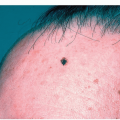
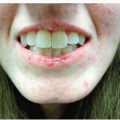
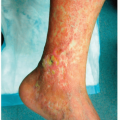
Cutaneous Manifestations of HIV Infection
OVERVIEW
The first organ that may be affected in human immunodeficiency virus (HIV) infection is the skin. Before the advent of highly active antiretroviral therapy (HAART) and cART (combination antiretroviral therapy), disease progression was accompanied by a variety of HIV-associated skin diseases described in this chapter. HIV infection was often suspected initially based on the occurrence of cutaneous diseases, such as Kaposi sarcoma (KS) or extensive molluscum contagiosum (MC), or in a patient with particularly severe or recalcitrant manifestations of a common skin disease, such as psoriasis or seborrheic dermatitis.
With the use of HAART and cART, the number and frequency of cutaneous manifestations have plummeted in the United States and other countries. Furthermore, in patients with advanced HIV infection, the cutaneous manifestations often remit spontaneously when such treatment is started. Nonetheless, some patients have viral resistance to these drugs or personal or economic reasons for not taking HIV medications, and in this group, the severe cutaneous manifestations of advanced HIV infection may still be seen, so it continues to be important for clinicians to be aware of the cutaneous manifestations of HIV.
Acute HIV infection is characterized by a transient blanchable erythematous morbilliform rash similar to the rash seen with other viral conditions and drug reactions, resembling measles. Fever, lymphadenopathy, sore throat, and malaise may accompany the eruption. The acute rash of HIV may appear several weeks after initial infection with HIV. As the number of CD4 cells decreases to fewer than 200 during the course of infection, signaling the onset of acquired immunodeficiency syndrome (AIDS), skin manifestations become more severe and increase in number.
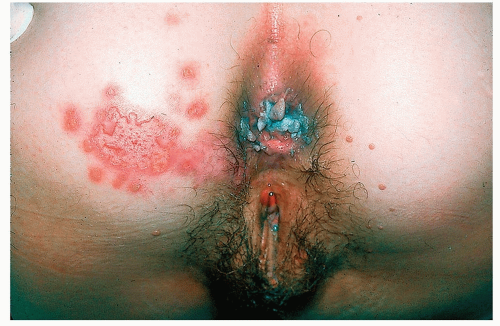
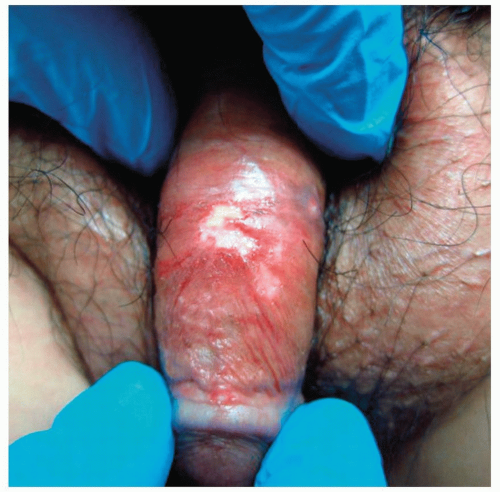 Figure 24-1 Herpes simplex. Shown here is an HIV-associated chronic ulcerated lesion that was resistant to acyclovir. He ultimately received intravenous foscarnet which helped heal his lesions. |
HIV-Associated Herpes Simplex (Figs. 24-1 and 24-2)
In the immunocompromised host, the clinical manifestations and course of herpes simplex virus (HSV) infection differs from those in immunocompetent patients (see Lips and Perioral Area, Genitals, and Diaper Area, Buttocks, and Gluteal Cleft). Recurrent oral and anogenital HSV infection is common in patients infected with HIV and may lead to chronic ulcerations.
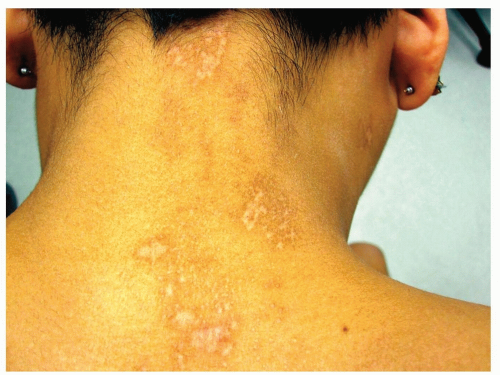
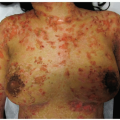
HIV-Associated Herpes Zoster (Figs. 24-3 and 24-4)
In patients with HIV-AIDS, cutaneous lesions may become extra-dermatomal, widespread, and prone to scarring.
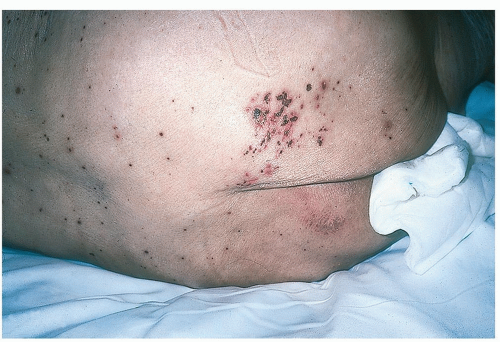 Figure 24-4 HIV-associated disseminated herpes zoster.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|