The expectations for improved results in postmastectomy reconstruction for women have increased in the past decade. The modified radical mastectomy has given way to breast conservation techniques using principles of skin preservation. Skin-sparing and nipple-sparing mastectomies have allowed plastic surgeons to perform breast reconstruction with the advantage of an intact skin envelope. Acellular dermal matrix is a biotechnological tissue prepared from either human or porcine skin. During processing, the cellular components that cause rejection and inflammation are removed, producing a structurally intact tissue matrix that serves as the biologic scaffold necessary for tissue ingrowth, angiogenesis, and tissue regeneration.
- •
Direct-to-implant immediate reconstruction has created a paradigm shift in surgery
- •
Direct-to-implant surgery is easily reproducible in immediate reconstruction
- •
Direct-to-implant surgery has acceptably low complication rates
- •
The use of acellular dermal matrix (ADM) allows the surgeon to insert implants without undue stress on overlying skin
- •
Skin-sparing and nipple areola–sparing mastectomies are excellent indications for direct-to-implant surgery
Overview
The expectations for improved results in postmastectomy reconstruction for women in 2011 have increased in the past decade. The surgical treatment of breast cancer has evolved since the era of Halstead’s radical mastectomy. The modified radical mastectomy has given way to breast conservation techniques using principles of skin preservation. The ultimate manifestation of this advancement can be seen in skin-sparing and nipple-sparing mastectomies. These innovations have provided plastic surgeons with the opportunity to perform breast reconstruction with the advantage of an intact skin envelope.
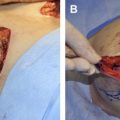
ADM is a biotechnological tissue prepared from either human or porcine skin. During processing, the cellular components that cause rejection and inflammation are removed, producing a structurally intact tissue matrix that serves as the biologic scaffold necessary for tissue ingrowth, angiogenesis, and, ultimately, tissue regeneration. ADM has been used extensively for soft tissue augmentation, including lip augmentation, depressed scar tissue repair, malar and submalar augmentation, rhinoplasty, and more recently for breast reconstruction. In all these settings, the ADM has shown good incorporation, with excellent postoperative healing, no resorption, and minimal risk for infection, extrusion, hematoma, or seroma. In addition, because this tissue is acellular, it may have greater tolerance for ischemia because it has the capability to remain in place without breakdown until vascular ingrowth and cellular integration develops. This process can be shown by a biopsy of the ADM at 6 weeks after surgery ( Fig. 1 ).
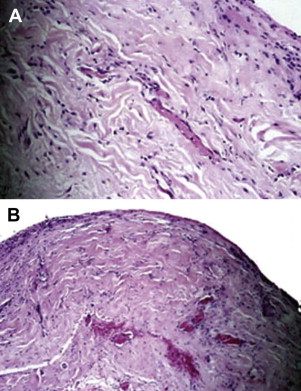
The Author’s Use of ADM s
In 2001, I began to make use of the unique properties of ADMs to provide coverage for either an implant or a tissue expander in breast reconstruction, and I have relied on 2 important conditions as selection criteria when deciding which type of prosthetic device to use:
- 1.
Vascularity of the overlying, postmastectomy skin envelope
- 2.
Whether or not additional skin surface area is required to create a natural breast shape.
Significantly, skin-sparing mastectomy allows the reconstructive surgeon to focus on how best to replace the glandular volume without the restraint of providing donor skin of similar color and texture. The question of which reconstructive technique to use has also become more complex and the emphasis is now on choosing the appropriate procedure for each patient. The current surgical repertoire comprises prosthetic techniques using tissue expanders and implants, and numerous autologous tissue flaps, including pedicled flaps, free tissue transfers, and perforator flaps.
With the discovery of genetic markers of breast cancer risk, the demand and indications for prophylactic mastectomy have increased. Furthermore, patients are rightfully adamant that their choices include procedures with reduced operative time and postoperative recovery. To meet these challenges, potential techniques needed to provide a combined, single-stage approach for both the mastectomy and the reconstruction. For many patients, the benefit of using a prosthetic approach is the simplicity of the procedures as well as the avoidance of distant donor-site morbidity. The advantages of a single, direct-to-implant operation, particularly in the patient needing prophylactic mastectomy, became obvious, and such operations have developed into a viable alternative to the other, more established reconstructive techniques. However, the surgical indications are specific and should be thoroughly familiar to both the surgeon and patient before selecting this direct to implant option.
Consultation for Direct-to-Implant Surgery
A comprehensive consultation with the patient before surgery is essential. This initial meeting provides the opportunity to review the risks and benefits of all reconstructive options as well as establishing candidacy for the direct-to-implant technique. This determination is directly related to the patient’s body habitus, the ablative nature of the surgery, and the specific desires of the patient for contralateral breast symmetry. Patients who are able to have skin-sparing or nipple areola–sparing mastectomies are prime candidates. In addition, expectations must be reviewed and a realistic understanding of the pros and cons of the surgery established.
Indications for Direct-to-Implant Technique
Skin-sparing mastectomy is indicated in most patients with breast cancer who are also planning for immediate reconstruction. Prophylactic mastectomy may be offered to patients who present with a high risk with or without genetic markers for developing breast cancer or for the patient who is considering prophylactic mastectomy on the opposite breast. In either situation, a direct-to-implant technique can be used.
The ideal candidate for the direct-to-implant technique is a woman with a medium or smaller breast size, grade 1 to 2 ptosis, and good skin quality. Patients with a history of smoking are required to abstain for 4 weeks before and after surgery. Morbidly obese patients are generally poor candidates for implant reconstruction and are usually better served by an autologous option.
Contraindications to the Direct-to-Implant Technique
There are few contraindications to the direct-to-implant technique.
Considerations in patients undergoing radiation therapy
An important consideration is how to proceed in the setting of radiation therapy. If the patient has received prior postlumpectomy radiation treatment and the skin changes are severe with a firm and nonexpansive skin envelope, it is our practice to recommend autologous tissue reconstruction. In our experience with those patients who have mild skin changes after receiving radiation therapy in the past, the chance of a vascular incorporation of the ADM in the radiated skin milieu is good, with an excellent indication for a successful outcome. A total of 40 patients in our series have received either preoperative or postoperative radiation treatments with no occurrence of capsular contracture, implant exposure, or infection requiring treatment.
In patients who are scheduled to receive adjuvant radiation therapy and who have declined an autologous tissue option, it is our practice to consider placement of a tissue expander in lieu of an implant. A pectoralis-ADM covering is created in the usual fashion. Expansion is performed rapidly with the goal volume reached before the initiation of the radiation treatment.
Skin viability
If there is any doubt as to the preoperative condition or intraoperative viability of the skin, then the procedure should be modified and an expander placed in the submuscular ADM pocket. A sufficient volume can then be injected into the expander; just enough to gently fill the skin envelope (hand-in-glove fit). In this way, skin tension can be avoided and filling of the expander can be performed once the skin has healed sufficiently.
In the past year, we have incorporated the use of intraoperative angiographic intravenous injection with the SPY (LifeCell Corp.) to assess the viability of the skin flaps after mastectomy and then after placement of the device. We have found that this technique not only provides instant feedback for the general/oncologic surgeon but also to the plastic surgeon who may see the effects of both the surgery and implant device on the overlying skin. The use of this technique in approximately 100 consecutive cases has predicted the final results.
Prophylactic mastectomy
A special consideration must be made for those patients presenting for prophylactic mastectomy who also desire a significant reduction in their breast size. In this situation, we do not recommend a nipple-sparing approach, because the viability of the nipple-areolar complex may be tenuous in the setting of a skin-reducing pattern or inverted-T incision. Skin pattern reduction, either vertical or Wise patterned, can be offered and used. Free nipple grafting has been performed in carefully selected settings with good outcome, but is subject to nipple loss from poor vascularity.
Preoperative Planning for Breast Implantation
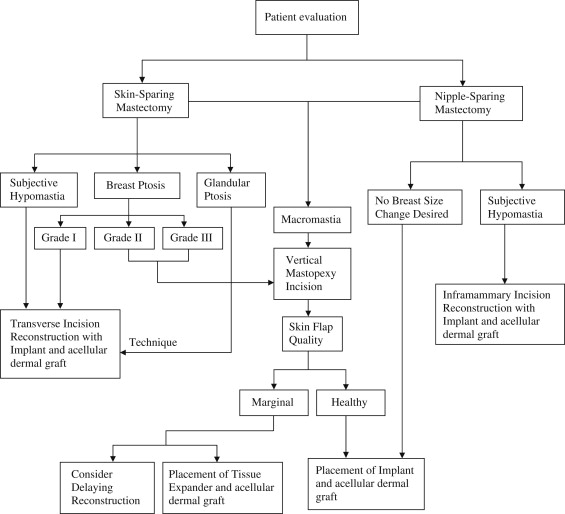
As stated previously, the quality of the skin flaps after mastectomy is a critical component for a successful outcome. Choosing the appropriately sized implant to fill the space beneath these flaps is also an important consideration. See the algorithm in Fig. 2 .
- •
We carefully measure the patient’s chest wall dimensions and also use an array of sizers before surgery to gauge the anticipated volume that will be required after the mastectomy
- •
In addition, a three-dimensional volumetric computer program is routinely used
- •
In our experience, smooth, round silicone gel implants provide the best projection and shape
- •
A notable point is to choose an implant base width that complements the chest diameter, because a concave lateral chest contour results if the implant is not sufficiently wide.