This article explores whether some new acellular dermal matrices (ADMs) can be applied to breast augmentation or reconstruction revision, and particularly whether they can withstand the centripetal pull and prevent recurrent stretch deformities following periareolar mastopexy. Acellular dermis use in breast reconstruction and aesthetic breast revision is a fortuitous development, because their original purpose was for burn reconstruction. Although level 1 evidence remains lacking, ADMs have become integral adjuncts in breast reconstruction, complex hernia, and aesthetic breast revision. New applications continue to be explored, although these are in early stages of development and their long-term value remains to be confirmed.
- •
Meshed acellular dermal matrix (ADM) as an internal bra may help prevent bottoming out and maintain upper pole fullness over the long term after mastopexy.
- •
Early experience shows a potentially useful application of ADM donut- or washer-shaped grafts in revision periareolar mastopexy.
- •
ADM grafts for periareolar mastopexy may prevent areolar widening and unfavorable scarring.
- •
Permanent suture and mesh materials for mastopexy support may be complicated by biofilms, infections, and other late-presenting problems not associated with ADMs.
General considerations in mastopexy
Although a popular procedure, mastopexy continues to be plagued by long-term loss of upper pole fullness despite early good results. Mastopexy was initially conceived as a skin reshaping operation, with parenchyma adapting passively to the skin envelope. Results with these techniques were generally satisfactory and they became the standard approach for several years. Mastopexy techniques are still described according to the cutaneous scar configuration. However, the push to short scar techniques prompted a focus on parenchymal reshaping and less reliance on the skin envelope for support. Nevertheless, these may also relapse over time, and more extensive parenchymal dissection and mobilization in an attempt to enhance projection and upper pole fullness is not always an optimal solution.
An internal bra composed of deepithelialized dermis has been proposed as a means of maintaining shape while limiting tension on the skin envelope. However, because of the surface area required, it is suitable primarily for cases of “remarkable hypertrophy or severe ptosis” and has not become popular. Dermal bra procedures are generally limited to Wise pattern mastopexy, and are less appropriate for limited scar techniques.
Because of these difficulties in maintaining shape and projection, various mesh materials have been tried for additional support. Polypropylene mesh was used as early as 1981 with reduction mammaplasty. With the introduction of short scar techniques, the concept of an internal mesh bra in the subcutaneous layer was developed. Absorbable mesh has been used, with the hope that a scar layer would form in the configuration of the mesh bra, but this technique did not produce long-lasting results with periareolar mastopexy. In an attempt to maintain shape, a mixed mesh (40% polyester, 60% absorbable polyglactin) was used with reportedly better results, although long-term follow-up was not specified. Preshaped polyester mesh has also been used with reported success. Follow-up histology showed a mechanically strong but supple mesh with collagen ingrowth. Despite the success reported by some, other reports have shown that a permanent foreign body in the subcutaneous layer of the breast may be subject to biofilm and infection. These types of concerns about synthetic mesh in the breast have limited its adoption.
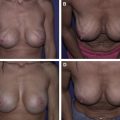
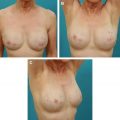
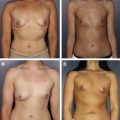
The use of autologous or cadaveric dermal slings for mastopexy mesh was reported by Colwell and Breuing in a series of 10 patients, 5 in each category. The authors proposed an algorithm for selecting either autologous tissue or ADM based on the quantity and quality of skin available. Results were stable at 6 months to 3 years in this series, indicating that tissue-based mesh could provide an alternative to synthetic mesh and durable results ( Fig. 1 ).
An acellular product, FortaPerm (Organogenesis, Canton, MA, USA), has also been used with periareolar mastopexy. FortaPerm is a highly crosslinked and laminated material derived from porcine intestinal submucosa, and its primary application is in urology, where it has been used for pubovaginal slings. It is believed to be slowly resorbed and replaced with a native collagen layer. For mastopexy support, the material is passed through a Zimmer mesher and the entire breast is wrapped. The ideal product would be noninflammatory and biocompatible, such as ADM, so it can be incorporated without loss of integrity.
Patient selection for ADM for mastopexy
Given the high cost of ADM materials, their use will likely become routine for primary mastopexy, despite the variability of long-term stability of shape and projection with standard techniques. However, for cases of recurrent ptosis or pseudoptosis, the use of a mesh bra provides an option. In the case of augmentation mastopexy with bottoming out, the use of ADM is well-established, so its use for mastopexy without implants represents an extension of the same concept. Patients who have experienced massive weight loss may have atrophic tissues despite an abundance of extra skin available for use as an autologous graft. In this sense, the same principle applies to patients receiving an implant and those with ptosis: replacing “like with like” through using a connective tissue matrix to reinforce weakened tissues that provide inadequate support. In addition, the cellular tissue requirements of an autogenous tissue are more demanding than those of the acellular dermal–collagen construct that ADMs provide, and also obviate the problems associated with thin, nonuniform pieces when trying to use the patient’s own tissues.
Patient selection for ADM for mastopexy
Given the high cost of ADM materials, their use will likely become routine for primary mastopexy, despite the variability of long-term stability of shape and projection with standard techniques. However, for cases of recurrent ptosis or pseudoptosis, the use of a mesh bra provides an option. In the case of augmentation mastopexy with bottoming out, the use of ADM is well-established, so its use for mastopexy without implants represents an extension of the same concept. Patients who have experienced massive weight loss may have atrophic tissues despite an abundance of extra skin available for use as an autologous graft. In this sense, the same principle applies to patients receiving an implant and those with ptosis: replacing “like with like” through using a connective tissue matrix to reinforce weakened tissues that provide inadequate support. In addition, the cellular tissue requirements of an autogenous tissue are more demanding than those of the acellular dermal–collagen construct that ADMs provide, and also obviate the problems associated with thin, nonuniform pieces when trying to use the patient’s own tissues.
Technical points: mastopexy hammock
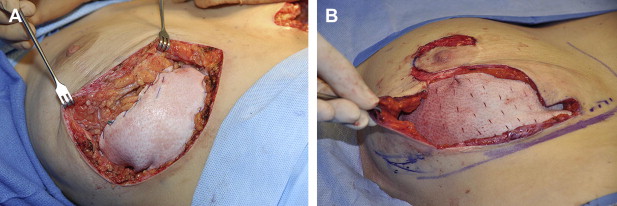
Given the limited experience with ADM mesh for mastopexy support, technical considerations are still evolving. A primary concern is selection of the appropriate ADM material. In expander/implant reconstruction, human-derived ADM may be favored because of its potential to expand, but this may be a counterproductive property for ptosis repair. For that reason, porcine-derived materials such as Strattice™ (LifeCell Corporation, Branchburg, NJ, USA) may be preferable. These materials are relatively inelastic and used for abdominal wall repair and revision implant surgery. However, the ability of porcine-derived ADM to conform to a three-dimensional contour is limited for the same reason. A premeshed version may become available, but a series of incisions with a #15 blade can suffice to expand and modify the product to some degree ( Fig. 2 ). Perforating may also improve the “take” of the material or minimize the risk of seroma formation in the subcutaneous plane, but too much may weaken it.
A critical decision in planning is the size and shape of the ADM. For a periareolar mastopexy, totally encasing the parenchymal mound in a cone of ADM may be required for optimal projection, as is done with synthetic and composite mesh materials using the Góes method. Most cases will probably only require a sling across the lower pole, analogous to a demi cup bra. Further experience will help refine the process for selecting the optimal size and orientation.
To provide fixation of the mesh at the boundaries of the breast mound, adequate undermining is required. Vigilance in attention to flap thickness is necessary because of the wider undermining. Fixation to chest wall is necessary unless the mesh is used only for shaping, but generally, setting the inframammary, medial, and lateral folds is helpful and necessary if a sling effect is desired. If possible, a cuff of the graft a few millimeters wide is splayed onto the chest wall and sutured with #00 polydioxanone or similar resorbable material. The anterior or superior edge may be sutured directly to the parenchyma or deepithelialized dermis. Sitting the patient upright to asses shape is critical before final tailoring and adjustments. Matching the internal bra to the skin envelope in the upright position avoids irregularities from redundancy and overresection leading to tension on the closure.
Periareolar Mastopexy
Periareolar mastopexy has a long history in breast surgery, dating back to the 1970s according to recent literature. Since its inception, it has been associated with a wide variety of complications or at least issues that have made it less than ideal with surgeons mainly adding a vertical component or looking at other techniques. These issues were well reviewed by Spear and colleagues in 1990 and 2001. As described, Góes has used the periareolar approach but also adds gland reshaping, and often uses internal mesh support to help hold the gland in position and remove periareolar tension. Hammond and colleagues described an excellent and intriguing technique of an interlocking polytetrafluoroethylene (Gore-Tex; W. L. Gore & Associates, Inc., Flagstaff, AZ, USA) suture that can maintain nice areolar shape but still has the potential for Biofilm, extrusion, and suture track infection. Secondary to these limitations, many surgeons, except in minimal nipple repositioning, have added a vertical component that helps limit the flattening from a periareolar mastopexy alone, unless some additional breast shaping is performed.
ADMs
Beginning with AlloDerm® in treating complex burn wounds and now extending into multiple uses and subspecialties, a multitude of ADMs are now being used in reconstructive breast surgery and a wide variety of ever-increasing applications across surgical specialties. As described throughout this issue of Clinics in Plastic Surgery, ADMs are being used to correct a wide variety of aesthetic breast complications, including malposition, stretch deformity, coverage issues of wrinkling and rippling, and capsular contracture among others. In only a matter of time they will make their way into primary breast procedures, and they have already been implemented primarily for breast reductions/mastopexies as an internal sling or hammock. This section reviews early experience with the use of a periareolar piece alone to provide support and long-term maintenance of areolar diameter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree