Congenital Ptosis
Adam R. Sweeney
Christopher B. Chambers
DEFINITION
Blepharoptosis, commonly referred to as ptosis, is eyelid positioning inferior to normal posture. Often, ptosis is defined as asymmetry of 1 mm or more between the two upper eyelids or a marginal reflex distance of less than 2.5 mm.1
Congenital ptosis refers to cases presenting within the first year of life, as an isolated finding or as a manifestation of ophthalmic or systemic disorders.
Typically, congenital ptosis results from fibrofatty degeneration of the levator complex.
Congenital ptosis affects an estimated 1 in 842 births in the United States.1
ANATOMY
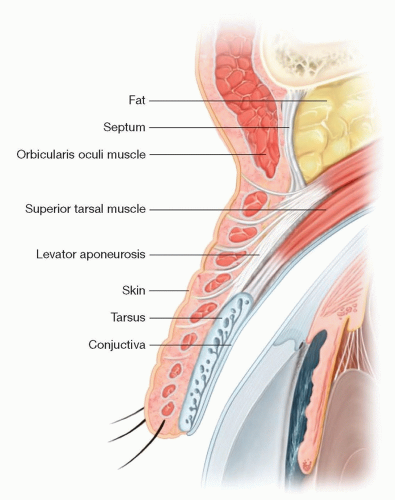
The anterior lamella is made up of the skin and the preseptal orbicularis (FIG 1).
The posterior lamella is made up of the tarsus and the palpebral conjunctiva.
The tarsus is a fibrous plate located in the eyelid. It is 9 to 10 mm in height in the upper eyelid and 4 mm in height in the lower lid. The length of the tarsus is approximately 22 to 25 mm.
Posterior to the orbital septum lies the preaponeurotic fat pad, an important surgical landmark.
The levator aponeurosis is the primary retractor of the upper eyelid and is located just posterior to the preaponeurotic fat.
The levator palpebrae originates above the annulus of Zinn and attaches to Whitnall ligament, a transverse facial suspensory structure. This attachment allows the levator muscle’s horizontal vector to be redirected to the vertical vector created from its anterior extension, the levator aponeurosis, which terminates at the anterior tarsus.
Muller muscle arises from the posterior layer of the levator muscle and inserts into the upper border of the tarsal plate.
The lid crease is formed from levator aponeurosis fibers inserting into the fascicular bundles of the pretarsal orbicularis.
In patients not of Asian descent, the lid crease is located between the upper border of the tarsus and the insertion of the orbital septum, which is approximately 3 to 5 mm superior to the upper border of the tarsus. The lid crease is approximately 9 to 11 mm and 8 to 9 mm superior to the eyelid margin in females and males, respectively.
In Asians, the lid crease is much lower secondary to a more anterior preaponeurotic fat pad and low/absent attachment of the aponeurosis fibers to the fascicular bundles of the pretarsal orbicularis.
The levator muscle is a striated muscle and is innervated by cranial nerve (CN) III, whereas Muller muscle is a smooth muscle innervated by the sympathetic chain.
The frontalis muscle inserts into the orbicularis oculi at the inferior brow.
PATHOGENESIS
There are multiple different etiologies of congenital ptosis.
Approximately 80% of congenital ptosis arises from dysgenesis or fibrosis of the levator muscle with remaining integrity of the levator aponeurosis, termed myogenic ptosis or simple congenital ptosis.1,2
Myogenic ptosis is more common unilaterally than bilaterally.
Neurogenic etiologies are much less common and arise from innervation abnormalities during development such as abnormal motor nerve connections of the levator muscle
and branches of the trigeminal nerve innervating the external pterygoid muscle (Marcus Gunn jaw winking), interrupted sympathetic nervous chain (Horner syndrome), congenital cranial nerve III palsy, or congenital cranial dysinnervation disorders such as Duane retraction syndrome.
Aponeurotic ptosis is caused by a defect in the tendon’s ability to redirect the action supplied by the levator muscle. This is classically different from disinsertion of the aponeurosis from the levator muscle, as is commonly seen in advancing age or from trauma including childbirth.
Mechanical ptosis is caused by a forced inferior excursion of the eyelid such as seen in tumor, eyelid inflammation/edema, cicatricial processes, or foreign body.
Traumatic ptosis usually can be found to be inclusive in one of the above categories and may arise in utero or from trauma, such as during childbirth.
NATURAL HISTORY
Congenital ptosis may be mild and benign with no impact on vision or function of the child.
Severe congenital ptosis may cause amblyopia due to deprivation or astigmatism.
Twenty-five percent of patients with congenital ptosis develop amblyopia of the involved eye.2
PATIENT HISTORY AND PHYSICAL FINDINGS
Hallmark findings distinguishing congenital myogenic ptosis from acquired ptosis: absence or irregular upper eyelid crease, decreased levator function (particularly prominent in upward gaze), eyelid retraction in downward gaze, and presence of lagophthalmos (a common finding in congenital ptosis).
Marcus Gunn jaw-winking ptosis involves elevations of the eyelid with pterygoid muscle movement usually evident with sucking or chewing. Monitoring for association of lid height in various gazes and facial movements including jaw movement is important to rule out this condition.
Horner syndrome classically manifests with ptosis, meiosis, and anhidrosis ipsilateral to the neurological defect. Ipsilateral lower lid inverse ptosis may also be seen. Heterochromia characterizes the congenital form from acquired Horner syndrome and necessitates systemic workup.
Margin reflex distance (MRD) of the upper lid and vertical palpebral fissure height should be routinely assessed, when possible.
MRD1 in down gaze, evaluating chin, head, and brow position should be noted as compensatory mechanisms.
Strength of Bell phenomenon (eye elevation and abduction on attempted lid closure) may indicate whether dysgenesis of the levator muscle includes the superior rectus muscle.
Perform a pupil exam monitoring for symmetry.
Test extraocular muscle movements assessing for partial CN III palsy or assessing for hypotropia-related pseudoptosis.
Test the frontalis contribution by immobilizing the brow in primary position as children often will attempt to correct ptosis by recruiting the frontalis muscle.
Assess corneal exposure issues with fluorescein staining.
The phenylephrine test is performed by instilling one eye drop of 2.5% phenylephrine to the inferior cul-de-sac. This elevates the eyelids within 10 minutes via the sympathetic response on smooth muscles of the eyelid, principally Muller muscle. The MRD1 should be assessed before and 10 minutes after instillation. Demonstration of adequate improvement of the ptosis after phenylephrine test may guide the surgical technique required, such as a Muller muscle resection. Unilateral phenylephrine dosing may reveal a contralateral ptosis masked by Hering law of equal bilateral innervation.
Attaining visual acuity and fixation preferences may help detect amblyopia. Evaluation of these patients with a pediatric ophthalmologist is important.
IMAGING
Quality full facial photographs should be obtained for preoperative planning and intraoperative reference.
In older children or adults with congenital ptosis, visual field testing with taped and untaped eyelids should be performed.
An A-scan may be performed if one is concerned about pseudoptosis, a term describing ptosislike appearance from pathology independent of the eyelid, such as microphthalmia or advanced hyperopia.
Cycloplegic refraction or autorefraction may be performed to detect ptosis-induced astigmatism that may be amblyogenic.
Congenital Horner syndrome should be evaluated with a tumor workup that may necessitate MRI investigation.
DIFFERENTIAL DIAGNOSIS
Myogenic: myasthenia gravis, chronic progressive external ophthalmoplegia, muscular dystrophy, and oculopharyngeal dystrophy
Myogenic etiology also seen in blepharophimosis-ptosisepicanthus inversus syndrome (BPES), which also may have euryblepharon, telecanthus, ear deformities, and hypoplasia of the superior orbital rims and nasal bridge
Neurogenic: Marcus Gunn jaw-winking ptosis, Horner syndrome, aberrant regeneration of the oculomotor nerve, Duane retraction syndrome
Aponeurotic ptosis refers to slowly progressive ptosis from involutional changes in the levator aponeurosis with gradual stretching or dehiscence of this structure.
Mechanical ptosis from excessive upper eyelid weight such as secondary to an eyelid mass, foreign body, or eyelid edema
Pseudoptosis: Microphthalmia (underdevelopment of the orbit, lids, and socket) or advanced hyperopia with smaller anteroposterior globe length
NONOPERATIVE MANAGEMENT
If ptosis is not cosmetically bothersome and does not appear to affect visual axis or lead to astigmatism, observation may be appropriate.
SURGICAL MANAGEMENT
When potentially amblyogenic, prompt ptosis surgery is indicated.
The timing of surgical correction in the absence of visually threatening ptosis is debated with many advocating for correction at approximately age 4 when structures are more defined and the child is more cooperative5; however, others suggest earlier treatment advocating ease of development and postoperative care.
Consideration of the type of surgery should reflect the degree of ptosis, levator function, and emphasis on cosmetic outcomes.
Surgeon preference often is considered when choosing a technique; however, surgeons should be comfortable with the major techniques including frontalis suspension, levator resection, and Muller muscle surgery.
When levator function is less than 3 to 4 mm, frontalis suspension is typically preferred when possible.2,5
External levator resection or advancement may be employed for patients with moderate levator function and mild to moderate ptosis.2,5
A poor Bell phenomenon may require a temporary lower lid retraction suture, or Frost suture, to protect the cornea following ptosis surgery.
Frontalis suspension may utilize a silicone, Mersilene mesh, Gore-Tex, Ptose-Up strips, or Supramid material. However, if the child is older than 3 or 4 years, autogenous fascia lata may be utilized, which some report yields better results.6
Preoperative Planning
General anesthesia is recommended for pediatric cases.
Review of the facial photos and exam including attention to the MRD1, vertical fissure height, Bell phenomenon, and extraocular muscle
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree