Chapter 11 The Microbotox Technique
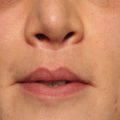
Was this the face that launched a thousand ships, and burnt the topless towers of Ilium? Oh sweet Helen, make me immortal with a kiss!
C M
I developed the Microbotox technique in 2001. In this procedure, tiny droplets of botulinum toxin (Botox [Allergan]) are injected superficially into the skin of the forehead and superficial muscle fibers of the frontalis muscle to improve the appearance of horizontal rhytids without compromising the lifting action of the deeper fibers of the frontalis while simultaneously improving the texture and quality of the forehead skin.1–4
Since its inception, the Microbotox technique has evolved into a versatile chemoresurfacing technique that alters the sheen and texture of skin by decreasing sweat, oil, and sebum production; improving acne and rosacea; reducing the appearance of open pores; decreasing fine lines without altering deep muscle movement; lifting and sculpting the jawline; smoothing the neck and under-eye areas; and generally giving a natural appearance to the face without an “over-Botoxed” look.1 It is also regularly used to treat hypertrophic and keloid scars when used in conjunction with intralesional triamcinolone. It can also improve the appearance of acute breast and abdominal striae as well as thigh and buttock cellulite.
The key to the technique is the delivery of multiple, evenly distributed microdroplets of Botox into the dermal and subdermal layer of the skin that then diffuse into the superficial layer of the facial muscles immediately below, leaving the function of the deeper layers of muscles intact. This decreases fine lines and wrinkles in difficult-to-treat areas such as the lateral forehead, the undereye area, and the neck and jawline. In the skin, the effect of the Botox is to decrease the production of sweat (which is well documented) and sebaceous secretions and bring about atrophy of the sweat and sebaceous glands, which in turn causes a thinning and tightening of the skin envelope.5–7 Pores appear reduced in size as a result, and the skin becomes smooth and unlined. Acne and rosacea are visibly improved.
The accurate dispersion of Botox superficially can only be achieved by keeping the droplet size small and delivering these at regular intervals of approximately 1 cm. Droplet size ultimately controls diffusion, which allows more precise delivery of the toxin to the target layers. The aim is not to paralyze the muscle totally as in traditional Botox techniques.
HISTORICAL BACKGROUND
When Botox was first made available commercially for clinical use in the mid-1990s, it was the first time that physicians encountered a drug that could be delivered so easily to selectively paralyze and weaken muscles. As an intramuscular injection it was a tremendous novelty to be able to render these muscles inactive, with the unintentional result of an era of “overenthusiastic, obsessive” paralysis, which creates the undesired over-Botoxed or frozen look.
Many patients complained that their forehead felt too frozen and stiff, and some had difficulty lifting their brows or even complained of droopy eyebrows and loss of definition of the eyelid crease. Early experience often involved injecting too much Botox into the forehead in the mistaken belief that a smooth forehead was the only desired ideal for patients.
As practitioners refined their appreciation of beauty over the years, it became evident that patients did not want a smooth forehead at the expense of low set, angry eyebrows. What was desired was a natural, smooth-looking forehead that could still move and elevate the eyebrows. This appears to be a paradox, because the muscles responsible for the forehead lines are the same muscles that are responsible for elevation of the eyebrows. It therefore became obvious that a technique of Botox administration was needed that decreased visible forehead lines but still allowed the underlying muscles to move and the eyebrows to elevate.
A common observation was that when the Botox was injected intramuscularly into the frontalis muscle, the overlying forehead skin would often become shiny, smooth, and tight with few if any visible pores. Many patients liked this “resurfaced” look. It was subsequently discovered that this effect was the result of the Botox diffusing back into the skin and inhibiting the sweat and sebaceous glands because the droplet size recommended was too large and had a greater radius of diffusion beyond its intended target area.
Traditionally 100 units of Botox was reconstituted with 2.5 ml saline, and a 1 ml syringe would therefore contain 40 units. Thus 0.1 ml of this reconstituted solution contained 4 units of Botox, which became the default recommended dose for each of the five points of the glabellar area (20 units) and the six points of the crow′s-feet (24 units) injection patterns that are currently approved for on-label use in many territories.
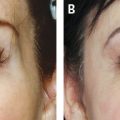
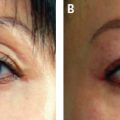
Another clinical problem encountered was in achieving a smooth lower eyelid. After the conventionally placed Botox injections for the glabellar, crow′s-feet, and forehead regions, patients often experienced pronounced “bunny lines” and fine wrinkles just under the lower lid eyelash margin that they found disturbing. The administration of traditional Botox to the infraorbital area and to the hypertrophic muscle bundle of the lower lid may provide a pleasing result, with a reduction in visible fine lines and a slight opening of the orbital aperture, which makes the eye look bigger and more attractive. These are usually younger patients without significant lower eye bags. However, some patients experience distressing complications with resulting bags under the eyes, a waterlogged appearance, and an unwelcome inanimate response of the lower lid with smiling. These patients feel they look worse than before the Botox administration. These are invariably older patients with unrecognized eye bags or skin laxity in whom relaxation of the infraorbital orbicularis oculi muscle allows the eye bags to bulge and become more visible. The action of the muscles before Botox administration helps to keep the skin tightened in a state of tension and push the eye bags inward, thus rendering them less obvious. The issue is only unmasked when the muscles relax and are no longer able to provide any resistance to the eye bags and they herniate outward.
A third problem area was the neck. Early techniques advocated administering traditional Botox (Botox diluted with 2 to 2.5 ml of saline) into the anterior and lateral platysmal bands without injecting into the muscle between these bands, over the horizontal neck creases, or above the jawline. Some patients had good results with softening of the platysmal bands and improvement of the cervicomental angle, but none experienced a lifting of the jawline, reduction of horizontal lines, or improvement of neck skin quality.
In looking for a solution to these three problems, and drawing on my experience with intradermal injections of Botox to the axilla to decrease hyperhidrosis and odor, I developed the Microbotox technique.5–7
ORIGIN OF MICROBOTOX AND ITS NOMENCLATURE
This technique was originally termed Mesobotox. However, that this term did not accurately portray the scientific principles and concepts underpinning the technique; hence the term Microbotox was coined and adopted in 2002. It is essentially an intradermal or subdermal injection of evenly spaced, very dilute Botox to inhibit the action of sebaceous and sweat glands and the superficial layer of facial muscles. It requires careful preparation of the solution and a sensitive and refined injection technique, which is the key to a successful outcome. Injecting too large a bolus at any given point will flood the area with Botox and may cause total muscle paralysis, which is not desired.
PHYSIOLOGIC BASIS FOR ACTION
Botox is well known as a versatile drug that inhibits a variety of receptors, including substance P. New uses of the toxin are constantly being discovered, such as in the reduction of masseteric muscle and parotid gland hypertrophy.4,8–10 The principle action of Botox is to block cholinergic receptors, which inhibits neuromuscular transmission. This relaxes muscles, which in turn decreases the intensity of facial wrinkles. Sweating is also largely mediated through cholinergic receptors and is inhibited by Botox as well. Hence Botox is able to decrease muscular activity and alter the quality of the overlying skin of the injected area.
CONCEPT OF MICROBOTOX
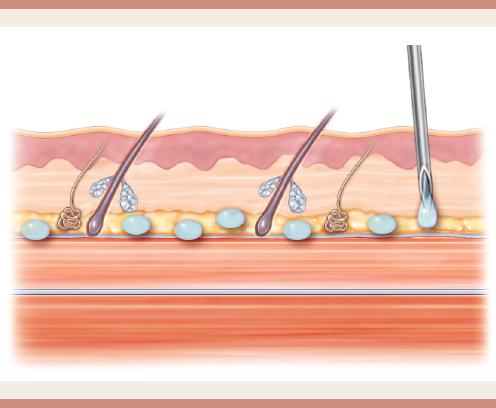
In traditional Botox administration, the objective is to bring about muscle weakening or paralysis; in the case of Botox facial sculpting, the goal is atrophy of the masseteric muscle bulk or reduction of iatrogenic parotid gland hypertrophy.4,8–10 Therefore the Botox should be injected into the muscle itself for best effect (Fig. 11-1). This can sometimes lead to pain and bruising. Because the margin for error is higher when injecting into the muscle, surgeons may be more cavalier in their injection technique in these traditional areas, often not ensuring that the correct dose of Botox is being delivered in a precise fashion.
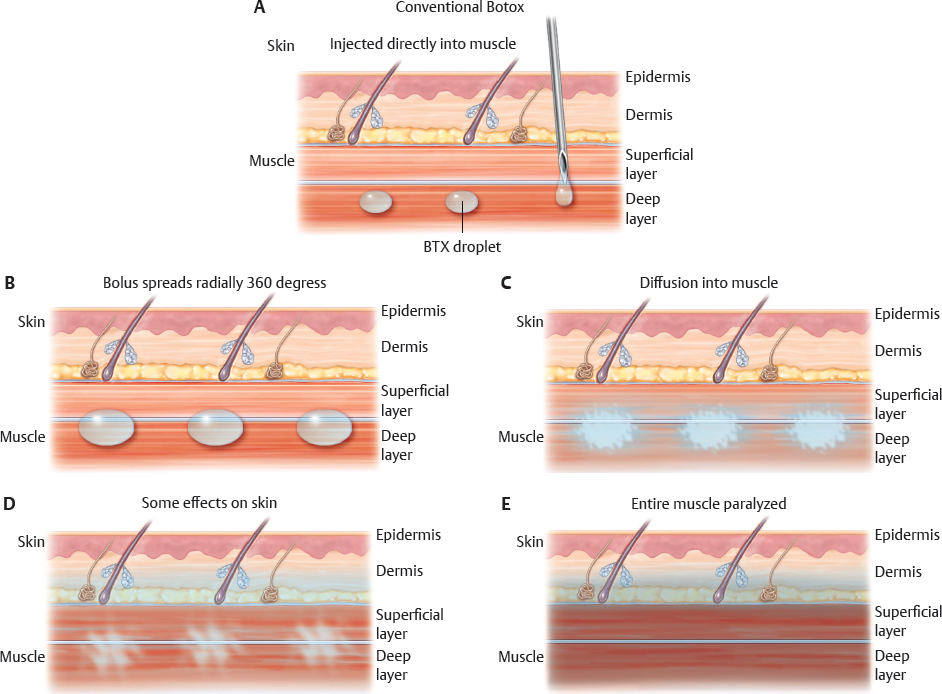
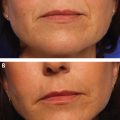
For Microbotox, the delivery technique is very important, because multiple tiny boluses of Botox are injected into the dermis or into the junction between the dermis and the superficial layer of the facial or neck muscles. This effectively weakens the superficial layer of these muscles, which are uniquely attached to the undersurface of the facial skin and are responsible for the fine lines and wrinkles that patients dislike. In the skin, the sweat and sebaceous gland activity is reduced (mediated through both cholinergic and noradrenergic receptors), and they become atrophic. This causes the skin envelope to shrink, and patients feel tighter and lifted. Reduction of sebaceous secretion also helps in the control of acne but more importantly makes open pores appear smaller and fewer. As a result the skin looks more refined and has a smooth sheen to it (Fig. 11-2).
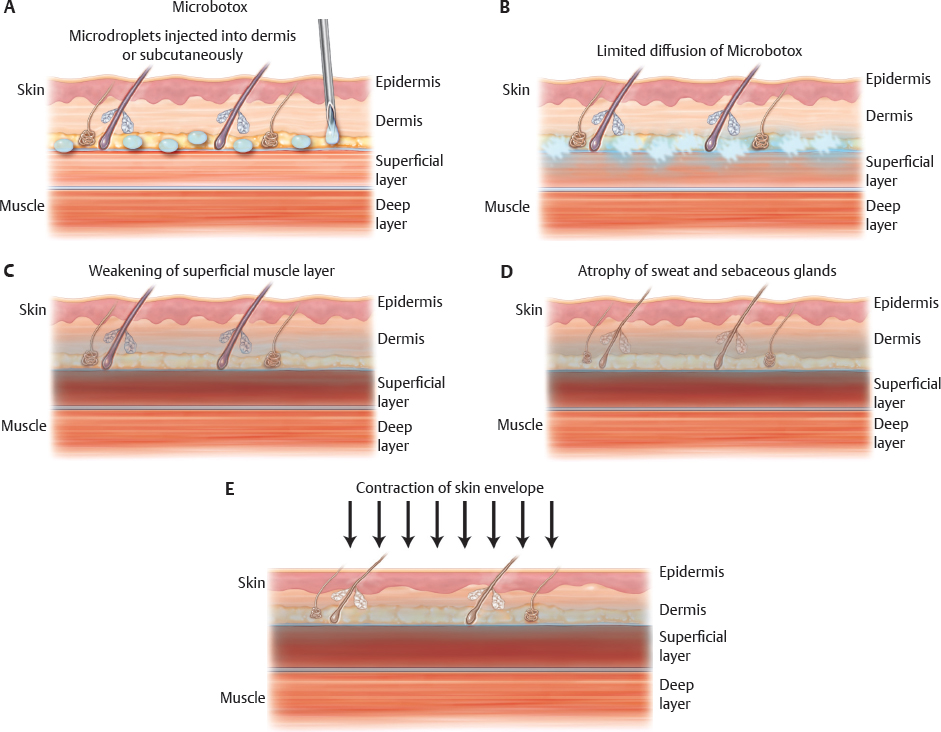
DILUTION AND INJECTION TECHNIQUE FOR MICROBOTOX
A 100-unit bottle of Botox is diluted with 2.5 ml of normal saline. This dilution is used for all injections of standard Botox to the face or masseter muscles (Botox facial slimming); as mentioned previously, 0.1 ml of this solution contains 4 units of Botox, and 0.05 ml contains 2 units of Botox.6
For the Microbotox technique, depending on the region of the face or neck to be injected, the required quantity is drawn up into a 1 ml syringe, which is then topped up to 1 ml with normal saline or 0.5% lidocaine.
For example, if the combined forehead, glabellar, and crow′s-feet regions require 24 units of Botox, then 0.6 ml of the prepared standard Botox (2.5 ml dilution) is drawn into a 1 ml syringe and an additional 0.4 ml of saline or 0.5% lidocaine is added to create 1 ml of injectable solution. This equates to 24 units of Botox in 1 ml of solution. I prefer lidocaine for the additional diluent and have not observed any decrease in effect or duration of the toxin with its use
Different dilutions are used for different parts of the face, neck, and body, especially when treating patients solely for pore closure or smoothing of the skin when disturbing the underlying muscle activity is not desirable. I use three standard dilutions:
1. 20 units in 1 ml solution for decreasing oily skin, visible pores, and rosacea in the T zone and over the central third of the face, including the nose. This dilution may also be used for infraorbital fine lines.
2. 24 units in 1 ml solution for treating the forehead, glabellar, and crow′s-feet regions.
3. 28 units in 1 ml solution for treating one side of the jawline and neck to smooth the appearance of vertical bands and horizontal creases, to elevate the jowls, and to improve cervicomental contouring.11 Two syringes (2 ml, or 56 units of Botox) are required to adequately cover both sides of the upper two thirds of the lower face and neck. Occasionally in thick necks with strong platysmal bands, as seen in heavyset patients, three syringes (3 ml, or 74 units of Botox) may be required.
Experience is required to develop proper injection technique; novice injectors can practice by filling a 1 ml syringe with normal saline, attaching a 30- or 31-gauge needle, and then injecting rows of microdroplets onto a smooth reflective surface, such as a mirror. Physicians should practice this until they are adept at delivering small or large droplets consistently. Most physicians attempting this exercise are surprised to learn that they typically overinject the Botox and do not deliver evenly sized boluses with each injection (Fig. 11-3).

In reality, a 0.1 ml droplet of solution is quite large; an inaccurately placed droplet near the eyebrow (when treating glabellar frown lines) can cause unwanted diffusion to the levator muscles, thereby causing temporary ptosis of the upper eyelid. The volume of a droplet directly affects its radius of diffusion.
A 0.05 ml droplet contains 2 units of Botox and is the volume of each droplet I use when doing standard intramuscular injections. Where muscles are thicker or more dense (as in men), 0.1 ml droplets are used.
For Microbotox, a 0.05 ml droplet can be injected instead as multiple smaller droplets. Depending on the skill of the operator, 0.05 ml can easily be injected in 10 to 14 drops (see Fig. 11-3). Clinically, if the operator can divide an injection of 0.05 ml into 10 drops, this is sufficient. A 1 ml syringe of Microbotox solution should deliver 100 to 120 droplets if performed correctly.
The small boluses of Botox should be injected slowly and evenly, with boluses spaced about 1 cm apart in a gridlike fashion. Once the injections can be performed steadily and the boluses made even smaller, the injection distance can be reduced to less than 1 cm. All air bubbles must be carefully removed from the syringe before injection, because they may compromise the injection accuracy.
The Forehead
The objective of Microbotox of the forehead is to retain as much muscular function and hence eyebrow elevation as possible while simultaneously smoothing the skin, reducing pore size, improving the sheen, and reducing rhytids, especially those over the lateral forehead, which are a reflection of overactive frontalis muscle activity. A total of 24 units is sufficient for the entire forehead, including the eight points of injection over the glabellar and eyebrow region to decrease corrugator activity and the eight points over the crow′s-feet area. If traditional Botox has already been given to the glabellar, eyebrow, and central forehead region for a browlift, 12 units (0.5 ml of the prepared solution) is sufficient to treat the lateral forehead alone (Fig. 11-4). This treatment will typically last 4 months.
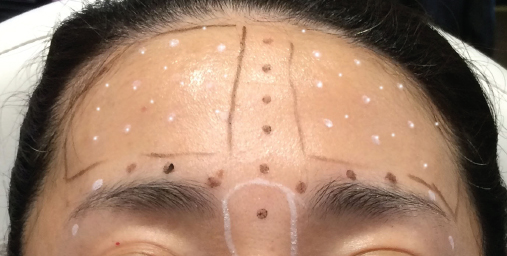
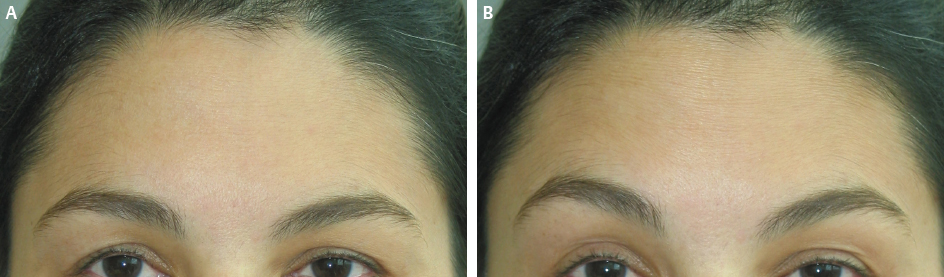
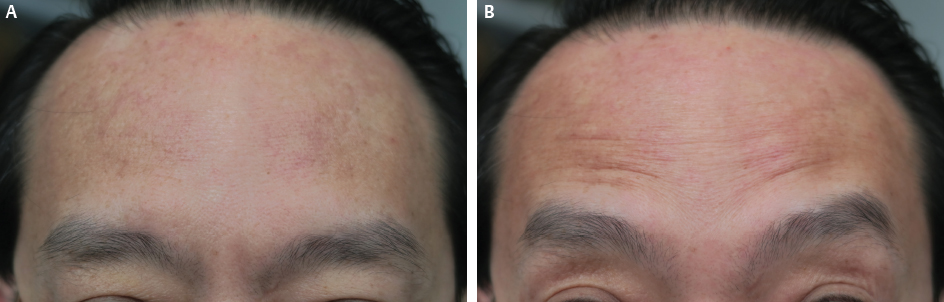
On average the forehead will be covered with 40 to 50 injection points. To anesthetize the forehead, a supraorbital nerve block with a small bolus of 0.5% lidocaine without adrenaline administered to the supraorbital nerves will provide adequate numbness. In addition, 5% topical lidocaine can be used to supplement the areas not covered by the nerve blocks. Patients seldom complain of pain even if an anesthetic is not used because of the small volume of the injection. Underinjecting the lateral forehead is preferable to avoid lowering of the eyebrow or creating a sensation of heaviness. Patients should have a smooth forehead but still be able to elevate their eyebrows and look natural (Figs. 11-5 and 11-6).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree