Introduction
Chemical peels are a method of skin resurfacing to address a variety of patient concerns from dyschromias to acne scars and wrinkles. Many physicians may have switched from chemical peels to the ease of dialing in settings on their lasers to resurface skin. However, it is the author’s belief that with the proper understanding of peel-tissue interaction, one can selectively resurface various parts of the skin, thus allowing for control and artistry in the resurfacing process. Depending on the depth of resurfacing, peels can be classified into four levels: very superficial peels only penetrate through the stratum corneum and the uppermost portions of the epidermis; superficial chemical peels penetrate the epidermis but not more than the basal layer of the epidermis; medium-depth peels penetrate the entire epidermis plus the papillary dermis; and deep chemical peels create a wound to the level of the upper and mid-reticular dermis.
Each level of peel will have a different end result on the skin with less improvement seen with the more superficial peels and more dramatic change with medium-depth peels. Healing time and complications vary among the different categories of peels as well, with some peels being more appropriate for certain skin types. Therefore, to maximize the benefits of a peel for a patient and to minimize adverse effects, it is important to choose which, if any, peel is appropriate for each patient.
Chemical peels remain very important and highly versatile tools for skin resurfacing and rejuvenation. Although newer fractionated ablative and non-ablative laser technology has added to the arsenal of tools for skin resurfacing, these lasers are either cost-prohibitive for certain patients, not advisable for certain skin types, and, most importantly, not as flexible for cosmetic physicians who like to tailor their skin resurfacing approach for each patient.
Skin resurfacing, whether by peels or lasers, still requires a through patient evaluation, knowledge of skin anatomy, proper skin preparation, and, as with any surgical procedure, the ability to identify and quickly treat complications. The key to successful skin resurfacing lies in choosing the proper depth to resurface the skin, that is, not too superficially (too little improvement) and not too deeply (risk for scarring and permanent color change).
When performed correctly, chemical peels can play an important role in cosmetic surgery and can be tailored to address most skin issues. Further adding to their versatility, advanced chemical peel techniques can be used in combination with laser resurfacing, nonablative lasers, and surgical procedures to enhance the overall outcome for patients.
Indications for Chemical Peels
As the largest organ in the body, the skin plays an important role as a barrier to environmental insults such as ultraviolet (UV) radiation, temperature extremes, and environmental pollution. Furthermore, systemic conditions such as hormonal changes, inflammatory skin diseases, and systemic diseases can affect the skin. A knowledge of skin anatomy and at which level in the skin a particular skin condition (wrinkles, lentigines, melasma, scars, actinic keratosis) exists is crucial to performing a safe and effective resurfacing procedure ( Table 14.1 ). The balance lies in peeling the skin deeply enough to address the patient’s concerns without either peeling too superficially (missing the clinical concern) or peeling too deeply (increasing the risk for complications and prolonging the recovery time).
| Anatomic Skin Level | Clinical Presentation | Treatment Options |
|---|---|---|
| Epidermis |
|
|
| Dermis |
| |
| Epidermis and Dermis | Mixed-type melasma | Medium-Depth Resurfacing |
a Best treated with electrodessication (using an epilating needle for dermal lesions).
b Best treated with chromophore specific lasers.
Aging Skin (Intrinsic and Extrinsic)
Aging is a multifactorial process that occurs as external forces (extrinsic aging) act on the skin while internal, chronologic aging (intrinsic aging) progresses. Starting at around of 18 years of age, there is a natural decline in fibroblast function resulting in decreased collagen and elastin production. This is referred to as intrinsic aging . This reduction is on the order of approximately 1% per year starting at 18 years of age. Extrinsic aging is caused by external factors such as UV radiation, high-energy visible light, and infrared light, all of which act on the skin to accelerate the aging process by causing some degree of inflammation and oxidation within the cells. Many complex changes are occurring in the skin that reflect both intrinsic and extrinsic aging. This topic is covered in more depth in Chapter 12 .
Patient Evaluation
Patients seek cosmetic surgery for many reasons ranging from the obvious concerns to very subtle issues that bother them. Thus, as with any cosmetic surgery procedure, it is of paramount importance to evaluate and select the patient correctly. Clearly delineating what the procedure will and will not achieve helps keep the patient’s expectations in check. Nothing is better than having high quality before and after photographs of patients with a wide range of skin types to show new patients during the consultation.
As with any cosmetic surgery procedure, the most challenging patients and the ones who require the greatest degree of caution are those who present with barely noticeable skin defects. These patients are most likely to closely scrutinize results, and they tend to be disappointed in what they may perceive as not significant enough improvement.
Every patient requires a thorough medical, social, and family history to identify possible contraindications to resurfacing ( Table 14.2 ). Certain medications may affect wound healing, such as prednisone or immunosuppressants. Other medications may indicate that the patient has an underlying psychiatric disorder. Heavy smokers or patients treated with radiation to the face may have problems with wound healing as resurfaced skin requires intact and functioning pilosebaceous units and a good blood supply to reepithelialize correctly. Lastly, it is important to inquire about the tendency to develop postinflammatory hyperpigmentation, hypertrophic or keloid scars, or poor wound healing.
| Pertinent history | Relative contraindications | Absolute contraindications | |
|---|---|---|---|
| Medical |
|
|
|
| Social |
| Smoking/vaping/nicotine use |
|
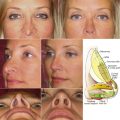
All patients should be examined in a well-lit room with no makeup on. Acne scars can be harder to fully appreciate in direct lighting. Therefore acne scar patients should be examined with indirect overhead light to cast shadows onto the skin to better delineate scar morphology and to highlight the areas involved. Skin conditions that can Koebnerize to areas that are resurfaced should be identified as well (i.e., vitiligo, psoriasis, lichen planus, verrucae vulgaris and plana) ( Fig. 14.1 ).
Patients seeking treatment for melasma should be questioned about the use of hormone intrauterine devices (IUDs), hormone replacement therapy, hormone cervical rings, or oral contraceptives. The use of hormone-containing medications will continue to stimulate the melasma and may lead to treatment failure or worsening of the condition.
Contraindications to Skin Resurfacing
Contraindications to skin resurfacing can be extrapolated to resurfacing with peels and lasers. However, what gives chemical peels an advantage over laser resurfacing procedures is that with the proper skin conditioning as well as the proper procedure depth, patients of most skin types can be treated. Furthermore, areas that are usually not amenable to laser resurfacing (neck, lips, eyebrows, ears) can be safely peeled with the proper chemical peel allowing for safe combination resurfacing in one sitting to give overall rejuvenation with little to no lines of demarcation.
Just from the injury to the skin with a peel, darker-complexion patients are at risk for temporary postinflammatory hyperpigmentation (PIH). With peels that reach the reticular dermis, these patients are at risk for permanent hypopigmentation. To minimize this risk for PIH, the length of preoperative skin conditioning should be extended to 3 months and resumed immediately upon reepithelialization of the skin. Because PIH is usually transient, it is not a contraindication to resurfacing; rather, it should be anticipated and addressed before resurfacing.
When performing resurfacing that is deeper than an epidermal-level procedure, the general health and nutritional status of the patient becomes an important consideration. Deeper laser resurfacing and medium-depth and deep peels require a healthy nutritional status and well-functioning immune system for uneventful wound healing. Patients who have undergone bariatric surgery oftentimes are deficient in vital nutrients, iron, and protein. Blood laboratory tests can help identify issues. Immunocompromised patients such as transplant recipients or those on medications for autoimmune diseases are immunologically impaired, putting them at risk for infection. These patients may require coverage with an oral antibiotic during the healing period (penicillin, cephalosporin, or trimethoprim/sulfamethoxazole).
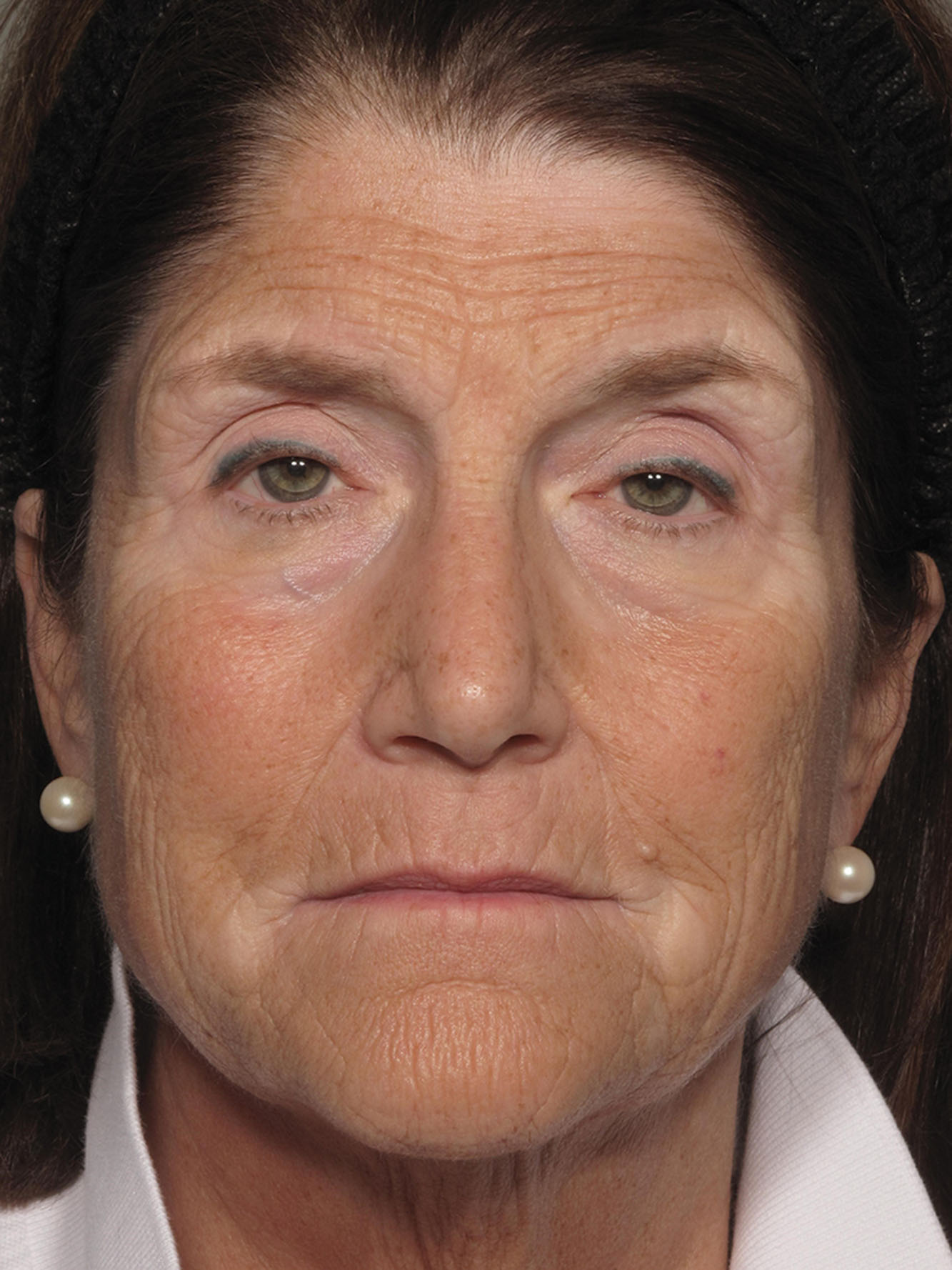
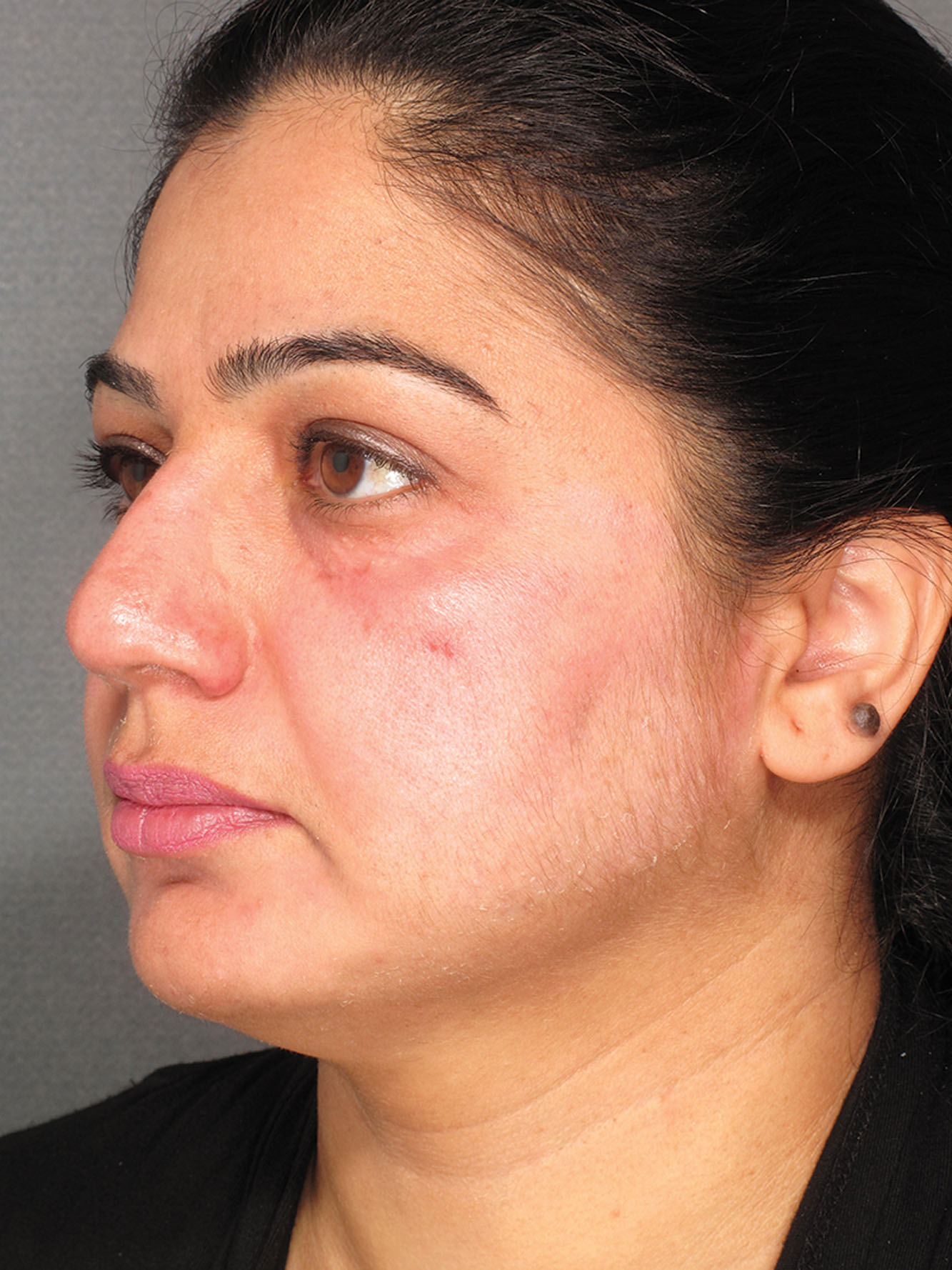
Patients should be asked questions to ascertain issues with wound healing, hypertrophic or keloid scars, or a tendency to develop PIH. Inflammatory skin conditions can also flare post-resurfacing, thus it is important to inquire about the presence of seborrheic dermatitis, atopic dermatitis, and rosacea. Probably, the most challenging patients to treat are those with melasma ( Fig. 14.2 ). This is because the condition can flare and worsen post-resurfacing if the patient is taking exogenous hormones or is exposed to heat or sunlight too soon.

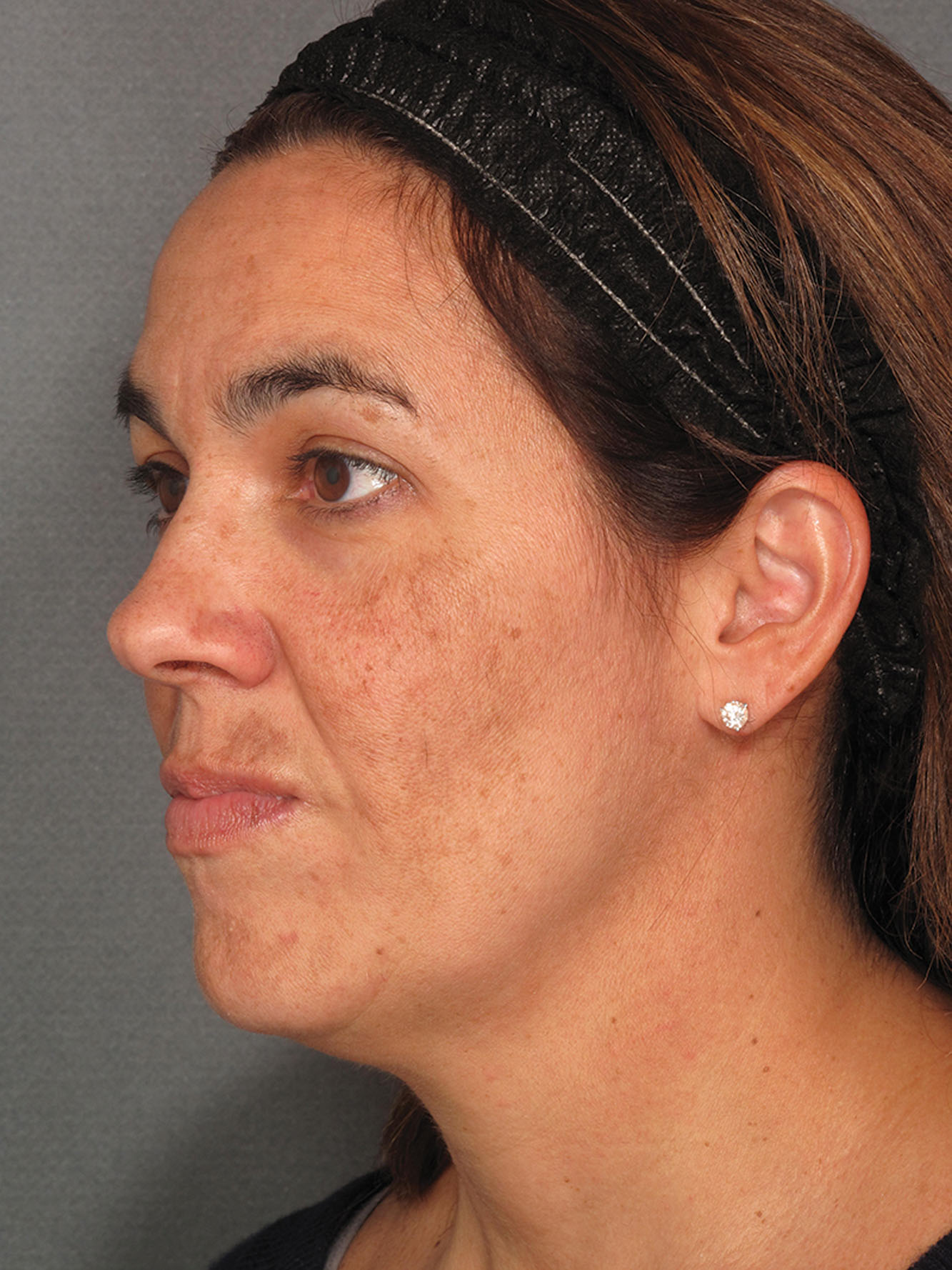




A history of recent systemic retinoid use was once considered an absolute contraindication for skin resurfacing because of concerns of increased hypertrophic scar formation in these patients. More recent studies and case series have shown that this concern may not be valid. Patients having laser hair removal, laser skin resurfacing, or medium-depth peels in these studies did not demonstrate increased adverse outcomes. Although these studies may be small, they do show the complexities associated with keloid formation, and they challenge the conventional thinking that isotretinoin impairs wound healing. For medium-depth peels or dermal-level laser resurfacing procedures, it may be prudent to stop isotretinoin 3–4 months before the peel. If a patient has an inflammatory condition such as acne or rosacea, oral antiinflammatory antibiotics (doxycycline) can be used temporarily to calm the condition down.
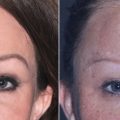
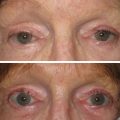
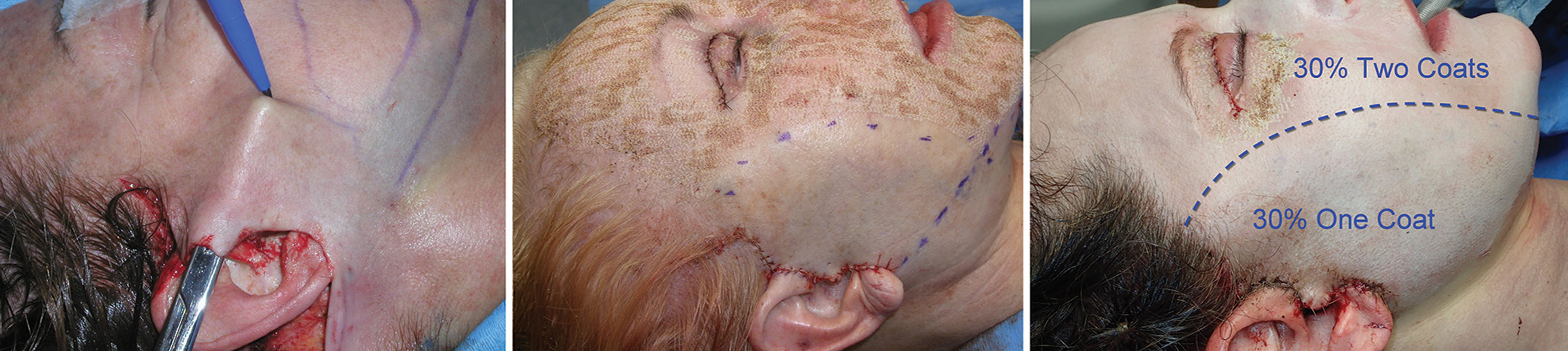
A similar question arises with regard to the safety of simultaneous skin resurfacing and cosmetic surgery. The goal is to optimize results for patients by combining skin resurfacing the same day as their surgical procedure. In the past, it was thought that combining these procedures increased the chance of impaired wound healing. Newer studies have shown safe outcomes when combining fractionated laser resurfacing with short-flap rhytidectomy, full-face laser skin ablation combined with rhytidectomy, and fractionated CO 2 laser, brow lifting, and surgical blepharoplasty ( Fig. 14.3 ). Care should be taken to minimize the depth of resurfacing over flaps (not deeper than the basal layer or papillary dermis) and kept away from incisions, whereas the peel or laser resurfacing can be performed more deeply over the central face (non-undermined skin). The safe window for resurfacing is either the same day as surgery or 6–12 months after a facelift or browlift procedure. The extensive undermining during facelifts/browlifts compromises the skin’s lymphatic drainage, so it is best to wait 6–12 months to reduce the risk for prolonged postoperative edema if the peel is not performed on the same day as the surgery.
Although most patients can safely undergo skin resurfacing, there are certain contraindications. The absolute contraindications include active infection at the treatment site, pregnancy, significant tendency to develop keloids, and the inability to adhere to postoperative instructions.
Evaluating Skin Type
When resurfacing skin, the patient must be evaluated correctly to help choose the correct procedure and depth of treatment and to help reduce postoperative complications. This evaluation must be performed in a standardized fashion. Skin color alone is not sufficient in guiding procedure depth. If one looks more closely, there are some important variations that exist, even among patients of the same skin color. Particular attention should be paid to patients who have freckles, develop melasma, or are prone to PIH. Regardless of ethnic background, the presence of these issues heralds the risk for postprocedure hyperpigmentation.
Fitzpatrick phototype is simply a way to type the skin based on the ability to tan in response to UV exposure. In this classification, patients are categorized from I to VI as their skin color darkens and their ability to tan rather than burn increases. This classification was intended to help physicians treat patients with phototherapy and is limited in that it does not address the degree of photodamage present or assist in selecting the correct procedure depth. Glogau’s classification attempts to objectively quantify the amount of photodamage present, but it does not help determine the best resurfacing modality or depth or resurfacing needed.
In particular, both of these scales were devised before the emergence of nonablative and fractionally ablative technologies and fall short in addressing patients with thicker skin or darker skin types. The author utilizes the Obagi skin classification ( Table 14.3 ) to help with proper procedure planning.
| Skin variable | Skin conditioning: pre- and post-resurfacing | Suitable procedures and potential complications |
|---|---|---|
| Color |
|
|
| Oiliness |
|
|
| Thickness |
|
|
| Laxity | Lax skin requires long-term collagen stimulation to prevent further laxity. |
|
| Fragility | Goal is to maintain or possibly increase skin strength. |
|
a If systemic isotretinoin is used, it is prudent to delay medium or deep skin resurfacing at least 3 months (medium-depth resurfacing) to 6 months (deeper resurfacing).
The Obagi skin classification incorporates five variables that are important to address before any resurfacing procedures: skin color, oiliness, thickness, laxity, and fragility. This system helps identify patients who require a longer preoperative and postoperative skin conditioning program, those who are more likely to hyperpigment or hypopigment, those who are prone to delayed healing, and those who require a skin tightening procedure (peels, lasers) over a planing procedure (dermabrasion). The evaluation of all five factors helps maximize skin resurfacing results while minimizing complications.
Although the concern of permanent hypopigmentation exists, there are some patients at risk for pseudohyperpigmentation . These patients tend to have extensive photodamage, and they should be approached with caution. Pseudohypopigmentation refers to an area that once had extensive sun damage and is now resurfaced back to the patient’s baseline skin color and condition. Once the treated area heals, the absence of photodamage may stand out in stark contrast to nearby, untreated, photodamaged skin. This gives the appearance of hypopigmentation of the treated skin. However, when one compares the treated skin to other sun-protected areas, the color of the newly treated skin is not lighter than the patient’s baseline ( Fig. 14.4 ). To minimize this contrast and minimize lines of demarcation, one should consider using topical agents or lighter peels to blend in the skin adjacent to the treated area.





Skin Conditioning
The proper pre-resurfacing preparation of the skin is a major contributor to the overall outcome of the resurfacing procedure. Although patients like to see results quickly and may balk at the idea of using a comprehensive skincare regimen before having a procedure, the results they will see in their complexion in as little as 2–3 weeks serves to excite them while they await their procedure. In fact, for patients who are unsure about undergoing skin resurfacing, improving their skin with a proper skincare regimen can really motivate them or excite them to move forward with the skin resurfacing procedure.
Another goal of a comprehensive skincare protocol is to improve wound healing. Patients treated with topical retinoids tend to have a shorter healing time after skin resurfacing. Lastly, instituting an aggressive preconditioning program can help identify noncompliant patients. If patients quit their regimen once they develop the initial erythema and desquamation of a retinoid dermatitis, they may not follow postoperative instructions and may pick or peel their skin prematurely during the healing process. Therefore the goal of skin preconditioning is to restore the skin as much as possible to a normal state before wounding it. This is achieved by increasing dermal collagen production, regulating the melanocytes, normalizing keratinocyte atypia, and decreasing surface roughness (to allow more even acid penetration).
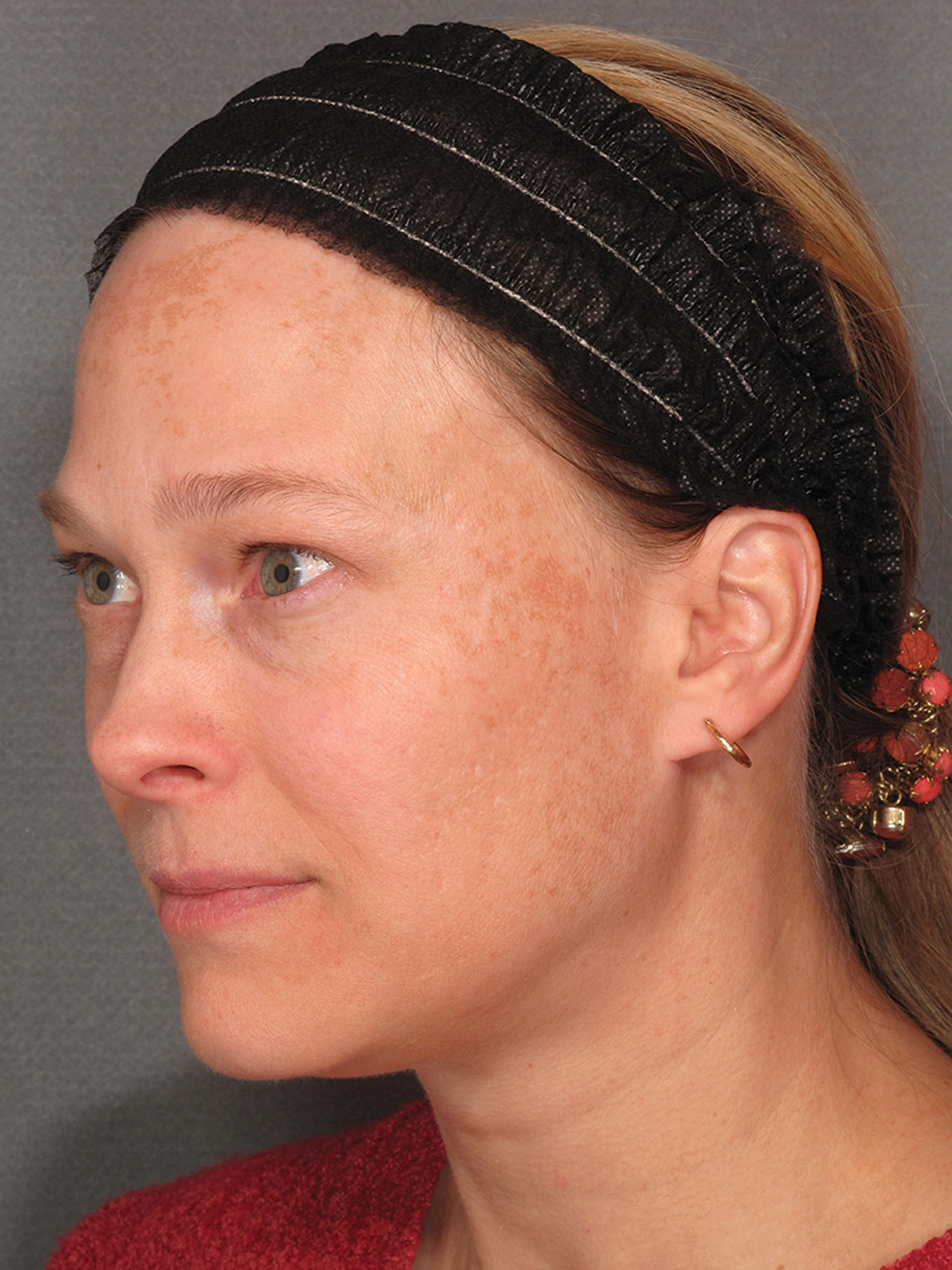
Proper skin conditioning should be started at least 6 weeks (8–12 weeks or longer for darker-skinned individuals) before resurfacing. See Chapter 12 to further understand how to put together a skincare regimen in anticipation of skin resurfacing. In addition to helping reduce the risk for hyperpigmentation post-resurfacing, the pre-resurfacing use of skincare products helps improve skin texture, thus motivating patients to proceed with further procedures to enhance their skin ( Fig. 14.5 ). Lastly, the ability of a patient to adhere to a skincare regimen helps predict which patients are most likely to be compliant with postoperative instructions.



Post-resurfacing skincare is restarted immediately once the wound is reepithelialized and the patient is able to tolerate the application of topical medications. Because reepithelialization time varies with wound depth, it may be as early as 3 days (with exfoliative procedures) to as late as 14 days. PIH may not be clinically evident until 3–4 weeks after the procedure, but it starts to form once the wound has healed. Because there may be a delay until it shows up, it is easier to try to prevent it by treating the skin prophylactically rather than to deal with this frustrating issue once it has occurred.
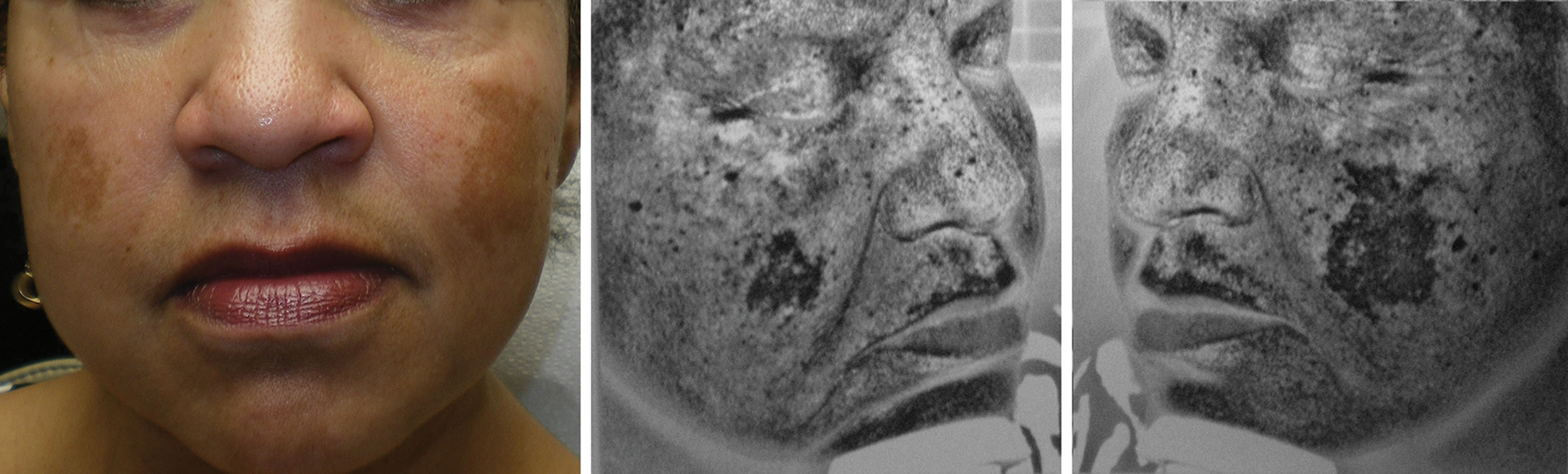
For novice physicians, the use of skin scanners, UV cameras, or simple UV lights (black lights/Wood’s lamp) can be of great assistance in better visualizing pigmentation issues in the skin. Epidermal melanin enhances with UV light, and any areas of loss of pigment become more apparent ( Fig. 14.6 ). Similarly, pigmentation that does not enhance with UV light may be dermal and very resistant to treatment. Performing a UV skin evaluation is helpful in educating the patient on their degree of sun damage and the expected effect of resurfacing, and it also serves to show improvement after treatment.
Herpes Prophylaxis
Previous exposure to herpes simplex virus (HSV) or varicella zoster virus (VZV) can allow the virus to lie dormant in the nerves and to reactivate during times of stress or skin injury (skin resurfacing). Because these viruses can cause severe scarring and can spread over the treated area very quickly, it is imperative that the chance of eruption be reduced or suppressed completely. The dosing of antiviral therapy is aimed at the prevention of outbreaks. It is the author’s preference to treat all patients with valacyclovir (Valtrex, Glaxo Smith Kline, Research Triangle Park, NC) 500 mg by mouth twice a day for 7 (medium-depth peels) to 14 (deeper peels or laser resurfacing) days until the skin has fully healed. This regimen is started 1 day before the procedure for all patients. However, if a patient has a history of frequent HSV outbreaks, the author increases the dose of valacyclovir to 1 g twice a day starting 1 week before the procedure and for 7 to 14 days afterward.
Antibiotics and anti-candida agents are best used only if an infection develops rather than empirically. The author routinely prescribes mupirocin ointment to be applied to the nares twice a day starting 1 week before skin resurfacing and for 1 week after skin resurfacing. This has greatly reduced the incidence of staphylococcal infections.
Chemical Peel Skin Resurfacing
Mechanisms of Action
There are many factors that affect the depth of penetration of a peel. Simply utilizing peel acid concentration or the type of acid as the sole determinant of depth can lead to complications. The most important points to consider in determining peel depth are acid concentration, volume of acid applied, skin thickness, percentage of body surface area treated, skin preconditioning, and in some cases (i.e., glycolic acid), the duration of contact of acid on the skin.
For medium-depth peeling, it is important to understand the main mechanism of action of the acid on the skin, especially when performing combination peels ( Table 14.4 ). This is either a keratolytic effect or a protein denaturant effect. The keratolytics are mainly used for superficial, exfoliative procedures, whereas the protein denaturants can be used both for superficial or deeper peels, as we will discuss in the following sections.
| Acid properties | Commonly used concentrations and formulations |
|---|---|
| Keratolytics |
|
| Protein denaturants |
|
a Phenol at concentrations below 50% has keratolytic properties.
Keratolytics
Keratolytic acids work by disrupting the bonds between the keratinocytes, thereby causing shedding of these layers. Glycolic acid and salicylic acid are the two most commonly used acids for light peels; however, there are many other peels and combination peels that incorporate lactic acid, mandelic acid, citric acid, resorcinol, retinoic acid, and Jessner’s solution. Jessner’s solution is a popular peeling solution composed of 14% each of resorcinol, salicylic acid, and lactic acid mixed in ethanol.
Salicylic acid and Jessner’s solution (contains salicylic acid) have an advantage over glycolic acid in that salicylic acid is lipophilic. Lipophilic agents penetrate acne lesions or oily skin better than hydrophilic agents such as glycolic acid. Another advantage is that salicylic acid and Jessner’s solution do not require close timing of skin contact time, as required with glycolic acid peels.
The main role of keratolytic peels is to address superficial conditions such as acne, mild sun damage, and mild dyschromias. These are oftentimes referred to as lunch-time peels as these light peels have the benefit of little to no down time. Nurses and aestheticians are usually delegated to perform these light peels as there is no anesthesia requirement, and they are relatively straightforward to perform. Patients must be aware that multiple sessions are required to see clinical improvement. A comprehensive skincare regimen can really help speed up the results and increase the results of these light peels.
Protein Denaturants
For medium-depth and deep peels, phenol and trichloroacetic acid (TCA) are the main protein denaturant peeling agents used. TCA has a long, proven safety record, while newer formulations of phenol peel mixtures have increased the versatility and safety of this once aggressive peeling agent. TCA and phenol work by causing protein coagulation and denaturation of the cells of the epidermis, dermis, and blood vessels as they penetrate into the skin. Once a certain volume of the acid is applied to the skin, it will keep coagulating proteins until it is used up. This means that TCA and phenol solutions cannot be neutralized once they begin to be absorbed into the skin. There may be time to wipe excess TCA off the surface of the skin if too much is applied, but phenol rapidly penetrates the skin. After about 2 minutes, the depth of TCA penetration can be observed, and a decision can be made if more acid is needed to drive the peel deeper. Phenol is a lot more rapid in its penetration, and the depth is apparent almost immediately. Subsequent application of acid will continue to drive the peel deeper until it is used up by coagulating proteins deeper in the skin. When used correctly, these acids can be used to achieve a variety of peel depths ranging from exfoliation to deep peels.
It is of utmost importance to purchase the peel solutions from a reputable source to reduce the risk for errors and complications. TCA solutions, for example, can be formulated by four different methods. The safest and most agreed-on method is the weight to volume (W:V) calculation. The author personally only purchases TCA from Delasco (Council Bluffs, IA). To further minimize errors, the author only keeps on hand 1 strength of TCA, 30% TCA solution, which is then modified as part of the Blue peel to create a 15%, 20%, 22.5%, or 24% solution. Similarly, there are many variations on phenol/croton oil peel formulas, requiring a reliable pharmacy to formulate these solutions. All chemical peel solution bottles are clearly labeled. To further increase safety, TCA and phenol solutions are kept in a separate cabinet from the light peel solutions that the aesthetician staff uses.
Trichloroacetic Acid Peels
As mentioned earlier, it is not correct to refer to TCA peels as light, medium , or deep solely based on TCA concentration. Acid concentration is only one variable affecting peel depth. For example, 1 mL of 40% TCA applied to the face will result in less skin penetration than 6 mL of 40% TCA applied over the same body surface area.
Another misconception is that lasers are easier to use once the settings are learned. With proper training and experience, one can perform peels to a number of skin depths with the same aptitude that one uses to dial in laser settings for skin resurfacing. Additionally, TCA peels can be used to blend into the hairline, brows, ears, and onto the neck, whereas lasers may be contraindicated in these areas.
TCA 10%–50% can be used as a sole peeling agent, but using higher concentrations comes with increased risk. The TCA molecule is hydrophilic, thereby allowing for patchy penetration of the peel solution through the lipid-containing, thick stratum corneum. Applying more TCA solution will penetrate further into certain areas (with thinner stratum corneum or denuded skin) than others, risking an uneven peel. Therefore it is a fine balance between reapplying TCA at high concentrations in areas that need it without risking too deep of a peel.
A way around this issue is to prepare the skin topically in a manner that facilitates even TCA penetration by making the stratum corneum more even and compact. Because oil hinders TCA penetration, oily skin must have adequate oil control before performing the peel. This can be achieved with a short course of isotretinoin for a few months ending about 3–6 months before the peel. To address any residual oil or lotions on the skin on the day of the peel, the skin must be properly degreased with 70% alcohol and, in some instances, acetone.
Combination peels or modified TCA peels have been developed to allow for more even penetration of TCA at 30%–35% without having to resort to higher concentrations. These peels are designed to reach the papillary dermis level in a more consistent manner.
The three most commonly used modified TCA peels are the Jessner’s solution–TCA peel, glycolic acid–TCA peel, and the Blue peel ( Table 14.5 ). These peels are designed to peel to a depth of the papillary dermis and at most, to the most superficial aspect of the reticular dermis. The main indications for TCA and modified TCA peels are for epidermal and upper dermal pathology: photodamage, actinic keratoses, lentigines, ephelides, fine rhytids, and very superficial, nonfibrotic (stretchable) scars. These peels are not suited for fibrotic scars, deep nonstretchable rhytids, or extensive laxity. If a rhytid or scar improves with stretching the skin, a medium-depth peel can help improve it. However, if the scar or rhytid is etched into the skin or is fibrotic, the tightening effect of the peel may not be enough to give adequate clinical improvement.
| Modified TCA peels | Solutions | Technique |
|---|---|---|
| Glycolic acid–TCA peel |
|
|
| Jessner’s solution–TCA peel |
|
|
| TCA-Blue peel |
|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree