension of the nasolabial folds and is bounded anteriorly by the oral commissure, whereas the inferior jowl is located lateral and inferior to the superior jowl fat. This inferior jowl pad is separated from the submandibular fat compartment by the mandibular septum, which inserts 1 cm superior to the mandibular border to the skin. The mandibular septum extends laterally to the angle of the mandible. Jowling is limited inferiorly by the septum and may occur with septal laxity ( Fig. 24.2 ).
Although various facial regions have been addressed with liposuction, the most commonly treated area remains the neck. Cervical anatomy has many variations, and the specific anatomic features pertinent to aesthetic appearance merit special attention. These considerations are critical in performing appropriate preoperative evaluation and tailoring the ultimate surgical approach.
The portion of the neck that is best addressed by liposuction is the central subunit, which is bounded superiorly by the inferior border of the mandible, posteriorly by the anterior border of the sternocleidomastoid muscle, and inferiorly by the thyroid cartilage. Beneath the skin lies a variable amount of fat. The quality of this fat varies from patient to patient as well as from one anatomic region to another. The adipose layer lies superficial to the platysma, a thin, broad-based muscle that originates from the superficial fascia over the pectoral and deltoid muscles, ascends over the clavicle, and inserts on the mandible below the oblique line and the skin at the lateral angle of the mouth. The posterior and superior borders extend in continuity with the superficial musculoaponeurotic system (SMAS). Significant variation may exist in the midline of the platysma, from the mentum to the hyoid bone. In some patients, the muscle fibers decussate across the midline, creating a muscular sling. In others, the absence of decussation may lead to a diastasis that worsens over time. Rejuvenation of the neck requires manipulation of one or more of these structures. It is important to note that optimal results following liposuction depend as much upon the resiliency and elasticity of the overlying skin as the amount of fat removed.
The marginal mandibular branch of the facial nerve is at risk when liposuction is directed over the mandible. The marginal mandibular nerve courses inferiorly, anterior to the angle of the mandible, 1 to 2 cm below the inferior margin of the mandible into the submandibular triangle. The nerve then ascends over the mandible to innervate the depressor muscles of the mouth 2 cm lateral to the oral commissure. Although the marginal mandibular nerve lies under the cover of the platysma, some patients may have attenuated muscle fibers; aggressive suctioning for jowls and mandibular contouring may place this nerve at risk of inadvertent injury.
Liposuction is usually performed in the adipose layer superficial to the platysma in the neck, an extremely safe region devoid of vital neurovascular structures. However, the surgeon will occasionally need to remove deeper layers of adipose tissue or dissect deep to the platysma to mobilize its medial ends for a platysmaplasty. Subplatysmal fat is also compartmentalized into the central fat (between the medial heads of the digastric muscle), medial fat (underlying the platysma), and lateral fat . Central fat is dark yellow, whereas the medial and lateral compartments are pale yellow, similar to buccal fat. Excision of subplatysmal fat warrants extreme caution given the risk of injury to the deep neurovascular structures. The anterior jugular veins and perforating branches of the submental vascular plexus lie deep to the platysma, near its midline. If violated, these vessels may be difficult to control, particularly with limited exposure and visualization.
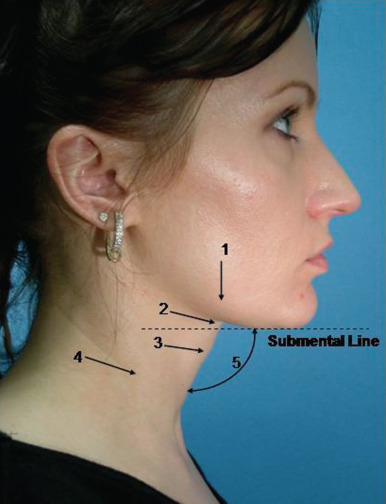
In 1980 Ellenbogen described five visual criteria that create the appearance of a youthful neck . These criteria are (1) a distinct mandibular border without jowl overhang; (2) a subhyoid depression, which gives the appearance of a long and thin neck; (3) a visible thyroid cartilage contour; (4) a visible anterior border of the sternocleidomastoid muscle; and (5) a cervicomental angle measuring between 105 and 120 degrees ( Fig. 24.3 ). These criteria were initially used to assess the results of platysma cervical lifts, but they are also applicable in the more global assessment of the neck. Not all of these criteria may be attainable with facial lipectomy, but they serve as useful guidelines for the goals of surgical treatment.
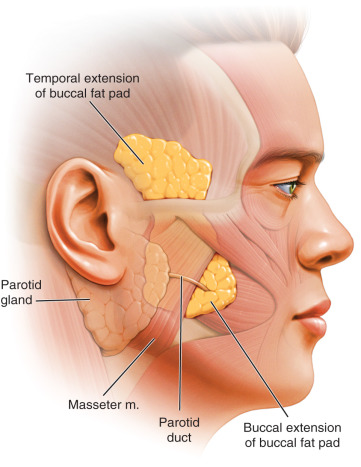
The buccal fat pad is usually located between the vertical masseter and horizontal buccinator, and is closely associated with the parotid duct and the facial nerve ( Fig. 24.4 ). Enveloped by the parotidomasseteric fascia, the buccal fat pad has been described as tubular in form with a main body and four extensions: the buccal, pterygoid, superficial, and deep temporal . The body and the buccal extensions are the most superficial segments and impart fullness to the cheeks and are clinically relevant for aesthetic surgery. Fifty percent of the volume of the buccal fat pad is within the body and buccal extension. The body rests centrally along the posterior maxilla and upper fibers of the buccinator. The buccal extension enters the cheek below the parotid duct and extends along the anterior border of the masseter, overlying the main portion of the buccinator. The parotid duct lies superficial to the fat pad and then penetrates the fat pad and the buccinator to enter the oral cavity opposite the maxillary second molar. Usually, directly beneath the parotid duct, lie several small branches of the facial nerve, including a large buccal branch. Its anterior limit is bounded by the facial vessels, which are in the same plane as the buccal fat pad. The buccal fat is enclosed by an extension of the parotid-masseteric fascia. This fascia encases the lateral surface of the masseter muscle and the branches of the fascial nerve. As it extends into the cheek beyond the anterior border of the masseter muscle, the fascia becomes more superficial and overlies the buccal fat pad, parotid duct, and the buccal branches of the facial nerve .
Preoperative Assessment
As with any cosmetic procedure, success depends on patient selection and careful preoperative evaluation. A full medical history should also be assessed to evaluate the appropriateness of surgical intervention and identify risk factors for suboptimal results. Comorbidities such as hypertension, coagulopathies, diabetes, and smoking may complicate healing in the postoperative period. Patients with significant weight gain are not good candidates for local lipectomy, as it is not a cure for overall obesity. However, lipectomy is effective for patients who are plagued with unwanted local deposits of fat, which may be a result of hereditary predisposition, poor dietary and exercise habits, age, medications, hormones, or weight gain. Even when weight loss regimens are implemented, facial areas such as the submental region are difficult to change. Although exercise programs help to tone muscles throughout the body, it is difficult to strengthen muscles of the face and neck; in addition, toned muscles do not necessarily reduce the amount of superficial adipose tissue.
A critical anatomic and aesthetic evaluation is essential. A systematic approach will prevent the surgeon from overlooking any critical anatomic features and from making an erroneous assessment of the locus of concern. Evaluation should start with an assessment of the patient’s overall body habitus. Patients of short and stocky stature with wide necks will not achieve a thin, contoured neck even with significant liposuction.
The surgeon must then assess the following:
- 1.
Skin condition. Skin should be evaluated for flexibility, elasticity, firmness, and adherence to the underlying tissues, all of which play a critical role in predicting outcomes . Skin with elastic integrity will more effectively redrape over the underlying liposculpted contour. Although it has been suggested that skin contractility may be suboptimal in patients older than 40 years , all patients need to be evaluated on an individual basis ( Fig. 24.5 ). Furthermore, crepe paper appearance of the skin is a preoperative predictor of failure from isolated liposuction without rhytidectomy .
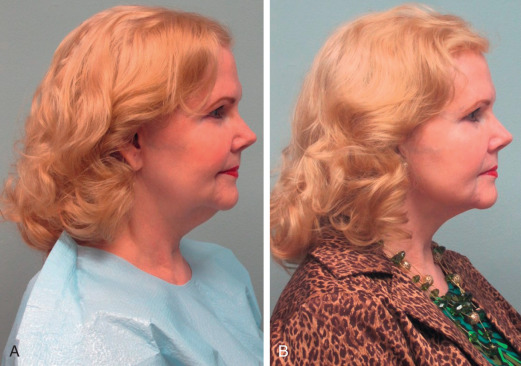
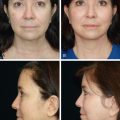
Figure 24.5
Preoperative profile (A) of a 65-year-old patient with submental and submandibular fullness. Although atypical of older patients, this patient’s skin contractility allowed for satisfactory improvement in the cervicomental angle with liposuction alone (B).
- 2.
Amount and location of fat. The surgeon should assess the location and amount of fat by palpation. This is best accomplished with the pinch and roll technique . The skin should be palpated or rolled between two fingers to determine the thickness of the skin and fat. In the cervical region, the presence of preplatysmal fat should be differentiated from subplatysmal fat. With palpation, subplatysmal fat is generally firmer owing to its connective tissue and fibrous content .
- 3.
Integrity of the platysma. The surgeon should evaluate the thickness and laxity of the platysma. The presence of platysmal bands at rest indicate that some form of platysmaplasty should be performed for proper rejuvenation of the neck . Furthermore, cervical liposuction may expose occult bands . This may be assessed by having patients strain their neck with their teeth clenched while making a grimace; with this provocative test, platysmal bands caused by laxity of the muscular anterior borders may be revealed.
- 4.
Condition of the surrounding skeletal framework. Deficiencies in the surrounding skeletal framework of the cervicofacial region may significantly affect the results of liposuction. Both Dedo and Kamer devised classification systems evaluating cervical abnormalities to guide preoperative evaluation and selection of the most appropriate surgical option . Dedo proposed that patients with either a short mandible-to-hyoid distance or low-lying hyoid have an obtuse cervicomental angle, limiting the effects of submental surgery ( Fig. 24.6 ). Correct projection of the mentum will give the impression of an acute cervicomental angle. To better assess this, the surgeon may drop a plumb-line down from the lower lip. In women, the mentum should be at or slightly behind this line when viewed from the lateral aspect. In men, the mentum should be on or slightly anterior to this line. In some patients, placement of a chin implant would accentuate the results of submental lipectomy; in others, the placement of cheek augmentation with volumizers or an implant will accentuate the results of buccal fat pad removal.
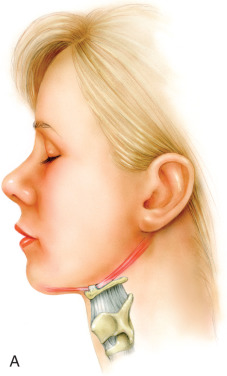
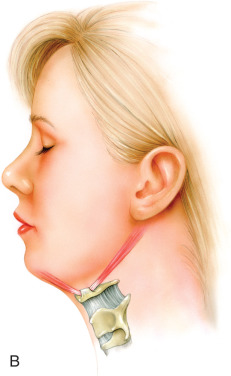
Figure 24.6
The hyoid bone should ideally rest cephalad and posterior to the mentum for a youthful neckline (A). A low-lying anterior hyoid bone limits the results of submental liposuction and cervical rejuvenation (B).
- 5.
Prominence of surrounding soft-tissue structures . The surgeon should assess for ptotic submandibular or large parotid glands. Liposuction in the submandibular region may enhance the appearance of the submandibular glands . Similarly, liposuction of cheek fat may enhance the anterior border of an enlarged parotid gland. Furthermore, patients with heavy masseter musculature may not benefit from facial liposuction.
Some patients are not good candidates for isolated lipectomy but may benefit from adjunctive procedures. Without offending patient sensibilities, the surgeon must recommend the procedure(s) likely to provide the most benefit. Obviously, the surgeon should make recommendations in light of the patient’s area of concern. For example, augmentation mentoplasty is a wonderful adjunct to cervical liposuction in creating the appearance of an acute cervicomental angle. However, most patients do not seek consultation with a surgeon for a chin implant; rather, they ask for improvement in their neck contour, and it is only when the advantage of an implant is pointed out that patients realize the benefits. Older patients need to be counseled that liposuction alone will not improve the appearance of aging skin or facial wrinkles. These patients may benefit from other rejuvenative procedures such as rhytidectomy or skin resurfacing.
Surgical Technique
The goals of cervicofacial lipectomy are to remove unwanted deposits of fat and to create a smooth contour. These goals are accomplished through liposuction of subcutaneous fat or by direct excision of undesirable submuscular fat. These procedures may be performed in isolation or in combination with other adjuvant therapies. Several technical nuances need to be appreciated to avoid complications and to optimize surgical results.
Equipment
A reliable aspiration device is essential to successful liposuction. Multiple suction devices are commercially available, but the most effective and efficient machines share several characteristic features. Although perfect vacuums (1 atm, 760 mm Hg [29.92 inches Hg]) are difficult to achieve in the clinical setting, suction devices are able to achieve vacuums close to 736 mm Hg (29 inches Hg). Low noise output (<55 dBA scale) and high flow rate (>100 L/min) are also desired features . In the cervicofacial region, vacuum pressures of 559 mm Hg to 584 mm Hg (22 to 23 inches Hg) are usually adequate for smooth and continuous suction. The surgeon should check the suction pressure before the start of any procedure to ensure that the pressure is within the desired range. Hand-held syringe liposuction, popularized by Fournier, is also a safe and efficient alternative to suction pump fat removal . Fournier believed this method minimized blood loss and provided the surgeon with accurate measurements of the amount of fat removed. Syringe liposuction is also an excellent backup should there be mechanical or electrical problems with a suction pump.
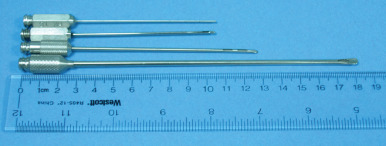
In addition to a reliable suction source, appropriate cannulas should be chosen. An abundance of cannulas are currently available ( Fig. 24.7 ). The surgeon will typically become familiar with three or four cannulas that he or she will use routinely, depending on the location and phase of liposuction (e.g., active fat removal, sculpting, or feathering). In the cervicofacial region, the most frequently used cannulas range in size from 1 mm (microcannulas) to 6 mm in diameter. Larger cannulas have the capacity to remove greater volumes of fat and are appropriate for areas such as the submental triangle. However, microcannulas are useful for fine sculpting and contouring, particularly in areas near vital neurovascular structures, such as the marginal mandibular nerve. Microcannulas are frequently used to contour the jowls, cheeks, and nasolabial folds.