Cosmetic otoplasty is a very dynamic technique and the description of the procedure is in continual flux. Otoplasty is much like rhinoplasty, in that it is a combination of art and science riddled with nuances and precision. Searching PubMed or Google is testament to the hundreds or thousands of ways this procedure is described. As with many procedures with many permutations, new does not necessarily mean better. I think cosmetic otoplasty is very similar to facelift surgery, in that many of the short cut procedures fail to match the results of procedures that are over a half century old. Sometimes the basics are timeless.
Embryology
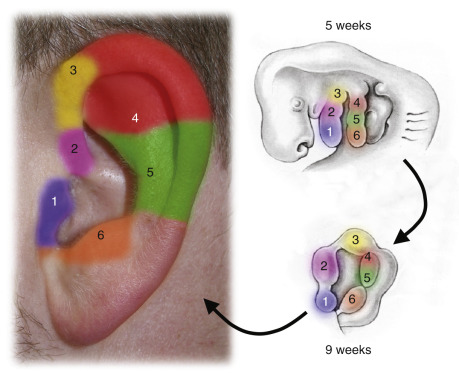
The external ear appears only in mammals. The internal, middle, and external ear development is a beautiful and complex embryologic orchestration. The classic description by His is as follows. The external ear forms from tissues of the first and second pharyngeal arches, which can be seen at 5 weeks ( Fig. 8.1 ). Six tissue elevations termed auricular hillocks of His become apparent at 6 weeks in utero ( Fig. 8.2 ). Three hillocks form from the first arch and three from the second arch. Each of the auricular hillocks forms a distinctive portion of the definitive external ear. For example, hillock 1 forms the tragus and hillock 6 forms the antitragus, as well as part of the helix ( Fig. 8.3 ). The lobule of the ear is not derived from the hillocks. The developing external ears are initially more caudal than the lower jaw. Growth of the lower jaw places the external ear in a relatively higher and more vertical orientation.
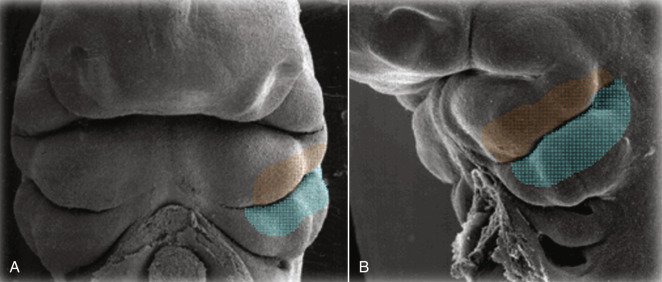

The classical embryologic tenets have been challenged. In this description, the first branchial arch contribution is limited to the tragus.
Normal Anatomy
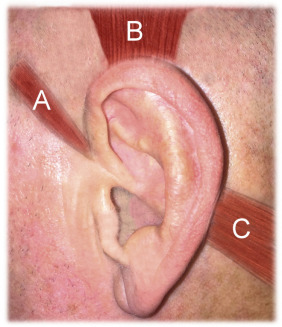
The developed external ear has evolved to capture and focus vibrations through the middle ear canal to the inner ear. In humans, many of the functions remain vestigial. Anyone who has ever witnessed animals whose life depends on detecting predators in nature, such as deer, has a better understanding of the complex movements and function of the mammalian external ear. Fig. 8.4 shows the normal anatomic components of the developed ear.
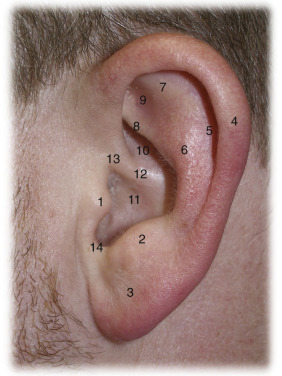
Other common measurements include the long axis of the ear, which inclines posteriorly at approximately a 20-degree angle from the vertical. The anterolateral aspect of the helix protrudes at a 21- to 30-degree angle from the scalp. The ear is positioned at approximately one ear length (5.5–7 cm) posterior to the lateral orbital rim between horizontal planes that intersect the eyebrow and columella.
The average length of a male auricle is 63.5 mm and the female 59 mm; the average width of the male auricle is 35.5 mm and the female is 32.5 mm. The helix should project 2–3 mm more laterally than the antihelix on the upper third of the ear on frontal view ( Fig. 8.5 ).

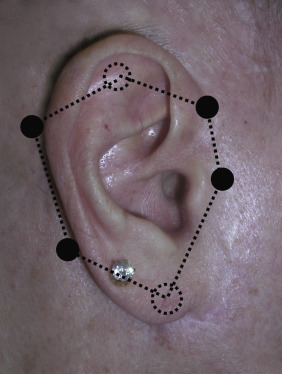
A very important measurement estimate to keep in mind is the distance that the auricle sits from the cranium. This will become paramount when diagnosing, planning, and performing cosmetic otoplasty. Although it varies from patient to patient, the distance from the temporal to lateral skin of the top of the helical rim is about 10–12 mm; the distance from the high mastoid region to the mid-helix is 16–18 mm; and the distance from the low mastoid skin to the lower portion of the helical rim is 18–22 mm ( Fig. 8.6 ). When making measurements for otoplasty on the top of the ear, I prefer to measure to the center of the helical rim, which averages 11 mm.

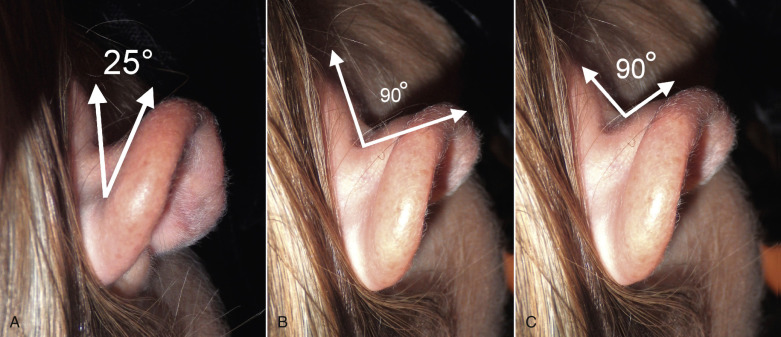
Classic otoplasty texts discuss complex angles of where the various components of the ear are in relation to other structures. These include the conchomastoid angle, conchocephalic angle, and auriculocephalic angle (also called the “cephaloauricular angle”) ( Fig. 8.7 ). These are often described differently in various texts and although they are important for the understanding of normal and abnormal ear posture, they are rarely used in treatment planning. I liken this to a facelift surgeon realizing a normal cervicomental angle is 90–110 degrees but not using this measurement in any way when performing facelift surgery. I rely much more on actual millimeter measurements than angles for otoplasty planning and surgery.
Neurologic Anatomic
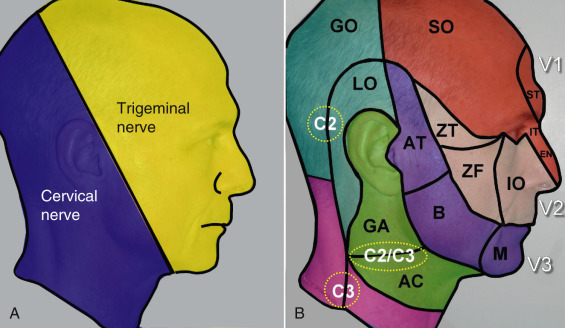
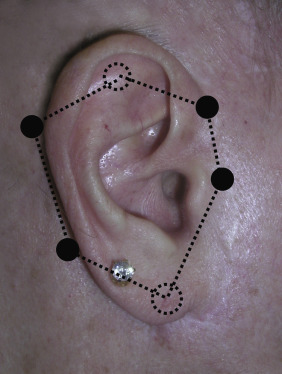
The auriculotemporal nerve is a branch of the mandibular division of the trigeminal nerve and supplies sensation to the tragus and helical crus. The anterior branch of the greater auricular nerve (from the cervical plexus) innervates most of the ear, including the helix, scapha, antihelix, concha, antitragus, external acoustic meatus, and lobule. The posterior branch of the greater auricular nerve also innervates some of the posterior ear. The mastoid branch of the lesser occipital nerve (from the cervical plexus) also innervates the posterior region of the external ear ( Figs. 8.8 , 8.9 ). The external auditory meatus also receives innervations from branches of the vagus (Arnold’s nerve) and glossopharyngeal nerves. The entire ear can be anesthetized by injecting local anesthesia along the base anteriorly and posteriorly. Supplemental anesthesia may be needed at the posterior wall of the external auditory canal supplied by the auricular branches of the vagus nerve (Arnold’s nerve). For other supplemental local anesthesia, a “ring block” is performed by injecting circumferentially around the ear ( Fig. 8.10 ).


Vascular Anatomy
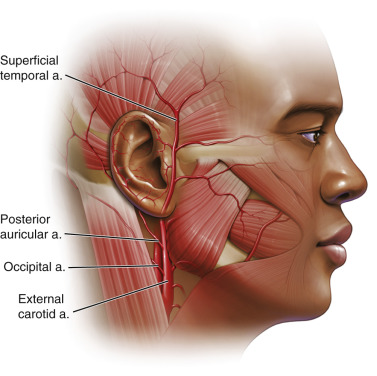
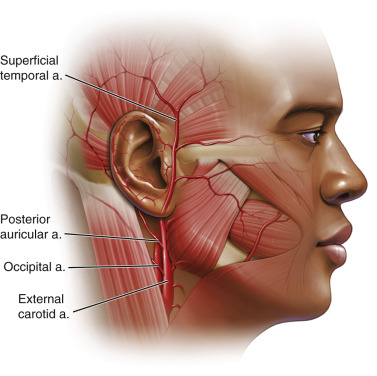
The arterial supply to the external ear are the posterior auricular from the external carotid, the anterior auricular from the superficial temporal, and a branch from the occipital artery.
The anterior arterial blood supply to the ear is primarily derived from the external carotid artery via the superficial temporal branch. The superficial temporal vessel exits the parotid capsule and passes under the anterior auricular muscle and divides into superior, medial, and inferior branches to supply the anterior surfaces of the auricle. The posterior auricular artery branches from the external carotid artery and runs parallel to the posterior auricular crease, deep to the posterior auricular muscle and greater auricular nerve. The posterior auricular artery (a branch of the external carotid) supplies the posterior surface of the ear and also has superior, medial, and inferior branches. The posterior ear also has arterial contribution from the mastoid branch of the occipital artery (a branch from the external carotid) ( Figs. 8.11 , 8.12 ).

The veins accompany the corresponding arteries. Venous drainage is from the superficial temporal and posterior auricular veins and lymphatic drainage is from the parotid preauricular nodes (anterior), the superficial cervical nodes (inferior), and the retroauricular (mastoid) nodes posteriorly.
Muscular Anatomy
The muscles of the auricle consist of two sets. The extrinsic, which connect it with the skull and scalp and move the auricle as a whole; and the intrinsic, which extend from one part of the auricle to another.
The extrinsic muscles are the anterior, superior, and posterior auricular ( Fig. 8.13 ). The anterior auricular , the smallest of the three, is thin, fan-shaped, and its fibers are pale and indistinct. It arises from the lateral edge of the galea aponeurotica, and its fibers converge to be inserted into a projection on the front of the helix. The superior auricular , the largest of the three, is thin and fan-shaped. Its fibers arise from the galea aponeurotica, and converge to be inserted by a thin, flattened tendon into the upper part of the cranial surface of the auricle. The posterior auricular consists of two or three fleshy fascicules, which arise from the mastoid portion of the temporal bone by short aponeurotic fibers. They are inserted into the lower part of the cranial surface of the concha.
The temporal branch of the facial nerve (cranial nerve VII) supplies the anterior and superior auricular muscles. The posterior auricular branch of cranial nerve VII supplies the posterior auricular muscle and the intrinsic auricular muscles. In humans, these muscles possess very little action: the anterior auricular draws the auricle forward and upward; the superior auricular slightly raises it; and the posterior auricular draws it backward. Some people have increased activity of this musculature and can wiggle their ears.
Cartilaginous Anatomy
The delicate and complex ear cartilage is one of the most unique anatomic forms in the body. The entire external ear possesses a cartilaginous framework, with the exception of the lobe and the tragal incisura ( Fig. 8.14 ).

Aberrant Anatomy
Prominauris is the condition of protruding ears. Growth disturbances of the auricle have been described to occur in 1 in 12,500 births or 5% of the population. The ear grows proportionally at a rapid rate, and 85% of ear development is complete by age 3. The ear is fully developed at 7–8 years of age. The fact that a small percentage of protruding ears are present at birth but a larger percentage seen at 1 year indicates that many cases of protruding ears are acquired deformities. The only difference between the neonatal ear and the adult ear is that, in the neonate, the cartilage is more malleable and soft. Otherwise, the anatomy is the same. Ear width reaches its mature size in boys at 7 years and in girls at 6 years. Ear length matures in girls at 12 and boys at 13 years of age. Ear cartilage becomes stiffer and calcified with age. Heredity plays an obvious part in the birth and development of protruding ears and is an autosomal dominant trait ( Fig. 8.15 ).

Lack of Antihelical Fold
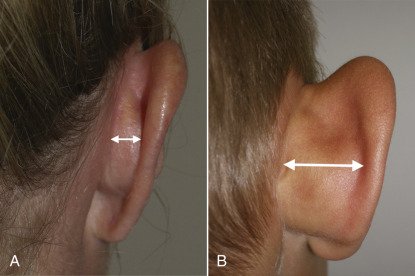
The antihelix includes the superior and anterior crus and forms a curvilinear separation between the conchal bowl and the scapha. The region between the crus is called the “fossa triangularis.” In developmental ear deformities, the antihelical fold is often ill-defined or absent ( Fig. 8.16 ). This deformity can be bilateral or unilateral.

Conchal Wall or Bowl Hypertrophy
Conchal bowl hyperplasia is a very common type of ear deformity leading to the protrusive ear. In this deformity, there is excessive growth of the poster wall of the concha and the chondroplasia can include the entire conchal bowl ( Figs. 8.17 , 8.18 ). The normal helical rim protrudes 10–20 mm from the mastoid skin in the lower posterior ear. This distance is increased with a hypertrophic conchal bowl.
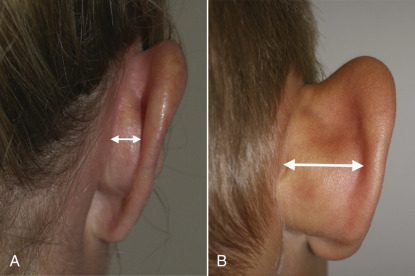
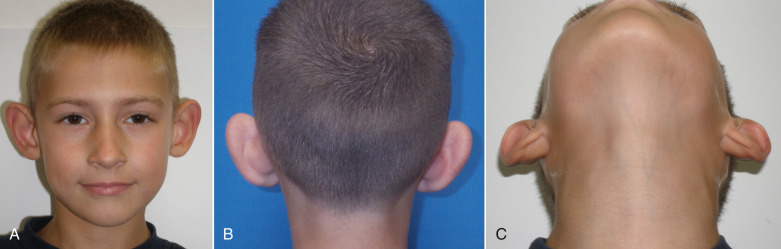
Combination Deformities
More commonly, patients exhibit the lack of an antihelical fold and conchal bowl hypertrophy simultaneously ( Fig. 8.19 ). This combination deformity is very common and is present in the majority of patients I have treated, as opposed to a sole deformity of undefined antihelical fold or posterior conchal wall excess.
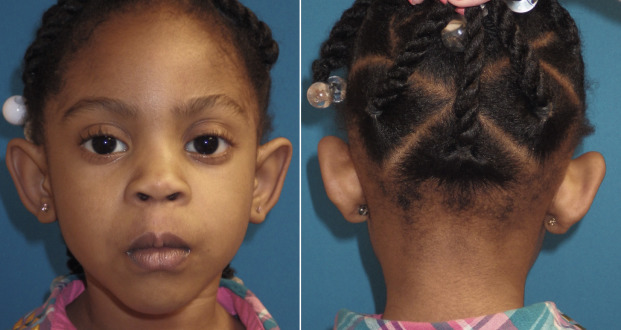
Many more complex deformities exist as a result of development such as microtia, cryptotia, and branchial arch syndrome, and their treatment is beyond the scope of this text.
Cosmetic Otoplasty Procedural Timing
One of the biggest challenges in otoplasty surgery is determining the proper age to undergo surgery. Despite being a benign condition, emotional trauma and behavioral problems, lack of self-esteem, and permanent damage to body image can be seen in children with protruding ears. These problems remain the prime reasons for performing surgery at an early age due to peer ridicule in primary school. Realizing this, the most opportune time to operate on most deformities is the preschool age. As 85% of ear development is complete by age 3 and the ear is fully developed at 7–8 years of age, there is little reason to wait for correction. Reviewing the literature shows surgeons performing ear surgery as early as 9 months of age but most surgeons agree that that otoplasty can be safely and effectively performed on 4 year olds.
Parents are often torn as how to approach the subject with a young child. I generally explain that it is elective surgery, so the only critical factor is if the child will be affected by peer ridicule. I also point out that virtually no children would select orthodontics but parents are proactive, as they understand the future implications on the child. Most children are not highly resistant to surgery and many are excited or apathetic. Children that are terrified present significant management problems and perhaps should be delayed for surgery until more mature. Children who are old enough to have been teased about their ears are often eager to have this elective surgery.
Nonsurgical Intervention
Nonsurgical correction of ear deformities, including prominent ears, usually have mixed results but recent advances have made neonatal treatment more predictable. Recent research has shown than newborn ear deformities are extremely common, affecting up to 30% of all full-term children (Jason Hall, Plastic Surgeon, Knoxville, TN, pers. comm.). Historically, pediatricians and plastic surgeons alike were advised to let the children “grow out of them,” as anatomic correction was not possible without complex external splinting. These splints had to be hand-designed and fabricated, and there was no standard treatment for all children. Surgeons and therapists have used a variety of materials in the past such as dental silicone, red-rubber catheters, tape, and skin adhesive alone or in combination, to treat these deformities. To further complicate treatment, any disruption of the device meant another lengthy and frustrating (for the parent and the surgeon) application. Results from these treatments were frequently suboptimal.
Unfortunately, only approximately one-third of external ear deformities self-correct. This leaves many newborns candidates for correction of deformities of the external ear. External ear molding in the newborn takes advantage of circulating maternal estrogens, which renders the cartilage of the external ear somewhat pliable until those estrogens disappear. At this point, the structure of the ear is difficult to change without surgical intervention. Constant, gentle pressure applied to the external ear during the period in which maternal estrogen is present in the newborn’s circulation, and that continues as this estrogen dissipates, will allow the auricular cartilage to assume a normal anatomic configuration (assuming proper pressure is applied). The estrogen levels are highest in the first 3 days after birth and decrease to normal levels by 6 weeks of age.
The EarWell Infant Ear Correction System (Becon Medical, Naperville, IL) is a device that allows for anatomic correction of most commonly seen types of deformities of the external ear: Stahl’s ear, lidding/lop ear, helical rim deformities, conchal crus deformities, prominent/cup ear, and cryptotia. In order for best results to be obtained, the device should be placed no later than 2 weeks after birth. Placement of the device in children older than 2 weeks of age leads to longer treatment times and less optimal establishment of the normal anatomic contour of the external ear. Getting patients in the office this early can be difficult, as pediatricians and parents can be hesitant to refer children to a surgeon in the early newborn period. This is compounded by the antiquated view held by many parents and practitioners that the majority of newborn external ear deformities self-correct. However, when children can be treated within the first 2 weeks of life, a nearly 100% correction of all but the most severe external ear deformities is routinely obtained.
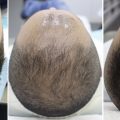
Placement of the device is straightforward for the experienced surgeon ( Fig. 8.20 ). After the diagnosis has been confirmed by physical examination, a thin strip of hair (1–2 cm wide) is shaved with the electric clippers supplied with the treatment kit. The skin is prepped with alcohol, and the self-adhesive cradle is applied to the child’s skin surrounding the ear. Helical rim and conchal formers are then placed within the cradle to correct the specific anatomic deformities present, and the perforated anterior shell is attached to the posterior cradle. This applies anterior forces to the retractors while allowing visual inspection of the child’s ear. Time from preparation to application is <5 min. The adhesive on the posterior cradle usually lasts for approximately 2 weeks, at which point the device is removed, the ear inspected, and a new device reapplied. A typical treatment course averages 6 weeks. However, if treatment can be initiated within the first week of life, treatment time can be shortened to 2 weeks with 95% efficacy.

Complications with the device are few and relatively minor. Skin breakdown at points of pressure from the device, usually in the conchal bowl in conchal crus deformities or at the helical rim, can occur, and are treated with local wound care and discontinuation of the device. These wounds usually occur after a few weeks of treatment, and heal uneventfully with local wound care. Skin irritation or erythema is sometimes seen. Discontinuation of treatment with a short course of antimicrobial cream (as these are usually superficial fungal infections caused by moisture around the device) is necessary before resuming treatment.
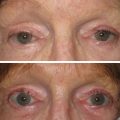
The EarWell Infant Ear Correction System is an effective means to correct external ear deformities in the newborn population that have a low likelihood of resolving spontaneously. This device is quick, easy to apply, painless for the patient, and allows for non-surgical correction of otherwise difficult anomalies of the external ear. Fig. 8.20 shows a before and after image of an infant treated with the EarWell device.
Surgical Procedures
Before any surgery is performed there is dialog that is very important to discuss with the patient and or caregivers. First, is the morphologic differences of ear symmetry. I explain to every single patient that it is rare that any otoplasty patient has ears that are exactly the same ( Fig. 8.21 ). Many patients have one ear larger or smaller than the other or one that sits higher or lower than the other. I further explain that if there is a discrepancy before surgery, there may likely be a small discrepancy after surgery. I elaborate that subtle asymmetries are what make us look natural. My explanation includes the statement that “otoplasty is a game of millimeters” and that I cannot guarantee that each ear will be exactly the same and that a several millimeter asymmetry is acceptable. Finally, I explain that the day after surgery when the dressing is removed the ears will be “pasted” down to the side of the head and appear over-corrected. They will relax over the next several months and revision surgery is not normally considered until the result stabilizes. It is very important to set the stage for these discussion preoperatively and have the patient sign off as part of the consent. Trying to explain the above points after surgery sounds like excuses.

As with any surgery, the surgeon must have a distinct set of goals in mind for appropriate surgical outcome. Classic goals of otoplasty include:
- •
Ear protrusion should be corrected by appropriate means for the specific diagnosis (antihelical fold, hypertrophic cartilage, or both)
- •
The helix of both ears should be seen beyond the antihelix from the front view
- •
The helix should have the appropriate thickness, taper and curve from top to bottom
- •
The postauricular sulcus should not be markedly decreased or distorted
- •
The helix-to-mastoid distance should fall in the normal range of 10–12 mm in the upper third, 16–18 mm in the middle third, and 20–22 mm in the lower third
- •
Realizing that minor asymmetry is normal and natural, the symmetry of any portion of one ear should be within 3 mm of the contralateral ear.
All patients are placed on Ciprofloxacin 500 mg BID for Pseudomonas coverage beginning 48 h before surgery and for 5–7 days after surgery.
Neurologic Anatomic
The auriculotemporal nerve is a branch of the mandibular division of the trigeminal nerve and supplies sensation to the tragus and helical crus. The anterior branch of the greater auricular nerve (from the cervical plexus) innervates most of the ear, including the helix, scapha, antihelix, concha, antitragus, external acoustic meatus, and lobule. The posterior branch of the greater auricular nerve also innervates some of the posterior ear. The mastoid branch of the lesser occipital nerve (from the cervical plexus) also innervates the posterior region of the external ear ( Figs. 8.8 , 8.9 ). The external auditory meatus also receives innervations from branches of the vagus (Arnold’s nerve) and glossopharyngeal nerves. The entire ear can be anesthetized by injecting local anesthesia along the base anteriorly and posteriorly. Supplemental anesthesia may be needed at the posterior wall of the external auditory canal supplied by the auricular branches of the vagus nerve (Arnold’s nerve). For other supplemental local anesthesia, a “ring block” is performed by injecting circumferentially around the ear ( Fig. 8.10 ).

Vascular Anatomy
The arterial supply to the external ear are the posterior auricular from the external carotid, the anterior auricular from the superficial temporal, and a branch from the occipital artery.
The anterior arterial blood supply to the ear is primarily derived from the external carotid artery via the superficial temporal branch. The superficial temporal vessel exits the parotid capsule and passes under the anterior auricular muscle and divides into superior, medial, and inferior branches to supply the anterior surfaces of the auricle. The posterior auricular artery branches from the external carotid artery and runs parallel to the posterior auricular crease, deep to the posterior auricular muscle and greater auricular nerve. The posterior auricular artery (a branch of the external carotid) supplies the posterior surface of the ear and also has superior, medial, and inferior branches. The posterior ear also has arterial contribution from the mastoid branch of the occipital artery (a branch from the external carotid) ( Figs. 8.11 , 8.12 ).
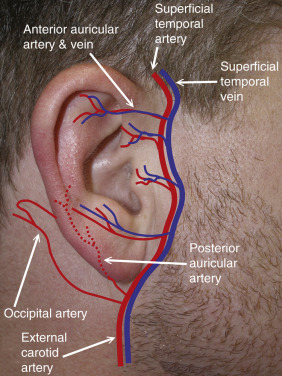
The veins accompany the corresponding arteries. Venous drainage is from the superficial temporal and posterior auricular veins and lymphatic drainage is from the parotid preauricular nodes (anterior), the superficial cervical nodes (inferior), and the retroauricular (mastoid) nodes posteriorly.
Muscular Anatomy
The muscles of the auricle consist of two sets. The extrinsic, which connect it with the skull and scalp and move the auricle as a whole; and the intrinsic, which extend from one part of the auricle to another.
The extrinsic muscles are the anterior, superior, and posterior auricular ( Fig. 8.13 ). The anterior auricular , the smallest of the three, is thin, fan-shaped, and its fibers are pale and indistinct. It arises from the lateral edge of the galea aponeurotica, and its fibers converge to be inserted into a projection on the front of the helix. The superior auricular , the largest of the three, is thin and fan-shaped. Its fibers arise from the galea aponeurotica, and converge to be inserted by a thin, flattened tendon into the upper part of the cranial surface of the auricle. The posterior auricular consists of two or three fleshy fascicules, which arise from the mastoid portion of the temporal bone by short aponeurotic fibers. They are inserted into the lower part of the cranial surface of the concha.
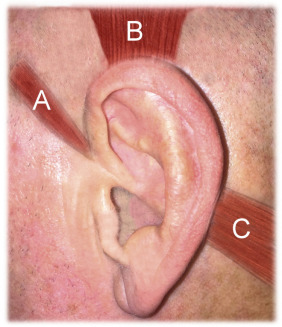
The temporal branch of the facial nerve (cranial nerve VII) supplies the anterior and superior auricular muscles. The posterior auricular branch of cranial nerve VII supplies the posterior auricular muscle and the intrinsic auricular muscles. In humans, these muscles possess very little action: the anterior auricular draws the auricle forward and upward; the superior auricular slightly raises it; and the posterior auricular draws it backward. Some people have increased activity of this musculature and can wiggle their ears.
Cartilaginous Anatomy
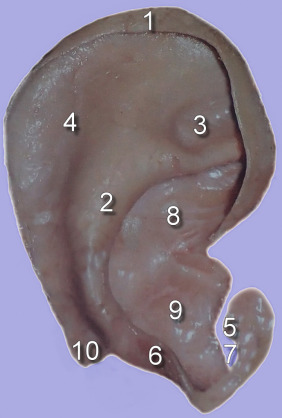
The delicate and complex ear cartilage is one of the most unique anatomic forms in the body. The entire external ear possesses a cartilaginous framework, with the exception of the lobe and the tragal incisura ( Fig. 8.14 ).
Aberrant Anatomy
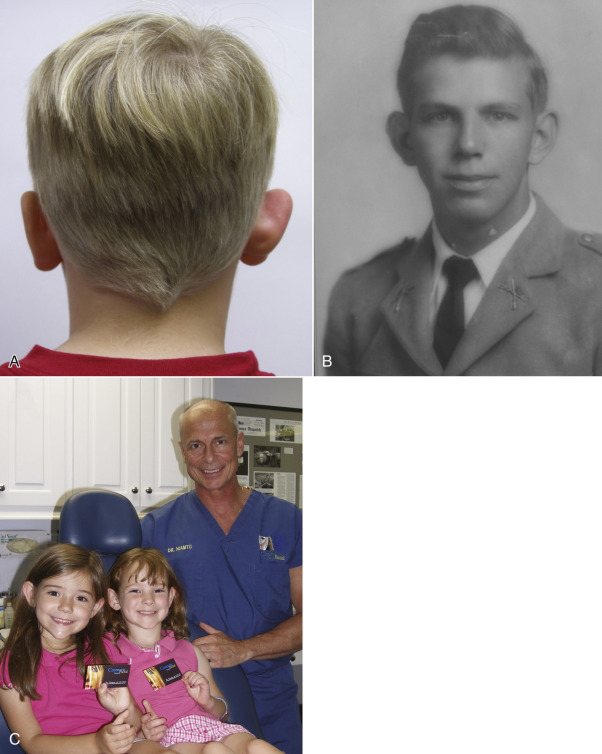
Prominauris is the condition of protruding ears. Growth disturbances of the auricle have been described to occur in 1 in 12,500 births or 5% of the population. The ear grows proportionally at a rapid rate, and 85% of ear development is complete by age 3. The ear is fully developed at 7–8 years of age. The fact that a small percentage of protruding ears are present at birth but a larger percentage seen at 1 year indicates that many cases of protruding ears are acquired deformities. The only difference between the neonatal ear and the adult ear is that, in the neonate, the cartilage is more malleable and soft. Otherwise, the anatomy is the same. Ear width reaches its mature size in boys at 7 years and in girls at 6 years. Ear length matures in girls at 12 and boys at 13 years of age. Ear cartilage becomes stiffer and calcified with age. Heredity plays an obvious part in the birth and development of protruding ears and is an autosomal dominant trait ( Fig. 8.15 ).
Lack of Antihelical Fold
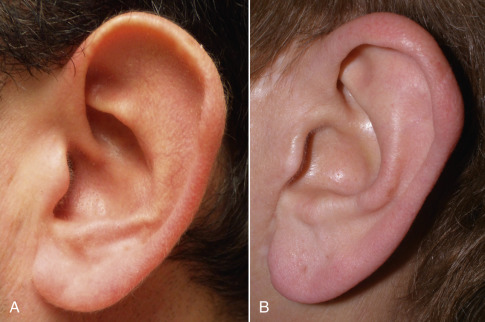
The antihelix includes the superior and anterior crus and forms a curvilinear separation between the conchal bowl and the scapha. The region between the crus is called the “fossa triangularis.” In developmental ear deformities, the antihelical fold is often ill-defined or absent ( Fig. 8.16 ). This deformity can be bilateral or unilateral.
Conchal Wall or Bowl Hypertrophy
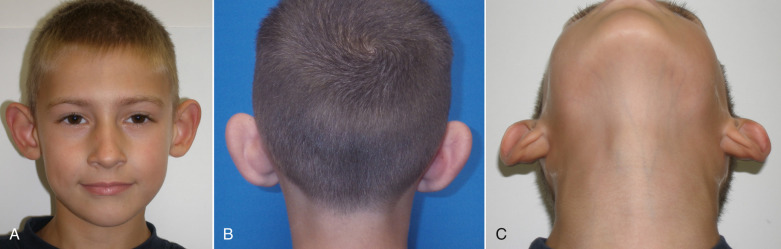
Conchal bowl hyperplasia is a very common type of ear deformity leading to the protrusive ear. In this deformity, there is excessive growth of the poster wall of the concha and the chondroplasia can include the entire conchal bowl ( Figs. 8.17 , 8.18 ). The normal helical rim protrudes 10–20 mm from the mastoid skin in the lower posterior ear. This distance is increased with a hypertrophic conchal bowl.
Combination Deformities
More commonly, patients exhibit the lack of an antihelical fold and conchal bowl hypertrophy simultaneously ( Fig. 8.19 ). This combination deformity is very common and is present in the majority of patients I have treated, as opposed to a sole deformity of undefined antihelical fold or posterior conchal wall excess.
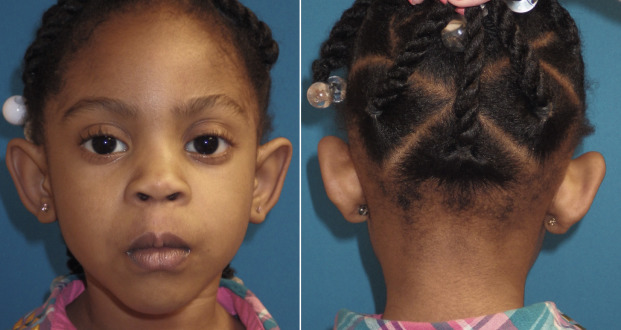
Many more complex deformities exist as a result of development such as microtia, cryptotia, and branchial arch syndrome, and their treatment is beyond the scope of this text.
Cosmetic Otoplasty Procedural Timing
One of the biggest challenges in otoplasty surgery is determining the proper age to undergo surgery. Despite being a benign condition, emotional trauma and behavioral problems, lack of self-esteem, and permanent damage to body image can be seen in children with protruding ears. These problems remain the prime reasons for performing surgery at an early age due to peer ridicule in primary school. Realizing this, the most opportune time to operate on most deformities is the preschool age. As 85% of ear development is complete by age 3 and the ear is fully developed at 7–8 years of age, there is little reason to wait for correction. Reviewing the literature shows surgeons performing ear surgery as early as 9 months of age but most surgeons agree that that otoplasty can be safely and effectively performed on 4 year olds.
Parents are often torn as how to approach the subject with a young child. I generally explain that it is elective surgery, so the only critical factor is if the child will be affected by peer ridicule. I also point out that virtually no children would select orthodontics but parents are proactive, as they understand the future implications on the child. Most children are not highly resistant to surgery and many are excited or apathetic. Children that are terrified present significant management problems and perhaps should be delayed for surgery until more mature. Children who are old enough to have been teased about their ears are often eager to have this elective surgery.
Nonsurgical Intervention
Nonsurgical correction of ear deformities, including prominent ears, usually have mixed results but recent advances have made neonatal treatment more predictable. Recent research has shown than newborn ear deformities are extremely common, affecting up to 30% of all full-term children (Jason Hall, Plastic Surgeon, Knoxville, TN, pers. comm.). Historically, pediatricians and plastic surgeons alike were advised to let the children “grow out of them,” as anatomic correction was not possible without complex external splinting. These splints had to be hand-designed and fabricated, and there was no standard treatment for all children. Surgeons and therapists have used a variety of materials in the past such as dental silicone, red-rubber catheters, tape, and skin adhesive alone or in combination, to treat these deformities. To further complicate treatment, any disruption of the device meant another lengthy and frustrating (for the parent and the surgeon) application. Results from these treatments were frequently suboptimal.
Unfortunately, only approximately one-third of external ear deformities self-correct. This leaves many newborns candidates for correction of deformities of the external ear. External ear molding in the newborn takes advantage of circulating maternal estrogens, which renders the cartilage of the external ear somewhat pliable until those estrogens disappear. At this point, the structure of the ear is difficult to change without surgical intervention. Constant, gentle pressure applied to the external ear during the period in which maternal estrogen is present in the newborn’s circulation, and that continues as this estrogen dissipates, will allow the auricular cartilage to assume a normal anatomic configuration (assuming proper pressure is applied). The estrogen levels are highest in the first 3 days after birth and decrease to normal levels by 6 weeks of age.
The EarWell Infant Ear Correction System (Becon Medical, Naperville, IL) is a device that allows for anatomic correction of most commonly seen types of deformities of the external ear: Stahl’s ear, lidding/lop ear, helical rim deformities, conchal crus deformities, prominent/cup ear, and cryptotia. In order for best results to be obtained, the device should be placed no later than 2 weeks after birth. Placement of the device in children older than 2 weeks of age leads to longer treatment times and less optimal establishment of the normal anatomic contour of the external ear. Getting patients in the office this early can be difficult, as pediatricians and parents can be hesitant to refer children to a surgeon in the early newborn period. This is compounded by the antiquated view held by many parents and practitioners that the majority of newborn external ear deformities self-correct. However, when children can be treated within the first 2 weeks of life, a nearly 100% correction of all but the most severe external ear deformities is routinely obtained.
Placement of the device is straightforward for the experienced surgeon ( Fig. 8.20 ). After the diagnosis has been confirmed by physical examination, a thin strip of hair (1–2 cm wide) is shaved with the electric clippers supplied with the treatment kit. The skin is prepped with alcohol, and the self-adhesive cradle is applied to the child’s skin surrounding the ear. Helical rim and conchal formers are then placed within the cradle to correct the specific anatomic deformities present, and the perforated anterior shell is attached to the posterior cradle. This applies anterior forces to the retractors while allowing visual inspection of the child’s ear. Time from preparation to application is <5 min. The adhesive on the posterior cradle usually lasts for approximately 2 weeks, at which point the device is removed, the ear inspected, and a new device reapplied. A typical treatment course averages 6 weeks. However, if treatment can be initiated within the first week of life, treatment time can be shortened to 2 weeks with 95% efficacy.
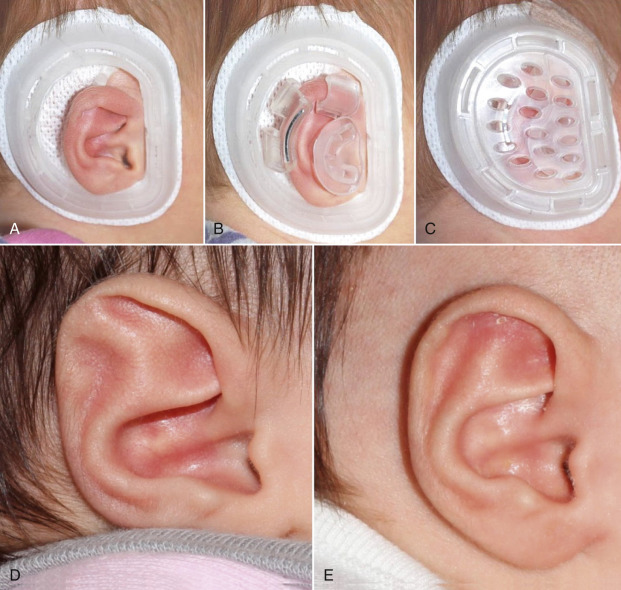
Complications with the device are few and relatively minor. Skin breakdown at points of pressure from the device, usually in the conchal bowl in conchal crus deformities or at the helical rim, can occur, and are treated with local wound care and discontinuation of the device. These wounds usually occur after a few weeks of treatment, and heal uneventfully with local wound care. Skin irritation or erythema is sometimes seen. Discontinuation of treatment with a short course of antimicrobial cream (as these are usually superficial fungal infections caused by moisture around the device) is necessary before resuming treatment.
The EarWell Infant Ear Correction System is an effective means to correct external ear deformities in the newborn population that have a low likelihood of resolving spontaneously. This device is quick, easy to apply, painless for the patient, and allows for non-surgical correction of otherwise difficult anomalies of the external ear. Fig. 8.20 shows a before and after image of an infant treated with the EarWell device.
Surgical Procedures
Before any surgery is performed there is dialog that is very important to discuss with the patient and or caregivers. First, is the morphologic differences of ear symmetry. I explain to every single patient that it is rare that any otoplasty patient has ears that are exactly the same ( Fig. 8.21 ). Many patients have one ear larger or smaller than the other or one that sits higher or lower than the other. I further explain that if there is a discrepancy before surgery, there may likely be a small discrepancy after surgery. I elaborate that subtle asymmetries are what make us look natural. My explanation includes the statement that “otoplasty is a game of millimeters” and that I cannot guarantee that each ear will be exactly the same and that a several millimeter asymmetry is acceptable. Finally, I explain that the day after surgery when the dressing is removed the ears will be “pasted” down to the side of the head and appear over-corrected. They will relax over the next several months and revision surgery is not normally considered until the result stabilizes. It is very important to set the stage for these discussion preoperatively and have the patient sign off as part of the consent. Trying to explain the above points after surgery sounds like excuses.
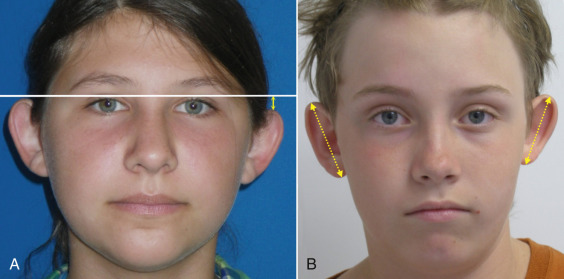
As with any surgery, the surgeon must have a distinct set of goals in mind for appropriate surgical outcome. Classic goals of otoplasty include:
- •
Ear protrusion should be corrected by appropriate means for the specific diagnosis (antihelical fold, hypertrophic cartilage, or both)
- •
The helix of both ears should be seen beyond the antihelix from the front view
- •
The helix should have the appropriate thickness, taper and curve from top to bottom
- •
The postauricular sulcus should not be markedly decreased or distorted
- •
The helix-to-mastoid distance should fall in the normal range of 10–12 mm in the upper third, 16–18 mm in the middle third, and 20–22 mm in the lower third
- •
Realizing that minor asymmetry is normal and natural, the symmetry of any portion of one ear should be within 3 mm of the contralateral ear.
All patients are placed on Ciprofloxacin 500 mg BID for Pseudomonas coverage beginning 48 h before surgery and for 5–7 days after surgery.
Surgical Techniques
So many techniques exist for cosmetic otoplasty it is impossible to cover them all. This chapter presents the two techniques that can be applied to the most common ear deformities and have produced safe, stable, and predictable results for decades. Although I have performed other techniques for otoplasty, including conchal set back and cartilage splitting procedures, they have not provided the predictability as the procedures described below.
The key to successful and predictable otoplasty is to first make the proper diagnosis and second to perform the correct procedure for the specific diagnosis or diagnoses. If a patient has a problem from conchal bowl cartilage excess, a suture procedure is an incorrect choice as it does not address the true diagnosis of excess cartilage. The same can be said about the absence of an antihelical fold. Removing cartilage will not help and suture reconstruction of the antihelical fold is required. Finally, most patients have combination deformities and require both cartilage reduction and antihelical fold reconstruction with sutures.
Mustardé Otoplasty for Antihelical Fold Reconstruction
The commonest procedure for otoplasty is the Mustardé otoplasty, as described by Dr. Jack Mustardé, Jr, in 1963. Dr. Mustardé was an ophthalmologist with a 60 year, very storied career, including being a prisoner of war in the Second World War, and funding and establishing the first plastic surgery hospital in western Africa. He was a renaissance man in many ways and figured out a simple solution to protruding ears. I often wonder why such a simple suture technique was not put forth a century earlier.
This chapter focuses on the simplest procedure for the simplest diagnoses and proceeds to the more complex approaches. The simplest deformity in prominauris is the absence or hypoplasia of the antihelical fold. In this situation, the conchal bowl is of normal proportion and if the ear is manually folded back, a normal antihelical fold appears ( Fig. 8.22 ).
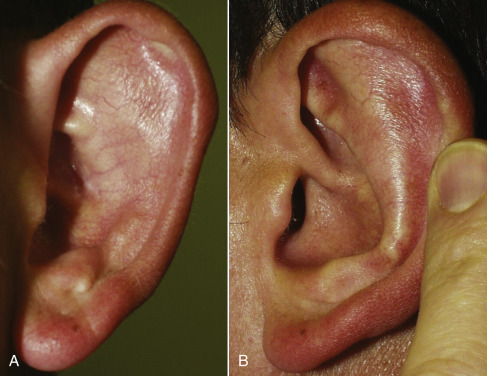
It may be confusing for novice surgeons to decide the appropriate procedure to set back the ear. In a patient with a simple lack of antihelical fold with a normal conchal bowl, pushing the pinna posterior as shown in Fig. 8.23 improves the deformity. If the patient has conchal bowl hypertrophy, pushing the upper ear distorts the pinna and does not move the ear as a whole. Pushing on the middle of the ear, however, produces a more natural result. This is due to the fact that pushing on the middle of the ear buckles the hypertrophic conchal bowl (in a similar manner that cartilage reduction) and sets the entire ear posterior. This maneuver means that this patient would not be a candidate for Mustardé otoplasty but rather needs cartilage reduction of the conchal bowl. In many cases, the patient may need both procedures. Patients with a normal antihelical fold but protruding ears, may only need conchal bowl reduction and not a Mustardé procedure.
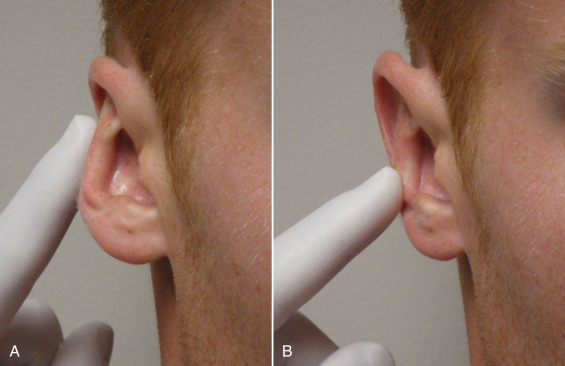
Again, the Mustardé procedure is most effective and stable on patients with normal conchal bowl cartilage dimensions but without a normal antihelical fold. As shown, folding the ear recreates the fold, the cartilage weakening and mattress sutures assist to hold the new fold in place during healing. Attempting to perform this procedure in a patient with conchal cartilaginous hypertrophy will not properly address the deformity and limit stability.
Many patients will actually need the Mustardé procedure and simultaneous cartilage reduction, and I frequently perform the Mustardé procedure first. Some surgeons worry about manipulating the sutured antihelix while trimming cartilage. Two to three Mustardé sutures maintains stability that allows moderate manipulation without disrupting sutures while reducing the cartilage. In previous texts, I outlined the combined procedure by performing the conchal bowl cartilage reduction (Davis procedure) first and then finishing with the Mustardé procedure. Further experience has shown more accurate surgery by performing the Mustardé procedure first, then removing cartilage as needed for passive ear position. I have not had a problem with disrupting the Mustardé sutures during the second part of the procedure. Technically, there is no right or wrong way to do this and surgeon preference may vary. If the surgeon places the Mustardé sutures first and is gentle with them (not disrupting them), I believe that the subsequent conchal bowl reduction can be performed in a more conservative and more accurate manner.
Mustardé Procedure Preoperative Marking
Pictures are taken on the morning of surgery with the hair away from the ears. The ears are then scrubbed with alcohol pads for the markings. Adults and older children are marked with a surgical marker in the upright position in the preoperative suite. Young or fidgety children are marked after sedation. Although most patients are candidates for the Mustardé procedure and cartilage reduction, I detail only the Mustardé technique in this part of the chapter and discuss cartilage reduction later. Preoperatively, the helical rim is positioned posteriorly with the finger to create an antihelical fold (AHF). The new fold and the planned suture entry points are then marked with a surgical marker. The new AHF is marked from superior to inferior and the markings include the superior and anterior crus. The delicate curvilinear form of the fold must be duplicated with the marker. A straight line AHF looks very unnatural. The Mustardé suture points are also marked on either side of the AHF ( Fig. 8.24 ). This is a critical marking and often confusing for the novice surgeon. The art of the Mustardé procedure is to realize how many sutures to place and where to place them to obtain a naturally formed, rounded, and curved antihelical fold. The shape and position of the new fold is directly related to the placement and position of the 4-0 Mersilene horizontal mattress sutures. Placing them too close will create a narrow fold. Placing them too far apart will create too wide of a fold and improper spacing can result in a straight AHF.
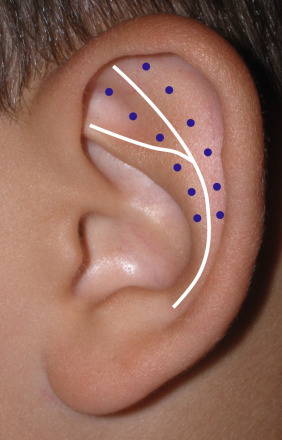
To understand the markings, the surgeon must understand the mechanics of the horizontal mattress sutures. The cadaver example shown in Fig. 8.25 shows how the horizontal mattress sutures fold the flat ear into a roll that becomes the new antihelical fold.

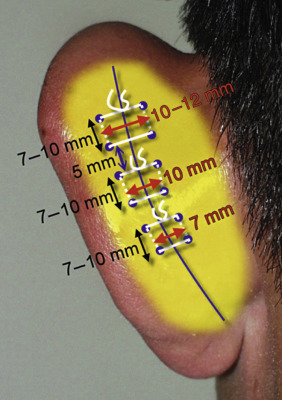
Although experienced surgeons can place Mustardé sutures with little or no markings, a well-planned template can greatly assist the novice surgeon. The top mattress suture is placed superiorly to extend the new fold close to the helical rim. The middle suture assists in creating the main curvature of the fold and the bottom suture assists in creating the secondary inferior portion of the AHF. The horizontal leg of the sutures is generally placed 10–12 mm across at the superior portion of the ear, approximately 10 mm across at the middle of the ear, and approximately 7 mm across at the inferior portion of the ear. Since the natural AHF tapers from top to bottom, the width of the sutures also decreases. The vertical leg of all of the sutures is the same for all sutures, approximately 7–10 mm. Each mattress suture is placed about 5 mm from the previous suture ( Fig. 8.26 ). These measurements are not absolute and vary from patient to patient and the specific deformity but these measurements serve as a basic approach. If a conchal bowl reduction is anticipated, these markings can be made at this time and are covered later in this chapter.
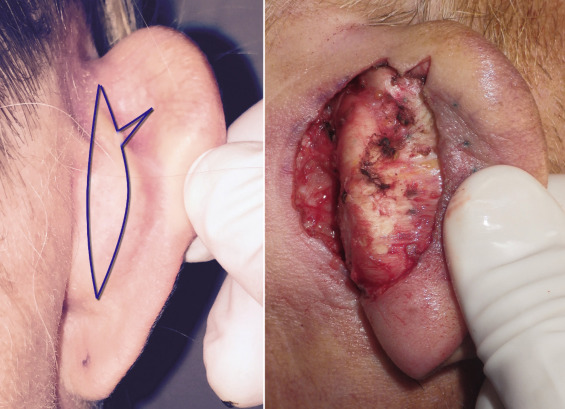
The posterior auricular incision is outlined on the back of the ear. Although numerous incision configurations exist, I prefer a simple vertical ellipse with a releasing incision ( Fig. 8.27 ). The incision is made about 5 mm superior to the sulcus on the conchal bowl. I prefer not to make the incision in the sulcus as access to the helix is more difficult. Wound contracture will nicely hide the incision very close to the sulcus when healed. The vertical boundaries of the incision are basically from the top of the conchal bowl to the bottom. The horizontal width of the incision is commensurate with the amount of planned ear setback. This is important as some surgeons will remove excess skin in false hopes of adding to the retraction of the ear. Ear position and cartilage cannot be maintained by skin removal. Excess tension on this incision is well known for hypertrophic scarring. Skin excision should be conservative on the initial incision and the average width of the center of the ellipse is 7–12 mm. If the surgeon desires additional skin removal, it can be completed just prior to wound closure. If Mustardé sutures are to be placed, the surgeon needs access to the superior pinna just below the helical rim. In order to facilitate this exposure, I prefer to make a 5- to 8-mm releasing incision at the upper third of the incision that is perpendicular to the long axis of the original incision ( Fig. 8.27 ).
Skin Incision and Dissection
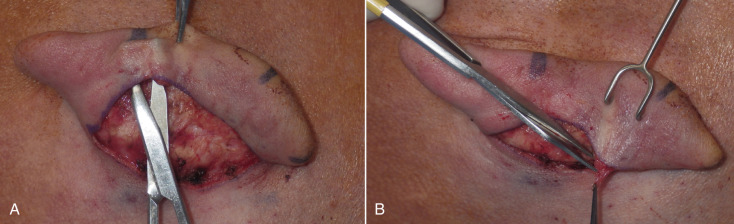
After the patient is prepped, draped, and anesthetized many surgeons perform marking tattoos at this point. Alternatively, these markings can be performed after the skin is dissected, as there is less tissue and fluid to dilute the ink. A scalpel, radiowave, or electrosurgery microneedle or CO 2 laser handpiece is used to incise the skin down to level of the perichondrium ( Fig. 8.28 ). If the surgeon proceeds immediately to the subperichondrial plane, the dissection is much easier, as the more superficial planes are friable and less defined. Once the correct level is determined, my preference is small silver-tipped radiowave bipolar forceps. This provides effortless dissection without harming the cartilage and is hemostatic. The silver alloy tip is resistant to debris fouling ( Fig. 8.29 ).

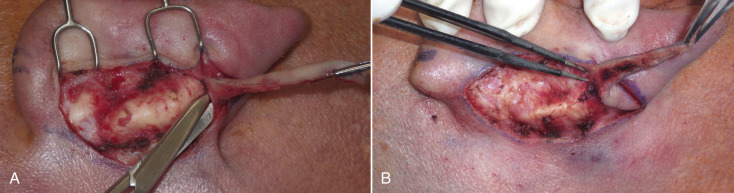
If a conchal bowl reduction (Davis procedure) is to be performed, significant postauricular soft tissue dissection needs to be performed but when doing a pure Mustardé procedure, this is not necessary. After the excision of the skin ellipse to the level of the perichondrium, the remainder of the soft tissue is undermined to expose the posterior pinna. Again, staying in the subperichondrial plane facilitates the dissection. I prefer small blunt scissors such as tenotomy scissors. The dissection is carried to or just short of the helical rim to allow sufficient access. Clipping and spreading the scissors easily dissects this plane ( Fig. 8.30A ). One pearl on this dissection is to remove excess soft tissue that is present under the superior incision margin ( Fig. 8.30B ). If left in place, this soft tissue can become entangled with the Mustardé sutures, entrapped in the knot. Removing the excess soft tissue at this phase makes things easier later. Dissection continues until the entire posterior pinna is exposed in the subperichondrial plane ( Fig. 8.31 ).